Biology:Megakaryocyte
A megakaryocyte (from mega- 'large', karyo- 'cell nucleus', and -cyte 'cell') is a large bone marrow cell with a lobated nucleus that produces blood platelets (thrombocytes), which are necessary for normal clotting. In humans, megakaryocytes usually account for 1 out of 10,000 bone marrow cells, but can increase in number nearly 10-fold during the course of certain diseases.[1] Owing to variations in combining forms and spelling, synonyms include megalokaryocyte and megacaryocyte.
Structure
In general, megakaryocytes are 10 to 15 times larger than a typical red blood cell, averaging 50–100 μm in diameter. During its maturation, the megakaryocyte grows in size and replicates its DNA without cytokinesis in a process called endomitosis. As a result, the nucleus of the megakaryocyte can become very large and lobulated, which, under a light microscope, can give the false impression that there are several nuclei. In some cases, the nucleus may contain up to 64N DNA, or 32 copies of the normal complement of DNA in a human cell.
The cytoplasm, just as the platelets that bud off from it, contains α-granules and dense bodies.
Heterogeneity and Functional Subpopulations
Recent single-cell RNA sequencing studies have revealed that megakaryocytes are not a homogeneous population, but rather comprise distinct subpopulations with specialized functions.[2][3] Megakaryocytes can be transcriptionally categorized into platelet generating, niche supporting, immune, and cycling cells, which are distinguished by their unique gene expression patterns and cellular markers.[2]
These functional subpopulations include:
Thrombopoietic megakaryocytes: The classic platelet-producing cells with high expression of genes involved in platelet formation and release.
Immune megakaryocytes: A significant population of these cells have been established to reside in the non-hematopoietic tissues and they display enhanced immune-related characteristics.[2] These cells express higher levels of immune-related genes and can participate in antigen presentation and immune responses.
Niche-supporting megakaryocytes: Megakaryocytes that support hematopoietic stem cell maintenance in the bone marrow niche through production of regulatory factors such as CXCL4 (platelet factor 4), transforming growth factor-β1, and fibroblast growth factor 1.[4][5]
Cycling megakaryocytes: Proliferating precursor cells that give rise to the mature megakaryocyte subtypes.[3]
Development
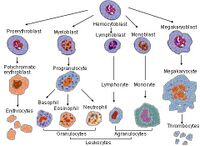
The megakaryocyte develops through the following lineage:
- CFU-Meg (hematopoietic stem cell/hemocytoblast) → megakaryoblast → promegakaryocyte → megakaryocyte
Megakaryocytes are derived from hematopoietic stem cell precursor cells in the bone marrow. They are produced primarily by the liver, kidney, spleen, and bone marrow. These multipotent stem cells live in the marrow sinusoids and are capable of producing all types of blood cells depending on the signals they receive. The primary signal for megakaryocyte production is thrombopoietin (TPO). TPO is sufficient but not absolutely necessary[6] for inducing differentiation of progenitor cells in the bone marrow towards a final megakaryocyte phenotype. Other molecular signals for megakaryocyte differentiation include GM-CSF, IL-3, IL-6, IL-11, chemokines (SDF-1, FGF-4),[7] and erythropoietin.[8]
The cell eventually reaches megakaryocyte stage and loses its ability to divide. However, it is still able to replicate its DNA and continue development, becoming polyploid.[8] The cytoplasm continues to expand and the DNA amount can increase up to 64n in humans and 256n in mice. Many of the morphological features of megakaryocyte differentiation can be recapitulated in non-hematopoietic cells by the expression of Class VI β-tubulin (β6) and they provide a mechanistic basis for understanding these changes.[9]
Stress-Induced Pathways
In recent years, several landmark studies have revealed novel insights into the regulation of megakaryopoiesis under stress conditions. It has been well-documented that systemic inflammation can lead to acute thrombocytopenia or thrombocytosis.[10]
Function
Platelet release
Once the cell has completed differentiation and become a mature megakaryocyte, it begins the process of producing platelets. The maturation process occurs via endomitotic synchronous replication whereby the cytoplasmic volume enlarges as the number of chromosomes multiplies without cellular division. The cell ceases its growth at 4N, 8N or 16N, becomes granular, and begins to produce platelets.[11] Thrombopoietin plays a role in inducing the megakaryocyte to form small proto-platelet processes. Platelets are held within these internal membranes within the cytoplasm of megakaryocytes. There are two proposed mechanisms for platelet release. In one scenario, these proto-platelet processes break up explosively to become platelets.[12] It is possible to visualize the spontaneous release of platelets using holotomographic live-cell imaging. Alternatively, the cell may form platelet ribbons into blood vessels. The ribbons are formed via pseudopodia and they are able to continuously emit platelets into circulation. In either scenario, each of these proto-platelet processes can give rise to 2000–5000 new platelets upon breakup. Overall, 2/3 of these newly produced platelets will remain in circulation while 1/3 will be sequestered by the spleen.
