Medicine:Pressure ulcer
| Pressure ulcer | |
|---|---|
| Other names | Decubitus (plural: decubitūs), or decubitous ulcers, pressure injuries, pressure sores, bedsores |
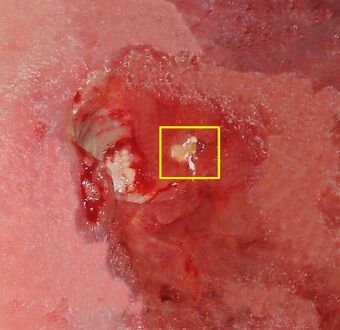 | |
| Stage IV decubitus displaying the tuberosity of the ischium protruding through the tissue, and possible onset of osteomyelitis. | |
| Specialty | Plastic surgery |
| Complications | infection |
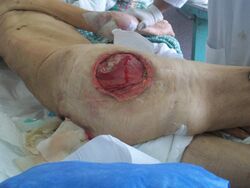
Pressure ulcers, also known as pressure sores, bed sores or pressure injuries, are localised damage to the skin and/or underlying tissue that usually occur over a bony prominence as a result of usually long-term pressure, or pressure in combination with shear or friction. The most common sites are the skin overlying the sacrum, coccyx, heels, and hips, though other sites can be affected, such as the elbows, knees, ankles, back of shoulders, or the back of the cranium.
Pressure ulcers occur due to pressure applied to soft tissue resulting in completely or partially obstructed blood flow to the soft tissue. Shear is also a cause, as it can pull on blood vessels that feed the skin. Pressure ulcers most commonly develop in individuals who are not moving about, such as those who are on chronic bedrest or consistently use a wheelchair. It is widely believed that other factors can influence the tolerance of skin for pressure and shear, thereby increasing the risk of pressure ulcer development. These factors are protein-calorie malnutrition, microclimate (skin wetness caused by sweating or incontinence), diseases that reduce blood flow to the skin, such as arteriosclerosis, or diseases that reduce the sensation in the skin, such as paralysis or neuropathy. The healing of pressure ulcers may be slowed by the age of the person, medical conditions (such as arteriosclerosis, diabetes or infection), smoking or medications such as anti-inflammatory drugs.
Although often prevented and treatable if detected early, pressure ulcers can be very difficult to prevent in critically ill people, frail elders, and individuals with impaired mobility such as wheelchair users (especially where spinal injury is involved). Primary prevention is to redistribute pressure by regularly turning the person. The benefit of turning to avoid further sores is well documented since at least the 19th century.[1] In addition to turning and re-positioning the person in the bed or wheelchair, eating a balanced diet with adequate protein[2] and keeping the skin free from exposure to urine and stool is important.[3]
The rate of pressure ulcers in hospital settings is high; the prevalence in European hospitals ranges from 8.3% to 23%, and the prevalence was 26% in Canadian healthcare settings from 1990 to 2003.[4] In 2013, there were 29,000 documented deaths from pressure ulcers globally, up from 14,000 deaths in 1990.[5]
The United States has tracked rates of pressure injury since the early 2000s. Whittington and Briones reported nationwide rates of pressure injuries in hospitals of 6% to 8%.[6] By the early 2010s, one study showed the rate of pressure injury had dropped to about 4.5% across the Medicare population following the introduction of the International Guideline for pressure injury prevention.[7] Padula and colleagues have witnessed a +29% uptick in pressure injury rates in recent years associated with the rollout of penalizing Medicare policies.[8]
Presentation
Complications
Pressure ulcers can trigger other ailments, cause considerable suffering, and can be expensive to treat. Some complications include autonomic dysreflexia, bladder distension, bone infection, pyarthrosis, sepsis, amyloidosis, anemia, urethral fistula, gangrene and very rarely malignant transformation (Marjolin's ulcer – secondary carcinomas in chronic wounds). Sores may recur if those with pressure ulcers do not follow recommended treatment or may instead develop seromas, hematomas, infections, or wound dehiscence. Paralyzed individuals are the most likely to have pressure sores recur. In some cases, complications from pressure sores can be life-threatening. The most common causes of fatality stem from kidney failure and amyloidosis.
Cause
There are four mechanisms that contribute to pressure ulcer development:[9]
- External (interface) pressure applied over an area of the body, especially over the bony prominences can result in obstruction of the blood capillaries, which deprives tissues of oxygen and nutrients, causing ischemia (deficiency of blood in a particular area), hypoxia (inadequate amount of oxygen available to the cells), edema, inflammation, and, finally, necrosis and ulcer formation. Ulcers due to external pressure occur over the sacrum and coccyx, followed by the trochanter and the calcaneus (heel). In healthy individuals, ulcers caused by external pressure do not occur when the body is stationary, such as during sleep, as involuntary movements of the body frequently occur, allowing for repositioning and the relief of pressure.[10]
- Friction is damaging to the superficial blood vessels directly under the skin. It occurs when two surfaces rub against each other. The skin over the elbows can be injured due to friction. The back can also be injured when patients are pulled or slid over bed sheets while being moved up in bed or transferred onto a stretcher.
- Shearing is a separation of the skin from underlying tissues. When a patient is partially sitting up in bed, skin may stick to the sheet, making the skin susceptible to shearing in case underlying tissues move downward with the body toward the foot of the bed. This may also be possible on a patient who slides down while sitting in a chair.
- Moisture is also a common pressure ulcer culprit. Sweat, urine, feces, or excessive wound drainage can further exacerbate the damage done by pressure, friction, and shear. It can contribute to maceration of surrounding skin thus potentially expanding the deleterious effects of pressure ulcers.
