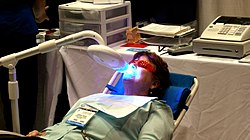
Medicine:Tooth whitening
Tooth whitening or tooth bleaching is the process of lightening the color of human teeth.[1] Whitening is often desirable when teeth become yellowed over time for a number of reasons, and can be achieved by changing the intrinsic or extrinsic color of the tooth enamel.[2] The chemical degradation of the chromogens within or on the tooth is termed as bleaching.[1]
Hydrogen peroxide (H2O2) is the active ingredient most commonly used in whitening products and is delivered as either hydrogen peroxide or carbamide peroxide.[1] Hydrogen peroxide is analogous to carbamide peroxide as it is released when the stable complex is in contact with water. When it diffuses into the tooth, hydrogen peroxide acts as an oxidising agent that breaks down to produce unstable free radicals. In the spaces between the inorganic salts in tooth enamel, these unstable free radicals attach to organic pigment molecules resulting in small, less heavily pigmented components.[3] Reflecting less light, these smaller molecules create a "whitening effect".[3] There are different products available on the market to remove stains.[1] For whitening treatment to be successful, dental professionals (dental hygienist or dentist) should correctly diagnose the type, intensity and location of the tooth discolouration.[3] Time exposure and the concentration of the bleaching compound, determines the tooth whitening endpoint.[1]
Natural shade
The perception of tooth colour is multi-factorial. Reflection and absorption of light by the tooth can be influenced by a number of factors including specular transmission of light through the tooth; specular reflection at the surface; diffuse light reflection at the surface; absorption and scattering of light within the dental tissues; enamel mineral content; enamel thickness; dentine colour, the human observer, the fatigue of the eye, the type of incident light, and the presence of extrinsic and intrinsic stains.[4] Additionally, the perceived brightness of the tooth can change depending on the brightness and colour of the background.[4]
The combination of intrinsic colour and the presence of extrinsic stains on the tooth surface influence the colour and thus the overall appearance of teeth.[2] The scattering of light and absorption within enamel and dentine determine the intrinsic colour of teeth and because the enamel is relatively translucent, the dentinal properties can play a major role in determining the overall tooth colour.[4] On the other hand, extrinsic stain and colour is the result of coloured regions that have formed within the acquired pellicle on the enamel surface and can be influenced by lifestyle behaviours or habits.[2] For example, dietary intake of tannin-rich foods, poor tooth brushing technique, tobacco products, and exposure to iron salts and chlorhexidine can darken the colour of a tooth.[2]
With increasing age, teeth tend to be darker in shade.[5] This can be attributed to secondary dentin formation and thinning of enamel due to tooth wear which contributes to a significant decrease in lightness and increase in yellowness.[5] Tooth shade is not influenced by gender or race.[5]
Staining and discolouration
Tooth discolouration and staining is primarily due to two sources of stain: intrinsic and extrinsic (see Figure 2).[1] In essence, tooth whitening primarily targets those intrinsic stains in which cannot be removed through mechanics such as a debridement (clean) or prophylaxis, in the dental office.[6] Below explains in-depth the differences between the two sources of which contribute to such discolouration of the tooth's surface.
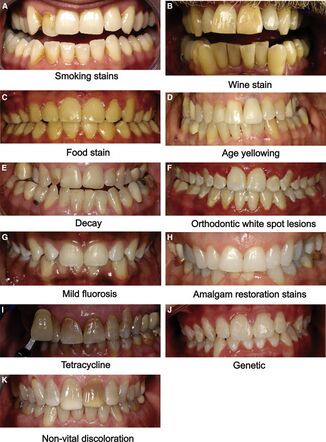
Extrinsic staining
Extrinsic staining, is largely due to environmental factors including smoking, pigments in beverages and foods, antibiotics, and metals such as iron or copper. Coloured compounds from these sources are adsorbed into acquired dental pellicle or directly onto the surface of the tooth causing a stain to appear.[7]
- Dental plaque: Dental plaque is a clear biofilm of bacteria that naturally forms in the mouth, particularly along the gumline, and it occurs due to the normal development and defences of the immune system.[8] Although usually virtually invisible on the tooth surface, plaque may become stained by chromogenic bacteria such as Actinomyces species.[9] Prolonged dental plaque accumulation on the tooth surface can lead to enamel demineralisation and formation of white spot lesions which appear as an opaque milk-coloured lesion.[10] The acidic by-products of fermentable carbohydrates derived from high-sugar foods contribute to greater proportions of bacteria, such as Streptococcus mutans and Lactobacillus in dental plaque. Higher consumption of fermentable carbohydrates will promote demineralisation and increase the risk of developing white spot lesions.[8]
- Calculus: neglected plaque will eventually calcify, and lead to the formation of a hard deposit on the teeth, especially around the gumline. The organic matrix of dental plaque and calcified tissues undergo a series of chemical and morphological changes that lead to calcification of the dental plaque and therefore leading to the formation of calculus.[11] The color of calculus varies, and may be grey, yellow, black, or brown.[9] The colour of calculus depends on how long it has been present in the oral cavity for; it typically starts off yellow and over time the calculus will begin to stain a darker colour and become more tenacious and difficult to remove.
- Tobacco: tar in the smoke from tobacco products (and also smokeless tobacco products) tends to form a yellow-brown-black stain around the necks of the teeth above the gumline.[9] The nicotine and tar in tobacco, combined with oxygen, turns yellow and over time will absorb into the pores of enamel and stain the teeth yellow. The dark brown to black stains along the gum line of the teeth are the result of the porous nature of calculus immediately picking up the stains from nicotine and tar.
- Betel chewing.[12] Betel chewing produces blood-red saliva that stains the teeth red-brown to nearly black.[13] The extract gel of betel leaf contain tannin, a chromogenic agent that causes discolouration of the tooth enamel.[14]
- Tannin is also present in coffee, tea, and red wine and produces a chromogenic agent that can discolor teeth.[15] Large consumptions of tannin-containing beverages stain the dental enamel brown due to the chromogenic nature.[16]
- Certain foods, including curries and tomato-based sauces, can cause teeth staining.[17]
- Certain topical medications: Chlorhexidine (antiseptic mouthwash) binds to tannins, meaning that prolonged use in persons who consume coffee, tea or red wine is associated with extrinsic staining (i.e. removable staining) of teeth.[18] Chlorhexidine mouthwash has a natural liking for sulphate and acidic groups commonly found in areas where plaque accumulates such as along the gumline, on the dorsum of the tongue and cavities. Chlorhexidine is retained in these areas and stain yellow-brown. The stains are not permanent and can be removed with proper brushing.[19]
- Metallic compounds. Exposure to such metallic compounds may be in the form of medication or occupational exposure. Examples include iron (black stain), iodine (black), copper (green), nickel (green), and cadmium (yellow-brown).[20] Sources of exposure to metal include placing metal into the oral cavity, metal-containing dust inhalation, or oral administration of drugs. Metals can enter the bony structure of the tooth, causing permanent discolouration, or can bind to the pellicle causing surface stain.[19]
Removal of extrinsic staining
Extrinsic staining may be removed through various treatment methods:
- Prophylaxis: dental prophylaxis includes the removal of extrinsic staining using a slow-speed rotary handpiece and a rubber cup with abrasive paste, mostly containing fluoride.[citation needed] The abrasive nature of the prophy paste, as it is known, acts to remove extrinsic staining using the action of the slow-speed handpiece and the paste against the tooth. Adversely, the action of the rubber cup together with the abrasive nature of the paste, removes around one micron of enamel from the tooth surface every time a prophylaxis is performed. This method of stain removal may only take place in the dental office.
