Medicine:Meninges
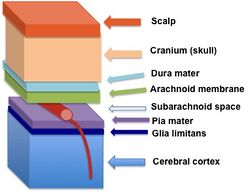
In anatomy, the meninges (/məˈnɪndʒiːz/;[1][2] sg. meninx /ˈmiːnɪŋks, ˈmɛnɪŋks/;[3] from grc μῆνινξ (mêninx) 'membrane')[4] are protective membranes that cover the brain and spinal cord. In mammals, three meninges have been clearly identified: the dura mater, the arachnoid mater, and the pia mater. Each layer has its own molecularly distinct type of fibroblasts.[5] The meninges act as a physical and immunological protective barrier for the brain and spinal cord, shielding the central nervous system (CNS) from injury.[6] They anchor and support the tissues of the CNS, and provide containment for cerebrospinal fluid (CSF) and the arteries and veins that supply blood to the brain and spinal cord.[7]
The dura mater surrounds the arachnoid mater and supports the dural sinuses, which carry blood from the brain to the heart.[8] The area between the arachnoid and pia mater is known as the subarachnoid space. It contains cerebrospinal fluid. The arachnoid and pia maters produce prostaglandin D2 synthase, a major cerebrospinal fluid protein.[9] The arachnoid mater provides a restrictive permeability barrier between the cerebrospinal fluid in the subarachnoid space and the circulation of blood in the dura.[5] The pia mater is a thin sheet of connective tissue that interfaces with the glial limitans superficialis.[6]
Structures
Dura mater
The dura mater (Latin: tough mother),[10][lower-alpha 1] is a durable, thick fibrous membrane that attaches to the inside of the skull and covers the brain and vertebrae. Its dense fibrous tissue is formed from an interlay of collagen fibers, elastin, and fibroblasts in an unformed extracellular matrix.[11] The dura mater is itself a two layered membrane: an outer endosteal (periosteal) layer lies closest to the skull, and an inner (meningeal or dura mater proper) layer lies closer to the brain.[12][6] These layers separate to surround the Dural venous sinuses. Sensory and autonomic nerves innervate the dura, and are dense near its blood vessels.[6] The dura's inner surface is covered by flattened fibrocytes which are adhered to by the outer cells of the arachnoid mater.[13] The dura mater surrounds the arachnoid mater and supports the dural sinuses which carry blood from the brain to the heart.[8]
The dura mater folds inwards upon itself to form four areas of infolding called dural reflections:[14][15]
- Falx cerebri: This sickle-shaped fold is the largest of the dural reflections. It separates the two cerebral hemispheres, and is anchored to the crista galli of the ethmoid bone and the internal occipital protuberance.[14]
- Tentorium cerebelli. The second largest fold is also crescent-shaped. It separates the occipital lobes of the cerebrum from the cerebellum. The falx cerebri attaches to it to form the roof of the posterior cranial fossa, which gives it a tentlike appearance.[14][16]
- Falx cerebelli: This vertical infolding is located inferior to the tentorium cerebelli. It partially separates the cerebellar hemispheres.[14]
- Diaphragma sellae: The smallest of the infoldings, it forms a roof over the sella turcica and seals the pituitary gland from the subarachnoid space.[14][17]
Arachnoid mater
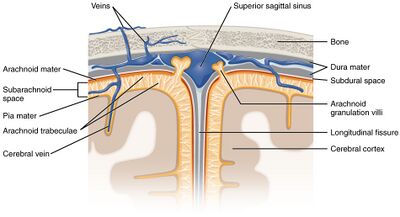
The arachnoid mater, or arachnoid membrane, is the middle element of the meninges. Thin and transparent, its name reflects its resemblance to a spider web. Its fibrous tissue cushions the central nervous system. Like the pia mater, it has an outer layer of tightly packed flat cells, forming the arachnoid barrier.[18]
The arachnoid is loosely fitting and does not closely follow the ridges and grooves on the surface of the brain. A large number of fine filaments called arachnoid trabeculae pass from the arachnoid through the subarachnoid space to blend with the tissue of the pia mater.[19] The arachnoid barrier creates a restrictive permeability barrier between the cerebrospinal fluid in the subarachnoid space and the blood circulation in the dura.[5]
