Medicine:Pain management
| Occupation | |
|---|---|
| Names | Physician |
Occupation type | Specialty |
Activity sectors | Medicine |
| Description | |
Education required |
|
Fields of employment | Hospitals, clinics |
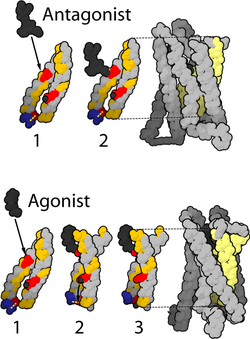
Pain management is an aspect of medicine and health care involving relief of pain (pain relief, analgesia, pain control) in various dimensions, from acute and simple to chronic and challenging. Most physicians and other health professionals provide some pain control in the normal course of their practice, and for the more complex instances of pain, they also call on additional help from a specific medical specialty devoted to pain, which is called pain medicine.
Pain management often uses a multidisciplinary approach for easing the suffering and improving the quality of life of anyone experiencing pain,[2] whether acute pain or chronic pain. Relieving pain (analgesia) is typically an acute process, while managing chronic pain involves additional complexities and ideally a multidisciplinary approach.
A typical multidisciplinary pain management team may include: medical practitioners, pharmacists, clinical psychologists, physiotherapists, occupational therapists, recreational therapists, physician assistants, nurses, and dentists.[3] The team may also include other mental health specialists and massage therapists. Pain sometimes resolves quickly once the underlying trauma or pathology has healed, and is treated by one practitioner, with drugs such as pain relievers (analgesics) and occasionally also anxiolytics.
Effective management of chronic (long-term) pain, however, frequently requires the coordinated efforts of the pain management team.[4] Effective pain management does not always mean total eradication of all pain. Rather, it often means achieving adequate quality of life in the presence of pain, through any combination of lessening the pain and/or better understanding it and being able to live happily despite it. Medicine treats injuries and diseases to support and speed healing. It treats distressing symptoms such as pain and discomfort to reduce any suffering during treatment, healing, and dying.
Defining pain
In the nursing profession, one common definition of pain is any problem that is "whatever the experiencing person says it is, existing whenever the experiencing person says it does".[5]
Pain management includes patient and communication about the pain problem.[6] To define the pain problem, a health care provider will likely ask questions such as:[6]
- How intense is the pain?
- How does the pain feel?
- Where is the pain?
- What, if anything, makes the pain lessen?
- What, if anything, makes the pain increase?
- When did the pain start?
After asking such questions, the health care provider will have a description of the pain.[6] Pain is often rated on a scale from 1 to 10, known as the Numeric Rating Scale (NRS);[7]
Rating Pain Level
- 0 No Pain
- 1 – 3 Mild Pain (nagging, annoying, interfering little with ADLs)
- 4 – 6 Moderate Pain (interferes significantly with ADLs)
- 7 – 10 Severe Pain (disabling; unable to perform ADLs)
This pain scale is based on a person reporting their pain intensity, with 0 representing no pain experienced and 10 indicating the worst possible pain.[8] The NRS is a common tool used by clinicians and in research to understand personal pain levels and monitor changes over time.[8] In the clinical context, pain management will then be used to address that pain.[6]
Adverse effects
There are many types of pain management. Each have their own benefits, drawbacks, and limits.[6]
A common challenge in pain management is communication between the health care provider and the person experiencing pain.[6] People experiencing pain may have difficulty recognizing or describing what they feel and how intense it is.[6] Health care providers and patients may have difficulty communicating with each other about how pain responds to treatments.[6] There is a risk in many types of pain management for the patient to take treatment that is less effective than needed or which causes other difficulties and side effects.[6] Some treatments for pain can be harmful if overused.[6] A goal of pain management for the patient and their health care provider is to identify the amount of treatment needed to address the pain without going beyond that limit.[6]
Another problem with pain management is that pain is the body's natural way of communicating a problem.[6] Pain is supposed to resolve as the body heals itself with time and pain management.[6] Sometimes pain management covers a problem, and the patient might be less aware that they need treatment for a deeper problem.[6]
Physical approaches
Physical medicine and rehabilitation
Physical medicine and rehabilitation (PM&R), a medical specialty, uses a range of physical techniques, such as heat and electrotherapy, as well as therapeutic exercises and behavioral therapy in the management of pain. PM&R techniques are usually part of an interdisciplinary or multidisciplinary program that might also include pharmaceuticals.[9] Spa therapy has shown positive effects in reducing pain among patients with chronic low back pain, but its evidence base is limited.[10] Studies have shown that kinesiotape can be used to reduce chronic low back pain.[11] The US Centers for Disease Control recommended that physical therapy and exercise be prescribed as first-line treatments (rather than opioids) for multiple causes of chronic pain in 2016 guidelines.[12] Applicable disorders include chronic low back pain, osteoarthritis of the hip and knee, and fibromyalgia.[12] Exercise alone or with other rehabilitation disciplines (including psychotherapeutic approaches) can have a positive effects on pain.[12] Besides improving the experience of pain itself, exercise can also improve individuals' well-being and general health.[12]
Manipulative and mobilization therapies are considered safe interventions for low back pain, with manipulation potentially offering a larger therapeutic effect.[13]
Specifically in chronic low back pain, education about the way the brain processes pain in conjunction with routine physiotherapy interventions may provide short-term relief of disability and pain.[14]
Exercise interventions

Physical activity interventions, such as tai chi, yoga, and Pilates, promote harmony of the mind and body through total body awareness. These practices incorporate breathing techniques, meditation, and a wide variety of movements while training the body to perform functionally by increasing strength, flexibility, and range of motion.[15] Physical activity can also benefit chronic sufferers by reducing inflammation and sensitivity and boosting overall energy.[16] Physical activity and exercise may improve chronic pain (pain lasting more than 12 weeks),[17] and overall quality of life, while minimizing the need for pain medications.[15] More specifically, walking has been effective in improving pain management in chronic low back pain.[18]
TENS
Transcutaneous electrical nerve stimulation (TENS) is a self-operated portable device intended to help regulate and control chronic pain via electrical impulses.[19] Limited research has explored the effectiveness of TENS in relation to pain management of multiple sclerosis (MS). MS is a chronic autoimmune neurological disorder, which consists of the demyelination of the nerve axons and the disruption of nerve conduction velocity and efficiency.[19] In one study, electrodes were placed over the lumbar spine, and participants received treatment twice a day and at any time when they experienced a painful episode.[19] This study found that TENS would benefit MS patients with localized or limited symptoms in one limb.[19] The research is mixed with whether or not TENS helps manage pain in MS patients.[citation needed]
Transcutaneous electrical nerve stimulation is ineffective for lower back pain. However, it might help with diabetic neuropathy[20] as well as other illnesses.
