Biology:Betacoronavirus NS7A protein
| Betacoronavirus NS7A protein | |||||||||
|---|---|---|---|---|---|---|---|---|---|
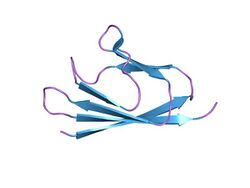 Structure of the SARS-coronavirus orf7a accessory protein | |||||||||
| Identifiers | |||||||||
| Symbol | bCoV_NS7A | ||||||||
| Pfam | PF08779 | ||||||||
| InterPro | IPR014888 | ||||||||
| |||||||||
In molecular biology, Betacoronavirus NS7A protein (also known by several other names, including SARS coronavirus X4, SARS-X4, ORF7a, or U122)[1] is a protein expressed by coronaviruses of the Betacoronavirus genus. The protein is expressed from the ORF7a gene. It is a type I transmembrane protein with an immunoglobulin-like protein domain. It was first discovered in SARS-CoV, the virus that causes severe acute respiratory syndrome (SARS).[2] The homolog in SARS-CoV-2, the virus that causes COVID-19, has about 85% sequence identity to the SARS-CoV protein.[3]
Function
A number of possible functions for the ORF7a protein have been described. The primary function is thought to be immunomodulation and interferon antagonism. The protein is not essential for viral replication.[1]
Viral protein interactions
Studies in SARS-CoV suggest that the protein forms protein-protein interactions with spike protein and ORF3a, and is present in mature virions, making it a minor viral structural protein.[1][4] It is unclear if this occurs in SARS-CoV-2.[5] It may have a role in viral assembly.[1]
Host effects
A number of interactions with host proteins and effects on host cell processes have been described. The SARS-CoV ORF7a protein has been reported to have binding activity to integrin I domains.[6]
It has also been reported to induce apoptosis via a caspase dependent pathway.[1][7] Also, it contains a motif which has been demonstrated to mediate COPII dependent transport out of the endoplasmic reticulum, and the protein is targeted to the Golgi apparatus.[8]
In SARS-CoV-2, ORF7a protein has been described as an effective interferon antagonist.[3] The SARS-CoV-2 protein may have immunomodulatory effects through interaction with monocytes.[5]
Structure
The ORF7a protein is a transmembrane protein with 121 amino acid residues in SARS-CoV-2[5] and 122 in SARS-CoV.[2] It is a type I transmembrane protein with an N-terminal signal peptide, an ectodomain that has an immunoglobulin fold, and a C-terminal endoplasmic reticulum retention signal sequence.[5][6][1] The structure contains seven beta strands which form two beta sheets, arranged in a beta sandwich.[2] Most of the sequence differences between SARS-CoV and SARS-CoV-2 occur in the Ig-like ectodomain and may produce differences in protein-protein interactions.[5]
Post-translational modifications
The SARS-CoV-2 ORF7a protein has been reported to be post-translationally modified by ubiquitination. Polyubiquitin chains attached to lysine 119 may be related to the protein's reported interferon antagonism.[3][9]
Expression and localization
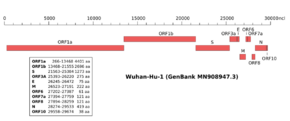 Genomic organisation of isolate Wuhan-Hu-1, the earliest sequenced sample of SARS-CoV-2, indicating the location of ORF7a | |
| NCBI genome ID | 86693 |
|---|---|
| Genome size | 29,903 bases |
| Year of completion | 2020 |
| Genome browser (UCSC) | |
Along with the genes for other viral accessory proteins, the ORF7a gene is located near those encoding the viral structural proteins, at the 5' end of the coronavirus RNA genome.[3] ORF7a is an overlapping gene that overlaps ORF7b.[10] In SARS-CoV, subcellular localization to the endoplasmic reticulum, Golgi apparatus, and ERGIC has been reported,[1] with similar Golgi localization described for SARS-CoV-2.[11]
Evolution
It is thought that ORF8 in SARS-CoV-2, with a similar Ig-like fold, may be a paralog of ORF7a that originated through gene duplication.[12][13]
Many SARS-CoV-2 genomes have been sequenced throughout the COVID-19 pandemic and a number of variations have been reported, including deletion mutations,[14] nonsense mutations (introducing a premature stop codon and truncating the protein),[15] and at least one gene fusion.[16]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Liu, DX; Fung, TS; Chong, KK; Shukla, A; Hilgenfeld, R (September 2014). "Accessory proteins of SARS-CoV and other coronaviruses.". Antiviral Research 109: 97–109. doi:10.1016/j.antiviral.2014.06.013. PMID 24995382.
- ↑ 2.0 2.1 2.2 "Structure and intracellular targeting of the SARS-coronavirus Orf7a accessory protein.". Structure 13 (1): 75–85. 2005. doi:10.1016/j.str.2004.10.010. PMID 15642263.
- ↑ 3.0 3.1 3.2 3.3 Redondo, Natalia; Zaldívar-López, Sara; Garrido, Juan J.; Montoya, Maria (7 July 2021). "SARS-CoV-2 Accessory Proteins in Viral Pathogenesis: Knowns and Unknowns". Frontiers in Immunology 12: 708264. doi:10.3389/fimmu.2021.708264. PMID 34305949.