Thrombopoietin (TPO) is a 353-amino acid protein encoded on chromosome 3p27. TPO is primarily synthesized in the liver[13] but can be made by kidneys, testes, brain, and even bone marrow stromal cells. It has high homology with erythropoietin. It is essential for the formation of an adequate quantity of platelets.
After budding off platelets, what remains is mainly the cell nucleus. This crosses the bone marrow barrier to the blood and is consumed in the lung by alveolar macrophages.
Effects of cytokines
Cytokines are signals used in the immune system for intercellular communication. There are many cytokines that affect megakaryocytes. Certain cytokines such as IL-3, IL-6, IL-11, LIF, erythropoietin, and thrombopoietin all stimulate the maturation of megakaryocytic progenitor cells.[14] Other signals such as PF4, CXCL5, CXCL7, and CCL5 inhibit platelet formation.[15]
Role in Hematopoietic Stem Cell Niche
Megakaryocytes play a crucial role in maintaining the hematopoietic stem cell (HSC) niche in the bone marrow, representing a feedback mechanism where HSC-derived cells regulate their progenitors.[16]
HSC Quiescence Regulation
Recent studies showed that megakaryocytes localize specifically with a subset of HSCs, and promotes their quiescence through the production of CXCL4 (also known as platelet factor-4) and transforming growth factor-β1.[17] Specifically:
- Spatial organization: Almost all VWF+ (megakaryocyte-biased) HSCs exist within 5μm of megakaryocytes, but are not significantly associated with arterioles.[18]
- Factor secretion: Megakaryocytes produce multiple HSC-regulatory factors including CXCL4, TGF-β1, and thrombopoietin that maintain HSC quiescence during homeostasis.[17]
Stress Response and Regeneration
Functionally, megakaryocytic IGF-1 hypersecretion promotes self-renewal and expansion of HSC through delicately coordinating proliferation, mitochondrial oxidative metabolism and ferroptosis to safeguard efficient HSC regeneration after injury.[19] During stress conditions:
- Myeloablative injury: Even after lethal irradiation-induced myeloablative conditioning, megakaryocytes also survive, migrate to the endosteal niche and drive endosteal niche expansion through the paracrine effect of platelet-derived growth factor-BB to facilitate the engraftment of transplanted HSC.[19]
- FGF1 signaling: FGF1 production by megakaryocytes can also promote HSC expansion under stress.[17]
Extravascular Localization and Tissue-Specific Functions
Traditionally considered bone marrow–resident cells, megakaryocytes are also found in extravascular locations such as the lungs and spleen, where they exhibit distinct morphologies and tissue-specific functions. In the lungs, extravascular megakaryocytes—smaller and more sessile—constitute up to 80% of the lung megakaryocyte population and express higher levels of cytokines, growth factors, and host defense genes, potentially contributing to inflammation during lung disease.[20] Single-cell RNA sequencing revealed that lung megakaryocytes (MkL) display gene expression patterns similar to antigen-presenting cells,[21] with in vitro and in vivo assays showing their ability to internalize and process antigenic proteins and bacterial pathogens, and to activate CD4⁺ T cells in an MHC II–dependent manner. Additionally, lung megakaryocytes in alveolar and interstitial regions exhibit location-dependent characteristics, responding rapidly to inhaled particles by engulfing them and upregulating inflammatory and thrombopoietic pathways.[22] In contrast, during pathological conditions such as sepsis, megakaryocytes can develop extramedullary in the spleen, producing a unique platelet subpopulation with high CD40L expression capable of inducing NETosis in neutrophils—a function not observed in bone marrow or lung megakaryocytes.[3]
Clinical significance
Megakaryocytes are directly responsible for producing platelets, which are needed for the formation of a thrombus, or blood clot. There are several diseases that are directly attributable to abnormal megakaryocyte function or abnormal platelet function.[23]
Essential thrombocythemia
