Medicine:Hypocalcemia
| Hypocalcemia | |
|---|---|
 | |
| Specialty | Endocrinology |
| Symptoms | Numbness, muscle spasms, seizures, confusion[1][2] |
| Complications | Cardiac arrest[1][2] |
| Causes | Hypoparathyroidism, vitamin D deficiency, kidney failure, pancreatitis, calcium channel blocker overdose, rhabdomyolysis, tumor lysis syndrome, bisphosphonates[1][2] |
| Diagnostic method | Blood serum < 2.1 mmol/L (corrected calcium or ionized calcium)[1][2][3] |
| Treatment | Calcium supplements, vitamin D, magnesium sulfate.[1][2] |
| Frequency | ~18% of people in hospital[4] |
Hypocalcemia is a medical condition characterized by low calcium levels in the blood serum.[5] The normal range of blood calcium is typically between 2.1–2.6 mmol/L (8.8–10.7 mg/dL, 4.3–5.2 mEq/L) while levels less than 2.1 mmol/L are defined as hypocalcemic.[1][3][6] Mildly low levels that develop slowly often have no symptoms.[2][4] Otherwise symptoms may include numbness, muscle spasms, seizures, confusion, or cardiac arrest.[1][2]
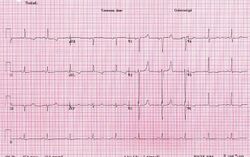
The most common cause for hypocalcemia is iatrogenic hypoparathyroidism.[2] Other causes include other forms of hypoparathyroidism, vitamin D deficiency, kidney failure, pancreatitis, calcium channel blocker overdose, rhabdomyolysis, tumor lysis syndrome, and medications such as bisphosphonates or denosumab.[1] Diagnosis should generally be confirmed with a corrected calcium or ionized calcium level.[2] Specific changes may be seen on an electrocardiogram (ECG).[1]
Initial treatment for severe disease is with intravenous calcium chloride and possibly magnesium sulfate.[1] Other treatments may include vitamin D, magnesium, and calcium supplements.[2] If due to hypoparathyroidism, hydrochlorothiazide, phosphate binders, and a low salt diet may also be recommended.[2] About 18% of people who are being treated in hospital have hypocalcemia.[4]
Signs and symptoms
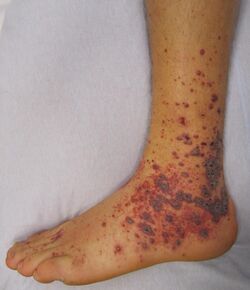
The neuromuscular symptoms of hypocalcemia are caused by a positive bathmotropic effect (i.e. increased responsiveness) due to the decreased interaction of calcium with sodium channels. Since calcium blocks sodium channels and inhibits depolarization of nerve and muscle fibers, reduced calcium lowers the threshold for depolarization.[7] The symptoms can be recalled by the mnemonic "CATs go numb" - convulsions, arrhythmias, tetany, and numbness in the hands and feet and around the mouth.[citation needed]
- Petechiae which appear as on-off spots, then later become confluent, and appear as purpura (larger bruised areas, usually in dependent regions of the body).[citation needed]
- Oral, perioral and acral paresthesias, tingling or 'pins and needles' sensation in and around the mouth and lips, and in the extremities of the hands and feet. This is often the earliest symptom of hypocalcaemia.
- Carpopedal and generalized tetany (unrelieved and strong contractions of the hands, and in the large muscles of the rest of the body) are seen.
- Latent tetany
- Trousseau sign of latent tetany (eliciting carpal spasm by inflating the blood pressure cuff and maintaining the cuff pressure above systolic)
- Chvostek's sign (tapping of the inferior portion of the cheekbone will produce facial spasms)[8]
- Tendon reflexes are hyperactive
- Life-threatening complications
- Cardiac arrhythmias
- Effects on cardiac output
- Negative chronotropic effect, or a decrease in heart rate.
