Medicine:Heterotopic ossification
| Heterotopic ossification | |
|---|---|
 | |
| Symptoms | localized pain, decreased range of motion, redness, swelling, warmth |
| Risk factors | joint replacement, traumatic brain injury, spinal cord injury, full body burns |
| Diagnostic method | bone scan, x-ray, CT scan, ultrasound, MRI |
| Treatment | physical therapy, NSAIDs, bisphosphonates, radiation, surgery |
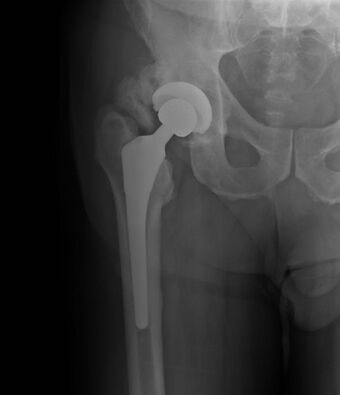
Heterotopic ossification (HO) is the abnormal process by which bone tissue forms outside of the skeleton in muscles and soft tissue. It forms following a traumatic injury, neurogenic injury, or genetic predisposition. The likelihood and severity of HO is linked to the severity of the injury. The most common sites of developing HO are the hip, knee, elbow and shoulder. While the exact mechanism of how HO develops is not known, it is believed to be a result of an abnormal muscle repair system, abnormal neurologic healing response below the level of injury, an abnormal inflammatory response, or a combination of them.[1]
Heterotopic ossification presents differently in different stages. In the initial inflammatory stage, there is pain, redness, swelling, warmth, generalized tenderness; this can mimic other more serious medical conditions and should require urgent evaluation.[2] In the late stage, there is more localized pain, decreased range of motion, and underlying tissue damage and complications. There are various blood or urine tests that can be useful in helping predict HO, but there is not one single gold standard lab.[3] Triple bone scan, X-rays and CT scans are the most useful and reliable imaging studies to rule out other similar medical conditions and confirm the diagnosis of HO.[4]
Heterotopic ossification does not have a single treatment to prevent its development or cure its progression. The goal of management should be to control pain, prevent long term complications, and allow the patient to continue to perform their own daily activities of living. This can be achieved through an array of options, ranging from physical therapy to prophylactic radiation and medications to surgical interventions.[1]
Epidemiology
Heterotopic ossification (HO) is a result of one of three initial insults: a traumatic injury, a neurogenic injury, or a genetic predisposition. It is more common in men (3:2 male to female ratio),[1] likely a result of increased muscle mass, increased physical activity, and hormonal signally pathways. It is also more commonly in those that suffer from prolonged intubation,[5] likely from an anoxic brain injury or prolonged immobilization. It is a hard diagnosis to make due to its overlap in symptoms with other common conditions.[6]
In patients that suffered a forearm fracture, 20% of patients will likely develop HO as a complication.[7] In patients that suffered a femoral shaft fracture, that percentage jumps to 52% of patients.[7] However, HO is even more common in military members that suffered combat related injuries. Military patients that suffered any combat related trauma were likely to have HO as a complication 68% of the time; that number increases to 86% if they had a concomitant traumatic brain injury with their orthopedic injury.[8]
Without a specific trauma or inciting event, patients will frequently develop arthritis in major joints (knees, hips and shoulders). This subjects them to eventual surgical treatment or joint replacement. In those patients, their ability to place weight on a joint or move their joint may be limited for a significant period of time. Therefore, this patient population is also subject to developing HO as a surgical complication. It was found that 44% of patients that received either a hip arthroscopy or total hip replacement developed HO.[4]
In patients that develop a lesion or injury to the nerves of their spinal cord, they can develop neurogenic heterotopic ossification. Neurologenic HO effects 20-29% of patients that developed a spinal cord injury (SCI). In an SCI, the spinal level of injury is important to know since complications typically arise distal or below the level of the injury. This is thought to be due to an impaired or abnormal healing response below the injury level. For this reason, the most common sites of HO in the SCI population are the hips and knees.[6]
In patients that develop an injury to their brain, they can also develop neurogenic heterotopic ossification. In traumatic brain injury (TBI) patients, neurogenic HO effects 5-20% of patients, specifically in those that suffered a severe TBI (initial GCS <15).[6] Patients that suffered a TBI due to a blast, commonly military members, have HO as a complication higher than 20% of the time.[6] Similar to SCI patients, TBI patients have HO commonly in sites below the level of neurologic injury. For this reason, the most common sites of HO in the TBI population are the hips, elbows, shoulders, and knees.