Risk factors
There are over 100 risk factors for pressure ulcers.[11] Factors that may place a patient at risk include immobility, diabetes mellitus, peripheral vascular disease, malnutrition, cerebral vascular accident and hypotension.[11][12] Other factors are age of 70 years and older, current smoking history, dry skin, low body mass index, urinary and fecal incontinence, physical restraints, malignancy, vasopressin prescription, and history of prior pressure injury development.[13]
Pathophysiology
Pressure ulcers may be caused by inadequate blood supply and resulting reperfusion injury when blood re-enters tissue. A simple example of a mild pressure sore may be experienced by healthy individuals while sitting in the same position for extended periods of time: the dull ache experienced is indicative of impeded blood flow to affected areas. Within 2 hours, this shortage of blood supply, called ischemia, may lead to tissue damage and cell death. The sore will initially start as a red, painful area. The other process of pressure ulcer development is seen when pressure is high enough to damage the cell membrane of muscle cells. The muscle cells die as a result and skin fed through blood vessels coming through the muscle die. This is the deep tissue injury form of pressure ulcers and begins as purple intact skin.[14]
According to Centers for Medicare and Medicaid Services, pressure ulcers are one of the eight preventable iatrogenic illnesses. If a pressure ulcer is acquired in the hospital, the hospital will no longer receive reimbursement for the person's care. Hospitals spend about $27 billion annually for treatment of pressure injuries.[15] Whereas, the cost of pressure injury prevention is cost-effective, if not cost-saving, and would cost less than half the amount of resources to prevent compared to treat in health systems.[16]
Sites
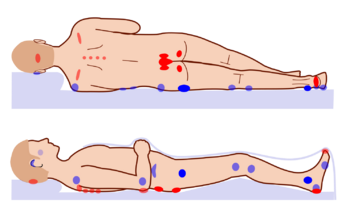
Common pressure sore sites include the skin over the coccyx, the sacrum, the ischia/ischium, the heels of the feet, over the heads of the long bones of the foot, buttocks, over the shoulder, and over the back of the head.[17]
Pressure reduction
Pressure must be removed from high risk body areas by frequent changes in position in bed or chair including turning side to side. Chair cushions and air mattresses should be used for immobile patients. Heels should be off of the bed.
Adequate diet
Eating by mouth is preferred and intake of food and fluid should meet calorie, protein and fluid needs. Work with a dietician if needed. Supplements may be needed.
Biofilm
In order to eliminate this problem, it is imperative to apply antiseptics at once. Hydrogen peroxide (a near-universal toxin) is not recommended for this task as it increases inflammation and impedes healing.[18] Cleaning the open wound with hypochlorous acid is helpful. Dressings with cadexomer iodine, silver, or honey have been shown to penetrate bacterial biofilms. Systemic antibiotics are not recommended in treating local infection in a pressure ulcer, as it can lead to bacterial resistance. They are only recommended if there is evidence of advancing cellulitis, bony infection, or bacteria in the blood.[19]
Diagnosis
Classification

The definitions of the pressure ulcer stages are revised periodically by the National Pressure Injury Advisory Panel (NPIAP)[20] in the United States and the European Pressure Ulcer Advisory Panel (EPUAP) in Europe.[21] Different classification systems are used around the world, depending upon the health system, the health discipline and the purpose for the classifying (e.g. health care versus, prevalence studies versus funding.[22] Briefly, they are as follows:[23][24]
- Stage 1: Intact skin with non-blanchable redness of a localized area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its color may differ from the surrounding area. The area differs in characteristics such as thickness and temperature as compared to adjacent tissue. Stage 1 may be difficult to detect in individuals with dark skin tones. May indicate "at risk" persons (a heralding sign of risk).
- Stage 2: Partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough. May also present as an intact or open/ruptured serum-filled blister. Presents as a shiny or dry shallow ulcer without slough or bruising. This stage should not be used to describe skin tears, tape burns, perineal dermatitis, maceration or excoriation.
- Stage 3: Full thickness tissue loss. Subcutaneous fat may be visible but bone, tendon or muscle are not exposed. Slough may be present but does not obscure the depth of tissue loss. May include undermining and tunneling. The depth of a stage 3 pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput and malleolus do not have (adipose) subcutaneous tissue and stage 3 ulcers can be shallow. In contrast, areas of significant adiposity can develop extremely deep stage 3 pressure ulcers. Bone/tendon is not visible or directly palpable.
- Stage 4: Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present on some parts of the wound bed. Often include undermining and tunneling. The depth of a stage 4 pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput and malleolus do not have (adipose) subcutaneous tissue and these ulcers can be shallow. Stage 4 ulcers can extend into muscle and/or supporting structures (e.g., fascia, tendon or joint capsule) making osteomyelitis likely to occur. Exposed bone/tendon is visible or directly palpable. In 2012, the National Pressure Injury Advisory Panel stated that pressure ulcers with exposed cartilage are also classified as a stage 4.
- Unstageable: Full thickness tissue loss in which actual depth of the ulcer is completely obscured by slough (yellow, tan, gray, green or brown) and/or eschar (tan, brown or black) in the wound bed. Until enough slough and/or eschar is removed to expose the base of the wound, the true depth, and therefore stage, cannot be determined. Stable (dry, adherent, intact without erythema or fluctuance) eschar on the heels is normally protective and should not be removed.