The arachnoid barrier layer is characterized by a distinct continuous basal lamina on its inner surface toward the innermost collagenous portion of the arachnoid reticular layer.[20]
Pia mater
The pia mater (Latin: tender mother)[21] is a very delicate membrane. It is the meningeal envelope that firmly adheres to the surfaces of the brain and spinal cord,[6] following all of the brain's contours (gyri and sulci).[22] It is a very thin sheet of connective tissue that interfaces with the glial limitans superficialis but lacks capillaries itself.[6]
Subarachnoidal lymphatic-like membrane
Leptomeninges
The arachnoid and pia mater are sometimes together called the leptomeninges,[23] literally "thin meninges" (Greek: λεπτός "leptos"—"thin"). Acute meningococcal meningitis can lead to an exudate within the leptomeninges along the surface of the brain.[24] Because the arachnoid is connected to the pia by cobweb-like strands, it is structurally continuous with the pia, hence the name pia-arachnoid or leptomeninges. They are responsible for the production of beta-trace protein (prostaglandin D2 synthase), a major cerebrospinal fluid protein.[9]
Subarachnoid space
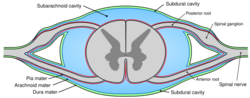
The subarachnoid space is the space that normally exists between the arachnoid and the pia mater. It is filled with cerebrospinal fluid and continues down the spinal cord. Spaces are formed from openings at different points along the subarachnoid space; these are the subarachnoid cisterns, which are filled with cerebrospinal fluid.[25]
The dura mater is attached to the skull,[12] whereas in the spinal cord, the dura mater is separated from the vertebrae by a space called the epidural space, which contains fat and blood vessels. The arachnoid is attached to the dura mater, while the pia mater is attached to the central nervous system tissue. If the dura mater and the arachnoid become separated due to injury or illness, the space between them is known as the subdural space.[26][27] There is another potential space, the subpial space, between the pia mater and the glia limitans.[28]
Clinical significance
Intracranial hemorrhage
Three types of intracranial hemorrhage can involve the meninges: epidural, subdural, and subarachnoid.[29]
- A subarachnoid hemorrhage is acute bleeding under the arachnoid; it may occur spontaneously or as a result of trauma.[30][29]
- A subdural hematoma (SDH) is an extracerebral collection of blood located in the potential space that can separate arachnoid from the dura mater. The origin is usually venous, caused by injury to the bridging veins that connect the dura mater and the arachnoid. Once these are torn, blood leaks into this area. SDHs occur in about 30% cases of severe head trauma.[29]
- An epidural hematoma (EDH) is a collection of blood between the skull and the dura mater, underlying a bare bone surface. It is often associated with skull fracture. EDH may be arterial (caused by injury of a meningeal artery) or venous (related to damage to of a dural venous sinus or bleeding from diploic veins).[29]
Meningioma
Meningiomas are the most common type of primary brain tumors to occur in adults. They are thought to arise from meningothelial arachnoid cells in the meninges. Most commonly they attach firmly to the inner surface of the dura and are well-circumscribed; but some tumors may show brain invasion.[31] More rarely, leptomeningeal cancers may metastasize from tumors elsewhere in the body to the cerebrospinal fluid and leptomeninges.[32]
Meningitis
Other medical conditions that affect the meninges include meningitis, which usually arises from a viral, bacterial, or fungal infection.[33][34]
Migraine
Migraine is a complex neurovascular pain disorder involving blood vessels, neurons, and cerebrospinal fluid within the meninges. The trigeminal nerve, located within the dura mater, carries sensory information about pain, touch, heat and cold from the face to the brain. The hypothalamus receives input from the trigeminal nerve and can modulate trigeminal nerve activity.[35][36][37] Migraine patients appear to experience impairments in cortical habituation, a process which would normally decrease cortical responses to repetitive sensory stimuli.[38][39]
