Medicine:Knee pain
| Knee pain | |
|---|---|
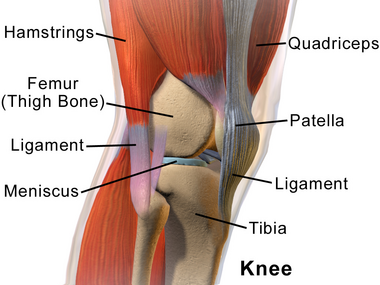 | |
| Human knee | |
| Specialty | Orthopedics |
Knee pain is pain in or around the knee.
The knee joint consists of an articulation between four bones: the femur, tibia, fibula and patella. There are four compartments to the knee. These are the medial and lateral tibiofemoral compartments, the patellofemoral compartment and the superior tibiofibular joint. The components of each of these compartments can experience repetitive strain, injury or disease.[1]
Running long distance can cause pain to the knee joint, as it is a high-impact exercise.[2]
The location and severity of knee pain may vary, depending on the cause of the problem. Signs and symptoms that sometimes accompany knee pain include:[1]
- Swelling and stiffness
- Redness and warmth to the touch
- Weakness or instability
- Popping or crunching noises
- Inability to fully straighten the knee
Causes
Injuries
Some common injuries based on the location include:[3]
- Sprain (Ligament sprain)
- Medial collateral ligament
- Lateral collateral ligament
- Anterior cruciate ligament
- Posterior cruciate ligament
- Tear of meniscus[4]
- Medial meniscus
- Lateral meniscus
- Strain (Muscle strain)
- Quadriceps muscles
- Hamstring muscles
- Popliteal muscle
- Patellar tendon
- Hamstring tendon
- Popliteal tendon
- Hemarthrosis – Hemarthrosis tends to develop over a relatively short period after injury, from several minutes to a few hours.[5]
Fractures
- Femoral fracture
- Tibial fracture
- Patella fracture[4]
Diseases
Some of the diseases of cause of knee pain include the following:
- Knee osteoarthritis[4]
- Chondromalacia patella
- Baker's cyst
- Meniscal cyst
- Discoid meniscus
- Osgood-Schlatter disease[4]
- Larsen-Johansson disease[4]
- Knee rheumatoid arthritis[4]
- Osteochondritis dissecans disease[6][7]
- Synovial chondromatosis disease[8]
- Tumors[9]
- Ankylosing spondylitis[10]
- Reactive arthritis[11]
- Tuberculosis arthritis[12]
- Septic arthritis (Pyogenic arthritis)[13]
- Osteomyelitis[14]
- Hemophilic arthritis[15]
- Gout (Gouty arthritis)[16]
- Neuroma[4]
Inflammations
- Bursitis of the knee
- Prepatellar bursitis - Housemaid's knee (most common)
- Infrapatellar bursitis - Clergyman's knee (Superficial infrapatellar bursitis and Deep infrapatellar bursitis)
- Semimembranosus bursitis
- Tendinitis[4]
- Patellar tendinitis (Jumper's knee)
- Hamstring tendinitis
- Popliteal tendinitis
- Synovitis of the knee
Deformities
Common deformities of the knee include:
- Bipartite patella (two-part kneecap)
- Genu varum (bow legs)
- Genu valgum (knock-knees)
- Genu recurvatum (Knee hyperextension)
- Knee flexion deformity
Syndromes
- Patellofemoral pain syndrome[4]
- Plica syndrome[4]
- Iliotibial band syndrome[4]
- Hoffa's syndrome[4][17]
- Joint hypermobility syndrome[18]
Dislocations
Cold temperature
Knee pain is more common among people working in the cold than in those in normal temperature.[21] Cold-induced knee pain may also be due to tenosynovitis of the tendons around the knee, in which cold exposure has a specific role, either as a causative or a contributing factor.[21] Frank arthritis has been reported in children due to frostbite from extreme cold causing direct chondrocyte injury.[22]
There is also a hereditary disease, familial cold autoinflammatory syndrome (FCAS), which often features knee pain, in addition to hives, fever and pain in other joints, following general exposure to cold.[23]
Knee pain due to less physical movement
Other causes
- Ligamentous laxity
- Fat pad impingement
- Knee effusion
- Deep vein thrombosis
- Peripheral vascular disease
- Exostosis
- Obesity = A systematic review and meta-analysis found that approximately 25% of new-onset knee pain cases were attributable to overweight[24]
Referred knee pain
Referred pain is that pain perceived at a site different from its point of origin but innervated by the same spinal segment.[25] Sometimes knee pain may be related to another area from body. For example, knee pain can come from ankle, foot, hip joints or lumbar spine.