- Micro-abrasion: allows a dental professional to make use of an instrument which emits a powder, water and compressed air to remove biofilm, and extrinsic staining. This stain removal method can only be undertaken in a dental office, not at home.
- Toothpaste: there are many available on the market that implement both peroxide as well as abrasive particles, such as silica gel, to help remove extrinsic stains, while the peroxide acts on intrinsic staining. This method of stain removal may take place at home as well as in a dental office.
Intrinsic staining
Intrinsic staining primarily occurs during the tooth development either before birth or at early childhood. Intrinsic stains are those that cannot be removed through mechanical measures such as debridement or a prophylactic stain removal. As the age of the person increases, the teeth can also appear yellower over time.[15] Below are examples of intrinsic sources of stains:
- Tooth wear and aging: Tooth wear is a progressive loss of enamel and dentine due to tooth erosion, abrasion and attrition. As enamel wears down, dentine becomes more apparent and chromogenic agents are penetrated in the tooth more easily. The natural production of secondary dentine also gradually darkens teeth with age.[21]
- Dental cavities (tooth decay):[12] The evidence regarding carious tooth discolouration is inconclusive, however the most reliable evidence suggests that carious lesion allows for exogenous agents to enter dentine and hence increased absorption of chromogenic agents causing discolouration to the tooth.[21]
- Restorative materials: The materials used during root canal treatments, such as eugenol and phenolic compounds, contain pigment that stain dentine. Restorations using amalgam also penetrate dentine tubules with tin over time therefore causing dark stains to the tooth.[21]
- Dental trauma[12] which may cause staining either as a result of pulp necrosis or internal resorption. Alternatively the tooth may become darker without pulp necrosis.
- Enamel hypoplasia: Enamel hypoplasia causes enamel to be thin and weak. It produces a yellow-brown discolouration and can also cause the enamel's smooth surface to be rough and pitted which causes the tooth to be susceptible to extrinsic staining, tooth sensitivity, malocclusion, and dental cavities.[22] The evidence regarding enamel hypoplasia is inconclusive, however the most likely cause is infection or trauma caused to the primary dentition. Disturbances to the developing tooth germ during neonatal and early childhood stages such as maternal vitamin D deficiency, infection, and medication intake can cause enamel hypoplasia.[21]
- Pulpal hyperemia: Pulpal hyperemia refers to inflammation of a traumatised tooth which can be caused by a stimuli such as trauma, thermal shock, or dental cavities. Pulpal hyperemia is reversible[23] and produces a red hue seen initially after trauma which has the ability to disappear if the tooth becomes revascularized.[21]
- Fluorosis:[20] Dental fluorosis causes enamel to become opaque, chalky white, and porous. The enamel can break down and cause the exposed subsurface enamel to become mottled and produce extrinsic dark brown-black stains.[24] Dental fluorosis occurs due to excessive ingestion of fluoride or overexposure to fluoride during the development of enamel which usually occurs between the ages of one to four. Fluoridated drinking water, fluoride supplements, topical fluoride (fluoride toothpastes), and formula prescribed for children can increase the risk of dental fluorosis. Fluoride is considered an important factor in the management and prevention of dental cavities, the safe level for daily fluoride intake is 0.05 to 0.07 mg/kg/day.[25]
- Dentinogenesis imperfecta:[20] Dentinogenesis imperfecta is a hereditary dentine defect, associated with osteogenesis imperfecta, which causes the tooth to become discoloured usually blue or brown in colour and translucent giving teeth an opalescent sheen.[21] The condition is autosomal dominant which means that the condition runs in the family.
- Amelogenesis imperfecta:[20] The appearance of amelogenesis imperfecta depends on the type of amelogenesis, there are 14 different subtypes and can vary from the appearance of hypoplasia to hypomineralisation which can produce different appearances of enamel from white mottling to yellow brown appearances.[21]
- Tetracycline and minocycline. Tetracycline is a broad-spectrum antibiotic,[26] and its derivative minocycline is common in the treatment of acne.[27] The drug is able to chelate calcium ions and is incorporated into teeth, cartilage, and bone.[26] Ingestion during the years of tooth development causes yellow-green discoloration of dentine visible through the enamel which is fluorescent under ultraviolet light. Later, the tetracycline is oxidized and the staining becomes more brown and no longer fluoresces under UV light.[9][28]
- Porphyria:[9] A rare metabolic disorder in which the body fails to adequately metabolise porphyrins, which leads to accumulation or excretion of porphyrins into teeth. The excretion of porphyrins produces purple-red pigments in teeth.[29]
- Hemolytic disease of the newborn:[9] This disease occurs when a newborn's red blood cells are being attacked by antibodies from the mother caused by an incompatibility between the mother and baby's blood. This condition can produce green staining of teeth due to jaundice, which is an inability to excrete bilirubin properly.[30]
- Root resorption:[31] Root resorption is clinically asymptomatic; however, it can produce a pink appearance at the amelocemental junction.[21]
- Alkaptonuria:[31] Metabolic disorder which promotes the accumulation of homogentisic acid in the body and may cause brown colour pigmentation in the teeth, gums, and buccal mucosa.[32]
Methods
Prior to proceeding to tooth whitening alternatives, it is advised that the patient comes into the dental office to have a comprehensive oral examination that consists of a full medical, dental, and social history. This will allow the clinician to see if there is any treatment that needs to be done such as restorations to remove cavities, and to assess whether or not the patient will be a good candidate to have the whitening done. The clinician would then debride (clean) the tooth surface with an ultrasonic scaler, hand instruments, and potentially a prophy paste to remove extrinsic stains as mentioned above. This will allow a clean surface for maximum benefits of whichever tooth whitening method the patient chooses.[6] Below will discuss the various types of tooth whitening methods including both internal application of bleaching and external application through the use of bleaching agents.
In-office
Before the treatment, the clinician should examine the patient: taking a health and dental history (including allergies and sensitivities), observe hard and soft tissues, placement and conditions of restorations, and sometimes x-rays to determine the nature and depth of possible irregularities. If this is not completed prior to the whitening agents being applied to the tooth surface, excessive sensitivity and other complications may occur.
