Medicine:Maggot therapy
| Maggot therapy | |
|---|---|
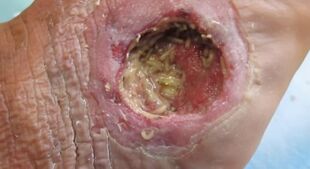 Maggot debridement therapy on a wound from a diabetic foot | |
| Other names | maggot debridement therapy (MDT), larval therapy, larva therapy, larvae therapy, biodebridement, biosurgery |
Maggot debridement therapy (also known as MDT, larval therapy, or simply maggot therapy) is a type of biotherapy involving the introduction of live, disinfected maggots (fly larvae) into non-healing skin and soft-tissue wounds of a human or other animal for the purpose of cleaning out the necrotic (dead) tissue within a wound (debridement), and disinfection. There is evidence that maggot therapy may help with wound healing.[1][2]
Medical uses

Maggot therapy improves healing in chronic ulcers.[1] In diabetic foot ulcers there is tentative evidence of benefit.[3] A Cochrane review of methods for the debridement of venous leg ulcers found maggot therapy to be broadly as effective as most other methods, but the study also noted that the quality of data was poor.[4]
In 2003, the United States Food and Drug Administration (FDA) cleared maggots from common green bottle fly for use as a "medical device" in the US for the purpose of treatment of:[5]
- Non-healing necrotic skin and soft tissue wounds
- Pressure ulcers
- Venous stasis ulcers
- Neuropathic foot ulcers
- Non-healing traumatic or post-surgical wounds
Limitations
The wound must be of a type that can benefit from the application of maggot therapy. A moist, exudating wound with sufficient oxygen supply is a prerequisite. Not all wound-types are suitable: wounds which are dry, or open wounds of body cavities do not provide a good environment for maggots to feed. In some cases it may be possible to make a dry wound suitable for larval therapy by moistening it with saline soaks.[6]
Patients and doctors may find maggots distasteful, although studies have shown that this does not cause patients to refuse the offer of maggot therapy.[7] Maggots can be enclosed in opaque polymer bags to hide them from sight. Dressings must be designed to prevent any maggots from escaping, while allowing air to get to the maggots.[8] Dressings are also designed to minimize the uncomfortable tickling sensation that the maggots often cause.[9]
Mechanisms of action
The maggots have four principal actions:
- Debridement[10]
- Disinfection of the wound[11]
- Stimulation of healing[11]
- Biofilm inhibition and eradication[12]
Debridement
In maggot therapy, large numbers of small maggots consume necrotic tissue far more precisely than is possible in a normal surgical operation, and can debride a wound in a day or two. The area of a wound's surface is typically increased with the use of maggots due to the undebrided surface not revealing the actual underlying size of the wound. They derive nutrients through a process known as "extracorporeal digestion" by secreting a broad spectrum of proteolytic enzymes[13] that liquefy necrotic tissue, and absorb the semi-liquid result within a few days. In an optimum wound environment maggots molt twice, increasing in length from about 2 mm to about 10 mm, and in girth, within a period of 48–72 hours by ingesting necrotic tissue, leaving a clean wound free of necrotic tissue when they are removed.[14]
Disinfection
Secretions from maggots believed to have broad-spectrum antimicrobial activity include allantoin, urea, phenylacetic acid, phenylacetaldehyde, calcium carbonate, proteolytic enzymes, and many others.[15] In vitro studies have shown that maggots inhibit and destroy a wide range of pathogenic bacteria including methicillin-resistant Staphylococcus aureus (MRSA), group A and B streptococci, and Gram-positive aerobic and anaerobic strains.[16] Other bacteria like Pseudomonas aeruginosa, E. coli or Proteus spp. are not attacked by maggots, and in case of Pseudomonas even the maggots are in danger.[17]
Biology of maggots


Those flies whose larvae feed on dead animals will sometimes lay their eggs on the dead parts (necrotic or gangrenous tissue) of living animals. The infestation by maggots of live animals is called myiasis. Some maggots will feed only on dead tissue, some only on live tissue, and some on live or dead tissue. The flies used most often for the purpose of maggot therapy are blow flies of the family Calliphoridae: the blow fly species used most commonly is Lucilia sericata, the common green bottle fly. Another important species, Protophormia terraenovae, is also notable for its feeding secretions, which combat infection by Streptococcus pyogenes and S. pneumoniae.[18]
History
Written records have documented that maggots have been used since antiquity as a wound treatment.[19] There are reports of the use of maggots for wound healing by Maya, Native Americans, and Aboriginals in Australia. Maggot treatment was reported in Renaissance times. Military physicians observed that soldiers whose wounds had become colonized with maggots experienced significantly less morbidity and mortality than soldiers whose wounds had not become colonized. These physicians included Napoleon's surgeon-general, Baron Dominique Larrey. Larrey reported during the French campaign in Egypt and Syria (1798–1801) that certain species of fly consumed only dead tissue and helped wounds to heal.[18]
Joseph Jones, a ranking Confederate medical officer during the American Civil War, stated:
I have frequently seen neglected wounds ... filled with maggots ... as far as my experience extends, these worms eat only dead tissues, and do not injure specifically the well parts.