- Deep Tissue Pressure Injury (formerly suspected deep tissue injury): Intact or non-intact skin with localized area of persistent non-blanchable deep red, maroon, purple discoloration or epidermal separation revealing a dark wound bed or blood filled blister. Pain and temperature change[25][26][27][28][29][30][31] often precede skin color changes. Discoloration may appear differently in darkly pigmented skin. This injury results from intense and/or prolonged pressure and shear forces at the bone-muscle interface. The wound may evolve rapidly to reveal the actual extent of tissue injury, or may resolve without tissue loss. If necrotic tissue, subcutaneous tissue, granulation tissue, fascia, muscle or other underlying structures are visible, this indicates a full thickness pressure injury (Unstageable, Stage 3 or Stage 4). Do not use DTPI to describe vascular, traumatic, neuropathic, or dermatologic conditions.[32]
The term medical device related pressure ulcer refers to a cause rather than a classification. Pressure ulcers from a medical device are classified according to the same classification system being used for pressure ulcers arising from other causes, but the cause is usually noted. Pressure injury from medical devices on mucous membranes should not be staged.
Ischemic fasciitis
Ischemic fasciitis (IF) is a benign tumor in the class of fibroblastic and myofibroblastic tumors[33] that, like pressure ulcers, may develop in elderly, bed-ridden individuals.[34] These tumors commonly form in the subcutaneous tissues (i.e. lower most tissue layer of the skin) that overlie bony protuberances such as those in or around the hip, shoulder, greater trochanter of the femur, iliac crest, lumbar region, or scapular region.[35] IF tumors differ from pressure ulcers in that they typically do not have extensive ulcerations of the skin and on histopathological microscopic analysis lack evidence of acute inflammation as determined by the presence of various types of white blood cells.[36] These tumors are commonly treated by surgical removal.[37]
Prevention
There are various approaches that are used widely for preventing pressure ulcers.[38] Suggested approaches include modifications to bedding and mattresses, different support systems for taking pressure off of affected areas, airing of surfaces of the body, skin care, nutrition, and organizational modifications (for example, changing the care routines in hospitals or homes where people require extended bedrest).[38][39] Overall, unbiased clinical studies to determine the effectiveness of these types of interventions and to determine the most effective intervention are needed in order to best prevent pressure ulcers.[38][40][41][42][43]
Clinical guidelines for preventing pressure ulcers
Numerous evidence-based and expert consensus-based clinical guidelines have been to developed to help guide medical professionals internationally[22] and in specific countries including the UK.[44][45][46] The Standardized Pressure Injury Prevention Protocol (SPIPP) Checklist is a derivative of the International Guideline that was designed to facilitate consistent implementation of pressure injury prevention.[47] In 2022, United States Congress passed legislation updating the Military Construction and Veterans Affairs and Related Agencies Appropriations Act, 2015 (H.R. 4355) to establish the SPIPP Checklist as law that United States Department of Veterans Affairs (VA) facilities should adhere to in order to keep patients safe from harm.
Risk assessment
Before turning and repositioning a person, a risk assessment tool is suggested to determine what is the best approach for preventing pressure ulcers in that person. Some of the most common risk assessment tools are the Braden Scale, Norton, or Waterlow tools. The type of risk assessment tool that is used, will depend on which hospital the patient is admitted to and the location. After the risk assessment tool is used, a plan will be developed for the patient individually to prevent Hospital-Acquired Pressure Injuries. This plan will consist of different turning and repositioning strategies. These risk assessment tools provide the nursing staff with a baseline for each patient regarding their individual risk for acquiring a pressure injury. Factors that contribute to these risk assessment tools are moisture, activity, and mobility. These factors are considered and scored using the scale being used, whether it be the Braden, Norton, or Waterlow scale. The numbers are then added up and based on that final number, a score will be given and appropriate measures will be taken to ensure that the patient is being properly repositioned. Unfortunately, this is not always completed in hospitals like it should be.[48]
Efforts in the United States and South Korea have sought to automate risk assessment and classification by training machine learning models on electronic health records.[49][50][51]
Redistribution of pressure
An important aspect of care for most people at risk for pressure ulcers and those with bedsores is the redistribution of pressure so that no pressure is applied to the pressure ulcer.[52] In the 1940s Ludwig Guttmann introduced a program of turning paraplegics every two hours thus allowing bedsores to heal. Previously such individuals had a two-year life-expectancy, normally succumbing to blood and skin infections. Guttmann had learned the technique from the work of Boston physician Donald Munro.[53] There is lack of evidence on prevention of pressure ulcer whether the patient is put in 30 degrees position or at the standard 90 degrees position.[54]
Various interventions have been developed to redistribute pressure including the use of different bed mattresses, support surfaces, and the use of static chairs.