The whitening shade guides are used to measure tooth colour. These shades determine the effectiveness of the whitening procedure, which may vary from two to seven shades.[33] These shades may be reached after a single in office appointment, or may take longer, depending on the individual. The effects of bleaching can last for several months, but may vary depending on the lifestyle of the patient. Consuming tooth staining foods or drinks that have a strong colour may compromise effectiveness of the treatment. These include food and drinks containing tannins such as; coffee, tea, red wines, and curry.
In-office bleaching procedures generally use a light-cured protective layer that is carefully painted on the gums and papilla (the tips of the gums between the teeth) to reduce the risk of chemical burns to the soft tissues. The bleaching agent is either carbamide peroxide, which breaks down in the mouth to form hydrogen peroxide, or hydrogen peroxide itself. The bleaching gel typically contains between 10% and 44% carbamide peroxide, which is roughly equivalent to a 3% to 16% hydrogen peroxide concentration. The legal percentage of hydrogen peroxide allowed to be given is 0.1–6%.[where?] Bleaching agents are only allowed to be given by dental practitioners, dental therapists, and dental hygienists.
Bleaching is least effective when the original tooth color is grayish and may require custom bleaching trays. Bleaching is most effective with yellow discolored teeth. If heavy staining or tetracycline damage is present on a patient's teeth, and whitening is ineffective (tetracycline staining may require prolonged bleaching, as it takes longer for the bleach to reach the dentine layer), there are other methods of masking the stain. Bonding, which also masks tooth stains, is when a thin coating of composite material is applied to the front of a person's teeth and then cured with a blue light. A veneer can also mask tooth discoloration.
In-chair whitening is faster and more effective in comparison to the take-home bleaching options. Some clinicians also make custom bleaching trays, which can take up to a week to create. After the whitening treatment is completed, the patient is able to use these trays for maintenance of their bleaching with at-home kits or for use with desensitising products.
Light-accelerated bleaching
Power or light-accelerated bleaching uses light energy which is intended to accelerate the process of bleaching in a dental office. Different types of energy can be used in this procedure, with the most common being halogen, LED, or plasma arc. Use of light during bleaching increases the risk of tooth sensitivity and may not be any more effective than bleaching without light when high concentrations of hydrogen peroxide are used.[34] A 2015 study showed that the use of a light activator does not improve bleaching, has no measurable effect, and rather is likely to increase the temperature of the associated tissues, resulting in damage.[35][36]
The ideal source of energy should be high energy to excite the peroxide molecules without overheating the pulp of the tooth.[37] Lights are typically within the blue light spectrum as this has been found to contain the most effective wavelengths for initiating the hydrogen peroxide reaction. A power bleaching treatment typically involves isolation of soft tissue with a resin-based, light-curable barrier, application of a professional dental-grade hydrogen peroxide whitening gel (25–38% hydrogen peroxide), and exposure to the light source for 6–15 minutes. Recent technical advances have minimized heat and UV emissions, allowing for a shorter patient preparation procedure.
For any whitening treatments, it is recommended that a comprehensive examination of the patient is done including the use of radiographs to aid in the diagnosis of the current condition of the mouth, including any allergies that may be present. The patient will need to have a healthy mouth and free of periodontal disease or cavities and to have had a debridement/clean done to remove any tartar or plaque build up.[38]
It is recommended to avoid smoking, drinking red wine, eating or drinking any deeply coloured foods after this as the teeth may stain considerably straight after treatment.
Nanoparticle catalysts for reduced hydrogen peroxide concentration
A recent addition to the field is new light-accelerated bleaching agents containing lower concentrations of hydrogen peroxide with a titanium oxide nanoparticle-based catalyst. Reduced concentrations of hydrogen peroxide cause lower incidences[spelling?] of tooth hypersensitivity.[39] The nanoparticles act as photocatalysts, and their size prevents them from diffusing deeply into the tooth. When exposed to light, the catalysts produce a rapid, localized breakdown of hydrogen peroxide into highly reactive radicals. Due to the extremely short lifetimes of the free radicals, they are able to produce bleaching effects similar to much higher concentration bleaching agents within the outer layers of the teeth where the nanoparticle catalysts are located. This provides effective tooth whitening while reducing the required concentration of hydrogen peroxide and other reactive byproducts at the tooth pulp.
Internal bleaching
Internal bleaching is a process which occurs after a tooth has been endodontically treated. This means that the tooth will have had the nerve of the tooth extirpated or removed through a root canal treatment at the dentist or by a specialist endodontist. Internal bleaching is often sought after in teeth which have been endodontically treated as tooth discolouration becomes a problem due to the lack of nerve supply to that tooth. It is common to have this internal bleaching done on an anterior tooth (a front tooth that you can see when smiling and talking). A way around this is by sealing off the bleaching agent inside the tooth itself and replacing it every few weeks until the desired shade has been achieved. The amount of time between appointments varies from patient to patient and with operator preference until the desired shade has been achieved.[40] Even though this is a great option, the disadvantage of this treatment is a risk of internal root resorption of the tooth that is being internally bleached. This may not occur in every patient or every tooth, and its occurrence is difficult to determine prior to completing the treatment.[40]
At home
At home tooth whitening products are available from dentists or 'over the counter' (OTC).[41] At home whitening methods include over-the-counter strips and gels, whitening rinses, whitening toothpastes, and tray-based tooth whiteners.[41] OTC products can be used for milder cases of tooth staining.[41] Home-based bleaching (following manufacturer's instructions) results in less tooth sensitivity than in-office bleaching.[42]
Strips and gels
The plastic whitening strips contain a thin layer of peroxide gel and are shaped to fit the buccal/labial surfaces of teeth.[1] Many different types of whitening strips are available on the market, after being introduced in the late 1980s.[1] Specific whitening strip products have their own set of instructions however the strips are typically applied twice daily for 30 minutes for 14 days.[1] In several days, tooth colour can lighten by 1 or 2 shades.[1] The tooth whitening endpoint does depend on the frequency of use and ingredients of the product.[1]
Whitening gels are applied onto the tooth surface with a small brush.[1] The gels contain peroxide and are recommended to be applied twice a day for 14 days.[1] The tooth whitening endpoint like that of the whitening strips.[1]
Rinses
Whitening rinses work by reaction of the oxygen sources such as hydrogen peroxide within the rinse and the chromogens on or within the tooth.[1] It is recommended to use twice a day, rinsing for one minute.[1] To see an improvement in shade colour, it can take up to three months.[1]
Toothpastes
Whitening toothpastes differ from regular toothpastes in that they contain higher amounts of abrasives and detergents to be more effective at removing tougher stains.[1] Some whitening toothpastes contain low concentrations of carbamide peroxide or hydrogen peroxide which help lighten tooth colour however they do not contain bleach (sodium hypochlorite).[1] With continuity of use over time, tooth colour can lighten by one or two shades.[1]
Tray-based
Tray-based tooth whitening is achieved by wearing a fitted tray containing carbamide peroxide bleaching gel overnight or for two to four hours a day.[1] If manufacturer's instructions are followed, tooth whitening can occur within three days and lighten teeth by one or two shades.[1] This type of tooth whitening is available over-the-counter and professionally from an oral health professional.[1]
Baking soda
Baking soda is a safe, low abrasive, and effective stain removal and tooth whitening toothpaste.[43] Tooth whitening toothpaste that have excessive abrasivity are harmful to dental tissue, therefore baking soda is a desirable alternative.[43] To date, clinical studies on baking soda report that there have been no reported adverse effects.[43] It also contains acid-buffering components that makes baking soda biologically antibacterial at high concentrations and capable of preventing growth of Streptococcus mutans.[43] Baking soda might be useful for cavities-prone patients, as well as those who wish to have whiter teeth.[43]
Pens
Whitening pens are a convenient way to touch up any dental surface. The plastic, convenient, tube contains a bleaching gel that can be easily applied in hard-to-reach spots. In order to work, the gel needs to stay on the tooth surface for around 20–30 minutes.[44]
Indications
Tooth whitening may be undertaken for a variety of reasons, but whitening may also be recommended to some individuals by dental professionals.[45]
- Intrinsic tooth staining
- Aesthetics
- Dental fluorosis
- Endodontic treatment (internal bleaching)
- Tetracycline staining
Contraindications
Some groups are advised to carry out tooth whitening with caution as they may be at higher risk of adverse effects.