The first documented therapeutic use of maggots in the United States is credited to a second Confederate medical officer Dr. J.F. Zacharias, who reported during the American Civil War that:
Maggots in a single day would clean a wound much better than any agents we had at our command ... I am sure I saved many lives by their use.
He recorded a high survival rate in patients he treated with maggots.[20]
During World War I, orthopedic surgeon William S. Baer recorded the case of a soldier left for several days on the battlefield who had sustained compound fractures of the femur and large flesh wounds. The soldier arrived at the hospital with maggots infesting his wounds but had no fever or other signs of infection and survived his injuries, which would normally have been fatal. After the war, Baer began using maggot therapy at Boston Children's Hospital in Massachusetts.[21][22]: 169–71
There were reports that American prisoners of war of the Japanese in World War II resorted to maggot therapy to treat severe wounds.[23][24]
A survey of US Army doctors published in 2013 found that 10% of them had used maggot therapy.[25]
Regulation
In the USA: in January 2004, the FDA granted permission to produce and market maggots for use in humans or animals as a prescription-only medical device for the following indications: "For debriding non-healing necrotic skin and soft tissue wounds, including pressure ulcers, venous stasis ulcers, neuropathic foot ulcers, and non-healing traumatic or post-surgical wounds."[26][27]
Veterinary use
The use of maggots to clean dead tissue from animal wounds is part of folk medicine in many parts of the world.[28] It is particularly helpful with chronic osteomyelitis, chronic ulcers, and other pus-producing infections that are frequently caused by chafing due to work equipment. Maggot therapy for horses in the United States was re-introduced after a study published in 2003 by veterinarian Dr. Scott Morrison. This therapy is used in horses for conditions such as osteomyelitis secondary to laminitis, sub-solar abscesses leading to osteomyelitis, post-surgical treatment of street-nail procedure for puncture wounds infecting the navicular bursa, canker, non-healing ulcers on the frog, and post-surgical site cleaning for keratoma removal.[29]
However, there have not been many case studies done with maggot debridement therapy on animals, and as such it can be difficult to accurately assess how successful it is.[30]
References
- ↑ 1.0 1.1 Sun, Xinjuan; Jiang, Kechun; Chen, Jingan et al. (2014). "A systematic review of maggot debridement therapy for chronically infected wounds and ulcers". International Journal of Infectious Diseases 25: 32–7. doi:10.1016/j.ijid.2014.03.1397. PMID 24841930.
- ↑ Nasoori, A.; Hoomand, R. (December 2017). "Maggot debridement therapy for an electrical burn injury with instructions for the use of Lucilia sericata larvae". Journal of Wound Care 26 (12): 734–41. doi:10.12968/jowc.2017.26.12.734. PMID 29244970. https://www.researchgate.net/publication/321856095.
- ↑ Tian, X; Liang, XM; Song, GM et al. (September 2013). "Maggot debridement therapy for the treatment of diabetic foot ulcers: a meta-analysis". Journal of Wound Care 22 (9): 462–9. doi:10.12968/jowc.2013.22.9.462. PMID 24005780.
- ↑ Gethin, Georgina; Cowman, Seamus; Kolbach, Dinanda N. (14 September 2015). "Debridement for venous leg ulcers". Cochrane Database of Systematic Reviews 2015 (9). doi:10.1002/14651858.CD008599.pub2. PMID 26368002.
- ↑ "Product Classification: Maggots, Medical". Food and Drug Administration. https://www.fda.gov/media/74541/download.
- ↑ Gottrup, Finn; Jørgensen, Bo (2011). "Maggot Debridement: An Alternative Method for Debridement". ePlasty (Copenhagen) 11 (33): 290–302. PMID 21776326.
- ↑ Parnés, A.; Lagan, K. M. (2007). "Larval therapy in wound management: A review". International Journal of Clinical Practice 61 (3): 488–93. doi:10.1111/j.1742-1241.2006.01238.x. PMID 17313618. https://pure.ulster.ac.uk/ws/files/11471026/Parnes_Lagan_2007_LTreview.pdf.
