Biology:Mesenchymal stem cell
| Mesenchymal stem cell | |
|---|---|
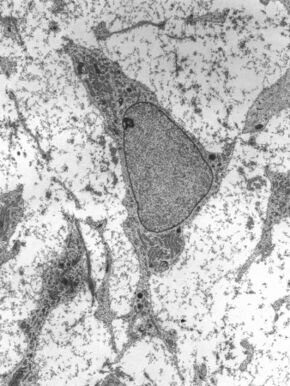 Transmission electron micrograph of a mesenchymal stem cell displaying typical ultrastructural characteristics | |
| Details | |
| Identifiers | |
| Latin | cellula mesenchymatica praecursoria |
| Anatomical terms of microanatomy | |
Mesenchymal stem cells (MSCs), also known as mesenchymal stromal cells or medicinal signaling cells, are multipotent stromal cells that can differentiate into a variety of cell types, including osteoblasts (bone cells), chondrocytes (cartilage cells), myocytes (muscle cells) and adipocytes (fat cells which give rise to marrow adipose tissue).[1][2][3][4]
The primary function of MSCs is to respond to injury and infection by secreting and recruiting a range of biological factors, as well as modulating inflammatory processes to facilitate tissue repair and regeneration. Extensive research interest has led to more than 80,000 peer-reviewed papers on MSCs.[5]
Structure
Definition
Mesenchymal stem cells (MSCs), a term first used (in 1991) by Arnold Caplan at Case Western Reserve University,[6] are characterized morphologically by a small cell body with long, thin cell processes.
The International Society for Cellular Therapy has identified a few criteria to define mesenchymal stem cell (MSC):[7]
- MSC must be plastic-adherent when maintained in standard culture conditions.
- MSC must express CD105, CD73 and CD90, and lack expression of CD45, CD34, CD14 or CD11b, CD79alpha or CD19 and HLA-DR surface molecules.
- MSC must differentiate to osteoblasts, adipocytes and chondroblasts in vitro.
While the terms mesenchymal stem cell (MSC) and marrow stromal cell have been used interchangeably for many years, neither term is sufficiently descriptive:
- Mesenchyme is embryonic connective tissue that is derived from the mesoderm and that differentiates into hematopoietic and connective tissue, whereas MSCs do not differentiate into hematopoietic cells.[8]
- Stromal cells are connective tissue cells that form the supportive structure in which the functional cells of the tissue reside. While this is an accurate description for one function of MSCs, the term fails to convey the relatively recently discovered roles of MSCs in the repair of tissue.[9]
- The term encompasses multipotent cells derived from other non-marrow tissues, such as placenta,[10] umbilical cord blood, adipose tissue, adult muscle, corneal stroma,[11] or the dental pulp of deciduous (baby) teeth.[12] The cells do not have the capacity to reconstitute an entire organ.
- Evidence shows that MSCs originate from progenitor perivascular cells called pericytes that reside on vessels.[13]
Morphology
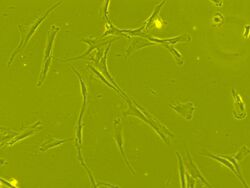

The cell body contains a large, round nucleus with a prominent nucleolus, which is surrounded by finely dispersed chromatin particles, giving the nucleus a clear appearance. The remainder of the cell body contains a small amount of Golgi apparatus, rough endoplasmic reticulum, mitochondria, and polyribosomes. The cells, which are long and thin, are widely dispersed, and the adjacent extracellular matrix is populated by a few reticular fibrils, but is devoid of the other types of collagen fibrils.[14][15] These distinctive morphological features of mesenchymal stem cells can be visualized label-free using live cell imaging.
Classification
Reviews have classified an MSC as having fibroblast-like structure, characterized by cell-surface markers and a potential to differentiate into bone, fat, or cartilage.[16][17]
Location in the body
MSCs are found throughout the human body.