- Negative inotropic effect, or a decrease in contractility
- ECG changes include the following:
- Intermittent QT prolongation, or intermittent prolongation of the QTc (corrected QT interval) on the ECG (electrocardiogram) is noted. The implications of intermittent QTc prolongation predisposes to life-threatening cardiac electrical instability (and this is therefore a more critical condition than constant QTc prolongation). This type of electrical instability puts the person at high risk of torsades de pointes, a specific type of ventricular tachycardia which appears on an EKG (or ECG) as something which looks a bit like a sine wave with a regularly increasing and decreasing amplitude. (Torsades de pointes can cause death, unless the person can be medically or electrically cardioverted and returned to a normal cardiac rhythm.)
Causes
Hypoparathyroidism is a common cause of hypocalcemia.[9] Calcium is tightly regulated by the parathyroid hormone (PTH). In response to low calcium levels, PTH levels rise, and conversely if there are high calcium levels then PTH secretion declines.[10] However, in the setting of absent, decreased, or ineffective PTH hormone, the body loses this regulatory function, and hypocalcemia ensues. Hypoparathyroidism is commonly due to surgical destruction of the parathyroid glands.[9] Hypoparathyroidism may also be due to autoimmune problem.[11][12] Some causes of hypocalcaemia are as follows:[citation needed]
- Hyperphosphatemia[13]
- Vitamin D deficiency
- Chronic liver disease
- Edetate disodium[13]
- Magnesium deficiency[14]
- Prolonged use of medications/laxatives (magnesium)[15]
- Osteomalacia[14]
- Chronic kidney failure[15]
- Ineffective active vitamin D[15]
- Hypoparathyroidism/genetic[15]
- After surgery hypoparathyroidism[15]
- Hungry bone syndrome
- Tumour lysis syndrome[16]
- Acute kidney injury[15]
- Rhabdomyolysis (initial stage)[14]
- As a complication of pancreatitis[14]
- Alkalosis[13]
- Massive red blood cell transfusion due to excess citrate in the blood
- As blood plasma hydrogen ion concentration decreases, caused by respiratory or metabolic alkalosis, the concentration of freely ionized calcium, the biologically active component of blood calcium, decreases. Because a portion of both hydrogen ions and calcium are bound to serum albumin, when blood becomes alkalotic, the bound hydrogen ions dissociate from albumin, freeing up the albumin to bind with more calcium and thereby decreasing the freely ionized portion of total serum calcium. For every 0.1 increase in pH, ionized calcium decreases by about 0.05 mmol/L. This hypocalcaemia related to alkalosis is partially responsible for the cerebral vasoconstriction that causes the lightheadedness, fainting, and paraesthesia often seen with hyperventilation.
- Neonatal hypocalcemia[17]
- Gain of function mutations of the calcium-sensing receptor
- Foscarnet use
- Loop diuretic use
- Crohn disease
- High level of lactic acid in the blood
- Pseudohypoparathyroidism
- Trauma[18]
Mechanism
Physiologically, blood calcium is tightly regulated within a narrow range for proper cellular processes. Calcium in the blood exists in three primary states: bound to proteins (mainly albumin), bound to anions such as phosphate and citrate, and as free (unbound) ionized calcium. Only the unbound ionized calcium is physiologically active. Normal blood calcium level is between 8.5 and 10.5 mg/dL (2.12 to 2.62 mmol/L) and that of unbound calcium is 4.65 to 5.25 mg/dL (1.16 to 1.31 mmol/L).[19]
Diagnosis