tDCS
Transcranial direct current stimulation (tDCS) is a non-invasive technique of brain stimulation that can modulate activity in specific brain cortex regions, and it involves the application of low-intensity (up to 2 mA) constant direct current to the scalp through electrodes in order to modulate the excitability of large cortical areas.[21] tDCS may have a role in pain assessment by contributing to efforts in distinguishing between somatic and affective aspects of pain experience.[21] Zaghi and colleagues (2011) found that the motor cortex, when stimulated with tDCS, increases the threshold for both the perception of non-painful and painful stimuli.[21] Although there is a greater need for research examining the mechanism of electrical stimulation in pain treatment, one theory suggests that the changes in thalamic activity may be due to the influence of motor cortex stimulation on the decrease in pain sensations.[21]
Concerning MS, a study found that daily tDCS sessions resulted in an individual's subjective report of pain decreased when compared to a sham condition.[19] In addition, the study found a similar improvement at 1 to 3 days before and after each tDCS session.[19]
Fibromyalgia is a disorder in which an individual experiences dysfunctional brain activity, musculoskeletal pain, fatigue, and tenderness in localized areas.[22] Research examining tDCS for pain treatment in fibromyalgia has found initial evidence for pain decreases.[22] Specifically, the stimulation of the primary motor cortex resulted in significantly greater pain improvement in comparison to the control group (e.g., sham stimulation, stimulation of the DLPFC).[22] However, this effect decreased after treatment ended, but remained significant for three weeks following the extinction of treatment.[22]
Acupuncture

Acupuncture involves the insertion and manipulation of needles into specific points on the body to relieve pain or for therapeutic purposes. An analysis of the 13 highest quality studies of pain treatment with acupuncture, published in January 2009 in the British Medical Journal, was unable to quantify the difference in the effect on pain of real, sham and no acupuncture.[23] A systematic review in 2019 reported that acupuncture injection therapy was an effective treatment for patients with nonspecific chronic low back pain, and is widely used in Southeast Asian countries.[24]
Light therapy
Research has found evidence that light therapy such as low level laser therapy is an effective therapy for relieving low back pain.[25][26] Instead of thermal therapy, where reactant energy is originated through heat, Low-Level Light Therapy (LLLT) utilizes photochemical reactions requiring light to function. Photochemical reactions need light in order to function. Photons, the energy created from light, from these photochemical reactions provide the reactants with energy to embed in muscles, thus managing pain.[27] One study conducted by Stausholm et al. showed that at certain wavelengths, LLLT reduced pain in participants with knee osteoarthritis.[28] LLLT stimulates a variety of cell types, which in turn can help treat tendonitis, arthritis, and pain relating to muscles.[citation needed]
Sound therapy
Audioanalgesia and music therapy are both examples of using auditory stimuli to manage pain or other distress. They are generally viewed as insufficient when used alone but also as helpful adjuncts to other forms of therapy.[citation needed]
Interventional procedures
Interventional radiology procedures for pain control, typically used for chronic back pain, include epidural steroid injections, facet joint injections, neurolytic blocks, spinal cord stimulators and intrathecal drug delivery system implants.
Pulsed radiofrequency, neuromodulation, direct introduction of medication and nerve ablation may be used to target either the tissue structures and organ/systems responsible for persistent nociception or the nociceptors from the structures implicated as the source of chronic pain.[29][30][31][32][33] Radiofrequency treatment has been seen to improve pain in patients with facet joint low back pain. However, continuous radiofrequency is more effective in managing pain than pulsed radiofrequency.[34]
An intrathecal pump is sometimes used to deliver very small quantities of medications directly to the spinal fluid. This is similar to epidural infusions used in labour and postoperatively. The major differences are that it is much more common for the drug to be delivered into the spinal fluid (intrathecal) rather than epidurally, and the pump can be fully implanted under the skin.
A spinal cord stimulator is an implantable medical device that creates electric impulses and applies them near the dorsal surface of the spinal cord, providing a paresthesia ("tingling") sensation that alters the perception of pain by the patient.
Intra-articular ozone therapy
Intra-articular ozone therapy has been seen to alleviate chronic pain in patients with knee osteoarthritis efficiently.[35]
Psychological approaches
Acceptance and commitment therapy
Acceptance and commitment therapy (ACT) is a type of cognitive behavioral therapy that emphasizes behavior modification over symptom reduction, focusing on changing the context of psychological experiences and employing experiential behavior change methods.[36] The central process in ACT revolves around psychological flexibility, which in turn includes processes of acceptance; awareness; present-oriented mindfulness in interacting with experiences; an ability to persist or change behavior; and an ability to be guided by one's values.[36] ACT has robust evidence in the scientific literature for a range of health and behavior problems, including chronic pain.[36] ACT facilitates the dual processes of acceptance and behavioral change, enabling patients to cultivate psychological flexibility. This approach allows for a more dynamic and adaptable focus in therapeutic interventions, enhancing overall treatment effectiveness.[36]
Recent research has applied ACT successfully to chronic pain in older adults due in part to its direction from individual values and being highly customizable to any stage of life.[36] In line with the therapeutic model of ACT, significant increases in process variables, pain acceptance, and mindfulness were also observed in a study applying ACT to chronic pain in older adults.[36] In addition, these primary results suggested that an ACT-based treatment may significantly improve levels of physical disability, psychosocial disability, and depression post-treatment and at a three-month follow-up for older adults with chronic pain.[36]
Cognitive behavioral therapy
Cognitive behavioral therapy (CBT) in the setting of pain management aims to aid individuals in understanding the relationship between their pain, thoughts, emotions, and behaviors. A main goal in treatment is cognitive—thinking, reasoning, and remembering—restructuring to encourage helpful thought patterns.[37] This will target healthy activities such as regular exercise and pacing. Lifestyle changes are also trained to improve sleep patterns and to develop better coping skills for pain and other stressors using various techniques (e.g., relaxation, diaphragmatic breathing, and even biofeedback).[citation needed]
Studies have demonstrated the usefulness of cognitive behavioral therapy in the management of chronic low back pain, producing significant decreases in physical and psychosocial disability.[38] CBT is significantly more effective than standard care in treatment of people with body-wide pain, like fibromyalgia. Evidence for the usefulness of CBT in the management of adult chronic pain is generally poorly understood, due partly to the proliferation of techniques of doubtful quality, and the poor quality of reporting in clinical trials. The crucial content of individual interventions has not been isolated, and the important contextual elements, such as therapist training and development of treatment manuals, have not been determined. The widely varying nature of the resulting data makes useful systematic review and meta-analysis within the field very difficult.[39]
In 2020, a systematic review of randomized controlled trials (RCTs) evaluated the clinical effectiveness of psychological therapies for the management of adult chronic pain (excluding headaches). There is no evidence that behaviour therapy (BT) is effective for reducing this type of pain; however, BT may be useful for improving a person's mood immediately after treatment. This improvement appears to be small and is short-term in duration.[40] CBT may have a small positive short-term effect on pain immediately following treatment. CBT may also have a small effect on reducing disability and potential catastrophizing that may be associated with adult chronic pain. These benefits do not appear to last very long following the therapy.[40] CBT may contribute towards improving the mood of an adult who experiences chronic pain, which could possibility be maintained for more extended periods of time.[40]
For children and adolescents, a review of RCTs evaluating the effectiveness of psychological therapy for the management of chronic and recurrent pain found that psychological treatments are effective in reducing pain when people under 18 years old have headaches.[41] This beneficial effect may be maintained for at least three months following the therapy.[42] Psychological treatments may also improve pain control for children or adolescents who experience pain unrelated to headaches. It is not known if psychological therapy improves a child's or an adolescent's mood and the potential for disability related to their chronic pain.[42]