Bone marrow
Bone marrow was the original source of MSCs,[18] and is still the most frequently utilized source. These bone marrow stem cells do not contribute to the formation of blood cells, and so do not express the hematopoietic stem cell marker CD34. They are sometimes referred to as bone marrow stromal stem cells.[19]
Cord cells
The youngest and most primitive MSCs may be obtained from umbilical cord tissue, namely Wharton's jelly and the umbilical cord blood. However, MSCs are found in much higher concentration in the Wharton's jelly compared to cord blood, which is a rich source of hematopoietic stem cells. The umbilical cord is available after a birth. It is normally discarded, and poses no risk for collection. These MSCs may prove to be a useful source of MSCs for clinical applications, due to their primitive properties and fast growth rate.[20]
Adipose tissue
Adipose-tissue-derived MSCs (AdMSCs), in addition to being easier and safer to isolate than bone-marrow-derived MSCs, can be obtained in larger quantities.[18][21]
Molar cells
The developing tooth bud of the mandibular third molar is a rich source of MSCs. While they are described as multipotent, it is possible that they are pluripotent. They eventually form enamel, dentin, blood vessels, dental pulp, and nervous tissues. These stem cells are capable of differentiating into chondrocytes, cardiomyocytes, melanocytes, and hepatocyte‐like cells in vitro.[12]
Amniotic fluid
Stem cells are present in amniotic fluid. As many as 1 in 100 cells collected during amniocentesis are pluripotent mesenchymal stem cells.[22]
Function
Differentiation capacity
MSCs have a great capacity for self-renewal while maintaining their multipotency. Recent work suggests that β-catenin, via regulation of EZH2, is a central molecule in maintaining the "stemness" of MSCs.[23] The standard test to confirm multipotency is differentiation of the cells into osteoblasts, adipocytes and chondrocytes as well as myocytes. Doubt remains about whether the MSC-derived neurons are functional.[24] The degree to which the culture will differentiate varies among individuals and how differentiation is induced, e.g., chemical vs. mechanical;[25] and it is not clear whether this variation is due to a different amount of "true" progenitor cells in the culture or variable differentiation capacities of individuals' progenitors. The capacity of cells to proliferate and differentiate is known to decrease with the age of the donor, as well as the time in culture.[26] Likewise, whether this is due to a decrease in the number of MSCs or a change to the existing MSCs is not known.
Immunomodulatory effects
MSCs have an effect on innate and specific immune cells, and research has shown an ability to suppress tumor growth.[27] MSCs produce many immunomodulatory molecules including prostaglandin E2 (PGE2),[28] nitric oxide,[29] indoleamine 2,3-dioxygenase (IDO), interleukin 6 (IL-6), and other surface markers such as FasL,[30] PD-L1 and PD-L2.[31]
MSCs have an effect on macrophages, neutrophils, NK cells, mast cells and dendritic cells in innate immunity. MSCs are able to migrate to the site of injury, where they polarize through PGE2 macrophages in M2 phenotype which is characterized by an anti-inflammatory effect.[32] Further, PGE2 inhibits the ability of mast cells to degranulate and produce TNF-α.[33][34] Proliferation and cytotoxic activity of NK cells is inhibited by PGE2 and IDO. MSCs also reduce the expression of NK cell receptors - NKG2D, NKp44 and NKp30.[35] MSCs inhibit respiratory flare and apoptosis of neutrophils by production of cytokines IL-6 and IL-8.[36] Differentiation and expression of dendritic cell surface markers is inhibited by IL-6 and PGE2 of MSCs.[37] The immunosuppressive effects of MSC also depend on IL-10, but it is not certain whether they produce it alone, or only stimulate other cells to produce it.[38]
Bone marrow MSCs are capable to produce IL-7 and IL-15 and have been shown to promote early NK cell differentiation as well as long-term cytotoxic memory CD8 T cell survival.[39] MSC expresses the adhesion molecules VCAM-1 and ICAM-1, which allow T-lymphocytes to adhere to their surface. Then MSC can affect them by molecules which have a short half-life and their effect is in the immediate vicinity of the cell.[29] These include nitric oxide,[40] PGE2, HGF,[41] and activation of receptor PD-1.[42] MSCs reduce T cell proliferation between G0 and G1 cell cycle phases[43] and decrease the expression of IFNγ of Th1 cells while increasing the expression of IL-4 of Th2 cells.[44] MSCs also inhibit the proliferation of B-lymphocytes between G0 and G1 cell cycle phases.[42][45]
Antimicrobial properties
MSCs produce several antimicrobial peptides (AMPs), including human cathelicidin LL-37,[46] β-defensins,[47] lipocalin 2[48] and hepcidin.[49] These peptides, together with the enzyme indoleamine 2,3-dioxygenase (IDO), are responsible for the broad-spectrum antibacterial activity of MSCs.[50]
Clinical significance

Mesenchymal stem cells can be activated and mobilized in reaction to injury and infection. As of May 2024, a search for "mesenchymal stem cells" or "mesenchymal stromal cells" at ClinicalTrials.gov returns more than 1,760 studies featuring MSCs[51] for more than 920 conditions.
