Medicine:Vein of Galen aneurysmal malformations
Vein of Galen aneurysmal malformations (VGAMs) and Vein of Galen aneurysmal dilations (VGADs) are the most frequent arteriovenous malformations in infants and fetuses.[1][2] A VGAM consists of a tangled mass of dilated vessels supplied by an enlarged artery.[3] The malformation increases greatly in size with age, although the mechanism of the increase is unknown.[3] Dilation of the great cerebral vein of Galen is a secondary result of the force of arterial blood either directly from an artery via an arteriovenous fistula or by way of a tributary vein that receives the blood directly from an artery.[1][3] There is usually a venous anomaly downstream from the draining vein that, together with the high blood flow into the great cerebral vein of Galen causes its dilation.[4] The right sided cardiac chambers and pulmonary arteries also develop mild to severe dilation.[5]
Signs and symptoms
Malformations often lead to cardiac failure, cranial bruits (pattern 1), hydrocephaly, and subarachnoid hemorrhage in neonates.[4] The heart failure is due to the size of the arteriovenous shunt that can steal 80% or more of the cardiac output, with large volumes of blood under high pressure returning to the right heart and pulmonary circulation and sinus venosus atrial septal defects.[4][5] It is also the most common cause of death in such patients.[6]
Associated conditions
Non-developmental syndromes also directly or indirectly affect the Great Cerebral Vein of Galen, although they are extremely rare. These include superior vena cava syndrome (SVCS), and thrombosis of the lateral sinus, superior sagittal sinus, internal jugular vein, or of the Great Cerebral Vein of Galen itself.[citation needed]
Genetics
10% of vein of Galen aneurysmal malformations are associated with deleterious heterozygous mutations of EPHB4[7]
Another study found that 30% of cases were associated with mutations in EPH receptor B4 (EPHB4) gene.[8]
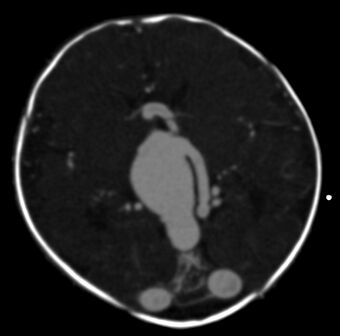
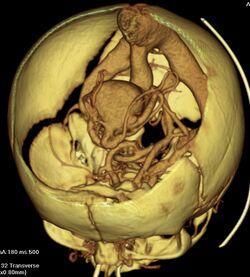
Diagnosis
Testing for a malformed vein of Galen is indicated when a patient has heart failure which has no obvious cause.[9] Diagnosis is generally achieved by signs such as cranial bruits and symptoms such as expanded facial veins.[4] The vein of Galen can be visualized using ultrasound or Doppler.[4] A malformed Great Cerebral Vein will be noticeably enlarged. Ultrasound is a particularly useful tool for vein of Galen malformations because so many cases occur in infancy and ultrasound can make diagnoses prenatally. Many cases are diagnosed only during autopsy as congestive heart failure occurs very early.[10]
Classification
Five patterns of Galenic arteriovenous malformations have been described:
| Pattern 1 | Many vessels, including anterior cerebral arteries, thalamic perforating arteries, and superior cerebellar arteries discharge into the vein of Galen.[10] |
|---|---|
| Pattern 2 | A single posterior choroidal artery drains into the vein of Galen.[10] |
| Pattern 3 | One or both posterior choroidal and one or both anterior cerebral arteries drain directly into the Galenic system.[10] |
| Pattern 4 | An angiomatous network of posterior choroidal and thalamic perforating arteries enter the Vein of Galen directly.[10] |
| Pattern 5 | A high flow arteriovenous malformation in the right inferior frontal lobe drains via the inferior sagittal sinus and pericallosal vein into the Vein of Galen.[4] |
These malformations develop in utero by the persistence of fistulae between primitive pia arachnoidal arteries and pial veins that cross each other at right angles.[4] Because the primitive Galenic system and the primitive choroidal system lie close together, an arteriovenous malformation involving the primitive choroidal system will inevitably involve the Galenic vein.[11] Larger arteriovenous shunts correlate with greater hemodynamic effects and earlier symptom onset; small arteriovenous shunts correlate with greater local mass effect causing progressive neurological impairment.[4]
Treatment
Treatment depends on the anatomy of the malformation as determined by angiography or Magnetic Resonance Imaging (MRI).[4]
Surgical
