Biology:Mechanotransduction
In cellular biology, mechanotransduction (mechano + transduction) is any of various mechanisms by which cells convert mechanical stimulus into electrochemical activity.[1][2][3][4] This form of sensory transduction is responsible for a number of senses and physiological processes in the body, including proprioception, touch,[5] balance, and hearing.[6][7][8] The basic mechanism of mechanotransduction involves converting mechanical signals into electrical or chemical signals.
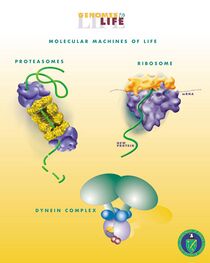
In this process, a mechanically gated ion channel makes it possible for sound, pressure, or movement to cause a change in the excitability of specialized sensory cells and sensory neurons.[9] The stimulation of a mechanoreceptor causes mechanically sensitive ion channels to open and produce a transduction current that changes the membrane potential of the cell.[10] Typically the mechanical stimulus gets filtered in the conveying medium before reaching the site of mechanotransduction.[11] Cellular responses to mechanotransduction are variable and give rise to a variety of changes and sensations. Broader issues involved include molecular biomechanics.
Single-molecule biomechanics studies of proteins and DNA, and mechanochemical coupling in molecular motors have demonstrated the critical importance of molecular mechanics as a new frontier in bioengineering and life sciences. Current findings indicate that the mechanotransduction channel in hair cells complex biological machine. Mechanotransduction also includes the use of chemical energy to do mechanical work.[12]
Cellular mechanotransduction
Cells continuously detect and respond to mechanical cues in their individual environments: substrate stiffness, shear stress, tension, and compression. These forces are converted into biochemical signals through mechanotransduction pathways, allowing cells to regulate their behavior: migration, death, structural changes, gene expression, and cell differentiation.[13]
General cellular mechanotransduction pathway
The following are the typical steps of a mechanotransduction pathway:[13]
- A mechanical force is applied (tension, rigidity, friction, sheer force, etc).
- A force-sensitive protein (often mechanosensitive channels) responds to the mechanical force.
- An electrochemical gradient or change in cell polarity is produced directly or indirectly by the force-sensitive protein.
- This gradient or polarity produces an effect or output that changes cell behavior.
Mechanical sensing structures
Cells use the following structures in specialized ways to detect mechanical forces.
- Ion channels - mechanosensitive channels modulate their activity based on physical pressures.[14]
- Extracellular matrix linked proteins - integrins and focal adhesions can transmit forces from the linked extracellular matrix to the cytoskeleton.[13]
- Cytoskeleton - actin, microtubules, and intermediate filaments act as force-transmitting networks.[13]
- Nucleus - deformations of the nuclear lamina can influence gene expression.[15]
Mechanical forces applied to these structures can activate intracellular signaling pathways, alter cytoskeletal tension, and change gene transcription (see linked sources for specific pathways).
Examples of these mechanical sensing structures leading to mechanotransduced behavior changes are listed below.
| Mechanical Cue | Cellular Sensor | Common Cellular Response(s) |
|---|---|---|
| Substrate stiffness | Integrins, cytoskeleton, nucleus | Differentiation[13], apoptosis[15], migration[13] |
| Sheer stress | Ion channels, glycocalyx | Endothelial alignment[16] |
| Compression | Cytoskeleton, nucleus | Gene regulation[15] |
| Tension | Integrins, cytoskeleton | Stress fiber formation, contractility |
Aberrant cellular mechanotransduction
Unusual or altered mechanotransduction has been correlated with changes in cell behavior. As well, changes to the medium on which cells grow (the extracellular matrix) can often regulate cell activity through to mechanotransduction. Thus, these changes to the extracellular matrix can result in unhealthy cell activity.
Cancer
Cell behavior changes resulting from aberrant mechanotransduction may lead to cancer. Substrate stiffness (more abundant around cancerous tissue) can be transduced into signaling pathways that lead to cell death or migration.[13][15] Apoptosis can be regulated by the stiffness of the extracellular matrix.[15] Rigidity-sensing complexes regulating where cells grow or travel is partially managed by mechanotransduction.[17] Alterations to this rigidity-sensing mechanotransduction can promote cancer: loss in rigidity-sensing complexes can, for example, lead to growth on soft tissue without apoptosis.[18]
Cross-linked extracellular matrix proteins in tumors leads to stiffness that has been shown to favor cancer development.[19] Through mechano-sensitive pathways, this stiffness can lead to metastasis through the stimulation of epithelial-mesenchymal transition (EMT)[20] which is associated with anoikis avoidance - stimulating cell migration.