Diagnosis
Knee MRIs should be avoided for knee pain without symptoms or effusion, unless there are non-successful results from a functional rehabilitation program.[26]
In some diagnosis, such as in knee osteoarthritis, magnetic resonance imaging does not prove to be clear for its determination.[27]
Management
Although surgery has a role in repairing traumatic injuries and broken bones, arthroscopic surgeries do not provide significant or lasting improvements to either pain or function to people with knee pain, and therefore should almost never be performed.[28] Knee pain is pain caused by wear and tear, such as osteoarthritis or a meniscal tear. Effective treatments for knee pain include physical therapy exercises,[29] pain-reducing drugs such as ibuprofen, joint stretching,[30][31] knee replacement surgery, and weight loss in people who are overweight.[28]
Overall, a combination of interventions seems to be the best choice when treating knee pain. Interventions such as exercises that target both the knee and the hip, foot bracing, and patellar taping are all recommended for use with patients who have knee pain.[32]
Current evidence suggests that psychological factors are elevated in individuals with patellofemoral pain.[33] Non-physical factors such as anxiety, depression, fear of movement, and catastrophizing are thought to have a linear correlation with increased pain experience and decreased physical function.[33] Catastrophizing is defined as imagining the worst possible outcome of an action or event.[34] The psychosocial factors may have either a positive or negative impact on adherence to rehabilitation programs for managing knee pain.[33] Furthermore, studies have found knee pain to be negatively associated with health-related quality of life, and an increase in knee pain to be associated with a reduction in patient-reported quality of life, as compared to those with no or stable knee pain, even in the relatively younger middle-aged population.[35] Several movement-based approaches have been associated with improvements in knee pain and stiffness in older adults. Practices such as the Feldenkrais Method and Tai Chi, which emphasize gentle, controlled movement and body awareness, have been reported to support mobility and pain management.[36]
Epidemiology
About 25% of people over the age of 50 experience knee pain from degenerative knee diseases.[28]
Society and culture
In the United States, more than US$3 billion is spent each year on arthroscopic knee surgeries that are known to be ineffective in people with degenerative knee pain.[28]
References
- ↑ 1.0 1.1 "Knee pain - Symptoms and causes" (in en). https://www.mayoclinic.org/diseases-conditions/knee-pain/symptoms-causes/syc-20350849.
- ↑ "Knee Injuries from Long Distance Running" (in en-GB). https://castleortho.co.uk/knee-injuries-long-distance-marathon-running/.
- ↑ Green, Shelby (24 November 2022). "Knee Pain Location Chart". feelgoodlife. https://www.feelgoodlife.com/knee-pain-location-chart/.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 "Exercise for treating patellofemoral pain syndrome". The Cochrane Database of Systematic Reviews 1. January 2015. doi:10.1002/14651858.CD010387.pub2. PMID 25603546.
- ↑ Darlene Hertling and Randolph M.Kessler. Management of Common Musculoskeletal Disorders. Third Edition. ISBN 0-397-55150-9
- ↑ "Osteochondritis Dissecans". https://www.lecturio.com/concepts/osteochondritis-dissecans/.
- ↑ "Definition of Osteochondritis dissecans". MedicineNet, Inc.. http://www.medterms.com/script/main/art.asp?articlekey=11789.
- ↑ "Synovial chondromatosis". Soft Tissue and Bone Tumours: WHO Classification of Tumours. International Agency for Research on Cancer. 2020. pp. 368–369. ISBN 978-92-832-4502-5. https://books.google.com/books?id=kaR9zQEACAAJ.
- ↑ "Neoplasm". Lexico. Oxford University Press. https://www.lexico.com/en/definition/neoplasm.
- ↑ "Ankylosing Spondylitis". https://www.lecturio.com/concepts/ankylosing-spondylitis/.
- ↑ "Reactive Arthritis". https://www.lecturio.com/concepts/reactive-arthritis/.
- ↑ "Tuberculosis (TB)" (in en). https://www.who.int/news-room/fact-sheets/detail/tuberculosis.
- ↑ "Septic Arthritis". https://www.lecturio.com/concepts/septic-arthritis/.
- ↑ "Osteomyelitis". https://www.lecturio.com/concepts/osteomyelitis/.
- ↑ "What Is Hemophilia?". U.S. Centers for Disease Control. 12 May 2020. https://www.cdc.gov/ncbddd/hemophilia/facts.html.
- ↑ "Gout". 9 September 2020. https://www.lecturio.com/concepts/gout/.
- ↑ DuBose, Matthew; Taqi, Muhammad (2024), "Hoffa Pad Impingement Syndrome", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 36943955, https://www.ncbi.nlm.nih.gov/books/NBK589637/, retrieved 2024-09-23
- ↑ Miklovic, Tyler; Sieg, Vanessa C. (2024), "Ehlers-Danlos Syndrome", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 31747221, https://www.ncbi.nlm.nih.gov/books/NBK549814/, retrieved 2024-09-23
- ↑ Hayat, Zara; El Bitar, Youssef; Case, Justin L. (2024), "Patella Dislocation", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 30855872, https://www.ncbi.nlm.nih.gov/books/NBK538288/, retrieved 2024-09-23
- ↑ Mohseni, Michael; Mabrouk, Ahmed; Simon, Leslie V. (2024), "Knee Dislocation", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 29262122, https://www.ncbi.nlm.nih.gov/books/NBK470595/, retrieved 2024-09-23
- ↑ 21.0 21.1 "Cold exposure and musculoskeletal disorders and diseases. A review". International Journal of Circumpolar Health 61 (2): 173–82. May 2002. doi:10.3402/ijch.v61i2.17450. PMID 12078965.
