Medicine:Fibrosis
| Fibrosis | |
|---|---|
 | |
| Micrograph of a heart showing fibrosis (yellow – left of image) and amyloid deposition (brown – right of image). Stained using Movat's stain. | |
| Specialty | Pathology, rheumatology |
| Complications | Cirrhosis |
| Risk factors | Repeated injuries, chronic inflammation.[1] |
Fibrosis, also known as fibrotic scarring, is a pathological wound healing in which connective tissue replaces normal parenchymal tissue to the extent that it goes unchecked, leading to considerable tissue remodelling and the formation of permanent scar tissue.[1][2]
Repeated injuries, chronic inflammation and repair are susceptible to fibrosis, where an accidental excessive accumulation of extracellular matrix components, such as the collagen, is produced by fibroblasts, leading to the formation of a permanent fibrotic scar.[1]
In response to injury, this is called scarring, and if fibrosis arises from a single cell line, this is called a fibroma. Physiologically, fibrosis acts to deposit connective tissue, which can interfere with or totally inhibit the normal architecture and function of the underlying organ or tissue. Fibrosis can be used to describe the pathological state of excess deposition of fibrous tissue, as well as the process of connective tissue deposition in healing.[3] Defined by the pathological accumulation of extracellular matrix (ECM) proteins, fibrosis results in scarring and thickening of the affected tissue — it is in essence an exaggerated wound healing response which interferes with normal organ function.[4]
Physiology
Fibrosis is similar to the process of scarring, in that both involve stimulated fibroblasts laying down connective tissue, including collagen and glycosaminoglycans. The process is initiated when immune cells such as macrophages release soluble factors that stimulate fibroblasts. The most well characterized pro-fibrotic mediator is TGF beta, which is released by macrophages as well as any damaged tissue between surfaces called interstitium. Other soluble mediators of fibrosis include CTGF, platelet-derived growth factor (PDGF), and interleukin 10 (IL-10). These initiate signal transduction pathways such as the AKT/mTOR[5] and SMAD[6] pathways that ultimately lead to the proliferation and activation of fibroblasts, which deposit extracellular matrix into the surrounding connective tissue. This process of tissue repair is a complex one, with tight regulation of extracellular matrix (ECM) synthesis and degradation ensuring maintenance of normal tissue architecture. However, the entire process, although necessary, can lead to a progressive irreversible fibrotic response if tissue injury is severe or repetitive, or if the wound healing response itself becomes deregulated.[4][7]
Anatomical location
Fibrosis can occur in many tissues within the body, typically as a result of inflammation or damage. Common sites of fibrosis include the lungs, liver, kidneys, brain, and heart:
Lungs
- Fibrothorax
- Pulmonary fibrosis
- Cystic fibrosis
- Idiopathic pulmonary fibrosis (idiopathic - "of unknown cause")
- Radiation-induced lung injury (following radiation therapies commonly used to treat cancer)
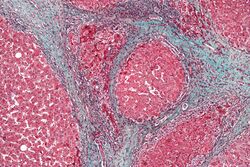
Liver
- Bridging fibrosis An advanced stage of liver fibrosis, seen in the progressive form of chronic liver diseases. The term “bridging” refers to the formation of a “bridge” by a band of mature and thick fibrous tissue from the portal area to the central vein. This form of fibrosis leads to the formation of pseudolobules. Long-term exposure to hepatotoxins, such as thioacetamide, carbon tetrachloride, and diethylnitrosamine, has been shown to cause bridging fibrosis in experimental animal models.[8]
- Senescence of hepatic stellate cells could prevent progression of liver fibrosis, although has not yet been implemented as a therapy due to risks assosciated with hepatic dysfunction.[9]
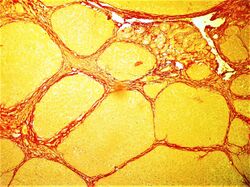
Kidney
- CYR61 induction of cellular senescence in the kidney has shown potential to limit renal fibrosis.[10]
Brain
- Glial scar
Heart
Myocardial fibrosis has two forms:
- Interstitial fibrosis, described in cases of congestive heart failure and hypertension, and as part of normal cellular aging.[11]
- Replacement fibrosis, indicating tissue damage from previous myocardial infarction.[11]
-
Healthy myocardium versus interstitial fibrosis in dilated cardiomyopathy. Alcian blue stain.
-
Replacement fibrosis in myocardial infarction, being boundless and dense.
Other
- Arterial stiffness
- Arthrofibrosis (knee, shoulder, other joints)
- Chronic kidney disease[12]
- Crohn's disease (intestine)
- Dupuytren's contracture (hands, fingers)
- Keloid (skin)
- Lipedema (fat cells, typically in lower limbs)
- Mediastinal fibrosis (soft tissue of the mediastinum)
- Myelofibrosis (bone marrow)
- Myofibrosis (skeletal muscle)[13]
- Peyronie's disease (penis)
- Nephrogenic systemic fibrosis (skin)
- Progressive massive fibrosis (lungs); a complication of pneumoconiosis
- Retroperitoneal fibrosis (soft tissue of the retroperitoneum)
- Scleroderma/systemic sclerosis (skin, lungs)
- Some forms of adhesive capsulitis (shoulder)
Fibrosis Reversal
Historically, fibrosis was considered an irreversible process. However, several recent studies have demonstrated reversal in liver and lung tissue,[14][15][16] and in cases of renal,[17] myocardial,[18] and oral-submucosal fibrosis.[19]
References
- ↑ 1.0 1.1 1.2 "Fibrotic disease and the T(H)1/T(H)2 paradigm". Nature Reviews. Immunology (Springer Science and Business Media LLC) 4 (8): 583–594. August 2004. doi:10.1038/nri1412. PMID 15286725.
