Engineering:Peptide receptor radionuclide therapy
| Peptide receptor radionuclide therapy | |
|---|---|
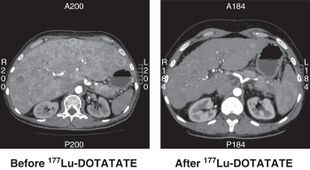 CT scan of non-functioning pancreatic NET before and 6 months after successful treatment with four cycles of 177Lu-DOTATATE. | |
| Specialty | oncology |
Peptide receptor radionuclide therapy (PRRT) is a type of radionuclide therapy, using a radiopharmaceutical that targets peptide receptors to deliver localised treatment, typically for neuroendocrine tumours (NETs).[1]
Mechanism
A key advantage of PRRT over other methods of radiotherapy is the ability to target delivery of therapeutic radionuclides directly to the tumour or target site. This works because some tumours have an abundance (overexpression) of peptide receptors, compared to normal tissue. A radioactive substance can be combined with a relevant peptide (or its analogue) so that it preferentially binds to the tumour.[2][3] With a gamma emitter as the radionuclide, the technique can be used for imaging with a gamma camera or PET scanner to locate tumours. When paired with alpha or beta emitters, therapy can be achieved, as in PRRT.[4]
The current generation of PRRT targets somatostatin receptors, with a range of analogue materials such as octreotide and other DOTA compounds. These are combined with indium-111, lutetium-177 or yttrium-90 for treatment.[5] 111In is primarily used for imaging alone, however in addition to its gamma emission there are also auger electrons emitted, which can have a therapeutic effect in high doses.[6]
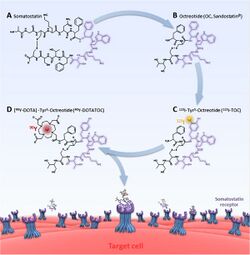
PRRT radiopharmaceuticals are constructed with three components; the radionuclide, chelator, and somatostatin analogue (peptide). The radionuclide delivers the actual therapeutic effect (or emission, such as photons, for imaging). The chelator is the essential link between the radionuclide and peptide. For 177Lu and 90Y this is typically DOTA (tetracarboxylic acid, and its variants) and DTPA (pentetic acid) for 111In.[7] Other chelators known as NOTA (triazacyclononane triacetic acid) and HYNIC (hydrazinonicotinamide) have also been experimented with, albeit more for imaging applications.[8][9] The somatostatin analogue affects biodistribution of the radionuclide, and therefore how effectively any treatment effect can be targeted. Changes affect which somatostatin receptor is most strongly targeted. For example, DOTA-lanreotide (DOTALAN) has a lower affinity for receptor 2 and a higher affinity for receptor 5 compared to DOTA-octreotide (DOTATOC).[6][10]
Applications
The body of research on the effectiveness of current PRRT is promising, but limited. Complete or partial treatment response has been seen in 20-30% of patients in trials treated with 177Lu-DOTATATE or 90Y-DOTATOC, among the most widely used PRRT drugs.[1][11][12][13] When it comes to comparing these two PRRT, Y-labeled and Lu-labeled PRRTs, it appears that Y-labeled is more effective for larger tumors, while Lu-labeled is better for smaller and primary tumors. The lack of ɤ-emission with Y-labeled PPRTs is also an important difference between Lu peptides and Y peptide. In particular, with Y-labeled PRRT it becomes difficult to set up a dose of radiations specific to the patient's needs.[14] In most cases PRRT is used for cancers of the gastroenteropancreatic[15] and bronchial tracts, and in some cases phaeochromocytoma, paraganglioma, neuroblastoma or medullary thyroid carcinoma.[1] Various approaches to approve effectiveness and limit side effects are being investigated, including radiosensitising drugs, fractionation regimes and new radionuclides.[16] Alpha emitters, which have much shorter ranges in tissue (limiting the effect on nearby healthy tissue), such as bismuth-213 or actinium-225 labelled DOTATOC are of particular interest.[17]
A comparative cohort study of 1051 neuroendocrine tumor patients undergoing 90Y-DOTATOC (n=910) or 177Lu-DOTATOC (n=141) reported no significant difference in overall survival between the groups. However, patients with high tumor accumulation and multiple lesions seemed to benefit from 90Y-DOTATOC, while patients with low tumor burden, solitary lesions and extra-hepatic disease experienced more favorable outcome on 177Lu-DOTATOC. There were significantly fewer cases of transitory hematotoxicity in the 177Lu-DOTATOC group compared with the 90Y-DOTATOC group (1.4% versus 10.1%, p=0.001).[18]