In patients that suffer a burn, there are various degrees to the severity of a burn; the depth to the burn and the surface area which the burn covers are two important factors. For HO complications, the surface area is the more influential variable. The likelihood of developing HO as a complication of a burn is between 1-4% if the burn covers at least 30% of the person's body.[4][9] This complication percentage increases as the burn percentage also increases. For burn patients, the most common site of HO is the elbow, likely due to increased motion at the joint to prevent flexure contractures. The elbow is a clinically significant site to monitor since this specific complication of HO can lead to cubital tunnel syndrome; other common, but less likely, sites are the shoulders, knees, forearms, and temporamandibular joint.[4][9]
Presentation of symptoms
While heterotopic ossification is not a direct result of a traumatic injury, it also does not have to present with symptoms. In the population that is symptomatic, it commonly follows a standard progression of symptoms.
Following the initial inciting traumatic or neurologic injury, there is a heightened inflammatory response. An abnormal or prolonged inflammatory response can lead to the early stages of HO.[2] Typically within the first 6 to 12 weeks, symptoms will start to arise; this is considered early HO. Here, immature bone forms within the affect joint or tissue, leading to generalized inflammatory symptoms. This manifests as symptoms of redness, warmth, and swelling (37% of patients), pain (35% of patients), or generalized tenderness and decreased range of motion (49% of patients) in the affected joint or tissue.[4][3] While these symptoms are more annoying than troubling in the context of HO, these symptoms can also be red flag signs for a more serious underlying condition and require medical evaluation.
As time continues, symptoms will typically progress from a more generalized inflammatory response to a localized pain center. This presents as localized tenderness, pain, and painful or decreased range of motion in the tissue or joint affected.[2] This is considered late HO. In all stages, if the abnormal bone formation grows to imping on surrounding structures, complications can arise depending on the structure involved. This can lead to nerve compression, vascular compression, pressure sores, lymphedema, ankylosis and present as pain, numbness, tingling, weakness, swelling, spasticity, decreased range of motion.[2] Presentation of physical exam symptoms will depend on the location and severity of the HO.[4]
Diagnosis
Since heterotopic ossification can present similar to other more serious pathologies, a physical exam alone may not confirm the diagnosis. Utilizing laboratory data and medical imaging together can provide a better picture to rule out more serious conditions and correctly identify the stage and severity of HO.[4]
Labs
Before treatment can begin for heterotopic ossification, more serious conditions must be ruled out. Lab work may begin with a routine complete blood count and comprehensive metabolic panel to monitor blood, immune system, and organ function. With serious conditions ruled out, more specific labs may be ordered to assist in diagnosing the severity and progression of HO. Since HO is an abnormal growth of bone outside the skeletal system, it is theorized that calcium, a major mineral of bones, may be abnormal during different stages of HO. However, tracking calcium is not a reliable method as calcium is strictly hormonally regulated in the body and will not be elevated in HO.[3] Alkaline phosphatase is an enzyme whose activity is linked to bone growth and has been found to be elevated in HO; however, it is not statistically significant in identifying HO alone.[10] However, it was found that in HO patients, alkaline phosphatase was elevated 2 weeks following their initial injury, peaked at 10 weeks post-injury, and returned to baseline by the 18 week post-injury mark.[4][3] Osteocalcin is a hormone produced during bone turnover that is neither sensitive nor specific for HO and cannot accurately predict its occurrence.[10] Understanding that HO is theorized to be a result of increased inflammation, blood inflammatory markers such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) can identify a body's inflammatory state; however, this is not a sensitive marker for HO.[11] While it is not specific to HO, it was found that 12 weeks after a total hip replacement, an ESR above 35mm/hr was a reliable predictor for developing severe HO in patients.[11] Similarly, elevation in creatine kinase (CK) was found to be associated with more aggressive forms of HO.[12] CK is an enzyme found in muscle tissue that, when found in the blood, can lead to believe there is active muscle damage.
In addition to blood work, a urinalysis can identify certain byproducts of HO that a clinician may use to rule in or rule out its diagnosis. A 24 hour urine hydroxyproline measurement can detect if one is building and breaking down bone at an increased rate compared to normal; however, this is not a reliable method to detect HO.[10] Contrasting, a 24 hour urine prostaglandin E2 lab can be elevated in the early stage of HO and will warrant a triple bone scan for further workup.[4][13] While prostaglandin E2 is not specific for HO and is more associated with inflammatory conditions, its elevation has been associated with early HO.