- ↑ Scavée, V; Polis, X; Schoevaerdts, J. C. (2003). "Maggot therapy: Many hands make light work". Acta Chirurgica Belgica 103 (4): 405–7. doi:10.1080/00015458.2003.11679453. PMID 14524161. http://www.belsurg.org/uploaded_pdfs/103/103_405_407.pdf. Retrieved 2015-03-04.
- ↑ Morgan, Rosemary (2002). "Larval therapy". Student BMJ 10: 259–302. doi:10.1136/sbmj.0208271. http://student.bmj.com/student/view-article.html?id=sbmj0208271.
- ↑ Chan, Dominic CW; Fong, Daniel HF; Leung, June YY; Patil, NG; Leung, Gilberto KK (October 2007). "Maggot debridement therapy in chronic wound care". Hong Kong Medical Journal 13 (5): 382–6. PMID 17914145. http://www.hkmj.org/abstracts/v13n5/382.htm.
- ↑ 11.0 11.1 Sherman, R. A. (2014). "Mechanisms of Maggot-Induced Wound Healing: What Do We Know, and Where Do We Go from Here?". Evidence-Based Complementary and Alternative Medicine 2014: 1–13. doi:10.1155/2014/592419. PMID 24744812.
- ↑ Sherman, R. A. (2009). "Maggot Therapy Takes Us Back to the Future of Wound Care: New and Improved Maggot Therapy for the 21st Century". Journal of Diabetes Science and Technology 3 (2): 336–44. doi:10.1177/193229680900300215. PMID 20144365.
- ↑ Reames, Mark K.; Christensen, Chris; Luce, Edward A. (1988). "The Use of Maggots in Wound Debridement". Annals of Plastic Surgery 21 (4): 388–91. doi:10.1097/00000637-198810000-00017. PMID 3232928.
- ↑ Jordan, Ashley; Khiyani, Neeraj; Bowers, Steven R.; Lukaszczyk, John J.; Stawicki, Stanislaw P. (2018). "Maggot debridement therapy: A practical review". International Journal of Academic Medicine 4 (1): 21–34. doi:10.4103/IJAM.IJAM_6_18.
- ↑ Heuer, Heike; Heuer, Lutz (2011). "Blowfly Strike and Maggot Therapy: From Parasitology to Medical Treatment". in Mehlhorn, Heinz. Nature Helps. Parasitology Research Monographs. pp. 301–23. ISBN 978-3-642-19381-1. https://archive.org/details/naturehelpshowpl00hmeh.
- ↑ Bowling, Frank L.; Salgami, Eleanna V.; Boulton, Andrew J.M. (February 2007). "Larval Therapy: A Novel Treatment in Eliminating Methicillin-Resistant Staphylococcus aureus From Diabetic Foot Ulcers". Diabetes Care 30 (2): 370–371. doi:10.2337/dc06-2348. PMID 17259512.
- ↑ Andersen, A. S.; Joergensen, B.; Bjarnsholt, T.; Johansen, H.; Karlsmark, T.; Givskov, M.; Krogfelt, K. A. (2009). "Quorum-sensing-regulated virulence factors in Pseudomonas aeruginosa are toxic to Lucilia sericata maggots". Microbiology 156 (2): 400–7. doi:10.1099/mic.0.032730-0. PMID 19892758.
- ↑ 18.0 18.1 Sherman, R. A.; Hall, M. J. R.; Thomas, S. (2000). "Medicinal Maggots: An Ancient Remedy for Some Contemporary Afflictions". Annual Review of Entomology 45: 55–81. doi:10.1146/annurev.ento.45.1.55. PMID 10761570.
- ↑ Whitaker, I. S.; Twine, C; Whitaker, M. J. et al. (2007). "Larval therapy from antiquity to the present day: Mechanisms of action, clinical applications and future potential". Postgraduate Medical Journal 83 (980): 409–13. doi:10.1136/pgmj.2006.055905. PMID 17551073.
- ↑ Donnelly, J. (1998). "Wound healing--from poultices to maggots. (a short synopsis of wound healing throughout the ages)". The Ulster Medical Journal 67 (Suppl 1): 47–51. PMID 9807955.
- ↑ Baer, William S. (1931). "The treatment of chronic osteomyelitis with the maggot (larva of the blow fly)". The Journal of Bone and Joint Surgery 13 (3): 438–75. http://jbjs.org/content/13/3/438.abstract. Retrieved 2015-03-03.
- ↑ Roach, Mary (2016-06-07) (in en). Grunt: The Curious Science of Humans at War (1 ed.). W. W. Norton & Company. ISBN 978-0-393-24544-8.
- ↑ Nimmons, Don Stewart (2003) (in en). Treasures of War. Xulon Press. p. 105. ISBN 978-1-59160-460-0. https://books.google.com/books?id=WTW-oTQhdj0C&pg=PA105.