The randomized controlled phase III Neuroendocrine Tumors Therapy (NETTER-1) trial evaluated the efficacy and safety of 177Lu-DOTATATE as compared with high-dose octreotide long-acting repeatable (LAR) in patients with advanced progressive somatostatin-receptor positive midgut neuroendocrine tumors. Patients were randomly assigned to receive either 177Lu-DOTATATE and octreotide LAR at a dose of 30 mg every four weeks for symptom control (n=116) or to only receive octreotide LAR at a dose of 60 mg every four weeks (n=113, control group). In total, 200 out of the 231 patients entered long-term follow-up. Final overall survival in the intention-to-treat population was median 48.0 months in the 177Lu-DOTATATE group versus median 36.3 months in the control group (p=0.30). In other words, there was numerical difference of 11.7 months, not reaching statistical significance. 177Lu-DOTATATE was associated with limited acute toxic effects. In neuroendocrine tumor patients with advanced well-differentiated disease and progression on somatostatin analogs, 177Lu-DOTATATE is likely to reduce the risk of disease progression and be associated with quality-of-life benefits.[19][20]
Dosimetry
Therapeutic PRRT treatments typically involve several gigabecquerels (GBq) of activity.[21] Several radiopharmaceuticals allow simultaneous imaging and therapy, enabling precise dosimetric estimates to be made. For example, the bremsstrahlung emission from 90Y and gamma emissions from 177Lu can be detected by a gamma camera. In other cases, imaging can be performed by labelling a suitable radionuclide to the same peptide as used for therapy.[22] Radionuclides that can be used for imaging include gallium-68, technetium-99m and fluorine-18.[21]
Currently used peptides can result in high kidney doses, as the radiopharmaceutical is retained for relatively long periods. Renal protection is therefore used in some cases, taking the form of alternative substances that reduce the uptake of the kidneys.[5][21][23]
Availability
PRRT is not yet widely available, with various radiopharmaceuticals at different stages of clinical trials. The cost of small volume production of the relevant radionuclides is high.[24] The cost of Lutathera, a commercial 177Lu-DOTATATE product, has been quoted by the manufacturer as £71,500 (€80,000 or $94,000 in July 2018) for 4 administrations of 7.4 GBq.[25]
United States
177Lu-DOTATATE (international nonproprietary name: lutetium (177Lu) oxodotreotide) was approved by the FDA in early 2018, for treatment of gastroenteropancreatic neuroendocrine tumors (GEP-NETs).[26][27]
Europe
Marketing authorisation for 177Lu-DOTATATE was granted by the European Medicines Agency on 26 September 2017.[28] 90Y-DOTATOC (international nonproprietary name: yttrium (90Y) edotreotide) and 177Lu-DOTATOC are designated as orphan drugs, but have not yet received marketing authorisation.[29][30]
United Kingdom
In guidance published in August 2018, lutetium (177Lu) oxodotreotide was recommended by NICE for treating unresectable or metastatic neuroendocrine tumours.[31]
Turkey
The first therapies in Turkey using 177Lu-DOTATATE PRRT were carried out in early 2014, for treatment of gastroenteropancreatic neuroendocrine tumors (GEP-NETs) at the Istanbul University-Cerrahpaşa.[32]
Australia
Research in Australia into the use of lutetium-177-labelled antibodies for various cancers began in the Department of Nuclear Medicine at Fremantle Hospital and Health Service (FHHS), Fremantle, Australia in the late 1990s.[33] The first therapies in Australia using 177Lu-DOTATATE PRRT for NET began in February 2005 on a trial basis under the Therapeutic Goods Administration's (TGA) Special Access Scheme (SAS) and compassionate usage of unapproved therapeutic goods.[34][35] Shortly after this, 177Lu-DOTATATE PRRT was provided to Western Australian NET patients on a routine basis under the SAS, as well as under various on-going research trials.[36][37][38][39][40][41][42][43][excessive citations]
In Australia, most centres synthesise the lutetium-177 peptide on-site from lutetium-177 chloride and the appropriate peptide.[44]
Side effects
Like any form of radiotherapy, ionising radiation can harm healthy tissue as well as the intended treatment target. Radiation from lutetium (177Lu) oxodotreotide can cause damage when the medicine passes through tubules in the kidney.[45] Arginine/lysine can be used to reduce renal radiation exposure during peptide receptor radionuclide therapy with lutetium (177Lu) oxodotreotide.[45]
See also
References
- ↑ 1.0 1.1 1.2 Zaknun, John J.; Bodei, L.; Mueller-Brand, J.; Pavel, M. E.; Baum, R. P.; Hörsch, D.; O’Dorisio, M. S.; O’Dorisiol, T. M. et al. (7 February 2013). "The joint IAEA, EANM, and SNMMI practical guidance on peptide receptor radionuclide therapy (PRRNT) in neuroendocrine tumours". European Journal of Nuclear Medicine and Molecular Imaging 40 (5): 800–816. doi:10.1007/s00259-012-2330-6. PMID 23389427.
