Biology:Abscopal effect
The abscopal effect is a hypothesis in the treatment of metastatic cancer whereby shrinkage of untreated tumors occurs concurrently with shrinkage of tumors within the scope of the localized treatment. R.H. Mole proposed the term “abscopal” (‘ab’ - away from, ‘scopus’ - target) in 1953 to refer to effects of ionizing radiation “at a distance from the irradiated volume but within the same organism.”[1]
Initially associated with single-tumor, localized radiation therapy, the term “abscopal effect” has also come to encompass other types of localized treatments such as electroporation and intra-tumoral injection of therapeutics.[2] However, the term should only be used when truly local treatments result in systemic effects. For instance, chemotherapeutics commonly circulate through the blood stream and therefore exclude the possibility of any abscopal response.
The mediators of the abscopal effect of radiotherapy were unknown for decades. In 2004, it was postulated for the first time that the immune system might be responsible for these “off-target” anti-tumor effects.[3] Various studies in animal models of melanoma,[4][5] mammary,[5][6] and colorectal tumors[5][7] have substantiated this hypothesis. Abscopal effects of Targeted intraoperative radiotherapy have been seen in clinical studies, including in randomized trials where women treated with lumpectomy for breast cancer combined with whole breast radiotherapy showed reduced mortality from non-breast-cancer causes when compared with whole breast radiotherapy.[8][9] Furthermore, immune-mediated abscopal effects were also described in patients with metastatic cancer.[10] Whereas these reports were extremely rare throughout the 20th century, the clinical use of immune checkpoint blocking antibodies such as ipilimumab or pembrolizumab has greatly increased the number of abscopally responding patients in selected groups of patients such as those with metastatic melanoma [11][12] or lymphoma.[13]
Mechanisms
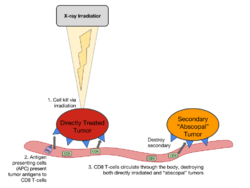
Similar to immune reactions against antigens from bacteria or viruses, the abscopal effect requires priming of immune cells against tumor antigens.[10] Local irradiation of a tumor nodule may lead to immunogenic forms of tumor cell death and liberation of tumor cell-derived antigens. These antigens can be recognized and processed by antigen-presenting cells within the tumor (dendritic cells and macrophages). Cytotoxic T cells which recognize these tumor antigens may in turn be primed by the tumor antigen-presenting cells. In contrast to the local effect of irradiation on the tumor cells, these cytotoxic T cells circulate through the blood stream and are thus able to destroy remaining tumor cells in distant parts of the body which were not irradiated. Accordingly, increases in tumor-specific cytotoxic T cells were shown to correlate with abscopal anti-tumor responses in patients.[11] Vice versa, the abscopal effect is abolished after experimental depletion of T cells in various animal models.[5][14]
Abscopal effects of ionizing radiation are often blocked by the immunosuppressive microenvironment inside the irradiated tumor which prevents effective T cell priming. This explains why the effect is so rarely seen in patients receiving radiotherapy alone. In contrast, the combination of immunomodulatory drugs such as ipilimumab and pembrolizumab can partially reconstitute systemic anti-tumor immune reactions induced after local tumor radiotherapy.[4] The optimal combination of radiation dose and fractionation with immunomodulatory drugs is currently under intensive investigation. In this context, it was proposed that radiation doses above 10 to 12 Gray might be ineffective in inducing immunogenic forms of cell death.[15] However, there is so far no consensus on the optimal radiation regimen needed to increase the chance of abscopal tumor regression.
References
- ↑ Mole, R. H. "Whole body irradiation—radiobiology or medicine? The British Journal of Radiology 26.305 (1953): 234-241.
- ↑ Fend L, Yamazaki T, Remy C, et al. Immune Checkpoint Blockade, Immunogenic Chemotherapy or IFN-α Blockade Boost the Local and Abscopal Effects of Oncolytic Virotherapy. Cancer Res. 2017;77:4146-4157.
- ↑ Demaria S, Ng B, Devitt ML, et al. Ionizing radiation inhibition of distant untreated tumors (abscopal effect) is immune mediated. Int J Radiat Oncol Biol Phys. 2004;58:862‐870.