Imaging

While laboratory studies are not reliable for diagnosing heterotopic ossification, medical imaging studies are more sensitive and specific for accurately diagnosing HO. Although it may be the simplest, most inexpensive method, an x-ray will not be helpful during the early stage. The only definitive diagnostic test in the early stage is a bone scan, which will show heterotopic ossification as early as 2.5 weeks post-injury, which is over 2 weeks sooner than detected by x-ray.[4][3] While a bone scan is more specific less than one month post-injury, its use will be dependent on when symptoms begin. If symptoms arise after 4 weeks post-injury, and if the treatment team wants to rule out more serious complications, the team may begin with radiography or a CT scan. Their low cost and ability to detect immature bone formation while also checking for other diagnosis make them a useful tool to aid in the diagnosis.[4] A treatment team may also utilize other imaging techniques such as an ultrasound or MRI to aid in the diagnosis process, more commonly used to rule out more serious, similarly presenting underlying conditions.
When the initial presentation is swelling and increased temperature in a leg, thrombophlebitis or a deep vein clot cannot be ruled out with a clinical exam alone; therefore, ultrasound imaging may be necessary to differentiate.[4] Similarly, osteomyelitis and malignant soft tissue masses can present similarly to HO; in this case, MRI has been found helpful in correctly diagnosis HO.[4]
Classification types
Once heterotopic ossification has been diagnosed via imaging, the next step is assessing its severity and monitoring for progression of symptoms. There have been several classification systems identified, each dependent on the joint affected.[1]
The Brooker Classification System is utilized following total hip replacement to grade HO formation.
| Classification | Description |
|---|---|
| Class 1 | Island of bone within the soft tissue around the hip |
| Class 2 | Bone spurs on the hip or proximal femur, where the distance between the spurs is > 1cm |
| Class 3 | Bone spurs on the hip or proximal femur, where the distance between the spurs is < 1cm |
| Class 4 | Boney fusion of the hip and proximal femur |
The Hastings and Graham Classification System is utilized to grade HO formation at the elbow and forearm.
| Classification | Description |
|---|---|
| Category 1 | Asymptomatic (no functional limitations), HO present on radiographs |
| Category 2 | Symptomatic (functional limitations), HO present on radiography |
| Category 2A | limitations in elbow flexion/extension |
| Category 2B | limitations in forearm pronation/supination |
| Category 2B | limitations in elbow flexion/extension AND forearm pronation/supination |
| Category 3 | Symptomatic (functional limitations), complete boney fusion of the joint on radiograph |
Management
Physical Therapy / Passive Range of Motion
Conservative treatments such as passive range of motion exercises or other mobilization techniques provided by physical therapists or occupational therapists may also assist in preventing HO. For managing heterotopic ossification, there are mixed reviews in the literature about the success and efficacy of physical therapy (PT) and passive range of motion (PROM). In patients that had a total knee replacement, PT and PROM was found to be beneficial in preventing HO three months after surgery.[1] PT was also the superior choice of management to prevent HO in those patients that had a total hip replacement.[1] Patients that suffered a burn injury are encouraged to maintain range of motion in their effected joint to prevent flexure contractures; in these cases, PROM actually increased the likelihood of HO in these patients.[1][2] In those with a neurologic injury (SCI or TBI), PROM alone did not prevent HO, but its utilization with other treatment modalities was found to prevent contractures and maintain mobility.[16] In TBI patients that had HO of a joint, it was found that PROM of the joint did not worsen progression of HO; it was also found that when spasticity was not affecting the muscles of the affected joint, PROM under anesthesia improved joint motion.[17] A review article looked at 114 adult patients retrospectively and suggested that the lower incidence of HO in patients with a very severe TBI may have been due to early intensive physical and occupational therapy in conjunction with pharmacological treatment.[18] Another review article also recommended physiotherapy as an adjunct to pharmacological and medical treatments because passive range of motion exercises may maintain range at the joint and prevent secondary soft tissue contractures, which are often associated with joint immobility.[16]
Medications
NSAIDs