Hypnosis
A 2007 review of 13 studies found evidence for the efficacy of hypnosis in reducing pain in some conditions. However, the studies had limitations like small study sizes, raising issues of power to detect group differences, and lacking credible controls for placebo or expectation. The authors concluded that "although the findings provide support for the general applicability of hypnosis in the treatment of chronic pain, considerably more research will be needed to fully determine the effects of hypnosis for different chronic-pain conditions."[43]: 283
Hypnosis has reduced the pain of some harmful medical procedures in children and adolescents.[44] In clinical trials addressing other patient groups, it has significantly reduced pain compared to no treatment or some other non-hypnotic interventions.[45] The effects of self-hypnosis on chronic pain are roughly comparable to those of progressive muscle relaxation.[46]
A 2019 systematic review of 85 studies showed it to be significantly effective at reducing pain for people with high and medium suggestibility, but minimal effectiveness for people with low suggestibility. However, high-quality clinical data is needed to generalize to the whole chronic pain population.[47]
Mindfulness meditation
A 2013 meta-analysis of studies that used techniques centered around the concept of mindfulness concluded, "that MBIs [mindfulness-based interventions] decrease the intensity of pain for chronic pain patients."[48] A 2019 review of studies of brief mindfulness-based interventions (BMBI) concluded that BMBI are not recommended as a first-line treatment and could not confirm their efficacy in managing chronic or acute pain.[49]
Mindfulness-based pain management
Mindfulness-based pain management (MBPM) is a mindfulness-based intervention (MBI) providing specific applications for people living with chronic pain and illness.[50][51] Adapting the core concepts and practices of mindfulness-based stress reduction (MBSR) and mindfulness-based cognitive therapy (MBCT), MBPM includes a distinctive emphasis on the practice of 'loving-kindness', and has been seen as sensitive to concerns about removing mindfulness teaching from its original ethical framework within Buddhism.[50][52] It was developed by Vidyamala Burch and is delivered through the programs of Breathworks.[50][51]
Medications
The World Health Organization (WHO) recommends a pain ladder for managing pain relief with pharmaceutical medicine. It was first described for use in cancer pain. However it can be used by medical professionals as a general principle when managing any type of pain.[53][54] In the treatment of chronic pain, the three-step WHO Analgesic Ladder provides guidelines for selecting the appropriate medicine. The exact medications recommended will vary by country and the individual treatment center, but the following gives an example of the WHO approach to treating chronic pain with medications. If, at any point, treatment fails to provide adequate pain relief, then the doctor and patient move onto the next step.[citation needed]
| Common types of pain and typical drug management | |||
|---|---|---|---|
| Pain type | typical initial drug treatment | comments | |
| headache | doctor consultation is appropriate if headaches are severe, persistent, accompanied by fever, vomiting, or speech or balance problems;[55] self-medication should be limited to two weeks[55] | ||
| migraine | paracetamol, NSAIDs[55] | triptans are used when the others do not work, or when migraines are frequent or severe[55] | |
| menstrual cramps | NSAIDs[55] | some NSAIDs are marketed for cramps, but any NSAID would work[55] | |
| minor trauma, such as a bruise, abrasions, sprain | paracetamol, NSAIDs[55] | opioids not recommended[55] | |
| severe trauma, such as a wound, burn, bone fracture, or severe sprain | opioids[55] | more than two weeks of pain requiring opioid treatment is unusual[55] | |
| strain or pulled muscle | NSAIDs, muscle relaxants[55] | if inflammation is involved, NSAIDs may work better; short-term use only[55] | |
| minor pain after surgery | paracetamol, NSAIDs[55] | opioids rarely needed[55] | |
| severe pain after surgery | opioids[55] | combinations of opioids may be prescribed if pain is severe[55] | |
| muscle ache | paracetamol, NSAIDs[55] | if inflammation involved, NSAIDs may work better.[55] | |
| toothache or pain from dental procedures | paracetamol, NSAIDs[55] | this should be short term use; opioids may be necessary for severe pain[55] | |
| kidney stone pain | paracetamol, NSAIDs, opioids[55] | opioids usually needed if pain is severe.[55] | |
| pain due to heartburn or gastroesophageal reflux disease | antacid, H2 antagonist, proton-pump inhibitor[55] | heartburn lasting more than a week requires medical attention; aspirin and NSAIDs should be avoided[55] | |
| chronic back pain | paracetamol, NSAIDs[55] | opioids may be necessary if other drugs do not control pain and pain is persistent[55] | |
| osteoarthritis pain | paracetamol, NSAIDs[55] | medical attention is recommended if pain persists.[55] | |
| fibromyalgia | antidepressant, anticonvulsant[55] | evidence suggests that opioids are not effective in treating fibromyalgia[55] | |
Mild pain
Paracetamol (acetaminophen), or a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen will relieve mild pain.[56]
Mild to moderate pain
Moderate to severe pain
When treating moderate to severe pain, the type of the pain, acute or chronic, needs to be considered. The type of pain can result in different medications being prescribed. Certain medications may work better for acute pain, others for chronic pain, and some may work equally well on both. Acute pain medication is for rapid onset of pain such as from an inflicted trauma or to treat post-operative pain. Chronic pain medication is for alleviating long-lasting, ongoing pain.[citation needed]
Morphine is the gold standard to which all narcotics are compared. Semi-synthetic derivatives of morphine such as hydromorphone (Dilaudid), oxymorphone (Numorphan, Opana), nicomorphine (Vilan), hydromorphinol and others vary in such ways as duration of action, side effect profile and milligramme potency. Fentanyl has the benefit of less histamine release and thus fewer side effects. It can also be administered via transdermal patch which is convenient for chronic pain management. In addition to the transdermal patch and injectable fentanyl formulations, the FDA (Food and Drug Administration) has approved various immediate release fentanyl products for breakthrough cancer pain (Actiq/OTFC/Fentora/Onsolis/Subsys/Lazanda/Abstral). Oxycodone is used across the Americas and Europe for relief of serious chronic pain. Its main slow-release formula is known as OxyContin. Short-acting tablets, capsules, syrups and ampules which contain oxycodone are available making it suitable for acute intractable pain or breakthrough pain. Diamorphine, and methadone are used less frequently. Clinical studies have shown that transdermal buprenorphine is effective at reducing chronic pain.[57] Pethidine, known in North America as meperidine, is not recommended [by whom?] for pain management due to its low potency, short duration of action, and toxicity associated with repeated use.[citation needed] [ and dipipanone are also not recommended in new patients except for acute pain where other analgesics are not tolerated or are inappropriate, for pharmacological and misuse-related reasons. In some countries potent synthetics such as piritramide and ketobemidone are used for severe pain. Tapentadol is a newer agent introduced in the last decade.[citation needed]
For moderate pain, tramadol, codeine, dihydrocodeine, and hydrocodone are used, with nicocodeine, ethylmorphine and propoxyphene or dextropropoxyphene (less commonly).
Drugs of other types can be used to help opioids combat certain types of pain. Amitriptyline is prescribed for chronic muscular pain in the arms, legs, neck and lower back with an opiate, or sometimes without it or with an NSAID.
While opiates are often used in the management of chronic pain, high doses are associated with an increased risk of opioid overdose.[58]
In the U.S., the illegal use of opioids has led to an increasingly high threshold of prescribing analgesics to patients, and as a result minor pain killers were prescribed. Some medical analysts have criticized that development as it might cause premature deaths among cancer patients.[59]
Opioids
In 2009, the Food and Drug Administration stated: "According to the National Institutes of Health, studies have shown that properly managed medical use of opioid analgesic compounds (taken exactly as prescribed) is safe, can manage pain effectively, and rarely causes addiction."[60] In 2013, the FDA stated that "abuse and misuse of these products have created a serious and growing public health problem".[61]
Opioid medications can provide short, intermediate or long acting analgesia depending upon the specific properties of the medication and whether it is formulated as an extended release drug. Opioid medications may be administered orally, by injection, via nasal mucosa or oral mucosa, rectally, transdermally, intravenously, epidurally and intrathecally. In chronic pain conditions that are opioid responsive, a combination of a long-acting (OxyContin, MS Contin, Opana ER, Exalgo and Methadone) or extended release medication is often prescribed along with a shorter-acting medication (oxycodone, morphine or hydromorphone) for breakthrough pain, or exacerbations.