- Patients with unrealistic expectations
- Allergy to peroxide
- Pre-existing sensitive teeth
- Cracks or exposed dentine
- Enamel development defects
- Acid erosion
- Receding gums (gingival recession) and yellow roots
- Sensitive gums
- Defective dental restorations
- Tooth decay. White-spot decalcification may be highlighted and become more noticeable directly following a whitening process, but with further applications the other parts of the teeth usually become more white and the spots less noticeable.
- Active periapical pathology
- Untreated periodontal disease
- Pregnant or lactating women
- Children under the age of 16. This is because the pulp chamber, or nerve of the tooth, is enlarged until this age. Tooth whitening under this condition could irritate the pulp or cause it to become sensitive. Younger people are also more susceptible to abusing bleaching.[46]
- Persons with visible white fillings or crowns. Tooth whitening does not change the color of fillings and other restorative materials. It does not affect porcelain, other ceramics, or dental gold. However, it can slightly affect restorations made with composite materials, cements and dental amalgams. Tooth whitening will not restore color of fillings, porcelain, and other ceramics when they become stained by foods, drinks, and smoking, as these products are only effective on natural tooth structure. As such, a shade mismatch may be created as the natural tooth surfaces increase in whiteness and the restorations stay the same shade. Whitening agents do not work where bonding has been used and neither is it effective on tooth-colored filling materials. Other options to deal with such cases are the porcelain veneers or dental bonding.[47]
- Individuals with poor oral hygiene
Risks
Some of the common side effects involved in teeth whitening are increased sensitivity of the teeth, gum irritation, and extrinsic teeth discolouration.[41]
Hypersensitivity
Potassium nitrate and sodium fluoride in toothpastes are used to ease discomfort following bleaching, however, there is no evidence to suggest that this is a permanent method to eradicate the issue of hypersensitivity.[48]
Irritation of mucous membranes
Hydrogen peroxide is an irritant and cytotoxic. Hydrogen peroxide with concentrations of 10% or higher can cause tissue damage, be corrosive to mucous membranes and cause burning sensation to the skin.[49] Chemical burns can commonly occur whilst bleaching, irritation and discolouration of the mucous membranes may occur if a high concentration of oxidising agent comes in to contact with unprotected tissue. Poorly fitting bleaching trays are amongst the most common reasons for chemical burns. The temporary burning induced by whitening treatments can be reduced by using custom-made plastic trays or nightguards provided by the dental professional. This prevents the leakage of solution onto the surrounding mucosa.[50]
Uneven results
Uneven results are quite common after bleaching. Consuming less foods and drinks that cause surface staining of teeth can contribute to attaining a good result from tooth whitening.
Return to original pre-treatment shade
Nearly half the initial change in colour provided by an intensive in-office treatment (i.e., one hour treatment in a dentist's chair) may be lost in seven days.[51] Rebound is experienced when a large proportion of the tooth whitening has come from tooth dehydration (also a significant factor in causing sensitivity).[52] As the tooth rehydrates, tooth colour "rebounds", back toward where it started.[53]
Over-bleaching
Over-bleaching, more often known as the "bleached effect", occurs among treatments that promise a large change over a short period of time e.g., hours. Over-bleaching can emit a translucent and brittle appearance.[54]
Damage to enamel
Teeth enamel can have an adverse negative effect by whitening treatment.[55] Evidence from studies show that carbamide peroxide present in whitening gels can damage the enamel surface. Although this effect is not as damaging as phosphoric acid etch,[56] the increased irregularity of the teeth surface makes the teeth more susceptible to extrinsic staining, thus having an increased detrimental effect on the aesthetics. The increased porosity and changes in surface roughness may have an impact on the formation of supra- and subgingival plaque, thus increasing the adhesion of bacterial species such as Streptococcus mutans and Streptococcus sobrinus, significant contributors to dental cavities.[50] Dental restorations are susceptible to unacceptable colour change even when using the home-based systems.[1]
Weakened dentine
Intracoronal bleaching is a tooth whitening method that uses 30% more hydrogen peroxide. Such tooth whitening methods can weaken the mechanical properties of dentine and could potentially lead to severe tooth sensitivity.[57]
Effects on existing restorations
Dental restorations are susceptible to unacceptable colour change even when using the home-based systems.[1]
Ceramic crowns – aggressive bleaching can chemically react with ceramic crowns and reduce their stability.[1]
Dental amalgam – exposure to carbamide peroxide solutions increase mercury release for one to two days.[57][58] The release of amalgam components is said to be due to active oxidation. This increase in amalgam mercury release is proportional to the concentration of carbamide peroxide.[59]
Resin composite – bond strength between enamel and resin based fillings become weakened.[60] Many studies have found that 10-16% carbamide peroxide tooth bleaching gels (containing approximately 3.6–5.76% hydrogen peroxide) leads to an increase in the surface roughness and porosity of composite resins.[59] However, the saliva may exert a protective effect. In addition, changes in the reflectance of the composite have been analysed following whitening with high concentration (30-35%) hydrogen peroxide.[59] This suggests that tooth whitening negatively impacts composite resin restorations.[59]
Glass ionomer and other cements – studies suggest that solubility of these materials may increase.[61]
Bleachorexia
Bleachorexia is the term that is used to describe an individual that develops an unhealthy obsession with teeth whitening.[46] This condition is similar to body dysmorphic disorder. The characteristics of bleachorexia are the continuous use of whitening products even though the teeth cannot possibly become whiter, despite the provision of repeated treatment.[54] A person with bleachorexia will continually seek out for different whitening products, hence, it is recommended that a target shade is agreed upon before starting the treatment procedure to help with this problem.[54]
Home teeth whitening risks
The use of personalised home whitening trays is a patient administered therapy that is prescribed and dispensed by a dentist.[62] Patients need to actively participate in their treatment and follow the guidelines given by the dentist accurately.[63] Erratic or inaccurate use of the bleaching trays could cause harm to the patient such as blistering or sensitivity of the teeth and the surrounding soft tissue.[64] Inconsistent use of the bleaching trays can lead to the slowing and irregularity of the whitening process.[65] Some patients with a substantial gag reflex may not be able to tolerate the trays and would need to consider other methods of teeth whitening.[63]
Other risks
Evidence suggests that hydrogen peroxide might act as a tumour promoter.[66] Although cervical root resorption is more evidently observed in thermocatalytic bleaching methods, intracoronal internal bleaching may also lead to tooth root resorption.[66] Moreover, severe damage to intracoronal dentine and tooth crown fracture can occur due to this bleaching method.[66]
However, the International Agency of Research on Cancer (IARC) has concluded that there is insufficient evidence to prove that hydrogen peroxide is a carcinogen to humans.[67] Recently, the genotoxic potential of hydrogen peroxide was evaluated. The results indicated that the oral health products that contain or release hydrogen peroxide up to 3.6% will not increase the cancerous risk of an individual,[68] hence, it is safe to use in moderation.