- ↑ "Fact Sheet: What Is Peptide Receptor Radionuclide Therapy (PRRT)?". http://www.snmmi.org/AboutSNMMI/Content.aspx?ItemNumber=5691. Retrieved 12 May 2018.
- ↑ Reubi, Jean Claude (August 2003). "Peptide Receptors as Molecular Targets for Cancer Diagnosis and Therapy". Endocrine Reviews 24 (4): 389–427. doi:10.1210/er.2002-0007. PMID 12920149.
- ↑ Dash, Ashutosh; Chakraborty, Sudipta; Pillai, Maroor Raghavan Ambikalmajan; Knapp, Furn F. (Russ) (March 2015). "Peptide Receptor Radionuclide Therapy: An Overview". Cancer Biotherapy & Radiopharmaceuticals 30 (2): 47–71. doi:10.1089/cbr.2014.1741. PMID 25710506.
- ↑ 5.0 5.1 van Essen, Martijn; Krenning, Eric P.; Kam, Boen L. R.; de Jong, Marion; Valkema, Roelf; Kwekkeboom, Dik J. (2 June 2009). "Peptide-receptor radionuclide therapy for endocrine tumors". Nature Reviews Endocrinology 5 (7): 382–393. doi:10.1038/nrendo.2009.105. PMID 19488074.
- ↑ 6.0 6.1 Speer, Tod W. (2012) (in en). Targeted Radionuclide Therapy. Lippincott Williams & Wilkins. p. 40. ISBN 9781451153262. https://books.google.com/books?id=TMJm41g6YZYC&pg=PA40.
- ↑ Bombardieri, Emilio; Seregni, Ettore; Evangelista, Laura; Chiesa, Carlo; Chiti, Arturo (2018) (in en). Clinical Applications of Nuclear Medicine Targeted Therapy. Springer. p. 213. ISBN 9783319630670. https://books.google.com/books?id=uHpTDwAAQBAJ&pg=PA213.
- ↑ SAW, MAUNG MAUNG; Peitl, Petra; Velikyan, Irina (June 2012). "Medicinal Radiopharmaceutical Chemistry of Metal Radiopharmaceuticals". Cosmos 08 (1): 11–81. doi:10.1142/S0219607712300044. Bibcode: 2012Cosmo...8...11S.
- ↑ Fani, Melpomeni; Peitl, Petra; Velikyan, Irina (15 March 2017). "Current Status of Radiopharmaceuticals for the Theranostics of Neuroendocrine Neoplasms". Pharmaceuticals 10 (4): 30. doi:10.3390/ph10010030. PMID 28295000.
- ↑ Stigbrand, Torgny; Carlsson, Jorgen; Adams, Gregory P. (2008) (in en). Targeted Radionuclide Tumor Therapy: Biological Aspects. Springer Science & Business Media. p. 122. ISBN 9781402086960. https://books.google.com/books?id=-mT0Lthq_54C&pg=PA122.
- ↑ Kjaer, A; Knigge, U (June 2015). "Use of radioactive substances in diagnosis and treatment of neuroendocrine tumors.". Scandinavian Journal of Gastroenterology 50 (6): 740–7. doi:10.3109/00365521.2015.1033454. PMID 25959100.