Most opioid treatment used by patients outside of healthcare settings is oral (tablet, capsule or liquid), but suppositories and skin patches can be prescribed. An opioid injection is rarely needed for patients with chronic pain.
Although opioids are strong analgesics, they do not provide complete analgesia regardless of whether the pain is acute or chronic in origin. Opioids are effective analgesics in chronic malignant pain and modestly effective in nonmalignant pain management.[62] However, there are associated adverse effects, especially during the commencement or change in dose. When opioids are used for prolonged periods drug tolerance will occur. Other risks can include chemical dependency, diversion and addiction.[63][64]
Clinical guidelines for prescribing opioids for chronic pain have been issued by the American Pain Society and the American Academy of Pain Medicine. Included in these guidelines is the importance of assessing the patient for the risk of substance abuse, misuse, or addiction. Factors correlated with an elevated risk of opioid misuse include a history of substance use disorder, younger age, major depression, and the use of psychotropic medications.[65] Physicians who prescribe opioids should integrate this treatment with any psychotherapeutic intervention the patient may be receiving. The guidelines also recommend monitoring not only the pain but also the level of functioning and the achievement of therapeutic goals. The prescribing physician should be suspicious of abuse when a patient reports a reduction in pain but has no accompanying improvement in function or progress in achieving identified goals.[66]
The list below consists of commonly used opioid analgesics which have long-acting formulations. Common brand names for the extended release formulation are in parentheses.
- Oxycodone (OxyContin)
- Hydromorphone (Exalgo, Hydromorph Contin)
- Morphine (M-Eslon, MS Contin)
- Oxymorphone (Opana ER)
- Fentanyl, transdermal (Duragesic)
- Buprenorphine*, transdermal (Butrans)
- Tramadol (Ultram ER)
- Tapentadol (Nucynta ER)
- Methadone* (Metadol, Methadose)
- Hydrocodone bitartrate (Hysingla ER) and bicarbonate (Zohydro ER)
*Methadone and buprenorphine are each used both for the treatment of opioid addiction and as analgesics
Nonsteroidal anti-inflammatory drugs
The other major group of analgesics are nonsteroidal anti-inflammatory drugs (NSAID). They work by inhibiting the release of prostaglandins, which cause inflammatory pain. Acetaminophen/paracetamol is not always included in this class of medications. However, acetaminophen may be administered as a single medication or in combination with other analgesics (both NSAIDs and opioids). The alternatively prescribed NSAIDs such as ketoprofen and piroxicam have limited benefit in chronic pain disorders and with long-term use are associated with significant adverse effects. The use of selective NSAIDs designated as selective COX-2 inhibitors have significant cardiovascular and cerebrovascular risks which have limited their utilization.[67][68] Common NSAIDs include aspirin, ibuprofen, and naproxen. There are many NSAIDs such as parecoxib (selective COX-2 inhibitor) with proven effectiveness after different surgical procedures. Wide use of non-opioid analgesics can reduce opioid-induced side-effects.[69]
Antidepressants and antiepileptic drugs
Some antidepressant and antiepileptic drugs are used in chronic pain management and act primarily within the pain pathways of the central nervous system, though peripheral mechanisms have been attributed as well. They are generally used to treat nerve brain that results from injury to the nervous system. Neuropathy can be due to chronic high blood sugar levels (diabetic neuropathy). These drugs also reduce pain from viruses such as shingles, phantom limb pain and post-stroke pain.[citation needed] These mechanisms vary and in general are more effective in neuropathic pain disorders as well as complex regional pain syndrome.[70] A common anti-epileptic drug is gabapentin, and an example of an antidepressant would be amitriptyline.[citation needed]
Cannabinoids
The evidence for using cannabis for pain control varies in quality, but overall there is no good evidence cannabis is effective for any type of pain management, or that it is viable as a means of reducing opioid use.[71]
Ketamine
Low-dose ketamine is sometimes used as an alternative to opioids for the treatment of acute pain in hospital emergency departments.[72][73] Ketamine probably? reduces pain more than opioids and with less nausea and vomiting.[74]
Other analgesics
Other drugs which can potentiate conventional analgesics or have analgesic properties in certain circumstances are called analgesic adjuvant medications.[75] Gabapentin, an anticonvulsant, can reduce neuropathic pain itself and can also potentiate opiates.[76] Drugs with anticholinergic activity, such as orphenadrine and cyclobenzaprine, are given in conjunction with opioids for neuropathic pain. Orphenadrine and cyclobenzaprine are also muscle relaxants, and are useful in painful musculoskeletal conditions. Clonidine, an alpha-2 receptor agonist, is another drug that has found use as an analgesic adjuvant.[75] In 2021, researchers described a novel type of pain therapy — a CRISPR-dCas9 epigenome editing method for repressing Nav1.7 gene expression which showed therapeutic potential in three mouse models of chronic pain.[77][78]
Nefopam may be used when common alternatives are contraindicated or ineffective, or as an add-on therapy. However it is associated with adverse drug reactions and is toxic in overdose.[79]
Self-management
As of 2024, the patient is encouraged to play a major role in the management of their pain.[80]
Self-management of chronic pain has been described as the individual's ability to manage various aspects of their chronic pain.[81] Self-management can include building self-efficacy, monitoring one's own symptoms, goal setting and action planning. It also includes patient-physician shared decision-making, among others.[81] The benefits of self-management vary depending on self-management techniques used. They only have marginal benefits in management of chronic musculoskeletal pain.[82] Some research has shown that self-management of pain can use different approaches. Those approaches can range from different therapies such as yoga, acupuncture, exercise and other relaxation techniques. Patients could also take a more natural approach by taking different minerals, vitamins or herbs. However, research has shown there is a difference between rural patients and non-rural patients having more access to different self-management approaches. Physicians in these areas may be readily prescribing more pain medication in these rural cities due to being less experienced with pain management. Simply put, it is sometimes easier for rural patients to get a prescription that insurance pays for instead of natural approaches that cost more money than they can afford to spend on their pain management. Self-management may be a more expensive alternative.[83]
Future directions
A 2023 review said that future chronic pain diagnosis and treatment would be more personalized and precision based.[84]
Society and culture
The medical treatment of pain as practiced in Greece and Turkey is called algology (from the Greek άλγος, algos, "pain"). The Hellenic Society of Algology and the Turkish Algology-Pain Society are the relevant local bodies affiliated to the International Association for the Study of Pain (IASP).[85]
Undertreatment
Undertreatment of pain is the absence of pain management therapy for a person in pain when treatment is indicated.