Maintenance
Despite achieving the results of treatment, stains can return within an initial couple of months of treatment. Various methods may be employed to prolong the treatment results, such as:[citation needed]
- Brush or flush out mouth with water after eating and drinking
- Floss to remove plaque and biofilms between the teeth
- Take special care during the first 2 days – the first 24–48 hours after the whitening procedure is seen as the most crucial period in which you must protect for your teeth the most. Hence, it is vital that non-staining drinks or foods are eaten during this time as enamel is prone to adhere to stains.
- Drink fluids that may cause staining through a straw
- Depending on the method used to whiten the teeth, re-treatment every six months or after a year may be required. If an individual is a smoker or they consume beverages with the capacity to stain, regular re-treatments would be required.
History
Teeth whitening remedies have been present since ancient times. Despite seeming absurd, some methods were somewhat effective in their results.
Ancient Roman dentists believed in using urine with goat milk to make their teeth look whiter.[69][70][71] Pearly white teeth symbolized beauty and marked wealth. In the Auyrveda medicine system, oil pulling was used as an oral therapy. For this process today, swish coconut or olive oil in your mouth for up to 20 minutes each day. In the late 17th century, many people reached out to barbers, who used a file to file down the teeth before applying an acid that would, in fact, whiten the teeth. Although the procedure was successful, the teeth would become completely eroded and more prone to becoming decayed.[72] Guy de Chauliac suggested the following to whiten the teeth: "Clean the teeth gently with a mixture of honey and burnt salt to which some vinegar has been added."[73] In 1877, oxalic acid was proposed for whitening, followed by calcium hypochlorite.[73]
In the late 1920s, mouthwash containing pyrozone (ether peroxide) was found to reduce cavities while providing a whiter appearance to the teeth.[74] By 1940s and 1950s, ether and hydrogen peroxide gels were used to whiten vital teeth, whereas non-vital teeth were whitened using pyrozone and sodium perborate.[74]
In the late 1960s, Dr William Klusmeier, an Orthodontist from Fort Smith, Arkansas, introduced the custom tray bleaching. However, it was not until 1989 that Haywood and Heymann published an article in support of this method. Carbamide peroxide with a shelf life of one to two years, as opposed to hydrogen peroxide with a shelf life one to two months, was seen as a more stable agent for whitening teeth.[74]
Society and culture
Teeth whitening has become the most promoted and mentioned methodology in cosmetic dentistry. In excess of 100 million Americans brighten their teeth using different methods; spending $15 billion in 2010.[75] The US Food and Drug Administration only endorses gels that are under 6% hydrogen peroxide or 16% or less of carbamide peroxide. The Scientific Committee on Consumer Safety of the EU consider gels containing higher fixations can be dangerous.[citation needed]
As per European Council guidelines, only a certified dental professional can lawfully give tooth whitening products utilizing 0.1–6% hydrogen peroxide, provided the patient is 18 years of age or older.[76] In 2010, the UK General Dental Council became concerned of the "risk to patient safety from poor quality tooth whitening being carried out by untrained or poorly trained staff."[77] A public attitudes survey, conducted by the GDC, showed that 83% of people support "policies of regulating tooth whitening to protect patient safety and prosecuting illegal practice."[77] A group of dental professionals and associations called The Tooth Whitening Information Group (TWIG) was founded to advance protected and beneficial tooth whitening information and assistance to the general population. Reports can be made to the TWIG through their website with respect to any individual giving unlawful tooth whitening services, or if an individual has personally undergone treatment done by a non-dental professional.
In Brazil, all whitening items are classed as cosmetics (Degree II).[46] There are worries that this will bring about increasing abuse of whitening products and thus there have been calls for reanalysis.[46]
According to research, tooth whitening can produce positive changes in young participants’ Oral Health Related Quality of Life (OHRQoL) in aesthetic areas such as smiling, laughing, and showing teeth without embarrassment. However, its main side-effect, tooth sensitivity, does negatively affect quality of life.[78]
See also
- Gum depigmentation
- Oral hygiene
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 Carey, Clifton M. (June 2014). "Tooth Whitening: What We Now Know". The Journal of Evidence-Based Dental Practice 14 Suppl: 70–76. doi:10.1016/j.jebdp.2014.02.006. PMID 24929591.
- ↑ 2.0 2.1 2.2 2.3 Joiner, Andrew; Luo, Wen (2017). "Tooth colour and whiteness: A review". Journal of Dentistry 67: S3–S10. doi:10.1016/j.jdent.2017.09.006. PMID 28928097.
- ↑ 3.0 3.1 3.2 Kihn, Patricia W. (2007). "Vital Tooth Whitening". Dental Clinics of North America 51 (2): 319–331. doi:10.1016/j.cden.2006.12.001. PMID 17532915.
- ↑ 4.0 4.1 4.2 Joiner, A.; Hopkinson, I.; Deng, Y.; Westland, S. (2008). "A review of tooth colour and whiteness". Journal of Dentistry 36 (Suppl 1): S2-7. doi:10.1016/j.jdent.2008.02.001. PMID 18646363.
- ↑ 5.0 5.1 5.2 Veeraganta, SumanthK; Savadi, RavindraC; Baroudi, Kusai; Nassani, MohammadZ (2015). "Differences in tooth shade value according to age, gender and skin color: A pilot study". Journal of Indian Prosthodontic Society 15 (2): 138–141. doi:10.4103/0972-4052.155035. ISSN 0972-4052. PMID 26929500.