Head circumference measurements should be obtained regularly and monitored carefully to detect hydrocephalus. Neurosurgical procedures to relieve hydrocephalus are important. A ventriculoperitoneal shunt may be required in some infants. A pediatric cardiologist should be consulted to manage high-output failure, if present. Often patients need to be intubated. In most cases, the fistulous arteries feeding into the Vein of Galen must be blocked, thereby reducing the blood flow into the vein.[10] Open surgery has a high morbidity and mortality. Recent advances over the past few decades have made endovascular embolization the preferred method of treatment. These treatments are preferred because they offer little threat to the surrounding brain tissue. However, there have been several reported cases of arteriovenous malformations recurring.[12] The young age of many patients, the complex vascular anatomy, and the sensitive location of the Vein of Galen offer considerable challenges to surgeons.[13] Another treatment option is Radiotherapy. Radiotherapy, also called radiosurgery, involves the use of focused beams to damage the blood vessel.[12] Radiotherapy is often not pursued as a treatment because the effects of the procedure can take months or years and there is risk of damaging adjacent brain tissue.[12]
Medical care
Surgery is not always an option when the anatomy of the malformation creates too much of a risk. Recent improvements in endovascular procedures have made many cases, which were not surgically accessible, treatable.[12] Endovascular treatments involve delivering drugs, balloons, or coils to the site of the malformation through blood vessels via catheters.[12] These treatments work by limiting blood flow through the vein. There is, however, still risk of complications from endovascular treatments. The wall of the vein can be damaged during the procedure and, in some cases, the emboli can become dislodged and travel through the vascular system.[5] Two-dimensional echocardiography with color-flow imaging and pulsed Doppler ultrasound was used to evaluate one fetus and five neonates with a Vein of Galen malformation.[14] Color-flow imaging and pulsed Doppler ultrasonography provided anatomical and pathophysiological information regarding cardiac hemodynamics and intracranial blood flow; with the patient's clinical status, these methods provided a reliable, noninvasive means to evaluate the effectiveness of therapy and the need for further treatment in neonates with Vein of Galen malformations.[14] When none of these procedures are viable, shunting can be used to ameliorate the pressure inside the varix.[4] Seizures usually are managed with antiepileptic medications.[15]
Prognosis
The complications that are usually associated with vein of Galen malformations are usually intracranial hemorrhages.[16] Over half the patients with VGAM have a malformation that cannot be corrected. Patients frequently die in the neonatal period or in early infancy.[5]
Society and culture
Vein of Galen malformations are devastating complications. Studies have shown that 77% of untreated cases result in mortality.[13] Even after surgical treatment, the mortality rate remains as high as 39.4%.[13] Most cases occur during infancy when the mortality rates are at their highest. Vein of Galen malformations are a relatively unknown condition, attributed to the rareness of the malformations. Therefore, when a child is diagnosed with a faulty Great Cerebral Vein of Galen, most parents know little to nothing about what they are dealing with.[citation needed]
References
- ↑ Jump up to: 1.0 1.1 O'Brien M; Schechter M (September 1970). "Arteriovenous malformations involving the Galenic system". The American Journal of Roentgenology, Radium Therapy, and Nuclear Medicine 110 (1): 50–55. doi:10.2214/ajr.110.1.50. ISSN 0002-9580. PMID 5459527. http://www.ajronline.org/cgi/reprint/110/1/50.pdf. Retrieved October 25, 2009.[yes|permanent dead link|dead link}}]
- ↑ K.M. Auyeung, S. Laughlin, K.G. TerBrugge (October 2004). "Prenatal Diagnosis of Unusual Fetal Pial Arteriovenous Malformation". Interv Neuroradiol 9 (2): 163–8. doi:10.1177/159101990300900205. PMID 20591266.
- ↑ Jump up to: 3.0 3.1 3.2 Takashima S; Becker LE (May 1980). "Neuropathology of cerebral arteriovenous malformations in children". Journal of Neurology, Neurosurgery, and Psychiatry 43 (5): 380–385. doi:10.1136/jnnp.43.5.380. ISSN 0022-3050. PMID 7420086.
- ↑ Jump up to: 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 4.9 Nicholson AA; Hourihan MD; Hayward C (December 1989). "Arteriovenous malformations involving the vein of Galen". Archives of Disease in Childhood 64 (12): 1653–1655. doi:10.1136/adc.64.12.1653. ISSN 0003-9888. PMID 2696431.
- ↑ Jump up to: 5.0 5.1 5.2 5.3 McElhinney DB; Halbach VV; Silverman NH; Dowd CF; Hanley FL (June 1998). "Congenital cardiac anomalies with vein of Galen malformations in infants". Archives of Disease in Childhood. Fetal and neonatal edition 78 (6): 548–551. doi:10.1136/adc.78.6.548. ISSN 1359-2998. PMID 9713012.