Essential thrombocythemia (ET) is a disorder characterized by elevated numbers of circulating platelets. The disease occurs in 1–2 per 100,000 people. The 2016 WHO requirements for diagnosis include > 450,000 platelets/μL of blood (normal 150,000–400,000) and characteristic findings in a bone marrow biopsy. Some of the consequences of having such high numbers of platelets include thrombosis or clots in blood vessels. Thrombi form more frequently in arteries than veins. It seems ironic that having platelet counts above 1,000,000 platelets/μL can lead to hemorrhagic events.[24] Approximately half ET cases are due to a mutation in the JAK2 protein, a member of the JAK-STAT signaling pathway.[25] This mutation induces an unregulated proliferative signal from the thrombopoietin (TPO) receptor in the absence of TPO causing clonal expansion of bone marrow cells, especially megakaryocytes. There is a low risk of transformation to leukemia with this disorder. The primary treatment consists of anagrelide or hydroxyurea to lower platelet levels.
Congenital amegakaryocytic thrombocytopenia
Congenital amegakaryocytic thrombocytopenia (CAMT) is a rare inherited disorder. The primary manifestations are thrombocytopenia and megakaryocytopenia, for example low numbers of platelets and megakaryocytes. There is an absence of megakaryocytes in the bone marrow with no associated physical abnormalities.[26] The cause for this disorder appears to be a mutation in the gene for the TPO receptor, c-mpl, despite high levels of serum TPO.[27][28] In addition, there may be abnormalities with the central nervous system including the cerebrum and cerebellum that could cause symptoms.[27] The primary treatment for CAMT is bone marrow transplantation.
Bone marrow/stem cell transplant is the only remedy for this genetic disease. Frequent platelet transfusions are required to keep the patient from bleeding to death until transplant has been completed, although this is not always the case.
There appears to be no generic resource for CAMT patients on the web and this is potentially due to the rarity of the disease.
COVID-19 and Viral Infections
Recent research has revealed important roles of megakaryocytes in viral infections, particularly COVID-19. SARS-CoV-2 infection is associated with platelet hyperreactivity and increased rates of arterial and venous thrombosis.[29] SARS-CoV-2 mutations have resulted in several variants with differences in transmissibility, infectivity, and patient outcomes. Studies have shown that megakaryocytes can be directly infected by SARS-CoV-2, affecting both their transcriptome and platelet production.[30]
History
Early Discovery of Megakaryocytes (1869-1890s)
The history of megakaryocyte research begins with Italian pathologist Giulio Bizzozero (1846-1901), who first described these cells in 1869 as "giant bone marrow cells" or "Bizzozero's giant bone marrow cells."[31][32] Bizzozero, a pioneer of histology and one of the founders of modern hematology, was responsible for fundamental advances including the discovery of the hematopoietic function of the bone marrow and the observation of platelets.[31]
In 1868 Bizzozero demonstrated the erythrocytopoietic function of bone marrow, which he illustrated in several works, and in 1869 he discovered the megakaryocytes. However, despite his groundbreaking work identifying both platelets (1881) and megakaryocytes, Bizzozero never recognized the connection between these two cellular elements.[33]
In 1890, William Howell first coined the term "megakaryocyte" to describe these large bone marrow cells.[34]
Establishment of the Platelet-Megakaryocyte Connection (1906-1920)
James Homer Wright provided the crucial evidence in 1906 that megakaryocytes give rise to blood platelets, establishing for the first time the cellular relationship between these giant bone marrow cells and the small circulating platelets.[35][36]
In 1906, Wright introduced the initial concept that platelets arise from megakaryocyte extensions when he described the detachment of platelets from megakaryocyte pseudopods. Wright used his newly developed Wright's stain to demonstrate similarities between megakaryocyte granules and platelets and through microscopic analysis.[35]
In 1920, Di Guglielmo published detailed morphological observations showing megakaryocytes releasing platelets through two mechanisms: formation of long cytoplasmic extensions and direct fragmentation of cytoplasm - both mechanisms later confirmed by modern research.[31]
The Search for Thrombopoietin (1958-1994)
A major milestone in megakaryocyte research came in 1958 when Endre Kelemen and colleagues first coined the term "thrombopoietin" to describe the humoral substance responsible for the production of platelets.[37][38] Conspicuously absent from this golden age of HGF discovery was a growth factor for platelet production, dubbed thrombopoietin by Kelemen in 1958.