Support surfaces
The use of different types of mattresses including high density foam, surfaces with reactive fibers or gels in them, and surfaces that incorporate reactive water are sometimes suggested to redistribute pressure. The evidence supporting these interventions and whether they prevent new ulcers, increase the comfort level, or have other positive or more negative adverse effects is weak.[55][56] Many support surfaces redistribute pressure by immersing and/or enveloping the body into the surface. Some support surfaces, including antidecubitus mattresses and cushions, contain multiple air chambers that are alternately pumped.[57][58] Methods to standardize the products and evaluate the efficacy of these products have only been developed in recent years through the work of the S3I within NPUAP.[59]
There is some evidence that the use of foam mattresses is not as effective as support approaches that include alternating pressure air surfaces or reactive surfaces.[60][61] It is not clear if interventions that include a reactive air surface are more effective than reactive surfaces that include water or gel or other substrates.[62][63] In addition, the effectiveness of sheepskin overlays on top of mattresses is not clear.[38]
Evidence is uncertain regarding which support surfaces are most effective for pressure ulcer healing. While reactive air surfaces may promote healing more effectively than foam in some cases, the evidence is limited and inconsistent.[38]
Static chairs (as opposed to wheelchairs) have also been suggested for pressure redistribution.[64] Static chairs can include: standard hospital chairs; chairs with no cushions or manual/dynamic function; and chairs with integrated pressure redistributing surfaces and recline, rise or tilt functions. More research is needed to establish how effective pressure redistributing static chairs are for preventing pressure ulcers.[64]
For individuals with limited mobility, pressure shifting on a regular basis and using a wheelchair cushion featuring pressure relief components can help prevent pressure wounds.[65]
Nutrition
The benefits of nutritional interventions with various compositions for pressure ulcer prevention are uncertain.[66] The International Guideline on Pressure Injury Prevention and Treatment lists evidence-based recommendations for prevention of pressure injury and their treatment.[citation needed]
Organisational changes
There is some suggestion that organisational changes may reduce incidence of pressure ulcers, with healthcare professionals central to the prevention of pressure ulcers in both hospital[67] and community settings.[68] It is not clear from studies on the effectiveness of these approaches as to the best organisational change that would benefit those at risk of pressure ulcers including organisation of health services,[39] risk assessment tools,[69] wound care teams,[70] and education.[71][72] This is largely due to the lack of high-quality research in these areas.
Wound care and dressings
Caring for wounds and ulcers that have been started and the use of creams are also considerations in preventing worsening to ulcers and new primary ulcers. It is unclear if creams containing fatty acids are effective in reducing incidence of pressure ulcers compared to creams without fatty acids.[73] It is also unclear if silicone dressings reduce pressure ulcer incidence.[73] There is no evidence that massage reduces pressure ulcer incidence.[74] Controlling the heat and moisture levels of the skin surface, known as skin microclimate management, may also play a role in the prevention and control of pressure ulcers.[75] Skin care is also important because damaged skin does not tolerate pressure. However, skin that is damaged by exposure to urine or stool is not considered a pressure ulcer. These skin wounds should be classified as Incontinence Associated Dermatitis.
Treatment
Recommendations to treat pressure ulcers include the use of bed rest, pressure redistributing support surfaces, nutritional support, repositioning, wound care (e.g., debridement, wound dressings) and biophysical agents (e.g., electrical stimulation).[46] Reliable scientific evidence to support the use of many of these interventions, though, is lacking. More research is needed to assess how to best support the treatment of pressure ulcers, for example by repositioning.[40][76][42][43]
Debridement
Necrotic tissue should be removed in most pressure ulcers. The heel is an exception in many cases when the limb has an inadequate blood supply. Necrotic tissue is an ideal area for bacterial growth, which has the ability to greatly compromise wound healing. There are five ways to remove necrotic tissue.
- Autolytic debridement is the use of moist dressings to promote autolysis with the body's own enzymes and white blood cells. It is a slow process, but mostly painless, and is most effective in individuals with a properly functioning immune system.
- Biological debridement, or maggot debridement therapy, is the use of medical maggots to feed on necrotic tissue and therefore clean the wound of excess bacteria. Although this fell out of favor for many years, in January 2004, the FDA approved maggots as a live medical device.[77]
- Chemical debridement, or enzymatic debridement, is the use of prescribed enzymes that promote the removal of necrotic tissue.
- Mechanical debridement, is the use of debriding dressings, whirlpool or ultrasound for slough in a stable wound.
- Surgical debridement, or sharp debridement, is the fastest method, as it allows a surgeon to quickly remove dead tissue.
Dressings
It is not clear if one topical agent or dressing is better than another for treating pressure ulcers.[78] There is some evidence to suggest that protease-modulating dressings, foam dressings or collagenase ointment may be better at healing than gauze.[78] The wound dressing should be selected based on the wound and condition of the surrounding skin. There are some studies that indicate that antimicrobial products that stimulate the epithelization may improve the wound healing.[79] However, there is no international consensus on the selection of the dressings for pressure ulcers.[80] Evidence supporting the use of alginate dressings,[81] foam dressings,[82] and hydrogel dressings,[83] and the benefits of these dressings over other treatments is unclear.
Some guidelines for dressing are:[84]
| Condition | Cover dressing |
|---|---|
| None to moderate exudates | Gauze with tape or composite |
| Moderate to heavy exudates | Foam dressing with tape or composite |
| Frequent soiling | Hydrocolloid dressing, film or composite |
| Fragile skin | Stretch gauze or stretch net |
Other treatments
Other treatments include anabolic steroids,[85] medical grade honey,[86] negative pressure wound therapy,[87] phototherapy,[88] pressure relieving devices,[89] reconstructive surgery,[90] support surfaces,[91] ultrasound[92] and topical phenytoin.[93] There is little or no evidence to support or refute the benefits of most of these treatments compared to each other and placebo. It is not clear if electrical stimulation is an effective treatment for pressure ulcers.[94] In addition, the benefit of using systemic or topical antibiotics in the management of pressure ulcer is still unclear.[95] When selecting treatments, consideration should be given to patients' quality of life as well as the interventions' ease of use, reliability, and cost. The benefits of nutritional interventions with various compositions for pressure ulcer treatment are uncertain.[96]
Epidemiology
Each year, more than 2.5 million people in the United States develop pressure ulcers.[97] In acute care settings in the United States, the incidence of bedsores is 0.4% to 38%; within long-term care it is 2.2% to 23.9%, and in home care, it is 0% to 17%. Similarly, there is wide variation in prevalence: 10% to 18% in acute care, 2.3% to 28% in long-term care, and 0% to 29% in home care. There is a much higher rate of bedsores in intensive care units because of immunocompromised individuals, with 8% to 40% of those in the ICU developing bedsores.[98] However, pressure ulcer prevalence is highly dependent on the methodology used to collect the data. Using the European Pressure Ulcer Advisory Panel (EPUAP) methodology there are similar figures for pressure ulcers in acutely sick people in the hospital. There are differences across countries, but using this methodology, pressure ulcer prevalence in Europe was consistently high, from 8.3% (Italy) to 22.9% (Sweden).[99] A recent study in Jordan also showed a figure in this range.[100] Some research shows differences in pressure-ulcer detection among white and black residents in nursing homes.[101]
See also
- Perfusion – systemic biomechanics of blood delivery
References
- ↑ "Pressure ulcers: avoidable or unavoidable? Results of the National Pressure Ulcer Advisory Panel Consensus Conference". Ostomy/Wound Management 57 (2): 24–37. February 2011. PMID 21350270.