Consensus in evidence-based medicine and the recommendations of medical specialty organizations establish guidelines to determine the treatment for pain which health care providers ought to offer.[86] For various social reasons, persons in pain may not seek or may not be able to access treatment for their pain.[86] Health care providers may not provide the treatment which authorities recommend.[86] Some studies about gender biases have concluded that female pain recipients are often overlooked when it comes to the perception of their pain. Whether they appeared to be in high levels of pain didn't make a difference for their observers. The women participants in the studies were still perceived to be in less pain than they actually were. Men participants on the other hand were offered pain relief while their self reporting indicated that their pain levels didn't necessarily warrant treatment. Biases exist when it comes to gender. Prescribers have been seen over and under prescribing treatment to individuals based on them being male or female [87].There are other prevalent reasons that undertreatment of pain occurs. Gender is a factor as well as race. When it comes to prescribers treating patients racial disparities has become a real factor. Research has shown that non-white individuals pain perception has affected their pain treatment. The African-American community has been shown to suffer significantly when it comes to trusting the medical community to treat them. Oftentimes medication although available to be prescribed is dispensed in less quantities due to their pain being perceived on a smaller scale. The black community could be undermined by physicians thinking they are not in as much pain as they are reporting. Another occurrence may be physicians simply making the choice not to treat the patient accordingly in spite of the self-reported pain level. Racial disparity is definitely a real issue in the world of pain management.[88]
In children
Acute pain is common in children and adolescents as a result of injury, illness, or necessary medical procedures.[89] Chronic pain is present in approximately 15–25% of children and adolescents. It may be caused by an underlying disease, such as sickle cell anemia, cystic fibrosis, rheumatoid arthritis. Cancer or functional disorders such as migraines, fibromyalgia, and complex regional pain could also cause chronic pain in children.[90]
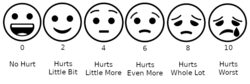
Pain assessment in children is often challenging due to limitations in developmental level, cognitive ability, or their previous pain experiences. Clinicians must observe physiological and behavioral cues exhibited by the child to make an assessment. Self-report, if possible, is the most accurate measure of pain. Self-report pain scales involve younger kids matching their pain intensity to photographs of other children's faces, such as the Oucher Scale, pointing to schematics of faces showing different pain levels, or pointing out the location of pain on a body outline.[91] Questionnaires for older children and adolescents include the Varni-Thompson Pediatric Pain Questionnaire (PPQ) and the Children's Comprehensive Pain Questionnaire. They are often utilized for individuals with chronic or persistent pain.[91]
Acetaminophen, nonsteroidal anti-inflammatory agents, and opioid analgesics are commonly used to treat acute or chronic pain symptoms in children and adolescents. However a pediatrician should be consulted before administering any medication.[91]
Caregivers may provide nonpharmacological treatment for children and adolescents because it carries minimal risk and is cost effective compared to pharmacological treatment. Nonpharmacologic interventions vary by age and developmental factors. Physical interventions to ease pain in infants include swaddling, rocking, or sucrose via a pacifier. For children and adolescents physical interventions include hot or cold application, massage, or acupuncture.[92] Cognitive behavioral therapy (CBT) aims to reduce the emotional distress and improve the daily functioning of school-aged children and adolescents with pain by changing the relationship between their thoughts and emotions. In addition this therapy teaches them adaptive coping strategies. Integrated interventions in CBT include relaxation technique, mindfulness, biofeedback, and acceptance (in the case of chronic pain).[93] Many therapists will hold sessions for caregivers to provide them with effective management strategies.[90]
In red-haired individuals
In recent studies, it has been noted that people who have red-hair through the MC1R receptor gene may react to opioids and perceive pain differently than the rest of the population.[94] The studies on this developing topic have only become notable in the past few years with researchers looking into how red-haired individuals may experience a different threshold in pain and react to pain management differently than others. Most studies find that redheads with this gene have a higher pain tolerance and can also react more sensitively to opiates but require more anesthesia.[95]
Professional certification
Pain management practitioners come from all fields of medicine. In addition to medical practitioners, a pain management team may often benefit from the input of pharmacists, physiotherapists, clinical psychologists and occupational therapists, among others. Together the multidisciplinary team can help create a package of care suitable to the patient.
Pain medicine in the United States
Pain physicians are often fellowship-trained board-certified anesthesiologists, neurologists, physiatrists, emergency physicians, or psychiatrists. Palliative care doctors are also specialists in pain management. The American Society of Interventional Pain Physicians, the American Board of Anesthesiology, the American Osteopathic Board of Anesthesiology (recognized by the AOABOS), the American Board of Physical Medicine and Rehabilitation, the American Board of Emergency Medicine and the American Board of Psychiatry and Neurology[96] each provide certification for a subspecialty in pain management following fellowship training. The fellowship training is recognized by the American Board of Medical Specialties (ABMS) or the American Osteopathic Association Bureau of Osteopathic Specialists (AOABOS). As the field of pain medicine has grown rapidly, many practitioners have entered the field, some non-ACGME board-certified.[97]
See also
- Equianalgesic
- List of investigational analgesics
- Opioid comparison, an example of an equianalgesic chart
- Pain Catastrophizing Scale
- Pain ladder
- Pain management during childbirth
- Pain psychology
References
- ↑ "Homology models of mu-opioid receptor with organic and inorganic cations at conserved aspartates in the second and third transmembrane domains". Archives of Biochemistry and Biophysics 375 (1): 31–49. March 2000. doi:10.1006/abbi.1999.1529. PMID 10683246.
- ↑ Chronic pain management: the essentials. U.K.: Greenwich Medical Media. 1997. p. 10. ISBN 978-1-900151-85-6. https://archive.org/details/chronicpainmanag0000hard.
- ↑ Pain management: an interdisciplinary approach. Churchill Livingstone. 2000. ISBN 978-0-443-05683-3. https://archive.org/details/painmanagementin0000main. "Pain management: an interdisciplinary approach."
- ↑ "The classification of pain". Pain management: A practical guide for clinicians. CRC Press. 2002. p. 29. ISBN 978-0-8493-0926-7. https://books.google.com/books?id=L2CSdeiMZi4C&q=%22the+classification+of+pain%22+thienhaus&pg=PA27.
- ↑ Pain: clinical manual. St. Louis: Mosby. 1999. ISBN 0-8151-5609-X.[page needed]
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 6.11 6.12 6.13 Consumer Reports (April 28, 2016). "Pain Relief: What You Need to Know". http://www.consumerreports.org/pain-relief/pain-relief-what-you-need-know/.
- ↑ "Numeric Rating Scale (NRS-11)". https://physiotherapy.ca/divisions/pain-science/numeric-rating-scale-nrs-11/.
- ↑ 8.0 8.1 Society, Canadian Paediatric. "Best practices in pain assessment and management for children | Canadian Paediatric Society" (in en). https://cps.ca/documents/position/pain-assessment-and-management.
- ↑ "Chronic pain in rehabilitation medicine". Disability and Rehabilitation 28 (6): 363–367. March 2006. doi:10.1080/09638280500287437. PMID 16492632.
- ↑ "Effectiveness of spa therapy for patients with chronic low back pain: An updated systematic review and meta-analysis". Medicine 98 (37). September 2019. doi:10.1097/MD.0000000000017092. PMID 31517832.
- ↑ "Effects of kinesiotape on pain and disability in individuals with chronic low back pain: a systematic review and meta-analysis of randomized controlled trials". Clinical Rehabilitation 33 (4): 596–606. April 2019. doi:10.1177/0269215518817804. PMID 30526011.
- ↑ 12.0 12.1 12.2 12.3 "CDC Guideline for Prescribing Opioids for Chronic Pain - United States, 2016" (in en-us). MMWR. Recommendations and Reports 65 (1): 1–49. March 2016. doi:10.15585/mmwr.rr6501e1. PMID 26987082.
- ↑ "Manipulation and mobilization for treating chronic low back pain: a systematic review and meta-analysis". The Spine Journal 18 (5): 866–879. May 2018. doi:10.1016/j.spinee.2018.01.013. PMID 29371112.
- ↑ Wood, Lianne; Hendrick, Paul A. (February 2019). "A systematic review and meta-analysis of pain neuroscience education for chronic low back pain: Short-and long-term outcomes of pain and disability". European Journal of Pain 23 (2): 234–249. doi:10.1002/ejp.1314. PMID 30178503. https://nottingham-repository.worktribe.com/output/1574403.