- ↑ Congressional Record. Pt 6. 152. 8 May 2006. pp. 7,908.
- ↑ Heitkamp, Rae A.; Peck, George W.; Kirkup, Benjamin C. (2013-11-14). "Maggot Debridement Therapy in Modern Army Medicine: Perceptions and Prevalence" (in en). Military Medicine 177 (11): 1,411–16. doi:10.7205/milmed-d-12-00200. PMID 23198524.
- ↑ Carrie Arnold for Scientific American. April 1, 2013 New Science Shows How Maggots Heal Wounds
- ↑ FDA CDRH 510(k) summary
- ↑ Root-Bernstein, Robert; Root-Bernstein, Michèle M. (1998). Honey, Mud, Maggots, and Other Medical Marvels. Houghton Mifflin. ISBN 978-0-395-92492-1.[unreliable medical source?]
- ↑ Sherman, Ronald A.; Morrison, Scott; Ng, David (2007). "Maggot debridement therapy for serious horse wounds – A survey of practitioners". The Veterinary Journal 174 (1): 86–91. doi:10.1016/j.tvjl.2006.05.012. PMID 16831562.
- ↑ Jones, Gemma; Wall, Richard (2008). "Maggot-therapy in veterinary medicine". Research in Veterinary Science 85 (2): 394–8. doi:10.1016/j.rvsc.2007.12.006. PMID 18237754.
Further reading
- Sherman, R. A. (2003). "Maggot Therapy for Treating Diabetic Foot Ulcers Unresponsive to Conventional Therapy". Diabetes Care 26 (2): 446–51. doi:10.2337/diacare.26.2.446. PMID 12547878.
- Van Der Plas, M. J. A.; Jukema, G. N.; Wai, S.-W.; Dogterom-Ballering, H. C. M.; Lagendijk, E. L.; Van Gulpen, C.; Van Dissel, J. T.; Bloemberg, G. V. et al. (2007). "Maggot excretions/secretions are differentially effective against biofilms of Staphylococcus aureus and Pseudomonas aeruginosa". Journal of Antimicrobial Chemotherapy 61 (1): 117–22. doi:10.1093/jac/dkm407. PMID 17965032.
- Cazander, G.; Van Veen, K.E.B.; Bernards, A.T.; Jukema, G.N. (2009). "Do maggots have an influence on bacterial growth? A study on the susceptibility of strains of six different bacterial species to maggots of Lucilia sericata and their excretions/secretions". Journal of Tissue Viability 18 (3): 80–7. doi:10.1016/j.jtv.2009.02.005. PMID 19362001.
- Cazander, Gwendolyn; Schreurs, Marco W. J.; Renwarin, Lennaert; Dorresteijn, Corry; Hamann, Dörte; Jukema, Gerrolt. N. (2012). "Maggot excretions affect the human complement system". Wound Repair and Regeneration 20 (6): 879–86. doi:10.1111/j.1524-475X.2012.00850.x. PMID 23110586.
- Mumcuoglu, Kosta Y.; Ingber, Arieh; Gilead, Leon; Stessman, Jochanan; Friedmann, Reuven; Schulman, Haim; Bichucher, Hellen; Ioffe-Uspensky, I et al. (1999). "Maggot therapy for the treatment of intractable wounds". International Journal of Dermatology 38 (8): 623–7. doi:10.1046/j.1365-4362.1999.00770.x. PMID 10487456.
- Bowler, P. G.; Duerden, B. I.; Armstrong, D. G. (2001). "Wound Microbiology and Associated Approaches to Wound Management". Clinical Microbiology Reviews 14 (2): 244–69. doi:10.1128/CMR.14.2.244-269.2001. PMID 11292638.
- Sherman, R. A.; Hall, M. J. R.; Thomas, S. (2000). "Medicinal Maggots: An Ancient Remedy for Some Contemporary Afflictions". Annual Review of Entomology 45: 55–81. doi:10.1146/annurev.ento.45.1.55. PMID 10761570.
- Nigam, Yamni; Bexfield, Alyson; Thomas, Stephen; Ratcliffe, Norman Arthur (2006). "Maggot Therapy: The Science and Implication for CAM Part I—History and Bacterial Resistance". Evidence-Based Complementary and Alternative Medicine 3 (2): 223–7. doi:10.1093/ecam/nel021. PMID 16786052.
External links
- Maggot Medicine film produced by Robert Cibis
- National Geographic video segment on Maggot Medicine on youtube.com
- The NIH Record; Medieval Miracle Workers — Are Maggots Making a Medical Comeback? The National Institutes of Health experience with maggot therapy
 |