Because a significant portion of calcium is bound to albumin, any alteration in the level of albumin will affect the measured level of calcium. A corrected calcium level based on the albumin level is: Corrected calcium (mg/dL) = measured total Ca (mg/dL) + 0.8 * (4.0 - serum albumin [g/dL]).[20] Since calcium is also bound to small anions, it may be more useful to correct total calcium for both albumin and the anion gap.[21][22]
Management
Management of this condition includes:
- Intravenous calcium gluconate 10% can be administered, or if the hypocalcaemia is severe, calcium chloride is given instead. This is only appropriate if the hypocalcemia is acute and has occurred over a relatively short time frame. But if the hypocalcemia has been severe and chronic, then this regimen can be fatal, because there is a degree of acclimatization that occurs. The neuromuscular excitability, cardiac electrical instability, and associated symptoms are then not cured or relieved by prompt administration of corrective doses of calcium, but rather exacerbated. Such rapid administration of calcium would result in effective over correction – symptoms of hypercalcemia would follow.[citation needed]
- However, in either circumstance, maintenance doses of both calcium and vitamin-D (often as 1,25-(OH)2-D3, i.e. calcitriol) are often necessary to prevent further decline[citation needed]
See also
- Milk fever (hypocalcemia in animals)
- Calcium deficiency (plant disorder)
- Hypomagnesemia with secondary hypocalcemia
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 Soar, J; Perkins, GD; Abbas, G; Alfonzo, A; Barelli, A; Bierens, JJ; Brugger, H; Deakin, CD et al. (October 2010). "European Resuscitation Council Guidelines for Resuscitation 2010 Section 8. Cardiac arrest in special circumstances: Electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution.". Resuscitation 81 (10): 1400–33. doi:10.1016/j.resuscitation.2010.08.015. PMID 20956045.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 Fong, J; Khan, A (February 2012). "Hypocalcemia: updates in diagnosis and management for primary care". Canadian Family Physician 58 (2): 158–62. PMID 22439169.
- ↑ 3.0 3.1 Pathy, M.S. John (2006). "Appendix 1: Conversion of SI Units to Standard Units". Principles and practice of geriatric medicine. 2 (4. ed.). Chichester [u.a.]: Wiley. p. Appendix. doi:10.1002/047009057X.app01. ISBN 9780470090558.
- ↑ 4.0 4.1 4.2 Cooper, MS; Gittoes, NJ (7 June 2008). "Diagnosis and management of hypocalcaemia". BMJ (Clinical Research Ed.) 336 (7656): 1298–302. doi:10.1136/bmj.39582.589433.be. PMID 18535072.
- ↑ LeMone, Priscilla; Burke, Karen; Dwyer, Trudy; Levett-Jones, Tracy; Moxham, Lorna; Reid-Searl, Kerry (2015) (in en). Medical-Surgical Nursing. Pearson Higher Education AU. p. 237. ISBN 9781486014408. https://books.google.com/books?id=MDXiBAAAQBAJ&pg=PA237.
- ↑ Minisola, S; Pepe, J; Piemonte, S; Cipriani, C (2 June 2015). "The diagnosis and management of hypercalcaemia". BMJ (Clinical Research Ed.) 350: h2723. doi:10.1136/bmj.h2723. PMID 26037642.
- ↑ Armstrong, C. M.; Cota, Gabriel (1999). "Calcium block of Na+ channels and its effect on closing rate". Proceedings of the National Academy of Sciences of the United States of America 96 (7): 4154–4157. doi:10.1073/pnas.96.7.4154. PMID 10097179. Bibcode: 1999PNAS...96.4154A.
- ↑ Durlach, J; Bac, P; Durlach, V; Bara, M; Guiet-Bara, A (June 1997). "Neurotic, neuromuscular and autonomic nervous form of magnesium imbalance". Magnesium Research 10 (2): 169–95. PMID 9368238.
- ↑ 9.0 9.1 Nussey, S. S.; Whitehead, S. A. (2013-04-08). Endocrinology: An Integrated Approach. CRC Press. p. 194. ISBN 9780203450437. https://books.google.com/books?id=pjZvmnZpKXsC.