- ↑ Cives, Mauro; Strosberg, Jonathan (20 February 2017). "Radionuclide Therapy for Neuroendocrine Tumors". Current Oncology Reports 19 (2): 9. doi:10.1007/s11912-017-0567-8. PMID 28220446.
- ↑ Bison, Sander M.; Konijnenberg, Mark W.; Melis, Marleen; Pool, Stefan E.; Bernsen, Monique R.; Teunissen, Jaap J. M.; Kwekkeboom, Dik J.; de Jong, Marion (5 March 2014). "Peptide receptor radionuclide therapy using radiolabeled somatostatin analogs: focus on future developments". Clinical and Translational Imaging 2 (1): 55–66. doi:10.1007/s40336-014-0054-2. PMID 24765618.
- ↑ Dash, Ashutosh; Chakraborty, Sudipta; Pillai, Maroor Raghavan Ambikalmajan; Knapp, Furn F. (Russ) (March 2015). "Peptide Receptor Radionuclide Therapy: An Overview" (in en). Cancer Biotherapy and Radiopharmaceuticals 30 (2): 47–71. doi:10.1089/cbr.2014.1741. ISSN 1084-9785. PMID 25710506.
- ↑ Liberini, Virginia; Huellner, Martin W.; Grimaldi, Serena; Finessi, Monica; Thuillier, Philippe; Muni, Alfredo; Pellerito, Riccardo E.; Papotti, Mauro G. et al. (2020-12-12). "The Challenge of Evaluating Response to Peptide Receptor Radionuclide Therapy in Gastroenteropancreatic Neuroendocrine Tumors: The Present and the Future". Diagnostics (Basel, Switzerland) 10 (12): 1083. doi:10.3390/diagnostics10121083. ISSN 2075-4418. PMID 33322819.
- ↑ Sabet, Amir; Biersack, Hans-Jürgen; Ezziddin, Samer (January 2016). "Advances in Peptide Receptor Radionuclide Therapy". Seminars in Nuclear Medicine 46 (1): 40–46. doi:10.1053/j.semnuclmed.2015.09.005. PMID 26687856.
- ↑ Lee, Sze Ting; Kulkarni, Harshad R.; Singh, Aviral; Baum, Richard P. (2017). "Theranostics of Neuroendocrine Tumors". Visceral Medicine 33 (5): 358–366. doi:10.1159/000480383. PMID 29177165.
- ↑ Romer, A.; Seiler, D.; Marincek, N.; Brunner, P.; Koller, M. T.; Ng, Q. K. T.; Maecke, H. R.; Müller-Brand, J. et al. (February 2014). "Somatostatin-based radiopeptide therapy with [177Lu-DOTA-TOC versus [90Y-DOTA]-TOC in neuroendocrine tumours"] (in en). European Journal of Nuclear Medicine and Molecular Imaging 41 (2): 214–222. doi:10.1007/s00259-013-2559-8. ISSN 1619-7070. PMID 24085501. http://link.springer.com/10.1007/s00259-013-2559-8.
- ↑ Strosberg, Jonathan; El-Haddad, Ghassan; Wolin, Edward; Hendifar, Andrew; Yao, James; Chasen, Beth; Mittra, Erik; Kunz, Pamela L. et al. (2017-01-12). "Phase 3 Trial of 177 Lu-Dotatate for Midgut Neuroendocrine Tumors" (in en). New England Journal of Medicine 376 (2): 125–135. doi:10.1056/NEJMoa1607427. ISSN 0028-4793. PMID 28076709.
- ↑ Strosberg, Jonathan R; Caplin, Martyn E; Kunz, Pamela L; Ruszniewski, Philippe B; Bodei, Lisa; Hendifar, Andrew; Mittra, Erik; Wolin, Edward M et al. (December 2021). "177Lu-Dotatate plus long-acting octreotide versus high‑dose long-acting octreotide in patients with midgut neuroendocrine tumours (NETTER-1): final overall survival and long-term safety results from an open-label, randomised, controlled, phase 3 trial" (in en). The Lancet Oncology 22 (12): 1752–1763. doi:10.1016/S1470-2045(21)00572-6. PMID 34793718. https://linkinghub.elsevier.com/retrieve/pii/S1470204521005726.