- ↑ 6.0 6.1 Bernie, Kristy Menage (2011). "Professional whitening". Access 25: 12–15. https://www.adha.org/sites/default/files/7122_Phillips_Whitening.pdf.
- ↑ Carey, Clifton (2019-03-14). "Tooth Whitening: What We Now Know". The Journal of Evidence-Based Dental Practice 14: 70–76. doi:10.1016/j.jebdp.2014.02.006. PMID 24929591.
- ↑ 8.0 8.1 Marsh, Philip D. (2006-07-10). "Dental plaque as a biofilm and a microbial community – implications for health and disease". BMC Oral Health 6 (1): S14. doi:10.1186/1472-6831-6-S1-S14. ISSN 1472-6831. PMID 16934115.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 Rajendran A; Sundaram S (10 February 2014). Shafer's Textbook of Oral Pathology (7th ed.). Elsevier Health Sciences APAC. pp. 386, 387. ISBN 978-81-312-3800-4. https://books.google.com/books?id=WnhtAwAAQBAJ&pg=P528.
- ↑ Srivastava, Kamna; Tikku, Tripti; Khanna, Rohit; Sachan, Kiran (2013). "Risk factors and management of white spot lesions in orthodontics". Journal of Orthodontic Science 2 (2): 43–49. doi:10.4103/2278-0203.115081. ISSN 2278-1897. PMID 24987641.
- ↑ Zander, Helmut A.; Hazen, Stanley P.; Scott, David B. (1960-02-01). "Mineralization of Dental Calculus.". Proceedings of the Society for Experimental Biology and Medicine 103 (2): 257–260. doi:10.3181/00379727-103-25479. ISSN 0037-9727. PMID 13846953.
- ↑ 12.0 12.1 12.2 Crispian Scully (21 July 2014). Scully's Medical Problems in Dentistry. Elsevier Health Sciences UK. ISBN 978-0-7020-5963-6. https://books.google.com/books?id=OZXdAwAAQBAJ.
- ↑ Norton, Scott A. (1998-01-01). "Betel: Consumption and consequences" (in en). Journal of the American Academy of Dermatology 38 (1): 81–88. doi:10.1016/S0190-9622(98)70543-2. ISSN 0190-9622. PMID 9448210. https://www.jaad.org/article/S0190-9622(98)70543-2/abstract.
- ↑ Hoppy, D; Noerdin, A; Irawan, B; Soufyan, A (August 2018). "Effect of betel leaf extract gel on color change in the dental enamel". Journal of Physics: Conference Series 1073 (3): 032028. doi:10.1088/1742-6596/1073/3/032028. ISSN 1742-6588. Bibcode: 2018JPhCS1073c2028H.
- ↑ 15.0 15.1 Felton, Simon (2013). Basic Guide to Oral Health Education and Promotion. Hoboken : Wiley.
- ↑ Kumar, Arun; Kumar, Vijay; Singh, Janardhan; Hooda, Anita; Dutta, Samir (2011-09-13). "Drug-Induced Discoloration of Teeth". Clinical Pediatrics 51 (2): 181–185. doi:10.1177/0009922811421000. ISSN 0009-9228. PMID 21917545.
- ↑ "Top 10 teeth-staining foods". https://www.bupa.co.uk/newsroom/ourviews/teeth-staining-foods.
- ↑ Scully C (2013). Oral and maxillofacial medicine : the basis of diagnosis and treatment (3rd ed.). Edinburgh: Churchill Livingstone. pp. 39, 41. ISBN 9780702049484.
- ↑ 19.0 19.1 "Extrinsic stains and management: A new insight". https://www.researchgate.net/publication/265169002.
- ↑ 20.0 20.1 20.2 20.3 Oral and Maxillofacial Pathology. Elsevier Health Sciences. 11 June 2008. pp. 70–74. ISBN 978-1-4377-2197-3. https://books.google.com/books?id=5QIEAQAAQBAJ&pg=PA70.
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 21.6 21.7 Watts, A.; Addy, M. (2001-03-01). "Tooth discolouration and staining: a review of the literature". British Dental Journal 190 (6): 309–316. doi:10.1038/sj.bdj.4800959. ISSN 1476-5373. PMID 11325156.
- ↑ Seow, W. K. (1991). "Enamel hypoplasia in the primary dentition: a review.". ASDC Journal of Dentistry for Children 58 (6): 441–452. ISSN 1945-1954. PMID 1783694.
- ↑ Baik, Un-Bong; Kim, Hoon; Chae, Hwa-Sung; Myung, Ji-Yun; Chun, Youn-Sic (2017). "Teeth discoloration during orthodontic treatment". The Korean Journal of Orthodontics 47 (5): 334–339. doi:10.4041/kjod.2017.47.5.334. ISSN 2234-7518. PMID 28861395.
- ↑ Fejerskov, O.; Manji, F.; Baelum, V. (February 1990). "The Nature and Mechanisms of Dental Fluorosis in Man". Journal of Dental Research 69 (2_suppl): 692–700. doi:10.1177/00220345900690s135. ISSN 0022-0345. PMID 2179331.
- ↑ "Dental fluorosis: Exposure, prevention and management". https://www.researchgate.net/publication/23959996.
- ↑ 26.0 26.1 Sánchez, AR; Rogers RS, 3rd; Sheridan, PJ (October 2004). "Tetracycline and other tetracycline-derivative staining of the teeth and oral cavity.". International Journal of Dermatology 43 (10): 709–15. doi:10.1111/j.1365-4632.2004.02108.x. PMID 15485524.
- ↑ Good, ML; Hussey, DL (August 2003). "Minocycline: stain devil?". The British Journal of Dermatology 149 (2): 237–9. doi:10.1046/j.1365-2133.2003.05497.x. PMID 12932226.
- ↑ Ibsen OAC; Phelan JA (14 April 2014). Oral Pathology for the Dental Hygienist. Elsevier Health Sciences. p. 173. ISBN 978-0-323-29130-9. https://books.google.com/books?id=nsvsAwAAQBAJ&pg=PA173.
- ↑ R. R. Welbury; Brown, G. J. (August 2002). "The management of porphyria in dental practice". British Dental Journal 193 (3): 145–146. doi:10.1038/sj.bdj.4801507. ISSN 1476-5373. PMID 12213008.
- ↑ Dean, Laura (2005). Hemolytic disease of the newborn. National Center for Biotechnology Information (US). https://www.ncbi.nlm.nih.gov/books/NBK2266/.
- ↑ 31.0 31.1 Watts, A; Addy, M (2001-03-24). "Tooth discolouration and staining: Tooth discolouration and staining: a review of the literature". British Dental Journal 190 (6): 309–316. doi:10.1038/sj.bdj.4800959. ISSN 1476-5373. PMID 11325156.