It has often been believed that the use of non-steroidal anti-inflammatory drugs (NSAIDs), specifically indomethacin, will prevent complete fracture healing. However, indomethacin and ibuprofen have shown some effect in preventing recurrence of heterotopic ossification after total hip replacement or spinal cord injury.[16] Therefore, balancing the risk of nonunion and benefits of preventing HO is the skill of NSAID utilization. While indomethacin is the mainstay of NSAID treatment for preventing HO, the FDA does not indicate its use.[1] Indomethacin has been used in early and intermediate stages of HO to limit its formation and progression; indomethacin compared to placebo reduced late HO at a statistically significantly rate.[1] Similar results were found in patients treated with rofecoxib and patients did not report significant side effects.[1] In patients at high-risk for HO following hip surgery, both standardized indomethacin treatment and selective COX-2 inhibitor NSAIDs were found to be equally efficacious as a single dose of radiation to the hip.[2] In SCI patients, NSAIDs were found to be beneficial in preventing HO and had the greatest efficacy when administered early after the incident.[2][19] When comparing SCI patients, prophylactic NSAIDs compared to placebo showed statistically significant lowered incidence of HO in the prophylactic patient population.[20]
Bisphosphonates
Bisphosphonates are the FDA approved medication for prevention and treatment of heterotopic ossification; they work by preventing bone growth in joints and soft tissues.[1] While it is FDA approved for HO, the literature has mixed perspectives on its efficacy. Some research has shown that there is not a clear benefit compared to placebo in preventing HO and that it can delay the symptom onset or could even worsen the HO formation.[2] There is also the risk of delaying bone healing following orthopedic surgery. In addition, there was not statistically significant findings compared to placebo in SCI patients to warrant the use of bisphosphonates as a prophylactic medication.[20] In contrast, other studies found that bisphosphonates were the most effective maintenance therapy,[19] especially in SCI and burn patients.[16] However, in this study, it was theorized that first generation bisphosphonates are more efficacious than subsequent generations due to the subsequent generations underlying mechanism of action affection only bone breakdown and not inhibiting abnormal bone formation.[16]

Radiation therapy
Prophylactic radiation therapy for the prevention of heterotopic ossification has been employed since the 1970s. A variety of doses and techniques have been used. However, higher doses of radiation have not shown statistically significant increase in benefit compared to lower doses of radiation; in fact, higher doses accompany the risk of worsening side effects.[1] Generally, radiation therapy should be delivered as close as practical to the time of surgery. A dose of 7-8 Gray in a single fraction within 24–48 hours of surgery has been used successfully. It was found that a single postoperative prophylactic dose of 700 cGy radiation compared to 400 cGy radiation decreased the incidence of HO from 42% to 25% in total hip replacement patients.[1] Treatment volumes include the peri-articular region, and can be used for hip, knee, elbow, shoulder, jaw or in patients after spinal cord trauma.
Single dose radiation therapy is well tolerated and is cost effective, without an increase in bleeding, infection or wound healing disturbances.[21]
Surgery
The only curative treatment is surgical resection when possible depending on location and size of the heterotopic ossification.[22] However recurrence may occur with rates between 2% and 31% depending on the report.[23] Specific to the TBI population, surgical removal of the abnormal bone was the most effective treatment strategy.[1][19] Additional treatment with bisphosphonate (etidronate) or indomethacin after resection surgery do not significantly reduce the rate of recurrence.[23]
Patho-mechanism
The underlying mechanism by which heterotopic ossification forms is not fully understood but has been studied in a mouse model. In this model, heterotopic ossifications develop after a injury to the central nervous system and muscle, with bone developing exclusively in injured muscles.[22] HO is thought to be caused by abnormal muscle repair. During normal muscle repair, muscle stem cells divide and differentiate to regenerate muscle fibres. This process is controlled by inflammatory cells and support muscle cell growth. A key step during normal muscle repair is the programmed cell death (apoptosis) triggered inflammatory cells to prevent the development of muscle fibrosis.[24] However, following a spinal cord injury, fibro-adipogenic progenitors fail to undergo apoptosis and instead accumulate and differentiate into bone forming osteoblasts.