Autoimmune disease
Clinical studies investigating the efficacy of mesenchymal stem cells in treating diseases are in clinical development around the world, particularly treating autoimmune diseases, graft versus host disease, Crohn's disease, multiple sclerosis, systemic lupus erythematosus and systemic sclerosis.[52][53]
Other diseases
Many of the early clinical successes using intravenous transplantation came in systemic diseases such as graft versus host disease and sepsis. Direct injection or placement of cells into a site in need of repair may be the preferred method of treatment, as vascular delivery suffers from a "pulmonary first pass effect" where intravenous injected cells are sequestered in the lungs.[54]
Further studies into the mechanisms of MSC action may provide avenues for increasing their capacity for tissue repair.[55][56]
Research
Laboratory research techniques use colony-forming unit-fibroblasts where raw unpurified bone marrow or purified bone marrow mononuclear cells are applied directly into plastic cell culture plates or flasks within two days.[57]
Researchers have successfully isolated and expanded MSCs from marrow samples, demonstrating their ability to differentiate into specific cell lineages under controlled laboratory conditions. Environmental factors like nutrients, spatial organization, and signaling molecules influence MSC behavior and differentiation.[57]
Researchers developed a nanoparticle system to help MSCs support bone regeneration more effectively by delivering a protective gene (Nrf2) and a steroid (dexamethasone).[58]
Other flow cytometry-based methods allow the sorting of bone marrow cells for specific surface markers, such as STRO-1.[59] STRO-1+ cells are generally more homogenous and have higher rates of adherence and higher rates of proliferation, but the exact differences between STRO-1+ cells and MSCs are not clear.[60]
The supplementation of basal media with fetal bovine serum or human platelet lysate is common in MSC culture. Prior to the use of platelet lysates for MSC culture, the pathogen inactivation process may inhibit pathogen transmission.[61] Various chemicals and methods, including low-level laser irradiation, have been used to increase stem cell proliferation.[62]
MSC exosomes are tested as a potential treatment for intravascular coagulation due to their possible anti-inflammatory and anticoagulant properties.[63]
History
Scientists Ernest A. McCulloch and James E. Till first revealed the clonal nature of marrow cells in the 1960s.[64][65] In 1970, Arnold Caplan identified certain conditions by which mesodermal cells differentiate into cartilage or myogenic (muscle) tissue and bone and named them mesenchymal stem cells.[4]
An ex vivo assay for examining the clonogenic potential of multipotent marrow cells was later reported in the 1970s by Friedenstein and colleagues.[66][67] In this assay system, stromal cells were referred to as colony-forming unit-fibroblasts (CFU-f).