- ↑ 21.0 21.1 21.2 IAEA (2013). Practical guidance on peptide receptor radionuclide therapy (PRRNT) for neuroendocrine tumors.. IAEA Human Health Series No. 20. Vienna: International Atomic Energy Agency. ISBN 978-92-0-129210-0. https://www-pub.iaea.org/books/IAEABooks/8789/Practical-Guidance-on-Peptide-Receptor-Radionuclide-Therapy-PRRNT-for-Neuroendocrine-Tumours.
- ↑ Cremonesi, M; Botta, F; Di Dia, A; Ferrari, M; Bodei, L; De Cicco, C; Rossi, A; Bartolomei, M et al. (February 2010). "Dosimetry for treatment with radiolabelled somatostatin analogues. A review.". The Quarterly Journal of Nuclear Medicine and Molecular Imaging 54 (1): 37–51. PMID 20168285. https://www.minervamedica.it/en/journals/nuclear-med-molecular-imaging/article.php.
- ↑ Rolleman, Edgar J.; Melis, Marleen; Valkema, Roelf; Boerman, Otto C.; Krenning, Eric P.; de Jong, Marion (14 November 2009). "Kidney protection during peptide receptor radionuclide therapy with somatostatin analogues". European Journal of Nuclear Medicine and Molecular Imaging 37 (5): 1018–1031. doi:10.1007/s00259-009-1282-y. PMID 19915842.
- ↑ Dash, Ashutosh; Pillai, Maroor Raghavan Ambikalmajan; Knapp, Furn F. (17 February 2015). "Production of 177Lu for Targeted Radionuclide Therapy: Available Options". Nuclear Medicine and Molecular Imaging 49 (2): 85–107. doi:10.1007/s13139-014-0315-z. PMID 26085854.
- ↑ "Information about lutetium (177Lu) oxodotreotide". National Institute for Health and Care Excellence. 29 August 2018. https://www.nice.org.uk/guidance/ta539/chapter/2-Information-about-lutetium-177Lu-oxodotreotide. Retrieved 3 September 2018.
- ↑ "Lutetium Lu 177 Dotatate Approved by FDA". Cancer Discovery 8 (4): OF2. April 2018. doi:10.1158/2159-8290.CD-NB2018-021. PMID 29487054.
- ↑ Office of the Commissioner (26 January 2018). "FDA approves new treatment for certain digestive tract cancers" (in en). https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm594043.htm. Retrieved 20 May 2018.
- ↑ "Lutathera" (in en). http://www.ema.europa.eu/ema/index.jsp?curl=pages/medicines/human/medicines/004123/human_med_002163.jsp. Retrieved 24 May 2018.
- ↑ "Yttrium (90Y) edotreotide" (in en). http://www.ema.europa.eu:80/ema/index.jsp?curl=pages/medicines/human/orphans/2009/11/human_orphan_000509.jsp. Retrieved 24 May 2018.
- ↑ "EU/03/14/1269". https://www.ema.europa.eu/en/medicines/human/orphan-designations/eu03141269. Retrieved 7 November 2020.
- ↑ "Lutetium (177Lu) oxodotreotide for treating unresectable or metastatic neuroendocrine tumours [TA539"]. 29 August 2018. https://www.nice.org.uk/guidance/ta539. Retrieved 3 September 2018.
- ↑ Kabasaka, Levent. "Lu-177-PSMA Real World Clinical Study: Out-patient or In-patient Treatment". https://cdn.ymaws.com/www.bnms.org.uk/resource/resmgr/presentations/spring_2018/sunday/h05_sun_1015_kebasakal.pdf.
- ↑ Turner, J Harvey (1998-12-31). Radiolanthanides in therapeutic nuclear oncology (Conference) | ETDEWEB. https://www.osti.gov/etdeweb/biblio/347100. Retrieved 2019-10-04.
- ↑ Australian Government Department of Health Therapeutic Goods Administration (2018-01-05). "Special Access Scheme: Guidance for health practitioners and sponsors" (in en). https://www.tga.gov.au/special-access-scheme-guidance-health-practitioners-and-sponsors.