Initiation of a migraine attack may begin with disruption in the hypothalamus and limbic system.[35][36][37] Gradually increasing hypothalamic activity has been observed in the period leading up to a migraine attack, followed by a disruption or collapse of hypothalamic connectivity to the limbic system during an attack.[40] Disruption of the connection between the hypothalamus and limbic system may increase activity in the pain pathway from the trigeminal nerve to the brain, resulting in a migraine attack.[35][36][37]
The meninges, particularly the dura mater, are rich in pain-sensitive nerve endings. Sensory information travels along trigeminal nerve fibers to cell bodies located within the trigeminal ganglion (TG). Axons of the trigeminal ganglion neurons enter the brainstem and travel to the trigeminal nucleus caudalis (TNC).[41][37][5]
The activity of calcitonin gene-related peptide (CGRP) in the meninges is linked to migraine.[6] CGRP is released from both the trigeminal ganglion (TG) and the trigeminal nucleus caudalis (TNC) in response to trigeminal nerve activation. CGRP activates receptors on meningeal blood vessels, causing dilation and changes in blood flow. CGRP also activates specialized nerve endings on the dura mater (nociceptors) that transmit pain signals from the dura to the central nervous system. Increased neuronal activity in the trigeminal pain pathway reaches higher cortical pain regions via the brainstem, midbrain and thalamus.[35][37]
Stimulation of the trigeminal nerve may result in release of neuropeptides such as CGRP, vasodilation of cerebral and dural blood vessels, neurogenic inflammation, and the transmission of pain signals via nerves in the meninges.[6] Cerebrospinal fluid may also play a role in migraine by transferring signals released from the brain to overlying pain-sensitive meningeal tissues, including dura mater.[6]
Other animals
In fish, there is a single membrane known as the primitive meninx.[42] Amphibians and reptiles have two meninges, and birds and mammals have three.[42] Mammals (as higher vertebrates) retain the dura mater, and the secondary meninx divides into the arachnoid and pia mater.[43]
History
The first known reference to the dura appears in Egypt, in Case 6 of the Edwin Smith Papyrus. Hippocrates described the dura in his monograph "On Injuries of the Head" and insisted that care should be taken to keep it intact and clean.[44] Celsus agreed, and described a method of treatment for depressed fractures.[45] Galen was the first to describe the pia mater in humans in the second century AD.[46]

The arachnoid layer was first described by Dutch physician Gerardus Blasius in 1664.[46] In 1695, Humphrey Ridley first described the subarachnoid cisterns. He also contributed to the understanding of the blood-brain barrier, and accurately described the fifth cranial nerve ganglion with its branches.[47] In 1699, Frederick Ruysch confirmed that the arachnoid mater formed a complete layer that surrounded the brain. Its current name is based on his description of its spiderlike morphology.[48] Arachnoid granulations were first described by Italian physician Antonio Pacchioni who published his Dissertatio Epistolaris de Glandulis Conglobatis Durae Meningis Humanae in 1705.[49]
In seven articles from 1899 to 1902, Italian anatomist Giuseppe Sterzi described comparative studies on the meninges from the lancelet to the human. He showed that the spinal meninges were very simple in adult lower vertebrates and in the early development of more advanced vertebrates.[50]
See also
- Cranial cavity
Notes
- ↑ Also rarely called meninx fibrosa or pachymeninx
References
- ↑ "meninges". https://oxfordlearnersdictionaries.com/definition/english/meninges.
- ↑ "Meninges". Merriam-Webster Dictionary. https://www.merriam-webster.com/dictionary/meninges. Retrieved 2012-07-28.
- ↑ "Meninx". Merriam-Webster Dictionary. https://www.merriam-webster.com/dictionary/meninx. Retrieved 2012-07-28.