- ↑ "Type-1 pericytes accumulate after tissue injury and produce collagen in an organ-dependent manner". Stem Cell Research & Therapy 5 (6): 122. November 2014. doi:10.1186/scrt512. PMID 25376879.
- ↑ "Glossary of dermatopathological terms.". DermNet NZ. http://dermnetnz.org/pathology/pathology-glossary.html.
- ↑ 4.0 4.1 "Epigenetics and the overhealing wound: the role of DNA methylation in fibrosis". Fibrogenesis & Tissue Repair 8: 18. 2015. doi:10.1186/s13069-015-0035-8. PMID 26435749.
- ↑ "Dual mTOR Inhibition Is Required to Prevent TGF-β-Mediated Fibrosis: Implications for Scleroderma". The Journal of Investigative Dermatology 135 (11): 2873–2876. November 2015. doi:10.1038/jid.2015.252. PMID 26134944.
- ↑ "TGF-beta signaling and the fibrotic response". FASEB Journal 18 (7): 816–827. May 2004. doi:10.1096/fj.03-1273rev. PMID 15117886.
- ↑ "Pulmonary fibrosis, part I: epidemiology, pathogenesis, and diagnosis". Expert Review of Respiratory Medicine 11 (5): 343–359. May 2017. doi:10.1080/17476348.2017.1312346. PMID 28345383.
- ↑ "Glibenclamide protects against thioacetamide-induced hepatic damage in Wistar rat: investigation on NLRP3, MMP-2, and stellate cell activation". Naunyn-Schmiedeberg's Archives of Pharmacology 391 (11): 1257–1274. November 2018. doi:10.1007/s00210-018-1540-2. PMID 30066023.
- ↑ "Hepatic stellate cell senescence in liver fibrosis: Characteristics, mechanisms and perspectives". Mechanisms of Ageing and Development 199: 111572. October 2021. doi:10.1016/j.mad.2021.111572. PMID 34536446.
- ↑ "Cellular senescence in the aging and diseased kidney". Journal of Cell Communication and Signaling 12 (1): 69–82. March 2018. doi:10.1007/s12079-017-0434-2. PMID 29260442.
- ↑ 11.0 11.1 "The Non-Fibrillar Side of Fibrosis: Contribution of the Basement Membrane, Proteoglycans, and Glycoproteins to Myocardial Fibrosis". Journal of Cardiovascular Development and Disease 6 (4): 35. September 2019. doi:10.3390/jcdd6040035. PMID 31547598.
- ↑ "Cellular and molecular mechanisms in kidney fibrosis". The Journal of Clinical Investigation 124 (6): 2299–2306. June 2014. doi:10.1172/JCI72267. PMID 24892703.
- ↑ "Chapter 2 - Musculoskeletal Diseases and Related Terms" (in en). A Manual of Orthopaedic Terminology (Eighth ed.). Philadelphia: W.B. Saunders. January 2015. pp. 43–104. doi:10.1016/B978-0-323-22158-0.00002-0. ISBN 978-0-323-22158-0.
- ↑ Ismail MH, Pinzani M. Reversal of liver fibrosis. Saudi J Gastroenterol. 2009 Jan;15(1):72-9. doi: 10.4103/1319-3767.45072. PMID 19568569; PMCID: PMC2702953.
- ↑ Zoubek ME, Trautwein C, Strnad P. Reversal of liver fibrosis: From fiction to reality. Best Pract Res Clin Gastroenterol. 2017 Apr;31(2):129-141. doi: 10.1016/j.bpg.2017.04.005. Epub 2017 Apr 24. PMID 28624101.
- ↑ C -H Chang, Y -H Juan, H -C Hu, K -C Kao, C -S Lee, Reversal of lung fibrosis: an unexpected finding in survivor of acute respiratory distress syndrome, QJM: An International Journal of Medicine, Volume 111, Issue 1, January 2018, Pages 47–48, https://doi.org/10.1093/qjmed/hcx190
- ↑ Eddy, A.A. Can renal fibrosis be reversed?. Pediatr Nephrol 20, 1369–1375 (2005). https://doi.org/10.1007/s00467-005-1995-
- ↑ Frangogiannis NG. Can Myocardial Fibrosis Be Reversed? J Am Coll Cardiol. 2019 May 14;73(18):2283-2285. doi: 10.1016/j.jacc.2018.10.094. PMID 31072571.
- ↑ Shetty SS, Sharma M, Kabekkodu SP, Kumar NA, Satyamoorthy K, Radhakrishnan R. Understanding the molecular mechanism associated with reversal of oral submucous fibrosis targeting hydroxylysine aldehyde-derived collagen cross-links. J Carcinog. 2021 Aug 13;20:9. doi: 10.4103/jcar.JCar_24_20. PMID 34526855; PMCID: PMC8411980.
External links
| Classification |
|---|
 |