The first clinical trials of MSCs were completed by Osiris Therapeutics, a pharmaceutical company co-founded in 1995 by Caplan, with entrepreneur Kevin Kimberlin and others,[68] when a group of 15 patients were injected with cultured MSCs to test the safety of the treatment.[69] The first regulatory approvals for MSCs were granted conditional approval in 2012 in Canada and New Zealand for treating Graft vs. Host Disease (GvHD) and, subsequently, in Japan to treat Crohn's Disease-related fistula.[70] MSC therapy was approved by the FDA in the United States of America in 2024 for Graft vs. Host Disease (GvHD).[71]
Since then, more than 1,500 clinical trials have been conducted to treat numerous conditions.[72]
Controversies
The term "mesenchymal stem cells" has been debated for years and remains controversial, despite its widespread adoption in scientific literature. It has been argued that "mesenchymal stem cells" or "MSCs" are not 'mesenchymal in origin' nor are they bonafide 'stem cells.' [73] Most mesenchymal cell or "MSC" preps only contain a minority fraction of true multipotent stem cells, with most cells being stromal in nature, and it has been proposed that the term should be renamed to 'mesenchymal stromal cells'.[74] Caplan proposed rephrasing MSCs to emphasize their role as "medicinal signaling cells."[75] Within the stem cell field, the shorthand "MSC" most commonly refers to "mesenchymal stromal/stem cells" because of the heterogeneous nature of the cellular preparations.[76]
The study of MSCs has been vastly done via a 'translation in reverse' strategy, prioritizing clinical applications before understanding the fundamental physiology and mechanisms that underlie the MSCs ability to differentiate into various tissues and modulate local cell activity. [77] This has led to the marketing and application of unregulated and unsafe mesenchymal stem cell therapies in for-profit clinics[78][79], leading to adverse outcomes for unsuspecting patients.[80] However, the overall benefit of mesenchymal stem cell therapies in regulated global clinical trials remains to be determined, and must be evaluated a case by case basis. For example, mesenchymal stem cell therapies have shown success in treating Graft vs. Host Disease (GvHD)[81].
See also
- Bone marrow
- Fibroblast
- Muse cell
- Intramembranous ossification
- Mesenchyme
- Multipotency
- Cord lining
- Bone marrow adipose tissue
- List of human cell types derived from the germ layers
References
- ↑ "Mesenchymal Stem Cells" (in en). Essential Current Concepts in Stem Cell Biology. Learning Materials in Biosciences. Cham: Springer International Publishing. 2020. pp. 21–39. doi:10.1007/978-3-030-33923-4_2. ISBN 978-3-030-33923-4.
- ↑ "Mesenchymal stem cells: immune evasive, not immune privileged". Nature Biotechnology 32 (3): 252–60. March 2014. doi:10.1038/nbt.2816. PMID 24561556.
- ↑ "Stem Cells Applications in Regenerative Medicine and Disease Therapeutics". International Journal of Cell Biology 2016. 2016. doi:10.1155/2016/6940283. PMID 27516776.
- ↑ 4.0 4.1 "Mesenchymal Stem Cells: Time to Change the Name!". Stem Cells Translational Medicine 6 (6): 1445–1451. June 2017. doi:10.1002/sctm.17-0051. PMID 28452204.
- ↑ "Mesenchymal Stem Cells: Characteristics, Function, and Application". Stem Cells Int 2019. 2019. doi:10.1155/2019/8106818. PMID 30956675.
- ↑ "Mesenchymal stem cells: revisiting history, concepts, and assays". Cell Stem Cell 2 (4): 313–319. April 2008. doi:10.1016/j.stem.2008.03.002. PMID 18397751.
- ↑ Dominici, M.; Le Blanc, K.; Mueller, I.; Slaper-Cortenbach, I.; Marini, F.C; Krause, D.S.; Deans, R.J.; Keating, A. et al. (2006). "Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement" (in en). Cytotherapy 8 (4): 315–317. doi:10.1080/14653240600855905. https://linkinghub.elsevier.com/retrieve/pii/S1465324906708817.
- ↑ "Regenerative medicine: a review". Revista Brasileira de Hematologia e Hemoterapia 31 (Suppl. 2). 2009. doi:10.1590/S1516-84842009000800017.
- ↑ "Eccentric exercise facilitates mesenchymal stem cell appearance in skeletal muscle". PLOS ONE 7 (1). 2012. doi:10.1371/journal.pone.0029760. PMID 22253772. Bibcode: 2012PLoSO...729760V.
- ↑ "Clinical applications of mesenchymal stem cells". Journal of Hematology & Oncology 5. April 2012. doi:10.1186/1756-8722-5-19. PMID 22546280.
- ↑ "Mesenchymal stem cells in the human corneal limbal stroma". Investigative Ophthalmology & Visual Science 53 (9): 5109–16. August 2012. doi:10.1167/iovs.11-8673. PMID 22736610.