- ↑ Pratibha, K.; Seenappa, T.; Ranganath, K. (2007). "Alkaptonuric ochronosis: Report of a case and brief review". Indian Journal of Clinical Biochemistry 22 (2): 158–161. doi:10.1007/BF02913337. PMID 23105706. PMC 3453790. http://medind.nic.in/iaf/t07/i2/iaft07i2p158.pdf.
- ↑ Delgado, E; Hernández-Cott, PL; Stewart, B; Collins, M; De Vizio, W (2007). "Tooth-whitening efficacy of custom tray-delivered 9% hydrogen peroxide and 20% carbamide peroxide during daytime use: A 14-day clinical trial". Puerto Rico Health Sciences Journal 26 (4): 367–72. PMID 18246965.
- ↑ He, LB; Shao, MY; Tan, K; Xu, X; Li, JY (August 2012). "The effects of light on bleaching and tooth sensitivity during in-office vital bleaching: a systematic review and meta-analysis.". Journal of Dentistry 40 (8): 644–53. doi:10.1016/j.jdent.2012.04.010. PMID 22525016.
- ↑ Baroudi, Kusai; Hassan, Nadia Aly (2015). "The effect of light-activation sources on tooth bleaching". Nigerian Medical Journal 55 (5): 363–8. doi:10.4103/0300-1652.140316. PMID 25298598. "The in-office bleaching treatment of vital teeth did not show improvement with the use of light activator sources for the purpose of accelerating the process of the bleaching gel and achieving better results.".
- ↑ "UTCAT2638, Found CAT view, CRITICALLY APPRAISED TOPICs". https://cats.uthscsa.edu/found_cats_view.php?id=2638&vSearch=.
- ↑ Sun, Grace (2000). "Lasers and Light Amplification in Dentistry". Dental Clinics of North America 44 (4).
- ↑ "Lodi Dentist Improves In-Office Whitening Treatment". Internet wire. http://go.galegroup.com.ez.library.latrobe.edu.au/ps/i.do?id=GALE%7CA433724644&v=2.1&u=latrobe&it=r&p=ITOF&sw=w.
- ↑ Bortolatto, J. F.; Pretel, H.; Floros, M. C.; Luizzi, A. C. C.; Dantas, A. a. R.; Fernandez, E.; Moncada, G.; Oliveira, O. B. de (2014-07-01). "Low Concentration H2O2/TiO_N in Office Bleaching A Randomized Clinical Trial". Journal of Dental Research 93 (7 suppl): 66S–71S. doi:10.1177/0022034514537466. ISSN 0022-0345. PMID 24868014.
- ↑ 40.0 40.1 SARRETT, DAVID C. (2002). "Tooth whitening today". The Journal of the American Dental Association 133 (11): 1535–1538. doi:10.14219/jada.archive.2002.0085. ISSN 0002-8177. PMID 12462698.
- ↑ 41.0 41.1 41.2 41.3 Eachempati, Prashanti; Kumbargere Nagraj, Sumanth; Kiran Kumar Krishanappa, Salian; Gupta, Puneet; Yaylali, Ibrahim Ethem (18 December 2018). "Home-based chemically-induced whitening (bleaching) of teeth in adults". The Cochrane Database of Systematic Reviews 2018 (12): CD006202. doi:10.1002/14651858.CD006202.pub2. ISSN 1469-493X. PMID 30562408.
- ↑ Carey, Clifton M. (June 2014). "Tooth Whitening: What We Now Know". The Journal of Evidence-based Dental Practice 14 Suppl: 70–76. doi:10.1016/j.jebdp.2014.02.006. ISSN 1532-3382. PMID 24929591.
- ↑ 43.0 43.1 43.2 43.3 43.4 Li, Yiming (2017). "Stain removal and whitening by baking soda dentifrice". The Journal of the American Dental Association 148 (11): S20–S26. doi:10.1016/j.adaj.2017.09.006. PMID 29056186.
- ↑ "Tooth Whitening Treatment". 18 January 2023. https://takehomesmile.com/tooth-whitening-treatment/.
- ↑ Carey, CM (2014). "Tooth Whitening: What we now know". J Evid Based Dent Pract 14 Suppl: 70–6. doi:10.1016/j.jebdp.2014.02.006. PMID 24929591.
- ↑ 46.0 46.1 46.2 46.3 Demarco, FF; Meireles, SS; Masotti, AS (2009). "Over-the-counter whitening agents: a concise review.". Brazilian Oral Research 23 (Suppl 1): 64–70. doi:10.1590/s1806-83242009000500010. PMID 19838560.
- ↑ "Tooth Whitening Treatments". http://www.ada.org/2993.aspx?currentTab=1#top.
- ↑ Wang, Y; Gao, J; Jiang, T; Liang, S; Zhou, Y; Matis, BA (August 2015). "Evaluation of the efficacy of potassium nitrate and sodium fluoride as desensitising agents during tooth bleaching treatment-A systematic review and meta-analysis.". Journal of Dentistry 43 (8): 913–23. doi:10.1016/j.jdent.2015.03.015. PMID 25913140.
- ↑ Li, Y (1996). "Biological properties of peroxide-containing tooth whiteners". Food and Chemical Toxicology 34 (9): 887–904. doi:10.1016/s0278-6915(96)00044-0. PMID 8972882.
- ↑ 50.0 50.1 Goldberg, Michel; Grootveld, Martin; Lynch, Edward (February 2010). "Undesirable and adverse effects of tooth-whitening products: a review". Clinical Oral Investigations 14 (1): 1–10. doi:10.1007/s00784-009-0302-4. ISSN 1436-3771. PMID 19543926.
- ↑ Kugel, G; Ferreira, S; Sharma, S; Barker, ML; Gerlach, RW (2009). "Clinical trial assessing light enhancement of in-office tooth whitening". Journal of Esthetic and Restorative Dentistry 21 (5): 336–47. doi:10.1111/j.1708-8240.2009.00287.x. PMID 19796303.
- ↑ Kugel, G; Ferreira, S (2005). "The art and science of tooth whitening". Journal of the Massachusetts Dental Society 53 (4): 34–7. PMID 15828604.
- ↑ Betke, H; Kahler, E; Reitz, A; Hartmann, G; Lennon, A; Attin, T (2006). "Influence of bleaching agents and desensitizing varnishes on the water content of dentin". Operative Dentistry 31 (5): 536–42. doi:10.2341/05-89. PMID 17024940.
- ↑ 54.0 54.1 54.2 Freedman GA (15 December 2011). "Chapter 14: Bleaching". Contemporary Esthetic Dentistry. Elsevier Health Sciences. ISBN 978-0-323-08823-7. https://books.google.com/books?id=JP82lK46EtEC&pg=PT1268.
- ↑ Azer, SS; Machado, C; Sanchez, E; Rashid, R (2009). "Effect of home bleaching systems on enamel nanohardness and elastic modulus". Journal of Dentistry 37 (3): 185–90. doi:10.1016/j.jdent.2008.11.005. PMID 19108942.
