Medicine:Post-thrombotic syndrome
| Post-thrombotic syndrome | |
|---|---|
| Other names | postphlebitic syndrome, venous stress disorder |
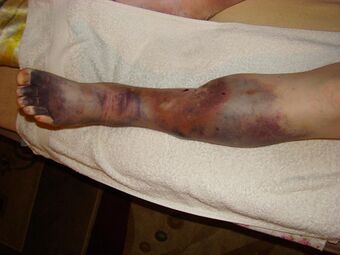 | |
| Person with post-thrombotic syndrome and leg ulcers | |
| Specialty | Hematology |
Post-thrombotic syndrome (PTS), also called postphlebitic syndrome and venous stress disorder is a medical condition that may occur as a long-term complication of deep vein thrombosis (DVT).
Signs and symptoms
Signs and symptoms of PTS in the leg may include:[1]
- pain (aching or cramping)
- heaviness
- itching or tingling
- swelling (edema)
- varicose veins
- brownish or reddish skin discoloration
- ulcer
These signs and symptoms may vary among patients and over time. With PTS, these symptoms typically are worse after walking or standing for long periods of time and improve with resting or elevating the leg.[1]
PTS lowers a person's quality of life after DVT, specifically with regards to physical and psychological symptoms and limitations in daily activities.[2][3][4]
Cause
Despite outgoing research, the cause of PTS is not entirely clear. Inflammation is thought to play a role[5][6] as well as damage to the venous valves from the thrombus itself. This valvular incompetence combined with persistent venous obstruction from thrombus increases the pressure in veins and capillaries. Venous hypertension induces a rupture of small superficial veins, subcutaneous hemorrhage[7] and an increase of tissue permeability. That is manifested by pain, swelling, discoloration, and even ulceration.[8]
Risk factors
The following factors increase the risk of developing PTS:[9][10][11][12][13][14][15]
- age > 65
- proximal DVT
- a second DVT in same leg as first DVT (recurrent ipsilateral DVT)
- persistent DVT symptoms 1 month after DVT diagnosis
- obesity
- poor quality of anticoagulation control (i.e. dose too low) during the first 3 months of treatment
Diagnosis
When physicians find a DVT in the clinical history of their patients, a postthrombotic syndrome is possible if the patients have suggestive symptoms. Ultrasonography for deep venous thrombosis must be performed to evaluate the situation: the degree of obstruction by clots, the location of these clots, and the detection of deep and/or superficial venous insufficiency.[16][17] Since signs and symptoms of DVT and PTS may be quite similar, a diagnosis of PTS should be delayed for 3–6 months after DVT diagnosis so an appropriate diagnosis can be made.[1]
Prevention
Prevention of PTS begins with prevention of initial and recurrent DVT. For people hospitalized at high-risk of DVT, prevention methods may include early ambulation, use of compression stockings or electrostimulation devices, and/or anticoagulant medications.[18] Elastic compression stockings may reduce the occurrence of PTS after clinically confirmed DVT.[19]
Increasingly, catheter-directed thrombolysis has been employed. This is a procedure in which a vascular interventionist will break up a clot using a variety of methods.[citation needed]
For people who have already had a single DVT event, the best way to prevent a second DVT is appropriate anticoagulation therapy.[20]
A second prevention approach may be weight loss for those who are overweight or obese. Increased weight can put more stress and pressure on leg veins, and can predispose patients to developing PTS.[13]
Treatment
Treatment options for PTS include proper leg elevation, compression therapy with elastic stockings, or electrostimulation devices, pharmacotherapy (pentoxifylline), herbal remedies (such as horse chestnut, rutosides), and wound care for leg ulcers.[1][21]
The benefits of compression bandages is unclear. They may be useful to treat edemas.[7]
Upper extremities
Patients with upper-extremity DVT may develop upper-extremity PTS, but the incidence is lower than that for lower-extremity PTS (15–25%).[22][23] No treatment or prevention methods are established, but patients with upper-extremity PTS may wear a compression sleeve for persistent symptoms.[20]
Epidemiology
PTS can affect 23 to 60% of patients in the two years following DVT of the leg. Of those, 10% may go on to develop severe PTS, involving venous ulcers.[24]
Society and culture
Treatment of PTS adds significantly to the cost of treating DVT. The annual health care cost of PTS in the United States has been estimated at $200 million, with costs over $3800 per patient in the first year alone, and increasing with disease severity.[24][25] PTS also causes lost work productivity: people with severe PTS and venous ulcers lose up to 2 work days per year.[26]
Research directions
The field of PTS still holds many unanswered questions that are important targets for more research. Those include:[citation needed]
- Fully defining the pathophysiology of PTS, including the role of inflammation and residual thrombus after completion of an appropriate duration of anticoagulant therapy
- Developing a PTS risk prediction model
- Role of thrombolytic ("clot-busting") drugs in PTS prevention
- Defining the true efficacy of elastic compression stockings for PTS prevention (and if effective, elucidating the minimum compression strength necessary and the optimal timing and duration of compression therapy)
- Whether PTS prevention methods are necessary for patients with asymptomatic, or distal DVT
- Additional treatment options for PTS with demonstrated safety and efficacy (compression and pharmacologic therapies)
References
- ↑ 1.0 1.1 1.2 1.3 "How I treat postthrombotic syndrome". Blood 114 (21): 4624–31. November 2009. doi:10.1182/blood-2009-07-199174. PMID 19741190.
- ↑ Kahn SR, Hirsch A, Shrier I. Effect of postthrombotic syndrome on health-related quality of life after deep venous thrombosis" Arch Intern Med 2002;162:1144-8.