- ↑ Huang, Cheng; Ito, Naoto; Tseng, Chien-Te K.; Makino, Shinji (August 2006). "Severe Acute Respiratory Syndrome Coronavirus 7a Accessory Protein Is a Viral Structural Protein". Journal of Virology 80 (15): 7287–7294. doi:10.1128/JVI.00414-06. PMID 16840309.
- ↑ 5.0 5.1 5.2 5.3 5.4 Zhou, Ziliang; Huang, Chunliu; Zhou, Zhechong; Huang, Zhaoxia; Su, Lili; Kang, Sisi; Chen, Xiaoxue; Chen, Qiuyue et al. (March 2021). "Structural insight reveals SARS-CoV-2 ORF7a as an immunomodulating factor for human CD14+ monocytes". iScience 24 (3): 102187. doi:10.1016/j.isci.2021.102187. PMID 33615195. Bibcode: 2021iSci...24j2187Z.
- ↑ 6.0 6.1 "Solution structure of the X4 protein coded by the SARS related coronavirus reveals an immunoglobulin like fold and suggests a binding activity to integrin I domains". J. Biomed. Sci. 13 (3): 281–93. May 2006. doi:10.1007/s11373-005-9043-9. PMID 16328780.
- ↑ "The molecular biology of SARS coronavirus.". Ann N Y Acad Sci 1102 (1): 26–38. 2007. doi:10.1196/annals.1408.002. PMID 17470909. Bibcode: 2007NYASA1102...26S.
- ↑ "Structure, expression, and intracellular localization of the SARS-CoV accessory proteins 7a and 7b.". Adv Exp Med Biol. Advances in Experimental Medicine and Biology 581: 115–20. 2006. doi:10.1007/978-0-387-33012-9_20. ISBN 978-0-387-26202-4. PMID 17037516.
- ↑ Cao, Zengguo; Xia, Hongjie; Rajsbaum, Ricardo; Xia, Xianzhu; Wang, Hualei; Shi, Pei-Yong (March 2021). "Ubiquitination of SARS-CoV-2 ORF7a promotes antagonism of interferon response". Cellular & Molecular Immunology 18 (3): 746–748. doi:10.1038/s41423-020-00603-6. PMID 33473190.
- ↑ Pekosz, Andrew; Schaecher, Scott R.; Diamond, Michael S.; Fremont, Daved H.; Sims, Amy C.; Baric, Ralph S. (2006). "Structure, Expression, and Intracellular Localization of the SARS-CoV Accessory Proteins 7a and 7b". The Nidoviruses. Advances in Experimental Medicine and Biology 581: 115–120. doi:10.1007/978-0-387-33012-9_20. ISBN 978-0-387-26202-4. PMID 17037516.
- ↑ Zhang, Jing; Cruz-cosme, Ruth; Zhuang, Meng-Wei; Liu, Dongxiao; Liu, Yuan; Teng, Shaolei; Wang, Pei-Hui; Tang, Qiyi (December 2020). "A systemic and molecular study of subcellular localization of SARS-CoV-2 proteins". Signal Transduction and Targeted Therapy 5 (1): 269. doi:10.1038/s41392-020-00372-8. PMID 33203855.
- ↑ Mariano, Giuseppina; Farthing, Rebecca J.; Lale-Farjat, Shamar L. M.; Bergeron, Julien R. C. (17 December 2020). "Structural Characterization of SARS-CoV-2: Where We Are, and Where We Need to Be". Frontiers in Molecular Biosciences 7: 605236. doi:10.3389/fmolb.2020.605236. PMID 33392262.
- ↑ Neches, Russell Y.; Kyrpides, Nikos C.; Ouzounis, Christos A. (23 February 2021). "Atypical Divergence of SARS-CoV-2 Orf8 from Orf7a within the Coronavirus Lineage Suggests Potential Stealthy Viral Strategies in Immune Evasion". mBio 12 (1). doi:10.1128/mBio.03014-20. PMID 33468697.
- ↑ Holland, LaRinda A.; Kaelin, Emily A.; Maqsood, Rabia; Estifanos, Bereket; Wu, Lily I.; Varsani, Arvind; Halden, Rolf U.; Hogue, Brenda G. et al. (July 2020). "An 81-Nucleotide Deletion in SARS-CoV-2 ORF7a Identified from Sentinel Surveillance in Arizona (January to March 2020)". Journal of Virology 94 (14): e00711-20. doi:10.1128/JVI.00711-20. PMID 32357959.
- ↑ Nemudryi, Artem; Nemudraia, Anna; Wiegand, Tanner; Nichols, Joseph; Snyder, Deann T.; Hedges, Jodi F.; Cicha, Calvin; Lee, Helen et al. (June 2021). "SARS-CoV-2 genomic surveillance identifies naturally occurring truncation of ORF7a that limits immune suppression". Cell Reports 35 (9): 109197. doi:10.1016/j.celrep.2021.109197. PMID 34043946.
- ↑ Addetia, Amin; Xie, Hong; Roychoudhury, Pavitra; Shrestha, Lasata; Loprieno, Michelle; Huang, Meei-Li; Jerome, Keith R.; Greninger, Alexander L. (August 2020). "Identification of multiple large deletions in ORF7a resulting in in-frame gene fusions in clinical SARS-CoV-2 isolates". Journal of Clinical Virology 129: 104523. doi:10.1016/j.jcv.2020.104523. PMID 32623351.