- ↑ "Pressure Ulcer and Nutrition". Indian Journal of Critical Care Medicine 22 (4): 283–289. April 2018. doi:10.4103/ijccm.IJCCM_277_17. PMID 29743767.
- ↑ "Review of the Current Management of Pressure Ulcers". Advances in Wound Care 7 (2): 57–67. February 2018. doi:10.1089/wound.2016.0697. PMID 29392094.
- ↑ "Support surfaces for pressure ulcer prevention". The Cochrane Database of Systematic Reviews 2015 (9). September 2015. doi:10.1002/14651858.CD001735.pub5. PMID 26333288.
- ↑ "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet 385 (9963): 117–171. January 2015. doi:10.1016/S0140-6736(14)61682-2. PMID 25530442.
- ↑ "National Prevalence and Incidence Study: 6-year sequential acute care data". Advances in Skin & Wound Care 17 (9): 490–494. Nov 2004. doi:10.1097/00129334-200411000-00016. PMID 15632743.
- ↑ "Hospital-acquired pressure ulcers: results from the national Medicare Patient Safety Monitoring System study". Journal of the American Geriatrics Society 60 (9): 1603–1608. September 2012. doi:10.1111/j.1532-5415.2012.04106.x. PMID 22985136.
- ↑ "Adverse Effects of the Medicare PSI-90 Hospital Penalty System on Revenue-Neutral Hospital-Acquired Conditions". Journal of Patient Safety 16 (2): e97–e102. June 2020. doi:10.1097/PTS.0000000000000517. PMID 30110019.
- ↑ "Pressure ulcers". BMJ 332 (7539): 472–475. February 2006. doi:10.1136/bmj.332.7539.472. PMID 16497764.
- ↑ "Causes and prevention of pressure sores" (in en). https://www.cancerresearchuk.org/about-cancer/coping/physically/skin-problems/pressure-sores/causes-and-prevention.
- ↑ 11.0 11.1 "Pressure ulcer prevention and management". JAMA 289 (2): 223–226. January 2003. doi:10.1001/jama.289.2.223. PMID 12517234.
- ↑ "Risk factors for pressure sores. A comparison of cross-sectional and cohort-derived data". Journal of the American Geriatrics Society 37 (11): 1043–1050. November 1989. doi:10.1111/j.1532-5415.1989.tb06918.x. PMID 2809051.
- ↑ "Using clinical data to predict high-cost performance coding issues associated with pressure ulcers: a multilevel cohort model". Journal of the American Medical Informatics Association 24 (e1): e95–e102. April 2017. doi:10.1093/jamia/ocw118. PMID 27539199.
- ↑ "Revised National Pressure Ulcer Advisory Panel Pressure Injury Staging System: Revised Pressure Injury Staging System". Journal of Wound, Ostomy, and Continence Nursing 43 (6): 585–597. Nov 2016. doi:10.1097/WON.0000000000000281. PMID 27749790.
- ↑ "The national cost of hospital-acquired pressure injuries in the United States". International Wound Journal 16 (3): 634–640. June 2019. doi:10.1111/iwj.13071. PMID 30693644.
- ↑ "Improving the quality of pressure ulcer care with prevention: a cost-effectiveness analysis". Medical Care 49 (4): 385–392. April 2011. doi:10.1097/MLR.0b013e31820292b3. PMID 21368685.
- ↑ Srb's Manual of Surgery (4 ed.). Jaypee Brother Medical Pub. 2013. p. 21. ISBN 978-93-5025-944-3.
- ↑ "Dealing with Pressure Sores | Pressure Care". 31 January 2017. https://www.airospring.co.uk/blogs/news/dealing-with-pressure-sores.
- ↑ "Pressure ulcers: prevention, evaluation, and management". American Family Physician 78 (10): 1186–1194. November 2008. PMID 19035067. http://www.aafp.org/afp/2008/1115/p1186.html. Retrieved 8 June 2012.
- ↑ "National Pressure Injury Advisory Panel (NPIAP)". http://www.npiap.com/.
- ↑ "European Pressure Ulcer Advisory Panel". http://www.epuap.org/.
- ↑ 22.0 22.1 Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline. The International Guideline (3rd ed.). internationalguideline.com. 2019. ISBN 978-0-6480097-8-8.
- ↑ "Revised National Pressure Ulcer Advisory Panel Pressure Injury Staging System: Revised Pressure Injury Staging System". Journal of Wound, Ostomy, and Continence Nursing 43 (6): 585–597. 2016. doi:10.1097/WON.0000000000000281. PMID 27749790.
- ↑ Prevention and treatment of pressure ulcers. Quick reference guide (Second ed.). Perth, Western Australia: National Pressure Ulcer Advisory Panel (U.S.), European Pressure Ulcer Advisory Panel, Pan Pacific Pressure Injury Alliance. 2014. ISBN 978-0-9579343-6-8. OCLC 945954574.