The term thrombopoietin (TPO) was coined in 1958 to describe the humoral substance responsible for platelet production following induced thrombocytopenia by Kelemen, Cserhati, and Tanos, who demonstrated its presence in thrombocythemic sera.[39]
For nearly four decades, scientists searched for this elusive factor. Despite several claims of the purification of thrombopoietin, none of these efforts led to the cloning of the molecule, the sine qua non of HGF identification. The breakthrough came when the proto-oncogene c-Mpl was identified in 1992, providing the key to finally isolating thrombopoietin.
Modern Era: Molecular Cloning and Clinical Applications (1994-Present)
Thrombopoietin, the primary regulator of blood platelet production, was postulated to exist in 1958, but was only proven to exist when the cDNA for the hormone was cloned in 1994. In 1994, five independent research teams simultaneously cloned thrombopoietin using different approaches, ending the 36-year search for this crucial hormone.[40][41][42]
This discovery revolutionized understanding of megakaryocyte biology and platelet production, leading to new therapeutic approaches for thrombocytopenia and deeper insights into hematopoietic stem cell regulation.
See also
- List of distinct cell types in the adult human body
References
- ↑ "Megakaryocyte quantifications in relation to thrombokinetics in primary thrombocythaemia and allied diseases". Scand. J. Haematol. 15 (5): 321–32. 1975. doi:10.1111/j.1600-0609.1975.tb01087.x. PMID 1060175.
- ↑ 2.0 2.1 2.2 Guo, Karen; Machlus, Kellie R.; Camacho, Virginia (January 2024). "The many faces of the megakaryocytes and their biological implications" (in en). Current Opinion in Hematology 31 (1): 1–5. doi:10.1097/MOH.0000000000000793. ISSN 1065-6251. PMID 37910197.
- ↑ 3.0 3.1 3.2 Puhm, Florian; Laroche, Audrée; Boilard, Eric (November 2023). "Diversity of Megakaryocytes". Arteriosclerosis, Thrombosis, and Vascular Biology 43 (11): 2088–2098. doi:10.1161/ATVBAHA.123.318782. PMID 37675634. https://www.ahajournals.org/doi/10.1161/ATVBAHA.123.318782.
- ↑ Zhao, Meng; Perry, John M.; Marshall, Heather; Venkatraman, Aparna; Qian, Pengxu; He, Xi C.; Ahamed, Jasimuddin; Li, Linheng (November 2014). "Megakaryocytes maintain homeostatic quiescence and promote post-injury regeneration of hematopoietic stem cells" (in en). Nature Medicine 20 (11): 1321–1326. doi:10.1038/nm.3706. ISSN 1546-170X. PMID 25326798. https://www.nature.com/articles/nm.3706.
- ↑ Bruns, Ingmar; Lucas, Daniel; Pinho, Sandra; Ahmed, Jalal; Lambert, Michele P.; Kunisaki, Yuya; Scheiermann, Christoph; Schiff, Lauren et al. (November 2014). "Megakaryocytes regulate hematopoietic stem cell quiescence through CXCL4 secretion" (in en). Nature Medicine 20 (11): 1315–1320. doi:10.1038/nm.3707. ISSN 1546-170X. PMID 25326802.
- ↑ "Normal platelets and megakaryocytes are produced in vivo in the absence of thrombopoietin". Blood 90 (9): 3423–29. November 1997. doi:10.1182/blood.V90.9.3423. PMID 9345025.