- ↑ Johnston IH; Whittle IR; Besser M; Morgan MK (May 1987). "Vein of Galen malformation: diagnosis and management". Neurosurgery 20 (5): 747–758. doi:10.1227/00006123-198705000-00013. ISSN 0148-396X. PMID 3601022.
- ↑ Vivanti, Alexandre; Ozanne, Augustin; Grondin, Cynthia; Saliou, Guillaume; Quevarec, Loic; Maurey, Helène; Aubourg, Patrick; Benachi, Alexandra et al. (April 2018). "Loss of function mutations in EPHB4 are responsible for vein of Galen aneurysmal malformation". Brain 141 (4): 979–988. doi:10.1093/brain/awy020. PMID 29444212.
- ↑ Duran D, Zeng X, Jin SC, Choi J, Nelson-Williams C, Yatsula B, Gaillard J, Furey CG, Lu Q, Timberlake AT, Dong W, Sorscher MA, Loring E, Klein J, Allocco A, Hunt A, Conine S, Karimy JK, Youngblood MW, Zhang J, DiLuna ML, Matouk CC, Mane S, Tikhonova IR, Castaldi C, López-Giráldez F, Knight J, Haider S, Soban M, Alper SL, Komiyama M, Ducruet AF, Zabramski JM, Dardik A, Walcott BP, Stapleton CJ, Aagaard-Kienitz B, Rodesch G, Jackson E, Smith ER, Orbach DB, Berenstein A, Bilguvar K, Vikkula M, Gunel M, Lifton RP, Kahle KT (2018) Mutations in chromatin modifier and ephrin signaling genes in vein of Galen malformation. Neuron
- ↑ "Vein of Galen Abnormalities". Duke University. http://www.dukehealth.org/services/cerebrovascular_center/treatments/vein_of_galen_abnormalitie. [|permanent dead link|dead link}}]
- ↑ Jump up to: 10.0 10.1 10.2 10.3 10.4 10.5 Hoffman HJ; Chuang S; Hendrick EB; Humphreys RP (September 1982). "Aneurysms of the vein of Galen. Experience at The Hospital for Sick Children, Toronto". Journal of Neurosurgery 57 (3): 316–322. doi:10.3171/jns.1982.57.3.0316. ISSN 0022-3085. PMID 7097326.
- ↑ Padget DH (May 1956). "The cranial venous system in man in reference to development, adult configuration, and relation to the arteries". The American Journal of Anatomy 98 (3): 307–355. doi:10.1002/aja.1000980302. ISSN 0002-9106. PMID 13362118.
- ↑ Jump up to: 12.0 12.1 12.2 12.3 12.4 The Arteriovenous Malformation Study Group (June 10, 1999). "Arteriovenous Malformations of the Brain in Adults". New England Journal of Medicine 340 (23): 1812–1818. doi:10.1056/NEJM199906103402307. ISSN 0028-4793. PMID 10362826.
- ↑ Jump up to: 13.0 13.1 13.2 Alexander, Michael J.; Spetzler, Robert F. (October 2005). Pediatric Neurovascular Disease: Surgical, Endovascular, and Medical Management. New York: Thieme Medical Publishers. ISBN 978-1-58890-368-6.
- ↑ Jump up to: 14.0 14.1 Ciricillo, S.F.; SCHMIDT K.G.; SILVERMAN N.H.; HIESHIMA G.B.; HIGASHIDA R.T.; HALBACH V.V.; EDWARDS M.S.B (1990). "Serial Ultrasonographic Evaluation of Neonatal Vein of Galen Malformations to Assess the Efficacy of Interventional Neuroradiological Procedures". Neurosurgery 27 (4): 544–548. doi:10.1227/00006123-199010000-00007. ISSN 0148-396X. PMID 2234356.
- ↑ Chatterjee, S. (May 22, 2009). "Antiepileptic drugs". Indian Journal of Pharmacology. http://medind.nic.in/ibi/t01/i3/ibit01i3p229.pdf. [sic]
- ↑ Meyers PM; Halbach VV; Phatouros CP; Dowd CF; Malek AM; Lempert TE; Lefler JE; Higashida RT (June 2000). "Hemorrhagic complications in vein of Galen malformations". Annals of Neurology 47 (6): 748–755. doi:10.1002/1531-8249(200006)47:6<748::AID-ANA7>3.0.CO;2-7. PMID 10852540.
External links
 |