- ↑ 15.0 15.1 "Physical activity and exercise for chronic pain in adults: an overview of Cochrane Reviews". The Cochrane Database of Systematic Reviews 4 (2). April 2017. doi:10.1002/14651858.CD011279.pub3. PMID 28436583.
- ↑ University, Utah State. "Exercise and Chronic Pain" (in en). https://extension.usu.edu/heart/research/exercise-and-chronic-pain.
- ↑ "Chronic Pain: Symptoms, Diagnosis, & Treatment". https://medlineplus.gov/magazine/issues/spring11/articles/spring11pg5-6.html.
- ↑ "The effectiveness of walking versus exercise on pain and function in chronic low back pain: a systematic review and meta-analysis of randomized trials". Disability and Rehabilitation 41 (6): 622–632. March 2019. doi:10.1080/09638288.2017.1410730. PMID 29207885.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 "Pain Management in Multiple Sclerosis: a Review of Available Treatment Options". Current Treatment Options in Neurology 21 (12). November 2019. doi:10.1007/s11940-019-0601-2. PMID 31773455.
- ↑ "Assessment: efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology 74 (2): 173–176. January 2010. doi:10.1212/WNL.0b013e3181c918fc. PMID 20042705.
- ↑ 21.0 21.1 21.2 21.3 "Assessment and treatment of pain with non-invasive cortical stimulation". Restorative Neurology and Neuroscience 29 (6): 439–451. 2011. doi:10.3233/RNN-2011-0615. PMID 22124038.
- ↑ 22.0 22.1 22.2 22.3 "A randomized, sham-controlled, proof of principle study of transcranial direct current stimulation for the treatment of pain in fibromyalgia". Arthritis and Rheumatism 54 (12): 3988–3998. December 2006. doi:10.1002/art.22195. PMID 17133529.
- ↑ "Acupuncture treatment for pain: systematic review of randomised clinical trials with acupuncture, placebo acupuncture, and no acupuncture groups". BMJ 338 (jan27 2). January 2009. doi:10.1136/bmj.a3115. PMID 19174438.
- ↑ "Acupoint injection for nonspecific chronic low back pain: A protocol of systematic review". Medicine 98 (29). July 2019. doi:10.1097/MD.0000000000016478. PMID 31335709.
- ↑ "Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline". Annals of Internal Medicine 147 (7): 492–504. October 2007. doi:10.7326/0003-4819-147-7-200710020-00007. PMID 17909210.
- ↑ "Low level laser therapy for nonspecific low-back pain". The Cochrane Database of Systematic Reviews 2011 (2). April 2008. doi:10.1002/14651858.CD005107.pub4. PMID 18425909.
- ↑ "Photochemical Reaction: Definition, Types, Equation, Mechanisms" (in en). https://testbook.com/chemistry/photochemical-reaction.
- ↑ Stausholm, Martin Bjørn; Naterstad, Ingvill Fjell; Joensen, Jon; Lopes-Martins, Rodrigo Álvaro Brandão; Sæbø, Humaira; Lund, Hans; Fersum, Kjartan Vibe; Bjordal, Jan Magnus (October 2019). "Efficacy of low-level laser therapy on pain and disability in knee osteoarthritis: systematic review and meta-analysis of randomised placebo-controlled trials". BMJ Open 9 (10). doi:10.1136/bmjopen-2019-031142. PMID 31662383.
- ↑ "Neural modulation by blocks and infusions". Pain Practice 6 (1): 34–38. March 2006. doi:10.1111/j.1533-2500.2006.00056.x. PMID 17309707.
- ↑ "Spinal cord stimulation in chronic pain management". Neurosurgery Clinics of North America 15 (3): 297–306. July 2004. doi:10.1016/j.nec.2004.02.012. PMID 15246338.
- ↑ "Motor cortex stimulation for long-term relief of chronic neuropathic pain: a 10 year experience". Pain 121 (1–2): 43–52. March 2006. doi:10.1016/j.pain.2005.12.006. PMID 16480828.
- ↑ Boswell, Mark V.; Trescot, Andrea M.; Datta, Sukdeb; Schultz, David M.; Hansen, Hans C.; Abdi, Salahadin; Sehgal, Nalini; Shah, Rinoo V. et al. (January 2007). "Interventional techniques: evidence-based practice guidelines in the management of chronic spinal pain". Pain Physician 10 (1): 7–111. PMID 17256025. http://www.painphysicianjournal.com/linkout?issn=1533-3159&vol=10&page=7.
- ↑ "Ablative procedures for chronic pain". Neurosurgery Clinics of North America 15 (3): 335–342. July 2004. doi:10.1016/j.nec.2004.02.009. PMID 15246341.
- ↑ "Pulsed Radiofrequency Versus Continuous Radiofrequency for Facet Joint Low Back Pain: A Systematic Review". World Neurosurgery 122: 390–396. February 2019. doi:10.1016/j.wneu.2018.10.191. PMID 30404055.
- ↑ "Intra-articular ozone therapy efficiently attenuates pain in knee osteoarthritic subjects: A systematic review and meta-analysis". Complementary Therapies in Medicine 42: 240–247. February 2019. doi:10.1016/j.ctim.2018.11.023. PMID 30670248.
- ↑ 36.0 36.1 36.2 36.3 36.4 36.5 36.6 "Treatment for chronic pain for adults in the seventh and eighth decades of life: a preliminary study of Acceptance and Commitment Therapy (ACT)". Pain Medicine 13 (7): 860–867. July 2012. doi:10.1111/j.1526-4637.2012.01407.x. PMID 22680627.
- ↑ "What Is Cognitive Behavioral Therapy?" (in en). American Psychological Association (APA). https://www.apa.org/ptsd-guideline/patients-and-families/cognitive-behavioral.
- ↑ "Comparison of operant behavioral and cognitive-behavioral group treatment for chronic low back pain". Journal of Consulting and Clinical Psychology 56 (2): 261–266. April 1988. doi:10.1037/0022-006x.56.2.261. PMID 2967314.
- ↑ "Can 'ehealth' technology deliver on its promise of pain management for all?". Pain 152 (8): 1701–1702. August 2011. doi:10.1016/j.pain.2011.05.004. PMID 21612868.
- ↑ 40.0 40.1 40.2 "Psychological therapies for the management of chronic pain (excluding headache) in adults". The Cochrane Database of Systematic Reviews 8 (5). August 2020. doi:10.1002/14651858.CD007407.pub4. PMID 32794606.
- ↑ "Psychological therapies (remotely delivered) for the management of chronic and recurrent pain in children and adolescents". The Cochrane Database of Systematic Reviews 4 (4). April 2019. doi:10.1002/14651858.cd011118.pub3. PMID 30939227.
- ↑ 42.0 42.1 "Psychological therapies for the management of chronic and recurrent pain in children and adolescents". The Cochrane Database of Systematic Reviews 9 (10). September 2018. doi:10.1002/14651858.CD003968.pub5. PMID 30270423.
- ↑ "Hypnotherapy for the management of chronic pain". The International Journal of Clinical and Experimental Hypnosis 55 (3): 275–287. July 2007. doi:10.1080/00207140701338621. PMID 17558718.
- ↑ "The effectiveness of hypnosis for reducing procedure-related pain in children and adolescents: a comprehensive methodological review". Journal of Behavioral Medicine 32 (4): 328–339. August 2009. doi:10.1007/s10865-009-9207-6. PMID 19255840.