- ↑ "Chemokine-mediated interaction of hematopoietic progenitors with the bone marrow vascular niche is required for thrombopoiesis". Nat Med 10 (1): 64–71. January 2004. doi:10.1038/nm973. PMID 14702636.
- ↑ 8.0 8.1 "Megakaryocyte development and platelet production". Br. J. Haematol. 134 (5): 453–66. September 2006. doi:10.1111/j.1365-2141.2006.06215.x. PMID 16856888.
- ↑ Yang, H; Ganguly, A; Cabral, F (2012). "Megakaryocyte Lineage Specific Class VI β-Tubulin Suppresses Microtubule Dynamics, Fragments Microtubules, and Blocks Cell Division.". Cytoskeleton 68 (3): 175–87. doi:10.1002/cm.20503. PMID 21309084.
- ↑ Noetzli, Leila J.; French, Shauna L.; Machlus, Kellie R. (July 2019). "New Insights Into the Differentiation of Megakaryocytes From Hematopoietic Progenitors". Arteriosclerosis, Thrombosis, and Vascular Biology 39 (7): 1288–1300. doi:10.1161/ATVBAHA.119.312129. ISSN 1524-4636. PMID 31043076.
- ↑ Hoffbrand, A. V.; Pettit, J. E.; Vyas, Paresh (2010). Megakaryocyte and Platelet Production. ISBN 978-0-323-04453-0. http://www.expertconsultbook.com/expertconsult/ob/book.do?method=display&type=bookPage&decorator=none&eid=4-u1.0-B978-0-323-04453-0..50006-9--cesec3&isbn=978-0-323-04453-0.
- ↑ "Platelets generated in vitro from proplatelet-displaying human megakaryocytes are functional". Blood 85 (2): 402–13. 1995. doi:10.1182/blood.V85.2.402.402. PMID 7529062.
- ↑ Jelkmann W (2001). "The role of the liver in the production of thrombopoietin compared with erythropoietin". Eur. J. Gastroenterol. Hepatol. 13 (7): 791–801. doi:10.1097/00042737-200107000-00006. PMID 11474308.
- ↑ "Growth factors affecting human thrombocytopoiesis: potential agents for the treatment of thrombocytopenia". Blood 80 (2): 302–07. 1992. doi:10.1182/blood.V80.2.302.302. PMID 1627792.
- ↑ "Megakaryocyte biology and related disorders". J. Clin. Invest. 115 (12): 3332–38. 2005. doi:10.1172/JCI26720. PMID 16322777.
- ↑ Zhan, Huichun; Kaushansky, Kenneth (2022-01-01). "Megakaryocytes as the Regulator of the Hematopoietic Vascular Niche". Frontiers in Oncology 12. doi:10.3389/fonc.2022.912060. ISSN 2234-943X. PMID 35814384.
- ↑ 17.0 17.1 17.2 Boulais, Philip E.; Frenette, Paul S. (2015-04-23). "Making sense of hematopoietic stem cell niches". Blood 125 (17): 2621–2629. doi:10.1182/blood-2014-09-570192. ISSN 1528-0020. PMID 25762174.
- ↑ Pinho, Sandra; Marchand, Tony; Yang, Eva; Wei, Qiaozhi; Nerlov, Claus; Frenette, Paul S. (2018-03-12). "Lineage-Biased Hematopoietic Stem Cells Are Regulated by Distinct Niches". Developmental Cell 44 (5): 634–641.e4. doi:10.1016/j.devcel.2018.01.016. ISSN 1878-1551. PMID 29456137.
- ↑ 19.0 19.1 Du, Changhong; Chen, Jun; Wang, Junping (2025-07-01). "New insights into the generation and function of megakaryocytes in health and disease". Haematologica 110 (7): 1500–1512. doi:10.3324/haematol.2024.287236. ISSN 1592-8721. PMID 40145277.
- ↑ Yeung, Anthony K.; Villacorta-Martin, Carlos; Hon, Stephanie; Rock, Jason R.; Murphy, George J. (2020-12-22). "Lung megakaryocytes display distinct transcriptional and phenotypic properties". Blood Advances 4 (24): 6204–6217. doi:10.1182/bloodadvances.2020002843. ISSN 2473-9537. PMID 33351116.