[25] The spinal cord injury stimulates the adrenal glands[26] to release the glucocorticoid corticosterone into the circulation. Excessive corticosterone causes an exaggerated inflammation response in the injured muscle with excessive release of oncostatin M and interleukin-1β.[27] Oncostatin M and interleukin-1 bind to their cognate receptors OSMR[28] and IL1R1[29] expressed by muscle fibro-adipogenic progenitors which in turn promote their proliferation and osteogenic differentiation. In support of this model, treatment with glucocorticoid receptor antagonists such as mifepristone or relacorilant or conditional deletion of the glucocorticoid receptor gene strongly inhibit the development of neurogenic heterotopic ossification after spinal cord injury in this mouse model.[27] Treatment with ruxolitinib, an inhibitor of JAK1 and JAK2 tyrosine kinases, which are activated downstream of OSMR, also reduces neurogenic heterotopic ossification in this model.[30] This mechanism also explains why infections, particularly with gram-negative bacteria, are associated with higher prevalence of neurogenic heterotopic ossifications in victims of traumatic brain and spinal cord injuries.[31][32][33][34] Lipopolysaccharides from gram-negative bacteria worsen heterotopic ossification by binding to their receptor Toll-like receptor 4 expressed by macrophages and muscle fibro-adipogenic progenitors and further increase oncostatin M and interleukin-1β release by macrophages.[34]
There are also rare genetic disorders causing heterotopic ossification such as fibrodysplasia ossificans progressiva (FOP), a condition that causes injured bodily tissues to be replaced by heterotopic bone. Characteristically exhibiting in the big toe at birth, it causes the formation of heterotopic bone throughout the body over the course of the sufferer's life, causing chronic pain and eventually leading to the immobilisation and fusion of most of the skeleton by abnormal growths of bone.[35]
Another rare genetic disorder causing heterotopic ossification is progressive osseous heteroplasia, is a condition characterized by cutaneous or subcutaneous ossification.[36]
See also
- Intramembranous ossification
- Myositis ossificans
- Fibrodysplasia ossificans progressiva
- Progressive osseous heteroplasia
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Xu, Yili; Huang, Mei; He, Wenzhen; He, Chen; Chen, Kaixuan; Hou, Jing; Huang, Min; Jiao, Yurui et al. (2022-01-25). "Heterotopic Ossification: Clinical Features, Basic Researches, and Mechanical Stimulations". Frontiers in Cell and Developmental Biology 10. doi:10.3389/fcell.2022.770931. ISSN 2296-634X. PMID 35145964. PMC 8824234. https://www.frontiersin.org/articles/10.3389/fcell.2022.770931/full.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Meyers, Carolyn; Lisiecki, Jeffrey; Miller, Sarah; Levin, Adam; Fayad, Laura; Ding, Catherine; Sono, Takashi; McCarthy, Edward et al. (April 2019). "Heterotopic Ossification: A Comprehensive Review" (in en). JBMR Plus 3 (4). doi:10.1002/jbm4.10172. ISSN 2473-4039. PMID 31044187. PMC 6478587. https://onlinelibrary.wiley.com/doi/full/10.1002/jbm4.10172.
- ↑ 3.0 3.1 3.2 3.3 3.4 Orzel, J. A., & Rudd, T. G. (1985). Heterotopic bone formation: clinical, laboratory, and imaging correlation. Journal of Nuclear Medicine, 26(2), 125-132.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 Mujtaba, Bilal; Taher, Ahmed; Fiala, Matthew J.; Nassar, Sameh; Madewell, John E.; Hanafy, Abdelrahman K.; Aslam, Rizwan (2019-09-24). "Heterotopic ossification: radiological and pathological review" (in en). Radiology and Oncology 53 (3): 275–284. doi:10.2478/raon-2019-0039. ISSN 1581-3207. PMID 31553710. PMC 6765162. https://www.sciendo.com/article/10.2478/raon-2019-0039.
- ↑ Firoozabadi, Reza; O'Mara, Timothy J.; Swenson, Alan; Agel, Julie; Beck, John D.; Routt, Milton (November 2014). "Risk Factors for the Development of Heterotopic Ossification After Acetabular Fracture Fixation" (in en). Clinical Orthopaedics & Related Research 472 (11): 3383–3388. doi:10.1007/s11999-014-3719-2. ISSN 0009-921X. PMID 24906813. PMC 4182364. https://journals.lww.com/00003086-201411000-00022.
- ↑ 6.0 6.1 6.2 6.3 Brady, Rhys D.; Shultz, Sandy R.; McDonald, Stuart J.; O'Brien, Terence J. (April 2018). "Neurological heterotopic ossification: Current understanding and future directions" (in en). Bone 109: 35–42. doi:10.1016/j.bone.2017.05.015. https://linkinghub.elsevier.com/retrieve/pii/S8756328217301734.
- ↑ 7.0 7.1 Dey, Devaveena; Wheatley, Benjamin M.; Cholok, David; Agarwal, Shailesh; Yu, Paul B.; Levi, Benjamin; Davis, Thomas A. (August 2017). "The traumatic bone: trauma-induced heterotopic ossification" (in en). Translational Research 186: 95–111. doi:10.1016/j.trsl.2017.06.004. PMID 28668522. PMC 6715128. https://linkinghub.elsevier.com/retrieve/pii/S193152441730213X.