- ↑ μῆνιγξ. Liddell, Henry George; Scott, Robert; A Greek–English Lexicon at the Perseus Project
- ↑ 5.0 5.1 5.2 5.3 Betsholtz, C; Engelhardt, B; Koh, GY; McDonald, DM; Proulx, ST; Siegenthaler, J (November 2024). "Advances and controversies in meningeal biology.". Nature Neuroscience 27 (11): 2056–2072. doi:10.1038/s41593-024-01701-8. PMID 39333784. PMC 11862877. https://escholarship.org/uc/item/7sx757mx.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 Levy, D; Moskowitz, MA (10 July 2023). "Meningeal Mechanisms and the Migraine Connection". Annual Review of Neuroscience 46: 39–58. doi:10.1146/annurev-neuro-080422-105509. ISSN 0147-006X. PMID 36913712.
- ↑ Castillero Mimenza, Oscar (January 2017). "Meninges: anatomía, partes y funciones en el cerebro". https://psicologiaymente.com/neurociencias/meninges.
- ↑ 8.0 8.1 Dasgupta, K; Jeong, J (2019). "Developmental biology of the meninges.". Genesis 57 (5). doi:10.1002/dvg.23288. PMID 30801905.
- ↑ 9.0 9.1 Yamashima, Tetsumori; Sakuda, Kazushige; Tohma, Yasuo; Yamashita, Junkoh; Oda, Hiroshi; Irikura, Daisuke; Eguchi, Naomi; Beuckmann, Carsten T. et al. (1 April 1997). "Prostaglandin D Synthase (β-Trace) in Human Arachnoid and Meningioma Cells: Roles as a Cell Marker or in Cerebrospinal Fluid Absorption, Tumorigenesis, and Calcification Process" (in en). Journal of Neuroscience 17 (7): 2376–2382. doi:10.1523/JNEUROSCI.17-07-02376.1997. PMID 9065498.
- ↑ "Definition of dura mater". Definition of dura mater. https://www.merriam-webster.com/dictionary/dura+mater. Retrieved 22 June 2022.
- ↑ Niestrawska, JA; Rodewald, M; Schultz, C; Quansah, E; Meyer-Zedler, T; Schmitt, M; Popp, J; Tomasec, I et al. (2023-10-15). "Morpho-mechanical mapping of human dura mater microstructure". Acta Biomaterialia 170: 86–96. doi:10.1016/j.actbio.2023.08.024. ISSN 1742-7061. PMID 37598794. https://www.sciencedirect.com/science/article/pii/S1742706123004865.
- ↑ 12.0 12.1 Suh, DC (March 2020). "Where Did the Dura Mater Come from?". Neurointervention 15 (1): 2–3. doi:10.5469/neuroint.2020.00045. PMID 32093449.
- ↑ Figueiredo, Marxa L.; Turek, John J. (2025-04-09) (in en). Dellmann's Textbook of Veterinary Histology. John Wiley & Sons. ISBN 978-1-394-19670-8. https://books.google.com/books?id=7gVVEQAAQBAJ&dq=inner+surface+of+the+dura+mater+inner+surface+is+covered+by+flattened+cells&pg=PA99.
- ↑ 14.0 14.1 14.2 14.3 14.4 Agur, Anne M. R.; Dalley, Arthur F. (2022-12-29) (in en). Moore's Essential Clinical Anatomy. Lippincott Williams & Wilkins. ISBN 978-1-9751-7425-5. https://books.google.com/books?id=HJWkEAAAQBAJ&dq=dura+has+four+areas+of+infolding:+Falx++cerebri+-StatPearls&pg=PT1071.
- ↑ Andreatta, Richard D. (2022-10-13) (in en). Neuroscience Fundamentals for Communication Sciences and Disorders, Second Edition. Plural Publishing. ISBN 978-1-63550-360-9. https://books.google.com/books?id=XfqUEAAAQBAJ&dq=arachnoid+loosley+fitting+sac&pg=PA259.