- ↑ "Using thermography to assess pressure injuries in patients with dark skin". Nursing 48 (9): 60–61. September 2018. doi:10.1097/01.NURSE.0000544232.97340.96. PMID 30134324.
- ↑ "Driving Outcomes and Improving Documentation with Long-Wave Infrared Thermography in a Long-term Acute Care Hospital". Advances in Skin & Wound Care 36 (4): 189–193. April 2023. doi:10.1097/01.ASW.0000912676.73372.a8. PMID 36790265.
- ↑ "Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline". www.internationalguideline.com. https://www.internationalguideline.com/guideline.
- ↑ "Using temperature of pressure-related intact discolored areas of skin to detect deep tissue injury: an observational, retrospective, correlational study". Ostomy/Wound Management 58 (8): 20–31. August 2012. PMID 22879313.
- ↑ "Use of Thermal Imaging to Identify Deep-Tissue Pressure Injury on Admission Reduces Clinical and Financial Burdens of Hospital-Acquired Pressure Injuries". Advances in Skin & Wound Care 32 (7): 312–320. July 2019. doi:10.1097/01.ASW.0000559613.83195.f9. PMID 31192867.
- ↑ "Heat transfer model for deep tissue injury: a step towards an early thermographic diagnostic capability". Diagnostic Pathology 9. February 2014. doi:10.1186/1746-1596-9-36. PMID 24555856.
- ↑ "Early Identification of Deep-Tissue Pressure Injury Using Long-Wave Infrared Thermography: A Blinded Prospective Cohort Study". Advances in Skin & Wound Care 35 (2): 95–101. February 2022. doi:10.1097/01.ASW.0000790448.22423.b0. PMID 34469910.
- ↑ "Revised National Pressure Ulcer Advisory Panel Pressure Injury Staging System: Revised Pressure Injury Staging System". Journal of Wound, Ostomy, and Continence Nursing 43 (6): 585–597. 2016. doi:10.1097/WON.0000000000000281. PMID 27749790.
- ↑ "The 2020 WHO Classification of Soft Tissue Tumours: news and perspectives". Pathologica 113 (2): 70–84. April 2021. doi:10.32074/1591-951X-213. PMID 33179614.
- ↑ "Atypical decubital fibroplasia with unusual histology". APMIS 109 (9): 631–635. September 2001. doi:10.1034/j.1600-0463.2001.d01-185.x. PMID 11878717.
- ↑ "Atypical decubital fibroplasia. A distinctive fibroblastic pseudotumor occurring in debilitated patients". The American Journal of Surgical Pathology 16 (7): 708–715. July 1992. doi:10.1097/00000478-199207000-00009. PMID 1530110.
- ↑ "Ischemic fasciitis: analysis of 44 cases indicating an inconsistent association with immobility or debilitation". The American Journal of Surgical Pathology 32 (10): 1546–1552. October 2008. doi:10.1097/PAS.0b013e31816be8db. PMID 18724246.
- ↑ "Ischemic Fasciitis of the Left Buttock in a 40-Year-Old Woman with Beta-Propeller Protein-Associated Neurodegeneration (BPAN)". The American Journal of Case Reports 19: 1249–1252. October 2018. doi:10.12659/AJCR.911300. PMID 30341275.
- ↑ 38.0 38.1 38.2 38.3 38.4 "Beds, overlays and mattresses for preventing and treating pressure ulcers: an overview of Cochrane Reviews and network meta-analysis". The Cochrane Database of Systematic Reviews 2021 (8). August 2021. doi:10.1002/14651858.CD013761.pub2. PMID 34398473.
- ↑ 39.0 39.1 "Organisation of health services for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2018 (12). December 2018. doi:10.1002/14651858.cd012132.pub2. PMID 30536917.
- ↑ 40.0 40.1 "Bed rest for pressure ulcer healing in wheelchair users". The Cochrane Database of Systematic Reviews 2016 (10). October 2016. doi:10.1002/14651858.CD011999.pub2. PMID 27748506.
- ↑ "Nutritional interventions for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2024 (2). February 2024. doi:10.1002/14651858.CD003216.pub3. PMID 38345088.
- ↑ 42.0 42.1 "Repositioning for treating pressure ulcers". The Cochrane Database of Systematic Reviews 1 (1). January 2015. doi:10.1002/14651858.CD006898.pub4. PMID 25561248.
- ↑ 43.0 43.1 "Wound cleansing for pressure ulcers". The Cochrane Database of Systematic Reviews 2013 (3). March 2013. doi:10.1002/14651858.CD004983.pub3. PMID 23543538.
- ↑ Pressure Ulcer Risk Assessment and Prevention: Recommendations. London: Royal College of Nursing. 2001. ISBN 1-873853-74-2. http://www.rcn.org.uk/__data/assets/pdf_file/0003/78501/001252.pdf. Retrieved 8 October 2021.
- ↑ "Pressure Relief and Wound Care". http://www.independentliving.co.uk/pressure-relief.html. Independent Living (UK)
- ↑ 46.0 46.1 National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel and Pan Pacific Pressure Injury Alliance (2014). Prevention and Treatment of Pressure Ulcers: Quick Reference Guide.. Perth, Australia: Cambridge Media. p. 19. ISBN 978-0-9579343-6-8. http://www.npuap.org/wp-content/uploads/2014/08/Updated-10-16-14-Quick-Reference-Guide-DIGITAL-NPUAP-EPUAP-PPPIA-16Oct2014.pdf. Retrieved 18 October 2016.