Fibrosis
Mechanotransduction pathways, such as FAK-ERK, have been shown to be involved in fibrosis.[21]
Ear
Air pressure changes in the ear canal cause the vibrations of the tympanic membrane and middle ear ossicles. At the end of the ossicular chain, movement of the stapes footplate within the oval window of the cochlea generates a pressure field within the cochlear fluids, imparting a pressure differential across the basilar membrane. A sinusoidal pressure wave results in localized vibrations of the organ of Corti: near the base for high frequencies, near the apex for low frequencies.[22] Hair cells in the cochlea are stimulated when the basilar membrane is driven up and down by differences in the fluid pressure between the scala vestibuli and scala tympani. This motion is accompanied by a shearing motion between the tectorial membrane and the reticular lamina of the organ of Corti, causing the hair bundles that link the two to be deflected, initiating mechano-electrical transduction. When the basilar membrane is driven upward, shear between the hair cells and the tectorial membrane deflects hair bundles in the excitatory direction, toward their tall edge. At the midpoint of an oscillation the hair bundles resume their resting position. When the basilar membrane moves downward, the hair bundles are driven in the inhibitory direction.[23]
Skeletal muscle
When a deformation is imposed on a muscle, changes in cellular and molecular conformations link the mechanical forces with biochemical signals, and the close integration of mechanical signals with electrical, metabolic, and hormonal signaling may disguise the aspect of the response that is specific to the mechanical forces.[24]
Cartilage
One of the main mechanical functions of articular cartilage is to act as a low-friction, load-bearing surface. Due to its unique location at joint surfaces, articular cartilage experiences a range of static and dynamic forces that include shear, compression and tension. These mechanical loads are absorbed by the cartilage extracellular matrix, where they are subsequently dissipated and transmitted to chondrocytes (cartilage cells).

Chondrocytes sense and convert the mechanical signals they receive into biochemical signals, which subsequently direct and mediate both anabolic (matrix building) and catabolic (matrix degrading) processes. These processes include the synthesis of matrix proteins (type II collagen and proteoglycans), proteases, protease inhibitors, transcription factors, cytokines and growth factors.[25][26]
The balance that is struck between anabolic and catabolic processes is strongly influenced by the type of loading that cartilage experiences. High strain rates (such as which occurs during impact loading) cause tissue damage, degradation, decreased matrix production and apoptosis.[27][28] Decreased mechanical loading over long periods, such as during extended bed-rest, causes a loss of matrix production.[29] Static loads have been shown to be detrimental to biosynthesis[30] while oscillatory loads at low frequencies (similar that of a normal walking gait) have been shown to be beneficial in maintaining health and increasing matrix synthesis.[31] Due to the complexity of in-vivo loading conditions and the interplay of other mechanical and biochemical factors, the question of what an optimal loading regimen may be or whether one exists remain unanswered.
In order for mechanical signals to be sensed, there need to be mechanoreceptors on the surface of chondrocytes. Candidates for chondrocyte mechanoreceptors include stretch-activated ion channels (SAC),[32] the hyaluronan receptor CD44, annexin V (a collagen type II receptor),[33] and integrin receptors (of which there exist several types on chondrocytes).