- ↑ Pariser, Daphne N.; Hilt, Zachary T.; Ture, Sara K.; Blick-Nitko, Sara K.; Looney, Mark R.; Cleary, Simon J.; Roman-Pagan, Estheany; Saunders, Jerry et al. (2021-01-04). "Lung megakaryocytes are immune modulatory cells". The Journal of Clinical Investigation 131 (1): e137377, 137377. doi:10.1172/JCI137377. ISSN 1558-8238. PMID 33079726.
- ↑ Qiu, Jiahuang; Ma, Juan; Dong, Zheng; Ren, Quanzhong; Shan, Qing'e; Liu, Jiao; Gao, Ming; Liu, Guoliang et al. (2024-08-27). "Lung megakaryocytes engulf inhaled airborne particles to promote intrapulmonary inflammation and extrapulmonary distribution". Nature Communications 15 (1): 7396. doi:10.1038/s41467-024-51686-y. ISSN 2041-1723. PMID 39191805. Bibcode: 2024NatCo..15.7396Q.
- ↑ Nurden AT (2005). "Qualitative disorders of platelets and megakaryocytes". Journal of Thrombosis and Haemostasis 3 (8): 1773–82. doi:10.1111/j.1538-7836.2005.01428.x. PMID 16102044.
- ↑ "Pathophysiology and treatment of platelet-mediated microvascular disturbances, major thrombosis and bleeding complications in essential thrombocythaemia and polycythaemia vera". Platelets 15 (2): 67–84. 2004. doi:10.1080/09537100310001646969. PMID 15154599.
- ↑ "A gain-of-function mutation of JAK2 in myeloproliferative disorders". N Engl J Med 352 (17): 1779–90. 2005-04-28. doi:10.1056/NEJMoa051113. PMID 15858187.
- ↑ "Congenital amegakaryocytic thrombocytopenia: an intrinsic hematopoietic stem cell defect". Am. J. Pediatr. Hematol. Oncol. 12 (2): 225–30. 1990. doi:10.1097/00043426-199022000-00020. PMID 2378417.
- ↑ 27.0 27.1 "Identification of mutations in the c-mpl gene in congenital amegakaryocytic thrombocytopenia". Proc. Natl. Acad. Sci. 96 (6): 3133–36. 1999. doi:10.1073/pnas.96.6.3132. PMID 10077649. Bibcode: 1999PNAS...96.3132I.
- ↑ "C-mpl mutations are the cause of congenital amegakaryocytic thrombocytopenia". Blood 97 (1): 139–46. 2001. doi:10.1182/blood.V97.1.139. PMID 11133753.
- ↑ Sowa, Marcin A.; Tuen, Michael; Schlamp, Florencia; Xia, Yuhe; Samanovic, Marie I.; Mulligan, Mark J.; Barrett, Tessa J. (December 2025). "Megakaryocyte phenotyping in response to SARS-CoV-2 variants". Platelets 36 (1). doi:10.1080/09537104.2025.2532459. ISSN 1369-1635. PMID 40702756.
- ↑ Allaeys, Isabelle; Lemaire, Guillaume; Leclercq, Mickaël; Lacasse, Emile; Fleury, Maude; Dubuc, Isabelle; Gudimard, Leslie; Puhm, Florian et al. (2024-06-11). "SARS-CoV-2 infection modifies the transcriptome of the megakaryocytes in the bone marrow". Blood Advances 8 (11): 2777–2789. doi:10.1182/bloodadvances.2023012367. ISSN 2473-9537. PMID 38522092.
- ↑ 31.0 31.1 31.2 Balduini, Carlo L. (2020-09-01). "100-Year-Old Haematologica Images: The Origin Of Megakaryocytes". Haematologica 105 (9): 2187. doi:10.3324/haematol.2020.262873. ISSN 1592-8721. PMID 33054039.