- ↑ Rai, R; Iwanaga, J; Shokouhi, G; Oskouian, RJ; Tubbs, RS (31 July 2018). "The Tentorium Cerebelli: A Comprehensive Review Including Its Anatomy, Embryology, and Surgical Techniques.". Cureus 10 (7). doi:10.7759/cureus.3079. PMID 30305987.
- ↑ Rasmussen, MK; Mestre, H; Nedergaard, M (1 April 2022). "Fluid transport in the brain.". Physiological Reviews 102 (2): 1025–1151. doi:10.1152/physrev.00031.2020. PMID 33949874.
- ↑ Abbott, NJ; Patabendige, AA; Dolman, DE; Yusof, SR; Begley, DJ (January 2010). "Structure and function of the blood-brain barrier.". Neurobiology of Disease 37 (1): 13–25. doi:10.1016/j.nbd.2009.07.030. PMID 19664713.
- ↑ Schröder, Hannsjörg; Vos, Rob A. I. de; Huggenberger, Stefan; Müller-Thomsen, Lennart; Rozemuller, Annemieke; Hedayat, Farman; Moser, Natasha (8 August 2023) (in en). The Human Brainstem: Anatomy and Pathology. Springer Nature. p. 71. ISBN 978-3-030-89980-6. https://books.google.com/books?id=fBfQEAAAQBAJ&dq=arachnoid+trabeculae+pass+from+the+arachnoid+through+the+subarachnoid+space+to+blend+with+the+tissue+of+the+pia+mater.&pg=PA71.
- ↑ Izadi, N; Solár, P; Hašanová, K; Zamani, A; Akbar, MS; Mrázová, K; Bartošík, M; Kazda, T et al. (8 January 2025). "Breaking boundaries: role of the brain barriers in metastatic process.". Fluids and Barriers of the CNS 22 (1): 3. doi:10.1186/s12987-025-00618-z. ISSN 2045-8118. PMID 39780275.
- ↑ "Definition of pia mater". Definition of pia mater. https://www.merriam-webster.com/dictionary/pia+mater. Retrieved 27 November 2015.
- ↑ Barichello, Tatiana; Dal-Pizzol, Felipe; Hasbun, Rodrigo (2024-11-30) (in en). Neurobiology of Infectious Diseases. Elsevier. p. 13. ISBN 978-0-443-19131-2. https://books.google.com/books?id=PE7VEAAAQBAJ&dq=gyri+pia+mater&pg=PA13.
- ↑ "leptomeninges". https://en.oxforddictionaries.com/definition/leptomeninges.
- ↑ Kumar, Vinay (2015). Robbins and Cotran Pathologic Mechanisms of Disease (9th ed.). Philadelphia: Elsevier Saunders. p. 1273. OCLC 892583347. "In acute meningitis, an exudate is evident within the leptomeninges over the surface of the brain (Fig. 28-21)."
- ↑ Hladky, SB; Barrand, MA (17 July 2024). "Regulation of brain fluid volumes and pressures: basic principles, intracranial hypertension, ventriculomegaly and hydrocephalus.". Fluids and Barriers of the CNS 21 (1): 57. doi:10.1186/s12987-024-00532-w. PMID 39020364.
- ↑ Carstens, Michael H. (27 September 2023) (in en). The Embryologic Basis of Craniofacial Structure: Developmental Anatomy, Evolutionary Design, and Clinical Applications. Springer Nature. p. 1040. ISBN 978-3-031-15636-6. https://books.google.com/books?id=w_XZEAAAQBAJ&dq=meninges+Giuseppe+Sterzi&pg=PA1040.
- ↑ Macpherson, D; Quondamatteo, F; Broom, M (May 2022). "Update on applied epidural anatomy.". BJA Education 22 (5): 182–189. doi:10.1016/j.bjae.2021.12.006. PMID 35496647.
- ↑ Server, A; Latysheva, A; Nedregaard, B; Rønnestad, AE; Marthinsen, PB (April 2025). "Neonatal subpial hemorrhage: clinical presentation, neuroimaging findings and outcome.". Neuroradiology 67 (4): 1071–1080. doi:10.1007/s00234-025-03589-y. PMID 40095005.