- ↑ "The Standardized Pressure Injury Prevention Protocol for improving nursing compliance with best practice guidelines". Journal of Clinical Nursing 28 (3–4): 367–371. February 2019. doi:10.1111/jocn.14691. PMID 30328652.
- ↑ "Pressure injury prevention practices among medical surgical nurses in a tertiary hospital: An observational and chart audit study". International Wound Journal 19 (5): 1165–1179. August 2022. doi:10.1111/iwj.13712. PMID 34729917.
- ↑ "Predictive models for pressure ulcers from intensive care unit electronic health records using Bayesian networks". BMC Medical Informatics and Decision Making 17 (Suppl 2). July 2017. doi:10.1186/s12911-017-0471-z. PMID 28699545.
- ↑ "Predicting the Incidence of Pressure Ulcers in the Intensive Care Unit Using Machine Learning". eGEMs 7 (1): 49. September 2019. doi:10.5334/egems.307. PMID 31534981.
- ↑ "Using EHR data to predict hospital-acquired pressure ulcers: a prospective study of a Bayesian Network model". International Journal of Medical Informatics 82 (11): 1059–1067. November 2013. doi:10.1016/j.ijmedinf.2013.06.012. PMID 23891086.
- ↑ "Pressure ulcers in the intensive care unit: The 'forgotten' enemy.". OPUS 12 Scientist 1 (2): 17–30. 2007.
- ↑ "Guttmann, Sir Ludwig (1899–1980)". Oxford Dictionary of National Biography. Oxford University Press. 2004.
- ↑ "Repositioning for pressure injury prevention in adults". The Cochrane Database of Systematic Reviews 2020 (6). June 2020. doi:10.1002/14651858.CD009958.pub3. PMID 32484259.
- ↑ "Alternating pressure (active) air surfaces for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013620.pub2. PMID 33969911.
- ↑ "Beds, overlays and mattresses for treating pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013624.pub2. PMID 33969896.
- ↑ "Preventing pressure ulcers: choosing a mattress". Professional Nurse 20 (4): 43–46. December 2004. PMID 15624622.
- ↑ "Antidecubitus Why?". Antidecubitus Systems Matfresses Cushions. COMETE s.a.s.. http://www.cometemedicali.it/images/Brochure%20antidecubito%202005%20INGLESE.pdf.
- ↑ "Remote monitoring of sitting behavior of people with spinal cord injury". Journal of Rehabilitation Research and Development 39 (4): 513–520. 2002. PMID 17638148.
- ↑ "Foam surfaces for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013621.pub2. PMID 34097765.
- ↑ "Alternative reactive support surfaces (non-foam and non-air-filled) for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013623.pub2. PMID 34097764.
- ↑ "Reactive air surfaces for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013622.pub2. PMID 33999463.
- ↑ "Alternative reactive support surfaces (non-foam and non-air-filled) for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 5 (5). May 2021. doi:10.1002/14651858.CD013623.pub2. PMID 34097764.
- ↑ 64.0 64.1 "Pressure redistributing static chairs for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 2022 (2). February 2022. doi:10.1002/14651858.CD013644.pub2. PMID 35174477.
- ↑ "A randomized clinical trial on preventing pressure ulcers with wheelchair seat cushions". Journal of the American Geriatrics Society 58 (12): 2308–2314. December 2010. doi:10.1111/j.1532-5415.2010.03168.x. PMID 21070197.
- ↑ "Nutritional interventions for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2024 (2). February 2024. doi:10.1002/14651858.CD003216.pub3. PMID 38345088.
- ↑ "Factors related to knowledge, attitude, and practice of nurses in intensive care unit in the area of pressure ulcer prevention: A multicenter study". Journal of Tissue Viability 29 (2): 76–81. May 2020. doi:10.1016/j.jtv.2020.02.002. PMID 32061501.
- ↑ "Psychosocial factors impacting community-based pressure ulcer prevention: A systematic review". International Journal of Nursing Studies 146. July 2023. doi:10.1016/j.ijnurstu.2023.104561. PMID 37542960. https://e-space.mmu.ac.uk/632911/3/1-s2.0-S0020748923001268-main.pdf.
- ↑ "Risk assessment tools for the prevention of pressure ulcers". The Cochrane Database of Systematic Reviews 1 (1). January 2019. doi:10.1002/14651858.cd006471.pub4. PMID 30702158.
- ↑ "Wound-care teams for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2015 (9). September 2015. doi:10.1002/14651858.cd011011.pub2. PMID 26373268.
- ↑ "Education of healthcare professionals for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 2018 (5). May 2018. doi:10.1002/14651858.cd011620.pub2. PMID 29800486.
- ↑ "Patient and lay carer education for preventing pressure ulceration in at-risk populations". The Cochrane Database of Systematic Reviews 2 (2). February 2021. doi:10.1002/14651858.cd012006.pub2. PMID 33625741.
- ↑ 73.0 73.1 "Dressings and topical agents for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 2024 (12). December 2024. doi:10.1002/14651858.CD009362.pub4. PMID 39625073.
- ↑ "Massage therapy for preventing pressure ulcers". The Cochrane Database of Systematic Reviews 2015 (6). June 2015. doi:10.1002/14651858.cd010518.pub2. PMID 26081072.
- ↑ "Hill-Rom Clinical Resource Center". https://library.hill-rom.com/browse?jobid=142.
- ↑ "Nutritional interventions for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2014 (6). June 2014. doi:10.1002/14651858.CD003216.pub2. PMID 24919719.