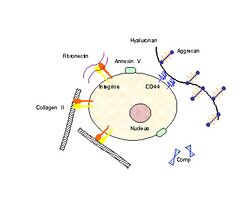
Using the integrin-linked mechanotransduction pathway as an example (being one of the better studied pathways), it has been shown to mediate chondrocyte adhesion to cartilage surfaces,[34] mediate survival signaling[35] and regulate matrix production and degradation.[36]
In addition to binding to extracellular matrix ligands, integrins are also receptive to autocrine and paracrine signals such as growth factors in the TGF-beta family. Chondrocytes have been shown to secrete TGF-b, and upregulate TGF-b receptors in response to mechanical stimulation; this secretion may be a mechanism for autocrine signal amplification within the tissue.[37]
Integrin signaling is just one example of multiple pathways that are activated when cartilage is loaded. Some intracellular processes that have been observed to occur within these pathways include phosphorylation of ERK1/2, p38 MAPK, and SAPK/ERK kinase-1 (SEK-1) of the JNK pathway[38] as well as changes in cAMP levels, actin re-organization and changes in the expression of genes which regulate cartilage extracellular matrix content.[39]
More recent studies have hypothesized that chondrocyte primary cilium act as a mechanoreceptor for the cell, transducing forces from the extracellular matrix into the cell. Each chondrocyte has one cilium and it is hypothesized to transmit mechanical signals by way of bending in response to extracellular matrix loading. Integrins have been identified on the upper shaft of the cilium, acting as anchors to the collagen matrix around it.[40] Recent studies published by Wann et al. in FASEB Journal have demonstrated for the first time that primary cilia are required for chondrocyte mechanotransduction. Chondrocytes derived from IFT88 mutant mice did not express primary cilia and did not show the characteristic mechanosensitive up regulation of proteoglycan synthesis seen in wild type cells[41]
References
- ↑ Biswas, Abhijit; Manivannan, M.; Srinivasan, Mandyam A. (2015). "Vibrotactile Sensitivity Threshold: Nonlinear Stochastic Mechanotransduction Model of the Pacinian Corpuscle". IEEE Transactions on Haptics 8 (1): 102–113. doi:10.1109/TOH.2014.2369422. PMID 25398183. https://zenodo.org/record/894772.
- ↑ Katsumi, A.; Orr, AW; Tzima, E; Schwartz, MA (2003). "Integrins in Mechanotransduction". Journal of Biological Chemistry 279 (13): 12001–4. doi:10.1074/jbc.R300038200. PMID 14960578.
- ↑ Qin, Y.; Qin, Y; Liu, J; Tanswell, AK; Post, M (1996). "Mechanical Strain Induces pp60src Activation and Translocation to Cytoskeleton in Fetal Rat Lung Cells". Journal of Biological Chemistry 271 (12): 7066–71. doi:10.1074/jbc.271.12.7066. PMID 8636139.
- ↑ Bidhendi, Amir J; Altartouri, Bara; Gosselin, Frédérick P.; Geitmann, Anja (2019). "Mechanical stress initiates and sustains the morphogenesis of wavy leaf epidermal cells". Cell Reports 28 (5): 1237–1250. doi:10.1016/j.celrep.2019.07.006. PMID 31365867. https://www.cell.com/action/showPdf?pii=S2211-1247%2819%2930890-3.
- ↑ Biswas, Abhijit; Manivannan, M.; Srinivasan, Mandyam A. (2014). "Nonlinear two stage mechanotransduction model and neural response of Pacinian Corpuscle". USA: IEEE. pp. 1–4. doi:10.1109/BSEC.2014.6867740.
- ↑ Tavernarakis, Nektarios; Driscoll, Monica (1997). "Molecular Modeling of Mechanotransduction in the Nematode Caenorhabditis Elegans". Annual Review of Physiology 59: 659–89. doi:10.1146/annurev.physiol.59.1.659. PMID 9074782.
- ↑ Howard, J; Roberts, W M; Hudspeth, A J (1988). "Mechanoelectrical Transduction by Hair Cells". Annual Review of Biophysics and Biophysical Chemistry 17: 99–124. doi:10.1146/annurev.bb.17.060188.000531. PMID 3293600.
- ↑ Hackney, CM; Furness, DN (1995). "Mechanotransduction in vertebrate hair cells: Structure and function of the stereociliary bundle". The American Journal of Physiology 268 (1 Pt 1): C1–13. doi:10.1152/ajpcell.1995.268.1.C1. PMID 7840137.
- ↑ Gillespie, Peter G.; Walker, Richard G. (2001). "Molecular basis of mechanosensory transduction". Nature 413 (6852): 194–202. doi:10.1038/35093011. PMID 11557988. Bibcode: 2001Natur.413..194G.
- ↑ Grigg, P (1986). "Biophysical studies of mechanoreceptors". Journal of Applied Physiology 60 (4): 1107–15. doi:10.1152/jappl.1986.60.4.1107. PMID 2422151.
- ↑ Biswas, Abhijit; Manivannan, M.; Srinivasan, Mandyam A. (2015). "Multiscale Layered Biomechanical Model of the Pacinian Corpuscle". IEEE Transactions on Haptics 8 (1): 31–42. doi:10.1109/TOH.2014.2369416. PMID 25398182. https://zenodo.org/record/894776.