- ↑ Forsberg, Jonathan Agner; Pepek, Joseph M; Wagner, Scott; Wilson, Kevin; Flint, James; Andersen, Romney C; Tadaki, Doug; Gage, Frederick A et al. (May 2009). "Heterotopic Ossification in High-Energy Wartime Extremity Injuries: Prevalence and Risk Factors:" (in en). The Journal of Bone and Joint Surgery-American Volume 91 (5): 1084–1091. doi:10.2106/JBJS.H.00792. ISSN 0021-9355. http://journals.lww.com/00004623-200905000-00007.
- ↑ 9.0 9.1 Kornhaber, Rachel; Foster, Nichola; Edgar, Dale; Visentin, Denis; Ofir, Elad; Haik, Josef; Harats, Moti (2017-01-01). "The development and impact of heterotopic ossification in burns: a review of four decades of research" (in en). Scars, Burns & Healing 3. doi:10.1177/2059513117695659. ISSN 2059-5131. PMID 29799559. PMC 5965316. https://journals.sagepub.com/doi/10.1177/2059513117695659.
- ↑ 10.0 10.1 10.2 Mysiw, W J; Tan, J; Jackson, R D (August 1993). "HETEROTOPIC OSSIFICATION". American Journal of Physical Medicine & Rehabilitation 72 (4): 184–187. doi:10.1097/00002060-199308000-00002. ISSN 0894-9115.
- ↑ 11.0 11.1 KJÆRSGAARD-ANDERSEN, PER; ASMUS, STEEN; WISBECH, NIELS; KRISTENSEN, SØREN SKYDT; PEDERSEN, POUL (November 1989). "Erythrocyte Sedimentation Rate and Heterotopic Bone Formation After Cemented Total Hip Arthroplasty". Clinical Orthopaedics and Related Research 248: 189–194. doi:10.1097/00003086-198911000-00030. ISSN 0009-921X.
- ↑ Sherman, Andrew L.; Williams, Joan; Patrick, Lornette; Banovac, Kresimir (January 2003). "The Value Of Serum Creatine Kinase In Early Diagnosis Of Heterotopic Ossification" (in en). The Journal of Spinal Cord Medicine 26 (3): 227–230. doi:10.1080/10790268.2003.11753688. ISSN 1079-0268. https://www.tandfonline.com/doi/full/10.1080/10790268.2003.11753688.
- ↑ Schurch, Brigitte; Capaul, Marcel; Vallotton, Michel B.; Rossier, Alain B. (July 1997). "Prostaglandin E2 measurements: Their value in the early diagnosis of heterotopic ossification in spinal cord injury patients" (in en). Archives of Physical Medicine and Rehabilitation 78 (7): 687–691. doi:10.1016/S0003-9993(97)90074-5. https://linkinghub.elsevier.com/retrieve/pii/S0003999397900745.
- ↑ Hug, Kevin T.; Alton, Timothy B.; Gee, Albert O. (June 2015). "In Brief: Classifications in Brief: Brooker Classification of Heterotopic Ossification After Total Hip Arthroplasty" (in en). Clinical Orthopaedics & Related Research 473 (6): 2154–2157. doi:10.1007/s11999-014-4076-x. ISSN 0009-921X. PMID 25427427. PMC 4419015. https://journals.lww.com/00003086-201506000-00046.
- ↑ Hastings, Hill; Graham, Thomas J. (August 1994). "THE CLASSIFICATION AND TREATMENT OF HETEROTOPIC OSSIFICATION ABOUT THE ELBOW AND FOREARM" (in en). Hand Clinics 10 (3): 417–437. doi:10.1016/S0749-0712(21)01180-X. https://linkinghub.elsevier.com/retrieve/pii/S074907122101180X.
- ↑ 16.0 16.1 16.2 16.3 16.4 Cipriano, Cara A. MD; Pill, Stephan G. MD, MSPT; Keenan, Mary Ann MD. Heterotopic Ossification Following Traumatic Brain Injury and Spinal Cord Injury. Journal of the American Academy of Orthopaedic Surgeons 17(11):p 689-697, November 2009.
- ↑ GARLAND, DOUGLAS E. M.D.; RAZZA, BRUCE E. M.D.; WATERS, ROBERT L. M.D.. Forceful Joint Manipulation in Head-injured Adults with Heterotopic Ossification. Clinical Orthopaedics and Related Research 169():p 133-138, September 1982.
- ↑ Simonsen, L.L., Sonne-Holm, S., Krasheninnikoff, M., Engberg, A.W. (2007). "Symptomatic heterotopic ossification after very severe traumatic brain injury in 114 patients: Incidence and risk factors". Injury, Int. J. Care Injured 38: 1146–1150.