- ↑ American Psychological Association (2 July 2004). "Hypnosis for the relief and control of pain". American Psychological Association. http://www.apa.org/research/action/hypnosis.aspx.
- ↑ "Hypnotic treatment of chronic pain". Journal of Behavioral Medicine 29 (1): 95–124. February 2006. doi:10.1007/s10865-005-9031-6. PMID 16404678.
- ↑ Thompson, Trevor; Terhune, Devin B.; Oram, Charlotte; Sharangparni, Joseph; Rouf, Rommana; Solmi, Marco; Veronese, Nicola; Stubbs, Brendon (April 2019). "The effectiveness of hypnosis for pain relief: A systematic review and meta-analysis of 85 controlled experimental trials". Neuroscience & Biobehavioral Reviews 99: 298–310. doi:10.1016/j.neubiorev.2019.02.013. PMID 30790634. http://gala.gre.ac.uk/id/eprint/23018/7/23108%20THOMPSON_The_Effectiveness_of_Hypnosis_for_Pain_Relief_2019.pdf.
- ↑ "Do mindfulness-based interventions reduce pain intensity? A critical review of the literature". Pain Medicine 14 (2): 230–242. February 2013. doi:10.1111/pme.12006. PMID 23240921.
- ↑ "Brief Mindfulness-Based Interventions for Acute and Chronic Pain: A Systematic Review". Journal of Alternative and Complementary Medicine 25 (3): 265–278. March 2019. doi:10.1089/acm.2018.0351. PMID 30523705.
- ↑ 50.0 50.1 50.2 "Evaluation of the breathworks mindfulness-based pain management programme: effects on well-being and multiple measures of mindfulness". Clinical Psychology & Psychotherapy 17 (1): 63–78. 2010. doi:10.1002/cpp.653. PMID 19911432.
- ↑ 51.0 51.1 "What is Mindfulness based Pain Management (MBPM)?" (in en). 22 January 2019. https://www.breathworks-mindfulness.org.uk/mbpm.
- ↑ "Evaluation of Breathworks' Mindfulness for Stress 8-week course: Effects on depressive symptoms, psychiatric symptoms, affects, self-compassion, and mindfulness facets in Brazilian health professionals". Journal of Clinical Psychology 75 (6): 970–984. June 2019. doi:10.1002/jclp.22749. PMID 30689206.
- ↑ "WHO - WHO's cancer pain ladder for adults". https://www.who.int/cancer/palliative/painladder/en/.
- ↑ Innovation in pain management: the transcript of a Witness seminar held by the Wellcome Trust Centre for the History of Medicine at UCL, London, on 12 december 2002. London: Wellcome Trust Centre for the History of Medicine at University College London. 2004. ISBN 978-0-85484-097-7. https://archive.org/details/innovationinpain00reyn.
- ↑ 55.00 55.01 55.02 55.03 55.04 55.05 55.06 55.07 55.08 55.09 55.10 55.11 55.12 55.13 55.14 55.15 55.16 55.17 55.18 55.19 55.20 55.21 55.22 55.23 55.24 55.25 55.26 55.27 55.28 55.29 Cite error: Invalid
<ref>tag; no text was provided for refs namedBBDchronicpain - ↑ MedlinePlus Encyclopedia Over-the-counter pain relievers
- ↑ "Treatment of Chronic Pain With Various Buprenorphine Formulations: A Systematic Review of Clinical Studies". Anesthesia and Analgesia 127 (2): 529–538. August 2018. doi:10.1213/ANE.0000000000002718. PMID 29239947.
- ↑ "Opioid prescriptions for chronic pain and overdose: a cohort study". Annals of Internal Medicine 152 (2): 85–92. January 2010. doi:10.7326/0003-4819-152-2-201001190-00006. PMID 20083827.
- ↑ "Opioid Abuse in Chronic Pain — Misconceptions and Mitigation Strategies≥" ma-assn.org. Retrieved May 10 2025.
- ↑ FDA.gov "A Guide to Safe Use of Pain Medicine" February 23, 2009
- ↑ "Abuse-deterrent opioids: evaluation and laveling guidance for industry". https://www.fda.gov/media/84819/download.
- ↑ "Ambulatory diagnosis and treatment of nonmalignant pain in the United States, 2000-2010". Medical Care 51 (10): 870–878. October 2013. doi:10.1097/MLR.0b013e3182a95d86. PMID 24025657.
- ↑ "Pain and opioid addiction: what is the connection?". Current Pain and Headache Reports 14 (1): 17–21. February 2010. doi:10.1007/s11916-009-0086-x. PMID 20425210.
- ↑ "Systematic review: treatment agreements and urine drug testing to reduce opioid misuse in patients with chronic pain". Annals of Internal Medicine 152 (11): 712–720. June 2010. doi:10.7326/0003-4819-152-11-201006010-00004. PMID 20513829.
- ↑ Thomas R. Frieden, Harold W. Jaffe, Joanne Cono, et al. CDC Guideline for Prescribing Opioids for Chronic Pain — United States, 2016. MMWR Recomm Rep 2016;65 Pg. 9-10
- ↑ "Guidelines for prescribing opioids for chronic pain". Psychiatr Times 27 (5): 20. 2010. https://www.psychiatrictimes.com/view/guidelines-prescribing-opioids-chronic-pain.
- ↑ "Nonopioid analgesics". The Medical Clinics of North America 91 (1): 97–111. January 2007. doi:10.1016/j.mcna.2006.10.011. PMID 17164106.
- ↑ "Opioids for chronic nonterminal pain". Southern Medical Journal 99 (11): 1245–1255. November 2006. doi:10.1097/01.smj.0000223946.19256.17. PMID 17195420.
- ↑ "Comparison of analgesic efficacy of acetaminophen monotherapy versus acetaminophen combinations with either pethidine or parecoxib in patients undergoing laparoscopic cholecystectomy: a randomized prospective study". Medicinski Glasnik 18 (1): 27–32. February 2021. doi:10.17392/1245-21. PMID 33155461.
- ↑ "Pharmacotherapy for neuropathic pain". Pain Practice 6 (1): 27–33. March 2006. doi:10.1111/j.1533-2500.2006.00055.x. PMID 17309706.
- ↑ "Cannabis and pain: a scoping review". Braz J Anesthesiol 72 (1): 142–151. 2022. doi:10.1016/j.bjane.2021.06.018. PMID 34280454.
- ↑ American College of Emergency Physicians (2017). "Optimizing the Treatment of Acute Pain in the Emergency Department". Annals of Emergency Medicine (Elsevier BV) 70 (3): 446–448. doi:10.1016/j.annemergmed.2017.06.043. PMID 28844277. "Subdissociative-dose ketamine (SDK) may be used either alone or as part of a multimodal approach to pain relief for traumatic and nontraumatic pain.".
- ↑ "Low-dose Ketamine For Acute Pain Control in the Emergency Department: A Systematic Review and Meta-analysis". Academic Emergency Medicine 28 (4): 444–454. April 2021. doi:10.1111/acem.14159. PMID 33098707.
- ↑ Sandberg, Mårten; Hyldmo, Per Kristian; Kongstad, Poul; Dahl Friesgaard, Kristian; Raatiniemi, Lasse; Larsen, Robert; Magnusson, Vidar; Rognås, Leif et al. (November 2020). "Ketamine for the treatment of prehospital acute pain: a systematic review of benefit and harm". BMJ Open 10 (11). doi:10.1136/bmjopen-2020-038134. PMID 33234621.