- ↑ Haywood, Van & Houck, V.M. & Heymann, H.O.. (1991). Nightguard vital bleaching: Effects of various solutions on enamel surface texture and color. Quintessence Int. 22. 775–782.
- ↑ 57.0 57.1 Rotstein, I; Mor, C; Arwaz, JR (1997). "Changes in surface levels of mercury, silver, tin, and copper of dental amalgam treated with carbamide peroxide and hydrogen peroxide in vitro". Oral Surg Oral Med Oral Pathol Oral Radiol Endod 83 (4): 506–509. doi:10.1016/s1079-2104(97)90154-2. PMID 9127386.
- ↑ Hummert, TW; Osborne, JW; Norling, BK; Cardenas, HL (1993). "Mercury in solution following exposure of various amalgams to carbamide peroxides". Am J Dent 6 (6): 305–309. PMID 7880482.
- ↑ 59.0 59.1 59.2 59.3 Attin, Thomas; Hannig, Christian; Wiegand, Annette; Attin, Rengin (November 2004). "Effect of bleaching on restorative materials and restorations--a systematic review". Dental Materials 20 (9): 852–861. doi:10.1016/j.dental.2004.04.002. ISSN 0109-5641. PMID 15451241.
- ↑ American Dental Association (November 2010). "Tooth Whitening/Bleaching:Treatment Considerations for Dentists and Their Patients". ADA Council on Scientific Affairs. http://www.ada.org/~/media/ADA/About%20the%20ADA/Files/whitening_bleaching_treatment_considrations_for_patients_and_dentists.ashx.
- ↑ Swift, EJ Jr; Perdigão, J (1998). "Effects of bleaching on teeth and restorations". Compend Contin Educ Dent 19 (8): 815–820. PMID 9918105.
- ↑ "Teeth Whitening" (in en). https://www.webmd.com/oral-health/teeth-whitening-and-bleaching.
- ↑ 63.0 63.1 Greenwall, Linda (2017-04-11), "Tooth Sensitivity Associated with Tooth Whitening", Tooth Whitening Techniques, CRC Press, pp. 295–306, doi:10.1201/9781315365503-20, ISBN 978-1-315-36550-3
- ↑ "Teeth whitening" (in en). 2018-04-26. https://www.nhs.uk/live-well/healthy-body/teeth-whitening/.
- ↑ Llena, Carmen; Villanueva, Alvaro; Mejias, Elena; Forner, Leopoldo (January 2020). "Bleaching efficacy of at home 16% carbamide peroxide. A long-term clinical follow-up study". Journal of Esthetic and Restorative Dentistry 32 (1): 12–18. doi:10.1111/jerd.12560. ISSN 1708-8240. PMID 31904193.
- ↑ 66.0 66.1 66.2 Dahl, J.E.; Pallesen, U. (2016-12-01). "Tooth Bleaching—a Critical Review of the Biological Aspects". Critical Reviews in Oral Biology & Medicine 14 (4): 292–304. doi:10.1177/154411130301400406. PMID 12907697.
- ↑ WORLD HEALTH ORGANIZATION INTERNATIONAL AGENCY FOR RESEARCH ON CANCER (1999). "IARC MONOGRAPHS ON THE EVALUATION OF CARCINOGENIC RISKS TO HUMANS: Re-evaluation of Some Organic Chemicals, Hydrazine and Hydrogen Peroxide". IARC 71: 1597. https://monographs.iarc.fr/ENG/Monographs/vol71/mono71.pdf.
- ↑ SCCNFP (1999). Scientific Committee on Cosmetic Products and Non-Food Products intended for Consumers. Hydrogen peroxide and hydrogen peroxide releasing substances in oral health products. SCCNFP/0058/98. Summary on http://europa.eu.int/comm/food/fs/sc/sccp/out83_en.html and http://europa.eu.int/comm/food/fs/sc/sccp/out89_en.html(read 2002.31.10)
- ↑ Lenkeit, Roberta Edwards (2018-10-23) (in en). High Heels and Bound Feet: And Other Essays on Everyday Anthropology, Second Edition. Waveland Press. pp. 72. ISBN 978-1-4786-3841-4. https://books.google.com/books?id=sapxDwAAQBAJ&dq=Teeth+whitening+ancient+Rome&pg=PA72.
- ↑ Perdigão, Jorge (2016-08-03) (in en). Tooth Whitening: An Evidence-Based Perspective. Springer. pp. 170. ISBN 978-3-319-38849-6. https://books.google.com/books?id=lB3KDAAAQBAJ&dq=Teeth+whitening+ancient+Rome&pg=PA170.
- ↑ Bonitz, Michael; Lopez, Jose; Becker, Kurt; Thomsen, Hauke (2014-04-09) (in en). Complex Plasmas: Scientific Challenges and Technological Opportunities. Springer Science & Business Media. pp. 465. ISBN 978-3-319-05437-7. https://books.google.com/books?id=EzW8BAAAQBAJ&dq=Teeth+whitening+ancient+Rome&pg=PA465.
- ↑ Vernon-Sparks, Lisa (2010-11-15). "A history of tooth-whitening" (in en-US). https://www.seattletimes.com/seattle-news/health/a-history-of-tooth-whitening/.
- ↑ 73.0 73.1 Freedman GA (15 December 2011). "Chapter 14: Bleaching". Contemporary Esthetic Dentistry. Elsevier Health Sciences. ISBN 978-0-323-08823-7. https://books.google.com/books?id=JP82lK46EtEC&pg=PT1268. [verification needed]
- ↑ 74.0 74.1 74.2 "Library Authentication - La Trobe University". https://login.ez.library.latrobe.edu.au/login?qurl=http%3a%2f%2fsearch.ebscohost.com%2flogin.aspx%3fdirect%3dtrue%26db%3dddh%26AN%3d55434991%26site%3dehost-live%26scope%3dsite.
- ↑ Krupp, Charla. (2008). How Not To Look Old. New York: Springboard Press, p.95.
- ↑ "Tooth Whitening". 8 Dec 2014. https://www.dentalprotection.org/uk/publications-resources/updates/updates/2014/12/08/tooth-whitening.
- ↑ 77.0 77.1 "Public Attitudes to Tooth Whitening Regulations (Presentation)". 12 December 2010. https://www.gdc-uk.org/docs/default-source/research/publicattitudestotoothwhitening.pdf?sfvrsn=993a40cf_2.
- ↑ Kothari, Siddharth; Gray, Andrew R.; Lyons, Karl; Tan, Xin Wen; Brunton, Paul A. (2019-05-01). "Vital bleaching and oral-health-related quality of life in adults: A systematic review and meta-analysis" (in en). Journal of Dentistry 84: 22–29. doi:10.1016/j.jdent.2019.03.007. ISSN 0300-5712. PMID 30904560.
 |