- ↑ 19.0 19.1 19.2 Aubut, Jo-Anne L.; Mehta, Swati; Cullen, Nora; Teasell, Robert W.; ERABI Group; SCIRE Research Team (2011-03-23). "A comparison of heterotopic ossification treatment within the traumatic brain and spinal cord injured population: An evidence based systematic review". NeuroRehabilitation 28 (2): 151–160. doi:10.3233/NRE-2011-0643. PMID 21447915. PMC 3206088. https://journals.sagepub.com/doi/full/10.3233/NRE-2011-0643.
- ↑ 20.0 20.1 Yolcu, Yagiz Ugur; Wahood, Waseem; Goyal, Anshit; Alvi, Mohammed Ali; Reeves, Ronald K.; Qu, Wenchun; Gerberi, Danielle J.; Bydon, Mohamad (June 2020). "Pharmacologic prophylaxis for heterotopic ossification following spinal cord injury: A systematic review and meta-analysi" (in en). Clinical Neurology and Neurosurgery 193. doi:10.1016/j.clineuro.2020.105737. https://linkinghub.elsevier.com/retrieve/pii/S0303846720300809.
- ↑ Principles and Practice of Radiation Oncology Fifth Edition, Perez and Brady, Lippincott pp. 1955–56
- ↑ 22.0 22.1 Genêt, François; Jourdan, Claire; Schnitzler, Alexis; Lautridou, Christine; Guillemot, Didier; Judet, Thierry; Poiraudeau, Serge; Denormandie, Philippe (2011-01-31). Feany, Mel. ed. "Troublesome Heterotopic Ossification after Central Nervous System Damage: A Survey of 570 Surgeries" (in en). PLOS ONE 6 (1). doi:10.1371/journal.pone.0016632. ISSN 1932-6203. PMID 21304993. Bibcode: 2011PLoSO...616632G.
- ↑ 23.0 23.1 Azhideh, Arash; Chansky, Howard; Yousefiasl, Maryam; Haseli, Sara; Mirghaderi, Peyman; Hernandez, Nicholas M.; Elahi, Reza; Nabipoor, Ali et al. (2025-10-24). "Recurrence of neurogenic heterotopic ossification after surgical excision and preventive strategies: A systematic review and meta-analysis" (in en). The Journal of Spinal Cord Medicine: 1–13. doi:10.1080/10790268.2025.2571821. ISSN 1079-0268. PMID 41134066. https://www.tandfonline.com/doi/full/10.1080/10790268.2025.2571821.
- ↑ Lemos, Dario R; Babaeijandaghi, Farshad; Low, Marcela; Chang, Chih-Kai; Lee, Sunny T; Fiore, Daniela; Zhang, Regan-Heng; Natarajan, Anuradha et al. (July 2015). "Nilotinib reduces muscle fibrosis in chronic muscle injury by promoting TNF-mediated apoptosis of fibro/adipogenic progenitors" (in en). Nature Medicine 21 (7): 786–794. doi:10.1038/nm.3869. ISSN 1078-8956. PMID 26053624. https://www.nature.com/articles/nm.3869.
- ↑ Tseng, Hsu-Wen; Girard, Dorothée; Alexander, Kylie A.; Millard, Susan M.; Torossian, Frédéric; Anginot, Adrienne; Fleming, Whitney; Gueguen, Jules et al. (2022-02-25). "Spinal cord injury reprograms muscle fibroadipogenic progenitors to form heterotopic bones within muscles" (in en). Bone Research 10 (1): 22. doi:10.1038/s41413-022-00188-y. ISSN 2095-6231. PMID 35217633.
- ↑ Debaud, Charlotte; Tseng, Hsu-Wen; Chedik, Malha; Kulina, Irina; Genêt, François; Ruitenberg, Marc J.; Levesque, Jean-Pierre (2021-08-01). "Local and Systemic Factors Drive Ectopic Osteogenesis in Regenerating Muscles of Spinal-Cord–Injured Mice in a Lesion-Level–Dependent Manner" (in en). Journal of Neurotrauma 38 (15): 2162–2175. doi:10.1089/neu.2021.0058. ISSN 0897-7151. https://www.liebertpub.com/doi/10.1089/neu.2021.0058.
- ↑ 27.0 27.1 Alexander, Kylie A.; Tseng, Hsu-Wen; Lao, Hong Wa; Girard, Dorothée; Barbier, Valérie; Ungerer, Jacobus P.J.; McWhinney, Brett C.; Samuel, Selwin G. et al. (2024). "A glucocorticoid spike derails muscle repair to heterotopic ossification after spinal cord injury" (in en). Cell Reports Medicine 5 (12). doi:10.1016/j.xcrm.2024.101849. PMID 39657663.