- ↑ Mazzarello, P.; Calligaro, A. L.; Calligaro, A. (October 2001). "Giulio Bizzozero: a pioneer of cell biology". Nature Reviews. Molecular Cell Biology 2 (10): 776–781. doi:10.1038/35096085. ISSN 1471-0072. PMID 11584305.
- ↑ Balduini, Carlo L. (2020-07-01). "100-Year-Old Haematologica Images: The Quarrel About The Origin Of Platelets (III)" (in en). Haematologica 105 (7): 1751. doi:10.3324/haematol.2020.256974. ISSN 1592-8721. PMID 32611572. PMC 7327630. https://haematologica.org/article/view/9923.
- ↑ Howell, W. H. (July 1890). "Observations upon the occurrence, structure, and function of the giant cells of the marrow" (in en). Journal of Morphology 4: 117–130. doi:10.1002/jmor.1050040106. ISSN 0362-2525. Bibcode: 1890JMorp...4..117H. http://deepblue.lib.umich.edu/handle/2027.42/50231.
- ↑ 35.0 35.1 Wright, James Homer (1910). "The histogenesis of the blood platelets" (in en). Journal of Morphology 21 (2): 263–278. doi:10.1002/jmor.1050210204. ISSN 1097-4687. Bibcode: 1910JMorp..21..263W. https://onlinelibrary.wiley.com/doi/abs/10.1002/jmor.1050210204.
- ↑ Nurden, Alan T.; Nurden, Paquita (August 2020). "Inherited thrombocytopenias: history, advances and perspectives". Haematologica 105 (8): 2004–2019. doi:10.3324/haematol.2019.233197. ISSN 1592-8721. PMID 32527953.
- ↑ Kelemen, E.; Cserhati, I.; Tanos, B. (December 1958). "Demonstration and some properties of human thrombopoietin in thrombocythaemic sera". Acta Haematologica 20 (6): 350–355. doi:10.1159/000205503. ISSN 0001-5792. PMID 13616931.
- ↑ Kaushansky, Kenneth (2024-04-18). "Thrombopoietin, the Primary Regulator of Platelet Production: From Mythos to Logos, a Thirty-Year Journey". Biomolecules 14 (4): 489. doi:10.3390/biom14040489. ISSN 2218-273X. PMID 38672505.
- ↑ Kaushansky, K. (July 2003). "Thrombopoietin: a tool for understanding thrombopoiesis". Journal of Thrombosis and Haemostasis 1 (7): 1587–1592. doi:10.1046/j.1538-7836.2003.00273.x. ISSN 1538-7933. PMID 12871295.
- ↑ Bartley, T. D.; Bogenberger, J.; Hunt, P.; Li, Y. S.; Lu, H. S.; Martin, F.; Chang, M. S.; Samal, B. et al. (1994-07-01). "Identification and cloning of a megakaryocyte growth and development factor that is a ligand for the cytokine receptor Mpl". Cell 77 (7): 1117–1124. doi:10.1016/0092-8674(94)90450-2. ISSN 0092-8674. PMID 8020099.
- ↑ de Sauvage, F. J.; Hass, P. E.; Spencer, S. D.; Malloy, B. E.; Gurney, A. L.; Spencer, S. A.; Darbonne, W. C.; Henzel, W. J. et al. (1994-06-16). "Stimulation of megakaryocytopoiesis and thrombopoiesis by the c-Mpl ligand". Nature 369 (6481): 533–538. doi:10.1038/369533a0. ISSN 0028-0836. PMID 8202154. Bibcode: 1994Natur.369..533D.
- ↑ Lok, S.; Kaushansky, K.; Holly, R. D.; Kuijper, J. L.; Lofton-Day, C. E.; Oort, P. J.; Grant, F. J.; Heipel, M. D. et al. (1994-06-16). "Cloning and expression of murine thrombopoietin cDNA and stimulation of platelet production in vivo". Nature 369 (6481): 565–568. doi:10.1038/369565a0. ISSN 0028-0836. PMID 8202158. Bibcode: 1994Natur.369..565L.
External links
- Megakaryocytes: Mature Many microscopic images of mature megakaryocytes including in disease settings.
- Megakaryocytes
- Cell size comparison
- CAMT Specific Infant Bone Marrow Transplant Journal
 |