- ↑ Bijlani, R. L.; Manjunatha, S. (2010-11-26). Understanding Medical Physiology: A Textbook for Medical Students. Jaypee Brothers Publishers. p. 465. ISBN 9789380704814. https://books.google.com/books?id=gUoRYgERRZMC.[yes|permanent dead link|dead link}}]
- ↑ "Hypoparathyroidism. Parathyroid symptoms and disease | Patient". http://patient.info/doctor/hypoparathyroidism-pro.
- ↑ "Hypoparathyroidism" (in en-US). https://rarediseases.org/rare-diseases/hypoparathyroidism/. "These cases may be called autoimmune hypoparathyroidism and develop when the body's own immune system mistakenly attacks parathyroid tissue and leads to the loss of the secretion of parathyroid hormone."
- ↑ 13.0 13.1 13.2 Metheny, Norma (2012). Fluid and electrolyte balance : nursing considerations (5th ed.). Sudbury, MA: Jones & Bartlett Learning. p. 93. ISBN 978-0-7637-8164-4. https://books.google.com/books?id=6UNGDx4ifDcC&q=causes+of+hypocalcemia&pg=PA93. Retrieved 4 September 2015.
- ↑ 14.0 14.1 14.2 14.3 Helms, Richard (2006). Textbook of therapeutics : drug and disease management (8. ed.). Philadelphia, Pa. [u.a.]: Lippincott Williams & Wilkins. p. 1035. ISBN 978-0-7817-5734-8. https://books.google.com/books?id=aVmRWrknaWgC&q=causes+of+hypocalcemia&pg=PA1035. Retrieved 4 September 2015.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 Fong, Jeremy; Khan, Aliya (2012). "Hypocalcemia: updates in diagnosis and management for primary care". Canadian Family Physician 58 (2): 158–62. PMID 22439169.
- ↑ Hall, edited by Patrick T. Murray, Hugh R. Brady, Jesse B. (2006). Intensive care in nephrology. London: Taylor & Francis. p. 129. ISBN 978-0-203-02482-9. https://books.google.com/books?id=dndxlhiJABQC&q=tumor+lysis+syndrome+causes+of+hypocalcemia&pg=PA129. Retrieved 4 September 2015.
- ↑ MedlinePlus Encyclopedia Hypocalcemia - infants
- ↑ Kronstedt, Shane; Roberts, Nicholas; Ditzel, Ricky; Elder, Justin; Steen, Aimee; Thompson, Kelsey; Anderson, Justin; Siegler, Jeffrey (2022). "Hypocalcemia as a predictor of mortality and transfusion. A scoping review of hypocalcemia in trauma and hemostatic resuscitation.". Transfusion 62 (S1): S158–S166. doi:10.1111/trf.16965. PMID 35748676.
- ↑ Siyam, Fadi F.; Klachko, David M. (2013). "What Is Hypercalcemia? The Importance of Fasting Samples". Cardiorenal Medicine 3 (4): 232–238. doi:10.1159/000355526. ISSN 1664-3828. PMID 24474951.
- ↑ (in en) Fluids & Electrolytes: A 2-in-1 Reference for Nurses. Lippincott Williams & Wilkins. 2006. p. 122. ISBN 9781582554259. https://books.google.com/books?id=Ap2Gc5U0TPwC&pg=PA122.
- ↑ Yap, E; Roche-Recinos, A; Goldwasser, P (30 December 2019). "Predicting Ionized Hypocalcemia in Critical Care: An Improved Method Based on the Anion Gap". The Journal of Applied Laboratory Medicine 5 (1): 4–14. doi:10.1373/jalm.2019.029314. PMID 32445343.
- ↑ Yap, E; Ouyang, J; Puri, I; Melaku, Y; Goldwasser, P (1 June 2022). "Novel methods of predicting ionized calcium status from routine data in critical care: External validation in MIMIC-III". Clinica Chimica Acta 531: 375–381. doi:10.1016/j.cca.2022.05.003. PMID 35526587.
External links
| Classification | |
|---|---|
| External resources |
 |