- ↑ 75.0 75.1 "Current pharmacotherapy of chronic pain". Journal of Pain and Symptom Management 19 (1 Suppl): S16–S20. January 2000. doi:10.1016/s0885-3924(99)00124-4. PMID 10687334.
- ↑ "Gabapentin as an adjuvant to opioid analgesia for neuropathic cancer pain". Journal of Pain and Symptom Management 17 (6): 441–445. June 1999. doi:10.1016/S0885-3924(99)00033-0. PMID 10388250.
- ↑ "Unique CRISPR gene therapy offers opioid-free chronic pain treatment". New Atlas. 11 March 2021. https://newatlas.com/science/crispr-gene-therapy-opioid-free-chronic-pain-relief/.
- ↑ "Long-lasting analgesia via targeted in situ repression of NaV1.7 in mice". Science Translational Medicine 13 (584). March 2021. doi:10.1126/scitranslmed.aay9056. PMID 33692134.
- ↑ "Use of nefopam for chronic pain". January 5, 2024. https://www.sps.nhs.uk/articles/use-of-nefopam-for-chronic-pain/.
- ↑ Kang, Youngjoo; Trewern, Louise; Jackman, John; Soni), Anushka Irani (nee; McCartney, David (January 2, 2024). "Chronic pain: supported self-management". BMJ 384. doi:10.1136/bmj-2022-072362. PMID 38167273. https://www.bmj.com/content/384/bmj-2022-072362.
- ↑ 81.0 81.1 "What Works and Does Not Work in a Self-Management Intervention for People With Chronic Pain? Qualitative Systematic Review and Meta-Synthesis". Physical Therapy 98 (5): 381–397. May 2018. doi:10.1093/ptj/pzy029. PMID 29669089.
- ↑ "The effectiveness of generic self-management interventions for patients with chronic musculoskeletal pain on physical function, self-efficacy, pain intensity and physical activity: A systematic review and meta-analysis". European Journal of Pain 22 (9): 1577–1596. October 2018. doi:10.1002/ejp.1253. PMID 29845678.
- ↑ Eaton, Linda H.; Langford, Dale J.; Meins, Alexa R.; Rue, Tessa; Tauben, David J.; Doorenbos, Ardith Z. (February 2018). "Use of Self-management Interventions for Chronic Pain Management: A Comparison between Rural and Nonrural Residents" (in en). Pain Management Nursing 19 (1): 8–13. doi:10.1016/j.pmn.2017.09.004. PMID 29153296.
- ↑ Rahman, Sadiq; Kidwai, Ali; Rakhamimova, Emiliya; Elias, Murad; Caldwell, William; Bergese, Sergio D. (December 18, 2023). "Clinical Diagnosis and Treatment of Chronic Pain". Diagnostics (Basel, Switzerland) 13 (24): 3689. doi:10.3390/diagnostics13243689. PMID 38132273.
- ↑ "The history of algology, algotherapy, and the role of inhibition". History and Philosophy of the Life Sciences 12 (1): 27–49. 1990. PMID 2243924.
- ↑ 86.0 86.1 86.2 Human Rights Watch (2 June 2011), Global State of Pain Treatment: Access to Medicines and Palliative Care, Human Rights Watch, https://www.hrw.org/report/2011/06/02/global-state-pain-treatment/access-medicines-and-palliative-care, retrieved 28 July 2016
- ↑ ""Brave Men" and "Emotional Women": A Theory-Guided Literature Review on Gender Bias in Health Care and Gendered Norms towards Patients with Chronic Pain". Pain Research & Management 2018. 2018. doi:10.1155/2018/6358624. PMID 29682130.
- ↑ Hoffman, Kelly M.; Trawalter, Sophie; Axt, Jordan R.; Oliver, M. Norman (19 April 2016). "Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites". Proceedings of the National Academy of Sciences 113 (16): 4296–4301. doi:10.1073/pnas.1516047113. PMID 27044069. Bibcode: 2016PNAS..113.4296H.
- ↑ American Academy of Pediatrics (September 2001). "The assessment and management of acute pain in infants, children, and adolescents". Pediatrics 108 (3): 793–797. doi:10.1542/peds.108.3.793. PMID 11533354.
- ↑ 90.0 90.1 "The interdisciplinary management of pediatric pain: Time for more integration". Techniques in Regional Anesthesia and Pain Management 17 (2013): 188–94. 2013. doi:10.1053/j.trap.2014.07.006.
- ↑ 91.0 91.1 91.2 "Pediatric Pain Management". American Medical Association. http://www.ama-cmeonline.com/pain_mgmt/printversion/ama_painmgmt_m6.pdf.
- ↑ "Nonpharmacologic pediatric pain management in emergency departments: a systematic review of the literature". Journal of Emergency Nursing 39 (2): 140–150. March 2013. doi:10.1016/j.jen.2012.09.011. PMID 23199786.
- ↑ "The role of cognitive behavioral therapy for chronic pain in adolescents". PM & R 5 (8): 697–704. August 2013. doi:10.1016/j.pmrj.2013.05.009. PMID 23953015.
- ↑ "Study finds link between red hair and pain threshold" (in EN). 2021-04-19. https://www.nih.gov/news-events/nih-research-matters/study-finds-link-between-red-hair-pain-threshold.
- ↑ Cepeda, M. Soledad; Carr, Daniel B. (November 2003). "Women Experience More Pain and Require More Morphine Than Men to Achieve a Similar Degree of Analgesia". Anesthesia & Analgesia 97 (5): 1464–1468. doi:10.1213/01.ane.0000080153.36643.83. PMID 14570666.
- ↑ "Taking a Subspecialty Exam - American Board of Psychiatry and Neurology". http://www.abpn.com/become-certified/taking-a-subspecialty-exam/.
- ↑ "ACGME sports, ACGME pain, or non-ACGME sports and spine: which is the ideal fellowship training for PM&R physicians interested in musculoskeletal medicine?". PM & R 5 (8): 718–23; discussion 723–5. August 2013. doi:10.1016/j.pmrj.2013.07.004. PMID 23953018.
Further reading
- Staats, Peter; Diwan, Sudhir (2014). Atlas of Pain Medicine Procedures. McGraw-Hill Education. ISBN 978-0-07-173876-7.
- Staats, Peter; Wallace, Mark S. (2015). Pain Medicine and Management: Just the Facts. McGraw-Hill Education. ISBN 978-0-07-181745-5.
- Manual of pain management. Hagerstwon, MD: Lippincott Williams & Wilkins. 2002. ISBN 978-0-7817-2313-8.
- Principles and practice of pain medicine. New York: McGraw-Hill, Medical Publishing Division. 2004. ISBN 978-0-07-144349-4.
- Pain Management. Philadelphia: Saunders. 2006. ISBN 978-0-7216-0334-6.
- "Ambulatory diagnosis and treatment of nonmalignant pain in the United States, 2000-2010". Medical Care 51 (10): 870–878. October 2013. doi:10.1097/MLR.0b013e3182a95d86. PMID 24025657.
- Graham, S. Scott (2015). The Politics of Pain Medicine: A Rhetorical-Ontological Inquiry. University of Chicago Press. ISBN 978-0-226-26405-9.
- Innovation in pain management: the transcript of a witness seminar held by the Wellcome Trust Centre for the History of Medicine at UCL, London, on 12 December 2002. Wellcome Trust Centre for the History of Medicine at UCL. 2004. ISBN 978-0-85484-097-7.
- Wailoo, Keith (2014). Pain: A Political History. JHU Press. Project MUSE book 30085. ISBN 978-1-4214-1365-5.
External links
 |