- ↑ {{cite book|last1=Nakano|first1=Tadashi|last2=Eckford|first2=Andrew W.|last3=Haraguchi|first3=Tokuko|title=Molecular Communication|url=https://books.google.com/books?id=uVhsAAAAQBAJ%7Cdate=12 September 2013|publisher=Cambridge University Press|isbn=978-1-107-02308-6}}
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 Wolfenson, Haguy; Yang, Bo; Sheetz, Michael P. (2019-02-10). "Steps in Mechanotransduction Pathways that Control Cell Morphology". Annual Review of Physiology 81: 585–605. doi:10.1146/annurev-physiol-021317-121245. ISSN 1545-1585. PMID 30403543. PMC 7476682. https://pmc.ncbi.nlm.nih.gov/articles/PMC7476682/.
- ↑ Roeterink, Renate M. A.; Casadevall I Solvas, Xevi; Collins, David J.; Scott, Daniel J. (December 2024). "Force versus Response: Methods for Activating and Characterizing Mechanosensitive Ion Channels and GPCRs". Advanced Healthcare Materials 13 (31). doi:10.1002/adhm.202402167. ISSN 2192-2659. PMID 39402780. PMC 11650423. https://pmc.ncbi.nlm.nih.gov/articles/PMC11650423/.
- ↑ 15.0 15.1 15.2 15.3 15.4 Faure, Laura M.; Venturini, Valeria; Roca-Cusachs, Pere (2025-03-15). "Cell compression - relevance, mechanotransduction mechanisms and tools". Journal of Cell Science 138 (6): jcs263704. doi:10.1242/jcs.263704. ISSN 1477-9137. PMID 40145202.
- ↑ Power, Gavin; Ferreira-Santos, Larissa; Martinez-Lemus, Luis A.; Padilla, Jaume (2024-10-01). "Integrating molecular and cellular components of endothelial shear stress mechanotransduction". American Journal of Physiology. Heart and Circulatory Physiology 327 (4): H989–H1003. doi:10.1152/ajpheart.00431.2024. ISSN 1522-1539. PMID 39178024. PMC 11482243. https://pmc.ncbi.nlm.nih.gov/articles/PMC11482243/.
- ↑ Meacci, Giovanni; Wolfenson, Haguy; Liu, Shuaimin; Stachowiak, Matthew R.; Iskratsch, Thomas; Mathur, Anurag; Ghassemi, Saba; Gauthier, Nils et al. (2016-11-07). "α-Actinin links extracellular matrix rigidity-sensing contractile units with periodic cell-edge retractions". Molecular Biology of the Cell 27 (22): 3471–3479. doi:10.1091/mbc.E16-02-0107. ISSN 1939-4586. PMID 27122603. PMC 5221581. https://pmc.ncbi.nlm.nih.gov/articles/PMC5221581/.
- ↑ Wang, Hong-Bei; Dembo, Micah; Wang, Yu-Li (November 2000). "Substrate flexibility regulates growth and apoptosis of normal but not transformed cells". American Journal of Physiology-Cell Physiology 279 (5): C1345–C1350. doi:10.1152/ajpcell.2000.279.5.C1345. ISSN 0363-6143. https://journals.physiology.org/doi/full/10.1152/ajpcell.2000.279.5.C1345.
- ↑ Paszek, Matthew J.; Zahir, Nastaran; Johnson, Kandice R.; Lakins, Johnathon N.; Rozenberg, Gabriela I.; Gefen, Amit; Reinhart-King, Cynthia A.; Margulies, Susan S. et al. (2005-09-01). "Tensional homeostasis and the malignant phenotype". Cancer Cell 8 (3): 241–254. doi:10.1016/j.ccr.2005.08.010. ISSN 1535-6108. https://www.sciencedirect.com/science/article/pii/S1535610805002680.
- ↑ Leight, Jennifer L.; Wozniak, Michele A.; Chen, Sophia; Lynch, Michelle L.; Chen, Christopher S. (March 2012). "Matrix rigidity regulates a switch between TGF-β1-induced apoptosis and epithelial-mesenchymal transition". Molecular Biology of the Cell 23 (5): 781–791. doi:10.1091/mbc.E11-06-0537. ISSN 1939-4586. PMID 22238361. PMC 3290638. https://pmc.ncbi.nlm.nih.gov/articles/PMC3290638/.
- ↑ Lagares, David; Busnadiego, Oscar; García-Fernández, Rosa Ana; Kapoor, Mohit; Liu, Shangxi; Carter, David E.; Abraham, David; Shi-Wen, Xu et al. (May 2012). "Inhibition of focal adhesion kinase prevents experimental lung fibrosis and myofibroblast formation". Arthritis and Rheumatism 64 (5): 1653–1664. doi:10.1002/art.33482. ISSN 1529-0131. PMID 22492165. PMC 3338902. https://pmc.ncbi.nlm.nih.gov/articles/PMC3338902/.