- ↑ 4.0 4.1 Twyman-Saint Victor C, Rech AJ, Maity A, et al. Radiation and dual checkpoint blockade activate non-redundant immune mechanisms in cancer. Nature. 2015;520:373-377.
- ↑ 5.0 5.1 5.2 5.3 Rodriguez-Ruiz ME, Rodriguez I, Garasa S, et al. Abscopal effects of radiotherapy are enhanced by combined immunostimulatory mabs and are dependent on CD8 T cells and crosspriming. Cancer Res. 2016;76:5994-6005.
- ↑ Demaria S, Kawashima N, Yang AM, et al. “Immune-mediated inhibition of metastases after treatment with local radiation and CTLA-4 blockade in a mouse model of breast cancer. Clin Cancer Res. 2005;11:728‐734.
- ↑ Dovedi SJ, Cheadle EJ, Popple A, et al. “Fractionated radiation therapy stimulates anti-tumor immunity mediated by both resident and infiltrating polyclonal T-cell populations when combined with PD1 blockade. Clin Cancer Res. 2017; 23(18); 5514-26.
- ↑ Kolberg, Hans‑Christian; Loevey, Gyoergy; Akpolat-Basci, Leyla; Stephanou, Miltiades; Fasching, Peter A; Untch, Michael; Liedtke, Cornelia; Bulsara, Max et al. (January 2017). "Targeted intraoperative radiotherapy tumour bed boost during breast-conserving surgery after neoadjuvant chemotherapy" (in en). Strahlentherapie und Onkologie 193 (1): 62–69. doi:10.1007/s00066-016-1072-y. ISSN 0179-7158. PMID 27858093. http://link.springer.com/10.1007/s00066-016-1072-y.
- ↑ Vaidya, Jayant S.; Bulsara, Max; Baum, Michael; Wenz, Frederik; Massarut, Samuele; Pigorsch, Steffi; Alvarado, Michael; Douek, Michael et al. (2021-05-25). "New clinical and biological insights from the international TARGIT-A randomised trial of targeted intraoperative radiotherapy during lumpectomy for breast cancer" (in en). British Journal of Cancer 125 (3): 380–389. doi:10.1038/s41416-021-01440-8. ISSN 1532-1827. PMID 34035435.
- ↑ 10.0 10.1 "Abscopal, immunological effects of radiotherapy: Narrowing the gap between clinical and preclinical experiences". Immunol Rev 280 (1): 249–279. Oct 17, 2017. doi:10.1111/imr.12573. PMID 29027221. https://epub.ub.uni-muenchen.de/50704/1/Brix-2017-Abscopal-immunological-effects-of-r.pdf.
- ↑ 11.0 11.1 "Immunologic correlates of the abscopal effect in a patient with melanoma". N Engl J Med 366 (10): 925–31. Mar 8, 2012. doi:10.1056/NEJMoa1112824. PMID 22397654.
- ↑ Hiniker SM, Reddy SA, Maecker HT, et al. A prospective clinical trial combining radiation therapy with systemic immunotherapy in metastatic melanoma. Int J Radiat Oncol Biol Phys. 2016;96:578-588.
- ↑ Perrone, Salvatore; Lopedote, Paolo; De Sanctis, Vitaliana; Iamundo De Cumis, Ilenia; Pulsoni, Alessandro; Strati, Paolo (2023-05-13). "Novel Drugs and Radiotherapy in Relapsed Lymphomas: Abscopal Response and Beyond" (in en). Cancers 15 (10): 2751. doi:10.3390/cancers15102751. ISSN 2072-6694.
- ↑ Vanpouille-Box C, Diamond JM, Pilones KA, et al. TGFbeta is a master regulator of radiation therapy-induced antitumor immunity. Cancer Res. 2015;75:2232-2242.
- ↑ Vanpouille-Box C, Alard A, Aryankalayil MJ, et al. DNA exonuclease Trex1 regulates radiotherapy-induced tumour immunogenicity. Nat Commun. 2017 Jun 9;8:15618.
 |