- ↑ "COSA:NETs guidelines/Radionuclide Therapy - Clinical Guidelines Wiki". https://wiki.cancer.org.au/australia/COSA:NETs_guidelines/Radionuclide_Therapy.
- ↑ Claringbold, Phillip G.; Brayshaw, Paul A.; Price, Richard A.; Turner, J. Harvey (2011-02-01). "Phase II study of radiopeptide 177Lu-octreotate and capecitabine therapy of progressive disseminated neuroendocrine tumours" (in en). European Journal of Nuclear Medicine and Molecular Imaging 38 (2): 302–311. doi:10.1007/s00259-010-1631-x. ISSN 1619-7089. PMID 21052661.
- ↑ Turner, J. H. (2009). "Defining Pharmacokinetics for Individual Patient Dosimetry in Routine Radiopeptide and Radioimmunotherapy of Cancer: Australian Experience" (in en). Current Pharmaceutical Design 15 (9): 966–82. doi:10.2174/138161209787582020. PMID 19275661.
- ↑ Claringbold, Phillip G.; Price, Richard A.; Turner, J. Harvey (2012-10-18). "Phase I-II Study of Radiopeptide 177Lu-Octreotate in Combination with Capecitabine and Temozolomide in Advanced Low-Grade Neuroendocrine Tumors". Cancer Biotherapy and Radiopharmaceuticals 27 (9): 561–569. doi:10.1089/cbr.2012.1276. ISSN 1084-9785. PMID 23078020.
- ↑ Kesavan, Murali; Claringbold, Phillip G.; Turner, J. Harvey (2014). "Hematological Toxicity of Combined177Lu-Octreotate Radiopeptide Chemotherapy of Gastroenteropancreatic Neuroendocrine Tumors in Long-Term Follow-Up". Neuroendocrinology 99 (2): 108–117. doi:10.1159/000362558. ISSN 1423-0194. PMID 24714208.
- ↑ Claringbold, Phillip G.; Turner, J. Harvey (August 2015). "NeuroEndocrine Tumor Therapy with Lutetium-177-octreotate and Everolimus (NETTLE): A Phase I Study". Cancer Biotherapy and Radiopharmaceuticals 30 (6): 261–269. doi:10.1089/cbr.2015.1876. ISSN 1084-9785. PMID 26181854.
- ↑ Claringbold, Phillip G.; Turner, J. Harvey (2015-06-10). "Pancreatic Neuroendocrine Tumor Control: Durable Objective Response to Combination 177Lu-Octreotate-Capecitabine-Temozolomide Radiopeptide Chemotherapy". Neuroendocrinology 103 (5): 432–439. doi:10.1159/000434723. ISSN 0028-3835. PMID 26065489.
- ↑ Kesavan, Murali; Turner, J. Harvey (August 2016). "Myelotoxicity of Peptide Receptor Radionuclide Therapy of Neuroendocrine Tumors: A Decade of Experience". Cancer Biotherapy and Radiopharmaceuticals 31 (6): 189–198. doi:10.1089/cbr.2016.2035. ISSN 1084-9785. PMID 27419665.
- ↑ Kesavan, Murali; Turner, J. Harvey; Meyrick, Danielle; Yeo, Sharon; Cardaci, Giuseppe; Lenzo, Nat P. (September 2018). "Salvage Radiopeptide Therapy of Advanced Castrate-Resistant Prostate Cancer with Lutetium-177-Labeled Prostate-Specific Membrane Antigen: Efficacy and Safety in Routine Practice". Cancer Biotherapy and Radiopharmaceuticals 33 (7): 274–281. doi:10.1089/cbr.2017.2403. ISSN 1084-9785. PMID 29989440.
- ↑ De Decker, Mario; Turner, J. Harvey (February 2012). "Automated Module Radiolabeling of Peptides and Antibodies with Gallium-68, Lutetium-177 and Iodine-131". Cancer Biotherapy and Radiopharmaceuticals 27 (1): 72–76. doi:10.1089/cbr.2011.1073. ISSN 1084-9785. PMID 22149590.
- ↑ 45.0 45.1 "LysaKare EPAR". https://www.ema.europa.eu/en/medicines/human/EPAR/lysakare. Text was copied from this source which is © European Medicines Agency. Reproduction is authorized provided the source is acknowledged.
 |