- ↑ "510(k)s Final Decisions Rendered for January 2004: Device: Medical Maggots". FDA. https://www.fda.gov/cdrh/510k/sumjan04.html.
- ↑ 78.0 78.1 "Dressings and topical agents for treating pressure ulcers". The Cochrane Database of Systematic Reviews 6 (6). June 2017. doi:10.1002/14651858.CD011947.pub2. PMID 28639707.
- ↑ "Beneficial effect of resin salve in treatment of severe pressure ulcers: a prospective, randomized and controlled multicentre trial". The British Journal of Dermatology 158 (5): 1055–1062. May 2008. doi:10.1111/j.1365-2133.2008.08461.x. PMID 18284391.
- ↑ "Dressings and topical agents for treating pressure ulcers". The Cochrane Database of Systematic Reviews 6 (6). June 2017. doi:10.1002/14651858.CD011947.pub2. PMID 28639707.
- ↑ "Alginate dressings for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2015 (5). May 2015. doi:10.1002/14651858.cd011277.pub2. PMID 25994366.
- ↑ "Foam dressings for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2017 (10). October 2017. doi:10.1002/14651858.cd011332.pub2. PMID 29025198.
- ↑ "Hydrogel dressings for treating pressure ulcers". The Cochrane Database of Systematic Reviews (John Wiley & Sons, Ltd) 2015 (2). February 2015. doi:10.1002/14651858.cd011226. PMID 25914909.
- ↑ "Wound and Pressure Ulcer Management". Johns Hopkins University. http://www.hopkinsmedicine.org/gec/series/wound_care.html.
- ↑ "Anabolic steroids for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2017 (6). June 2017. doi:10.1002/14651858.cd011375.pub2. PMID 28631809.
- ↑ "Use of Medical-Grade Honey to Treat Clinically Infected Heel Pressure Ulcers in High-Risk Patients: A Prospective Case Series". Antibiotics 12 (3): 605. March 2023. doi:10.3390/antibiotics12030605. PMID 36978472.
- ↑ "Negative pressure wound therapy for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2023 (5). May 2023. doi:10.1002/14651858.CD011334.pub3. PMID 37232410.
- ↑ "Phototherapy for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2014 (7). July 2014. doi:10.1002/14651858.cd009224.pub2. PMID 25019295.
- ↑ "Pressure-relieving devices for treating heel pressure ulcers". The Cochrane Database of Systematic Reviews 2014 (2). February 2014. doi:10.1002/14651858.cd005485.pub3. PMID 24519736.
- ↑ "Reconstructive surgery for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2022 (10). October 2022. doi:10.1002/14651858.CD012032.pub3. PMID 36228111.
- ↑ "Support surfaces for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2018 (10). October 2018. doi:10.1002/14651858.cd009490.pub2. PMID 30307602.
- ↑ "Therapeutic ultrasound for pressure ulcers". The Cochrane Database of Systematic Reviews (3). July 2006. doi:10.1002/14651858.cd001275.pub2. PMID 16855964.
- ↑ "Topical phenytoin for treating pressure ulcers". The Cochrane Database of Systematic Reviews 2017 (2). February 2017. doi:10.1002/14651858.cd008251.pub2. PMID 28225152.
- ↑ "Electrical stimulation for treating pressure ulcers". The Cochrane Database of Systematic Reviews 1 (1). January 2020. doi:10.1002/14651858.CD012196.pub2. PMID 31962369.
- ↑ "Antibiotics and antiseptics for pressure ulcers". The Cochrane Database of Systematic Reviews 4 (4). April 2016. doi:10.1002/14651858.CD011586.pub2. PMID 27040598.
- ↑ "Nutritional interventions for preventing and treating pressure ulcers". The Cochrane Database of Systematic Reviews 2024 (2). February 2024. doi:10.1002/14651858.CD003216.pub3. PMID 38345088.
- ↑ Agency for Healthcare Research and Quality. "Preventing Pressure Ulcers in Hospitals". http://www.ahrq.gov/research/ltc/pressureulcertoolkit/.
- ↑ "Pressure ulcers in America: prevalence, incidence, and implications for the future. An executive summary of the National Pressure Ulcer Advisory Panel monograph". Advances in Skin & Wound Care 14 (4): 208–215. 2001. doi:10.1097/00129334-200107000-00015. PMID 11902346.
- ↑ "Pressure ulcer prevalence in Europe: a pilot study". Journal of Evaluation in Clinical Practice 13 (2): 227–235. April 2007. doi:10.1111/j.1365-2753.2006.00684.x. PMID 17378869.
- ↑ "Do risk assessment scales for pressure ulcers work?". Journal of Tissue Viability 19 (4): 132–136. November 2010. doi:10.1016/j.jtv.2009.11.006. PMID 20036124.
- ↑ "Association of race and sites of care with pressure ulcers in high-risk nursing home residents". JAMA 306 (2): 179–186. July 2011. doi:10.1001/jama.2011.942. PMID 21750295.
Further reading
- "Pressure Ulcers: A Patient Safety Issue". Patient Safety and Quality: An Evidence-Based Handbook for Nurses.. Advances in Patient Safety. Rockville (MD): Agency for Healthcare Research and Quality (US). April 2008. https://www.ncbi.nlm.nih.gov/books/NBK2650/.
- "Risk assessment and prevention of pressure ulcers: a clinical practice guideline from the American College of Physicians". Annals of Internal Medicine 162 (5): 359–369. March 2015. doi:10.7326/M14-1567. PMID 25732278.
External links
| Classification | |
|---|---|
| External resources |
Template:Cutaneous ketatosis, ulcer, atrophy, necrobiosis, and vasculitis
 |