- ↑ 29.0 29.1 29.2 29.3 Parizel, Paul M.; Philips, C. Douglas (2020). "Traumatic Neuroemergency: Imaging Patients with Traumatic Brain Injury—An Introduction" (in en). Diseases of the Brain, Head and Neck, Spine 2020–2023. Springer International Publishing. pp. 77–92. doi:10.1007/978-3-030-38490-6_7. ISBN 978-3-030-38489-0. https://www.ncbi.nlm.nih.gov/books/NBK554351/.
- ↑ "Subarachnoid haemorrhage". Lancet 369 (9558): 306–18. 2007. doi:10.1016/S0140-6736(07)60153-6. PMID 17258671.
- ↑ Szulzewsky, F; Thirimanne, HN; Holland, EC (2024). "Meningioma: current updates on genetics, classification, and mouse modeling.". Upsala Journal of Medical Sciences 129. doi:10.48101/ujms.v129.10579. PMID 38571886.
- ↑ Nguyen, A; Nguyen, A; Dada, OT; Desai, PD; Ricci, JC; Godbole, NB; Pierre, K; Lucke-Wold, B (19 June 2023). "Leptomeningeal Metastasis: A Review of the Pathophysiology, Diagnostic Methodology, and Therapeutic Landscape.". Current Oncology 30 (6): 5906–5931. doi:10.3390/curroncol30060442. PMID 37366925.
- ↑ Garber, B; Glauser, J (1 September 2024). "Viral Meningitis and Encephalitis Update" (in en). Current Emergency and Hospital Medicine Reports 12 (3): 95–102. doi:10.1007/s40138-024-00294-7. ISSN 2167-4884.
- ↑ Gundamraj, V; Hasbun, R (1 June 2023). "Viral meningitis and encephalitis: an update.". Current Opinion in Infectious Diseases 36 (3): 177–185. doi:10.1097/QCO.0000000000000922. PMID 37093042.
- ↑ 35.0 35.1 35.2 35.3 Biscetti, L; Cresta, E; Cupini, LM; Calabresi, P; Sarchielli, P (1 May 2023). "The putative role of neuroinflammation in the complex pathophysiology of migraine: From bench to bedside". Neurobiology of Disease 180. doi:10.1016/j.nbd.2023.106072. ISSN 0969-9961. PMID 36907522. https://www.sciencedirect.com/science/article/pii/S0969996123000864.
- ↑ 36.0 36.1 36.2 Terrier, LM; Hadjikhani, N; Velut, S; Magnain, C; Amelot, A; Bernard, F; Zöllei, L; Destrieux, C (July 2021). "The trigeminal system: The meningovascular complex- A review.". Journal of Anatomy 239 (1): 1–11. doi:10.1111/joa.13413. PMID 33604906.
- ↑ 37.0 37.1 37.2 37.3 37.4 Edvinsson, JCA; Viganò, A; Alekseeva, A; Alieva, E; Arruda, R; De Luca, C; D'Ettore, N; Frattale, I et al. (5 June 2020). "The fifth cranial nerve in headaches.". The Journal of Headache and Pain 21 (1): 65. doi:10.1186/s10194-020-01134-1. PMID 32503421.
- ↑ "Neuromodulation in migraine". Handbook of Clinical Neurology, Vol. 199 (3rd series) Migraine Management. Elsevier. 1 January 2024. pp. 179–200. ISBN 978-0-12-823357-3.
- ↑ Ning, J; Zhang, Y; Wang, Y; Liu, C; Cheng, Y; Zhu, M; Dong, M; Yang, X et al. (2023). "Exploring the cortical habituation in migraine patients based on contingent negative variation.". Frontiers in Neurology 14. doi:10.3389/fneur.2023.1226554. PMID 37719755.