- ↑ Ehret, Günter (2009-05-08) (in en). Stiffness gradient along the basilar membrane as a basis for spatial frequency analysis within the cochlea. doi:10.18725/OPARU-1218. https://oparu.uni-ulm.de/xmlui/handle/123456789/1245.
- ↑ Fettiplace, Robert (September 12, 2017). "Hair cell transduction, tuning and synaptic transmission in the mammalian cochlea". Comprehensive Physiology 7 (4): 1197–1227. doi:10.1002/cphy.c160049. ISBN 978-0-470-65071-4. PMID 28915323.
- ↑ Burkholder, TJ (2007). "Mechanotransduction in skeletal muscle". Frontiers in Bioscience 12: 174–91. doi:10.2741/2057. PMID 17127292.
- ↑ Fitzgerald, J. B.; Jin, M; Dean, D; Wood, DJ; Zheng, MH; Grodzinsky, AJ (2004). "Mechanical Compression of Cartilage Explants Induces Multiple Time-dependent Gene Expression Patterns and Involves Intracellular Calcium and Cyclic AMP". Journal of Biological Chemistry 279 (19): 19502–11. doi:10.1074/jbc.M400437200. PMID 14960571.
- ↑ Fitzgerald, J. B.; Jin, M; Grodzinsky, AJ (2006). "Shear and Compression Differentially Regulate Clusters of Functionally Related Temporal Transcription Patterns in Cartilage Tissue". Journal of Biological Chemistry 281 (34): 24095–103. doi:10.1074/jbc.M510858200. PMID 16782710.
- ↑ Kurz, Bodo; Jin, Moonsoo; Patwari, Parth; Cheng, Debbie M.; Lark, Michael W.; Grodzinsky, Alan J. (2001). "Biosynthetic response and mechanical properties of articular cartilage after injurious compression". Journal of Orthopaedic Research 19 (6): 1140–6. doi:10.1016/S0736-0266(01)00033-X. PMID 11781016.
- ↑ Loening, A; James, IE; Levenston, ME; Badger, AM; Frank, EH; Kurz, B; Nuttall, ME; Hung, HH et al. (2000). "Injurious Mechanical Compression of Bovine Articular Cartilage Induces Chondrocyte Apoptosis". Archives of Biochemistry and Biophysics 381 (2): 205–12. doi:10.1006/abbi.2000.1988. PMID 11032407.
- ↑ Behrens, Fred; Kraft, Ellen L.; Oegema, Theodore R. (1989). "Biochemical changes in articular cartilage after joint immobilization by casting or external fixation". Journal of Orthopaedic Research 7 (3): 335–43. doi:10.1002/jor.1100070305. PMID 2703926.
- ↑ Torzilli, P. A.; Deng, X-H.; Ramcharan, M. (2006). "Effect of Compressive Strain on Cell Viability in Statically Loaded Articular Cartilage". Biomechanics and Modeling in Mechanobiology 5 (2–3): 123–32. doi:10.1007/s10237-006-0030-5. PMID 16506016.
- ↑ Sah, Robert L.-Y.; Kim, Young-Jo; Doong, Joe-Yuan H.; Grodzinsky, Alan J.; Plass, Anna H. K.; Sandy, John D. (1989). "Biosynthetic response of cartilage explants to dynamic compression". Journal of Orthopaedic Research 7 (5): 619–36. doi:10.1002/jor.1100070502. PMID 2760736.
- ↑ Mouw, J. K.; Imler, S. M.; Levenston, M. E. (2006). "Ion-channel Regulation of Chondrocyte Matrix Synthesis in 3D Culture Under Static and Dynamic Compression". Biomechanics and Modeling in Mechanobiology 6 (1–2): 33–41. doi:10.1007/s10237-006-0034-1. PMID 16767453.
- ↑ Von Der Mark, K.; Mollenhauer, J. (1997). "Annexin V interactions with collagen". Cellular and Molecular Life Sciences 53 (6): 539–45. doi:10.1007/s000180050069. PMID 9230933.