- ↑ Torossian, Frédéric; Guerton, Bernadette; Anginot, Adrienne; Alexander, Kylie A.; Desterke, Christophe; Soave, Sabrina; Tseng, Hsu-Wen; Arouche, Nassim et al. (2017-11-02). "Macrophage-derived oncostatin M contributes to human and mouse neurogenic heterotopic ossifications" (in en). JCI Insight 2 (21). doi:10.1172/jci.insight.96034. ISSN 2379-3708. PMID 29093266.
- ↑ Tseng, Hsu-Wen; Kulina, Irina; Girard, Dorothée; Gueguen, Jules; Vaquette, Cedryck; Salga, Marjorie; Fleming, Whitney; Jose, Beulah et al. (2020-12-01). "Interleukin-1 Is Overexpressed in Injured Muscles Following Spinal Cord Injury and Promotes Neurogenic Heterotopic Ossification" (in en). Journal of Bone and Mineral Research 37 (3): 531–546. doi:10.1002/jbmr.4482. ISSN 0884-0431. PMID 34841579. https://academic.oup.com/jbmr/article/37/3/531-546/7516831.
- ↑ Alexander, Kylie A.; Tseng, Hsu-Wen; Fleming, Whitney; Jose, Beulah; Salga, Marjorie; Kulina, Irina; Millard, Susan M.; Pettit, Allison R. et al. (2019). "Inhibition of JAK1/2 Tyrosine Kinases Reduces Neurogenic Heterotopic Ossification After Spinal Cord Injury". Frontiers in Immunology 10. doi:10.3389/fimmu.2019.00377. ISSN 1664-3224. PMID 30899259.
- ↑ Dizdar, Dilek; Tiftik, Tülay; Kara, Murat; Tunç, Hakan; Ersöz, Murat; Akkuş, Selami (2013). "Risk factors for developing heterotopic ossification in patients with traumatic brain injury" (in en). Brain Injury 27 (7–8): 807–811. doi:10.3109/02699052.2013.775490. ISSN 0269-9052. PMID 23730889. http://www.tandfonline.com/doi/full/10.3109/02699052.2013.775490.
- ↑ Reznik, J. E.; Biros, E.; Marshall, R.; Jelbart, M.; Milanese, S.; Gordon, S.; Galea, M. P. (2014). "Prevalence and risk-factors of neurogenic heterotopic ossification in traumatic spinal cord and traumatic brain injured patients admitted to specialised units in Australia". Journal of Musculoskeletal & Neuronal Interactions 14 (1): 19–28. ISSN 1108-7161. PMID 24583537.
- ↑ Citak, Mustafa; Suero, Eduardo M.; Backhaus, Manuel; Aach, Mirko; Godry, Holger; Meindl, Renate; Schildhauer, Thomas A. (2012). "Risk Factors for Heterotopic Ossification in Patients With Spinal Cord Injury: A Case-Control Study of 264 Patients" (in en). Spine 37 (23): 1953–1957. doi:10.1097/BRS.0b013e31825ee81b. ISSN 0362-2436. PMID 22614800. http://journals.lww.com/00007632-201211010-00005.
- ↑ 34.0 34.1 Salga, Marjorie; Samuel, Selwin G; Tseng, Hsu-Wen; Gatin, Laure; Girard, Dorothée; Rival, Bastien; Barbier, Valérie; Bisht, Kavita et al. (2023). "Bacterial Lipopolysaccharides Exacerbate Neurogenic Heterotopic Ossification Development" (in en). Journal of Bone and Mineral Research 38 (11): 1700–1717. doi:10.1002/jbmr.4905. ISSN 0884-0431. PMID 37602772. https://academic.oup.com/jbmr/article/38/11/1700-1717/7610375.
- ↑ Pignolo, Robert J; Shore, Eileen M; Kaplan, Frederick S (2011). "Fibrodysplasia Ossificans Progressiva: Clinical and Genetic Aspects" (in en). Orphanet Journal of Rare Diseases 6 (1): 80. doi:10.1186/1750-1172-6-80. ISSN 1750-1172. PMID 22133093.
- ↑ Pignolo, Robert; Ramaswamy, Girish; Fong, John; Shore, Eileen; Kaplan, Frederick (January 2015). "Progressive osseous heteroplasia: diagnosis, treatment, and prognosis" (in en). The Application of Clinical Genetics 8: 37–48. doi:10.2147/TACG.S51064. ISSN 1178-704X. PMID 25674011.
External links
| Classification | |
|---|---|
| External resources |
 |