- ↑ Stankewitz, A; Keidel, L; Rehm, M; Irving, S; Kaczmarz, S; Preibisch, C; Witkovsky, V; Zimmer, C et al. (2021). "Migraine attacks as a result of hypothalamic loss of control.". NeuroImage. Clinical 32. doi:10.1016/j.nicl.2021.102784. PMID 34425551.
- ↑ Price, S; Daly, DT (2025). Neuroanatomy, Trigeminal Nucleus. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK539823/.
- ↑ 42.0 42.1 Ostrander, Gary (12 September 2000) (in en). The Laboratory Fish. Elsevier. ISBN 978-0-12-529650-2. https://books.google.com/books?id=Hp4YSFiSD0IC&q=fish+meninges&pg=PT135.
- ↑ Kardong, Kenneth V. (1995). Vertebrates: Comparative Anatomy, Function, Evolution. Dubuque, Iowa: Wm. C. Brown Publishers.. p. 539. ISBN 0-697-21991-7.
- ↑ Ganz, JC (2024). "The meninges". Cranial Surgery - Part 2. Progress in Brain Research. 285. pp. 137–147. doi:10.1016/bs.pbr.2024.02.020. ISBN 978-0-443-31718-7.
- ↑ Talamonti, G; D'Aliberti, G; Cenzato, M (January 2020). "Aulus Cornelius Celsus and the Head Injuries.". World Neurosurgery 133: 127–134. doi:10.1016/j.wneu.2019.09.119. PMID 31568909.
- ↑ 46.0 46.1 Lu, S; Brusic, A; Gaillard, F (February 2022). "Arachnoid Membranes: Crawling Back into Radiologic Consciousness.". AJNR. American Journal of Neuroradiology 43 (2): 167–175. doi:10.3174/ajnr.A7309. PMID 34711549.
- ↑ Thakur, JD; Sonig, A; Chittiboina, P; Khan, IS; Wadhwa, R; Nanda, A (August 2012). "Humphrey Ridley (1653-1708): 17th century evolution in neuroanatomy and selective cerebrovascular injections for cadaver dissection.". Neurosurgical Focus 33 (2): E3. doi:10.3171/2012.6.FOCUS12139. PMID 22853834.
- ↑ Mortazavi, Martin M.; Quadri, Syed A.; Khan, Muhammad A.; Gustin, Aaron; Suriya, Sajid S.; Hassanzadeh, Tania; Fahimdanesh, Kian M.; Adl, Farzad H. et al. (2018-03-01). "Subarachnoid Trabeculae: A Comprehensive Review of Their Embryology, Histology, Morphology, and Surgical Significance". World Neurosurgery 111: 279–290. doi:10.1016/j.wneu.2017.12.041. ISSN 1878-8750. PMID 29269062. https://www.sciencedirect.com/science/article/pii/S1878875017321575.
- ↑ Artico, M; Galassi, FM; Carubbi, C; Vitale, M; Cofone, L (1 July 2025). "Antonio Pacchioni: italian physician and anatomist" (in English). The Lancet Neurology 24 (7): 567. doi:10.1016/S1474-4422(25)00200-5. ISSN 1474-4422. PMID 40541203. https://www.thelancet.com/journals/laneur/article/PIIS1474-4422(25)00200-5/abstract?rss=yes.
- ↑ Riva, Alessandro; Orrù, Beniamino; Riva, Francesca Testa (2000). "Giuseppe Sterzi (1876–1919) of the University of Cagliari: A brilliant neuroanatomist and medical historian" (in en). The Anatomical Record 261 (3): 105–110. doi:10.1002/1097-0185(20000615)261:3<105::AID-AR5>3.0.CO;2-H. ISSN 1097-0185. PMID 10867628. https://anatomypubs.onlinelibrary.wiley.com/doi/full/10.1002/1097-0185%2820000615%29261%3A3%3C105%3A%3AAID-AR5%3E3.0.CO%3B2-H.
External links
Lua error: not enough memory. Template:Meninges Lua error: not enough memory.
Lua error: Internal error: The interpreter exited with status 1.