- ↑ "Arthritis after frostbite injury in children". Arthritis and Rheumatism 22 (10): 1082–7. October 1979. doi:10.1002/art.1780221006. PMID 486219.
- ↑ Clinical trial number NCT00887939 for "Pathogenesis of Physical Induced Urticarial Syndromes" at ClinicalTrials.gov
- ↑ Silverwood V, Blagojevic-Bucknall M, Jinks C, Jordan JL, Protheroe J, Jordan KP (2015). "Current evidence on risk factors for knee osteoarthritis in older adults: a systematic review and meta-analysis." Osteoarthritis and Cartilage. 23 (4): 507–515. doi:10.1016/j.joca.2014.11.019. PMID 25447976. https://pubmed.ncbi.nlm.nih.gov/25447976/
- ↑ Porth, Carol (2011). Essentials of Pathophysiology: Concepts of Altered Health States. Lippincott Williams & Wilkins. p. 853. ISBN 978-1-58255-724-3.
- ↑ American Medical Society for Sports Medicine (24 April 2014), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation (American Medical Society for Sports Medicine), http://www.choosingwisely.org/doctor-patient-lists/american-medical-society-for-sports-medicine/, retrieved 29 July 2014
- "Management of patellofemoral pain syndrome". American Family Physician 75 (2): 194–202. January 2007. PMID 17263214.
- "Approach to the active patient with chronic anterior knee pain". The Physician and Sportsmedicine 40 (1): 41–50. February 2012. doi:10.3810/psm.2012.02.1950. PMID 22508250.
- "Prospective Predictors of Patellofemoral Pain Syndrome: A Systematic Review With Meta-analysis". Sports Health 4 (2): 115–20. March 2012. doi:10.1177/1941738111432097. PMID 23016077.
- "A review of the management of patellofemoral pain syndrome". The Physician and Sportsmedicine 41 (3): 19–28. September 2013. doi:10.3810/psm.2013.09.2023. PMID 24113699.
- "Anterior knee pain: a clinical comparison of rehabilitation methods". Clinical Journal of Sport Medicine 10 (1): 22–8. January 2000. doi:10.1097/00042752-200001000-00005. PMID 10695846.
- ↑ "Prevalence of knee osteoarthritis features on magnetic resonance imaging in asymptomatic uninjured adults: a systematic review and meta-analysis". British Journal of Sports Medicine 53 (20): bjsports–2018–099257. June 2018. doi:10.1136/bjsports-2018-099257. PMID 29886437.
- ↑ 28.0 28.1 28.2 28.3 "Arthroscopic surgery for degenerative knee arthritis and meniscal tears: a clinical practice guideline". BMJ 357. May 2017. doi:10.1136/bmj.j1982. PMID 28490431.
- ↑ "How to manage patellofemoral pain - Understanding the multifactorial nature and treatment options". Physical Therapy in Sport 32: 155–166. July 2018. doi:10.1016/j.ptsp.2018.04.010. PMID 29793124.
- ↑ "Knee Reviver, innovatief product voor gewrichtsparende behandeling bij knieartrose". 2024-01-01. https://www.nwo.nl/onderzoek-en-resultaten/onderzoeksprojecten/i/22/28022.html.
- ↑ "Kniedistractie - UMC Utrecht". https://www.umcutrecht.nl/nl/behandeling/kniedistractie.
- ↑ "2016 Patellofemoral pain consensus statement from the 4th International Patellofemoral Pain Research Retreat, Manchester. Part 2: recommended physical interventions (exercise, taping, bracing, foot orthoses and combined interventions)". British Journal of Sports Medicine 50 (14): 844–52. July 2016. doi:10.1136/bjsports-2016-096268. PMID 27247098.
- ↑ 33.0 33.1 33.2 "The psychological features of patellofemoral pain: a systematic review". British Journal of Sports Medicine 51 (9): 732–742. May 2017. doi:10.1136/bjsports-2016-096705. PMID 28320733.
- ↑ "Definition of CATASTROPHIZE". https://www.merriam-webster.com/dictionary/catastrophize.
- ↑ Singh, Ambrish; Campbell, Julie A.; Venn, Alison; Jones, Graeme; Blizzard, Leigh; Palmer, Andrew J.; Dwyer, Terence; Cicuttini, Flavia et al. (September 2021). "Association between knee symptoms, change in knee symptoms over 6-9 years, and SF-6D health state utility among middle-aged Australians". Quality of Life Research 30 (9): 2601–2613. doi:10.1007/s11136-021-02859-5. PMID 33942204.
- ↑ https://feldy.me/feldypedia/pain-and-discomfort/knee-stiffness-after-60
External links
| Classification | |
|---|---|
| External resources |
 |