- ↑ "The influence of venous thromboembolism on quality of life and severity of chronic venous disease". Journal of Thrombosis and Haemostasis 2 (12): 2146–51. December 2004. doi:10.1111/j.1538-7836.2004.00957.x. PMID 15613019.
- ↑ "Determinants of health-related quality of life during the 2 years following deep vein thrombosis". Journal of Thrombosis and Haemostasis 6 (7): 1105–12. July 2008. doi:10.1111/j.1538-7836.2008.03002.x. PMID 18466316.
- ↑ "Levels of inflammatory markers and the development of the post-thrombotic syndrome". Thrombosis and Haemostasis 101 (3): 505–12. March 2009. doi:10.1160/TH08-08-0511. PMID 19277412.
- ↑ "Inflammation in deep vein thrombosis and the development of post-thrombotic syndrome: a prospective study". Journal of Thrombosis and Haemostasis 7 (4): 582–7. April 2009. doi:10.1111/j.1538-7836.2009.03286.x. PMID 19175493.
- ↑ 7.0 7.1 "The post-thrombotic syndrome - a condition to prevent". Dermatology Online Journal 14 (3): 13. March 2008. PMID 18627714.
- ↑ "Valvular dysfunction and venous obstruction in the post-thrombotic syndrome". Thrombosis Research 123 Suppl 4 (Suppl 4): S62-5. 2009. doi:10.1016/s0049-3848(09)70146-x. PMID 19303507.
- ↑ "Risk factors for post-thrombotic syndrome in patients with a first deep venous thrombosis". Journal of Thrombosis and Haemostasis 6 (12): 2075–81. December 2008. doi:10.1111/j.1538-7836.2008.03180.x. PMID 18983518.
- ↑ "The long-term clinical course of acute deep venous thrombosis". Annals of Internal Medicine 125 (1): 1–7. July 1996. doi:10.7326/0003-4819-125-1-199607010-00001. PMID 8644983.
- ↑ "Long-term prognosis after deep venous thrombosis". Current Opinion in Hematology 15 (5): 494–8. September 2008. doi:10.1097/moh.0b013e32830abde2. PMID 18695373.
- ↑ "Predictors of the post-thrombotic syndrome during long-term treatment of proximal deep vein thrombosis". Journal of Thrombosis and Haemostasis 3 (4): 718–23. April 2005. doi:10.1111/j.1538-7836.2005.01216.x. PMID 15733061.
- ↑ 13.0 13.1 "Body mass index is associated with the development of the post-thrombotic syndrome". Thrombosis and Haemostasis 89 (2): 305–9. February 2003. doi:10.1055/s-0037-1613447. PMID 12574811.
- ↑ "Relation between quality of anticoagulant treatment and the development of the postthrombotic syndrome". Journal of Thrombosis and Haemostasis 3 (5): 939–42. May 2005. doi:10.1111/j.1538-7836.2005.01333.x. PMID 15869588.
- ↑ "Relationship between deep venous thrombosis and the postthrombotic syndrome". Archives of Internal Medicine 164 (1): 17–26. January 2004. doi:10.1001/archinte.164.1.17. PMID 14718318.
- ↑ "The natural history of calf vein thrombosis: lysis of thrombi and development of reflux". Journal of Vascular Surgery 28 (1): 67–73; discussion 73–4. July 1998. doi:10.1016/s0741-5214(98)70201-0. PMID 9685132.
- ↑ "Definition of post-thrombotic syndrome of the leg for use in clinical investigations: a recommendation for standardization". Journal of Thrombosis and Haemostasis 7 (5): 879–83. May 2009. doi:10.1111/j.1538-7836.2009.03294.x. PMID 19175497.
- ↑ "Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition)". Chest 133 (6 Suppl): 381S–453S. June 2008. doi:10.1378/chest.08-0656. PMID 18574271.
- ↑ Cochrane Vascular Group, ed (September 2017). "Compression therapy for prevention of post-thrombotic syndrome". The Cochrane Database of Systematic Reviews 9: CD004174. doi:10.1002/14651858.CD004174.pub3. PMID 28950030.
- ↑ 20.0 20.1 Kearon C, Kahn SR, Agnelli G, Goldhaber S, Raskob GE, Comerota AJ. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition)" Chest 2008;133:454S-545S.
- ↑ "Contemporary issues in the prevention and management of postthrombotic syndrome". The Annals of Pharmacotherapy 43 (11): 1824–35. November 2009. doi:10.1345/aph.1m185. PMID 19737994.
- ↑ "The post-thrombotic syndrome after upper extremity deep venous thrombosis in adults: a systematic review". Thrombosis Research 117 (6): 609–14. 2006. doi:10.1016/j.thromres.2005.05.029. PMID 16002126.
- ↑ "The long term clinical course of acute deep vein thrombosis of the arm: prospective cohort study". BMJ 329 (7464): 484–5. August 2004. doi:10.1136/bmj.38167.684444.3a. PMID 15256419.
- ↑ 24.0 24.1 "Incidence and cost burden of post-thrombotic syndrome". Journal of Thrombosis and Thrombolysis 28 (4): 465–76. November 2009. doi:10.1007/s11239-009-0309-3. PMID 19224134.
- ↑ "Economic burden of long-term complications of deep vein thrombosis after total hip replacement surgery in the United States". Value in Health 6 (1): 59–74. 2003. doi:10.1046/j.1524-4733.2003.00204.x. PMID 12535239.
- ↑ "Cost of long-term complications of deep venous thrombosis of the lower extremities: an analysis of a defined patient population in Sweden". Annals of Internal Medicine 126 (6): 454–7. March 1997. doi:10.7326/0003-4819-126-6-199703150-00006. PMID 9072931.
External links
| Classification |
|---|
 |