- ↑ Kurtis, Melissa S.; Tu, Buu P.; Gaya, Omar A.; Mollenhauer, Jürgen; Knudson, Warren; Loeser, Richard F.; Knudson, Cheryl B.; Sah, Robert L. (2001). "Mechanisms of chondrocyte adhesion to cartilage: Role of β1-integrins, CD44, and annexin V". Journal of Orthopaedic Research 19 (6): 1122–30. doi:10.1016/S0736-0266(01)00051-1. PMID 11781014.
- ↑ Pulai, Judit I.; Del Carlo, Marcello; Loeser, Richard F. (2002). "The ?5?1 integrin provides matrix survival signals for normal and osteoarthritic human articular chondrocytes in vitro". Arthritis & Rheumatism 46 (6): 1528–35. doi:10.1002/art.10334. PMID 12115183.
- ↑ Millward–Sadler, S. J.; Wright, M. O.; Davies, L. W.; Nuki, G.; Salter, D. M. (2000). "Mechanotransduction via integrins and interleukin–4 results in altered aggrecan and matrix metalloproteinase 3 gene expression in normal, but not osteoarthritic, human articular chondrocytes". Arthritis & Rheumatism 43 (9): 2091–2099. doi:10.1002/1529-0131(200009)43:9<2091::AID-ANR21>3.0.CO;2-C. PMID 11014361.
- ↑ Millward-Sadler, S. J.; Salter, D. M. (2004). "Integrin-Dependent Signal Cascades in Chondrocyte Mechanotransduction". Annals of Biomedical Engineering 32 (3): 435–46. doi:10.1023/B:ABME.0000017538.72511.48. PMID 15095818.
- ↑ Fanning, P. J.; Emkey, G; Smith, RJ; Grodzinsky, AJ; Szasz, N; Trippel, SB (2003). "Mechanical Regulation of Mitogen-activated Protein Kinase Signaling in Articular Cartilage". Journal of Biological Chemistry 278 (51): 50940–8. doi:10.1074/jbc.M305107200. PMID 12952976.
- ↑ Urban, J. P. G. (1994). "The Chondrocyte: A Cell Under Pressure". Rheumatology 33 (10): 901–908. doi:10.1093/rheumatology/33.10.901. PMID 7921748.
- ↑ McGlashan, S. R.; Jensen, CG; Poole, CA (2006). "Localization of Extracellular Matrix Receptors on the Chondrocyte Primary Cilium". Journal of Histochemistry and Cytochemistry 54 (9): 1005–14. doi:10.1369/jhc.5A6866.2006. PMID 16651393.
- ↑ Wann, AKExpression error: Unrecognized word "etal". (April 2012). "Primary cilia mediate mechanotransduction through control of ATP-induced Ca2+ signaling in compressed chondrocytes". FASEB J. 26 (4): 1663–71. doi:10.1096/fj.11-193649. PMID 22223751.
Further reading
- Khan, K M; Scott, A (2009). "Mechanotherapy: How physical therapists' prescription of exercise promotes tissue repair". British Journal of Sports Medicine 43 (4): 247–52. doi:10.1136/bjsm.2008.054239. PMID 19244270.
- Mammano, F.; Nobili, R (1993). "Biophysics of the cochlea: Linear approximation". The Journal of the Acoustical Society of America 93 (6): 3320–32. doi:10.1121/1.405716. PMID 8326060. Bibcode: 1993ASAJ...93.3320M.
- v. Békésy, Georg (1952). "DC Resting Potentials Inside the Cochlear Partition". The Journal of the Acoustical Society of America 24 (1): 72–76. doi:10.1121/1.1906851. Bibcode: 1952ASAJ...24...72V.
- 1. Kandel, E.R., Schwartz, J.H., Jessell, T.M., Principles of Neural Science. New York: McGraw-Hill ed, ed. 4th. 2000.
- Hudspeth, A. J.; Choe, Y.; Mehta, A. D.; Martin, P. (2000). "Putting ion channels to work: Mechanoelectrical transduction, adaptation, and amplification by hair cells". Proceedings of the National Academy of Sciences 97 (22): 11765–72. doi:10.1073/pnas.97.22.11765. PMID 11050207. Bibcode: 2000PNAS...9711765H.
- Hudspeth, A. J. (1989). "How the ear's works work". Nature 341 (6241): 397–404. doi:10.1038/341397a0. PMID 2677742. Bibcode: 1989Natur.341..397H.
External links
- www.du.edu/~kinnamon/3640/hearing/hearing.html
- Cellular+Mechanotransduction at the US National Library of Medicine Medical Subject Headings (MeSH)
 |