- ↑ 12.0 12.1 "Concise Reviews: Characteristics and Potential Applications of Human Dental Tissue-Derived Mesenchymal Stem Cells". Stem Cells 33 (3): 627–38. March 2015. doi:10.1002/stem.1909. PMID 25447379.
- ↑ "A perivascular origin for mesenchymal stem cells in multiple human organs". Cell Stem Cell 3 (3): 301–13. September 2008. doi:10.1016/j.stem.2008.07.003. PMID 18786417.
- ↑ Musculoskeletal system: anatomy, physiology, and metabolic disorders. Summit, New Jersey: Ciba-Geigy Corporation. 1987. p. 134. ISBN 978-0-914168-88-1.
- ↑ "Early histological and ultrastructural changes in medullary fracture callus". The Journal of Bone and Joint Surgery. American Volume 73 (6): 832–847. July 1991. doi:10.2106/00004623-199173060-00006. PMID 2071617.
- ↑ "Mesenchymal stromal cells and fibroblasts: a case of mistaken identity?". Cytotherapy 14 (5): 516–21. May 2012. doi:10.3109/14653249.2012.677822. PMID 22458957. https://www.sciencedirect.com/science/article/abs/pii/S1465324912706643.
- ↑ "Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement". Cytotherapy 8 (4): 315–7. 1 January 2006. doi:10.1080/14653240600855905. PMID 16923606. https://www2.dti.ufv.br/noticia/files/anexos/phpCDlYcY_5654.pdf.
- ↑ 18.0 18.1 "Same or Not the Same? Comparison of Adipose Tissue-Derived Versus Bone Marrow-Derived Mesenchymal Stem and Stromal Cells". Stem Cells and Development 21 (14): 2724–52. September 2012. doi:10.1089/scd.2011.0722. PMID 22468918.
- ↑ "Non-hematopoietic bone marrow stem cells: molecular control of expansion and differentiation". Experimental Cell Research. Molecular Control of Stem Cell Differentiation 306 (2): 330–5. June 2005. doi:10.1016/j.yexcr.2005.03.018. PMID 15925588.
- ↑ "Characteristics and Clinical Applications of Wharton's Jelly-Derived Mesenchymal Stromal Cells". Current Research in Translational Medicine 68 (1): 5–16. Jan 2020. doi:10.1016/j.retram.2019.09.001. PMID 31543433.
- ↑ "Adipose-derived stem cells: isolation, expansion and differentiation". Methods. Methods in stem cell research 45 (2): 115–20. June 2008. doi:10.1016/j.ymeth.2008.03.006. PMID 18593609.
- ↑ "What is Cord Tissue?". Americord Registry. CordAdvantage.com. 2018-10-30. http://cordadvantage.com/cord-tissue-banking.html.
- ↑ "β-Catenin Preserves the Stem State of Murine Bone Marrow Stromal Cells Through Activation of EZH2". Journal of Bone and Mineral Research 35 (6): 1149–1162. June 2020. doi:10.1002/jbmr.3975. PMID 32022326.
- ↑ "Differentiation of human adipose-derived adult stem cells into neuronal tissue: does it work?". Differentiation; Research in Biological Diversity 77 (3): 221–8. March 2009. doi:10.1016/j.diff.2008.10.016. PMID 19272520.
- ↑ "Matrix elasticity directs stem cell lineage specification". Cell 126 (4): 677–89. August 2006. doi:10.1016/j.cell.2006.06.044. PMID 16923388.
- ↑ "Donor age negatively impacts adipose tissue-derived mesenchymal stem cell expansion and differentiation". Journal of Translational Medicine 12 (1). January 2014. doi:10.1186/1479-5876-12-8. PMID 24397850.
- ↑ "Understanding the association of stem cells in fetal development and carcinogenesis during pregnancy" (in en). Advances in Cancer Biology - Metastasis 4. July 2022. doi:10.1016/j.adcanc.2022.100042. ISSN 2667-3940.
- ↑ "MSCs inhibit monocyte-derived DC maturation and function by selectively interfering with the generation of immature DCs: central role of MSC-derived prostaglandin E2". Blood 113 (26): 6576–6583. June 2009. doi:10.1182/blood-2009-02-203943. PMID 19398717.
- ↑ 29.0 29.1 "Inflammatory cytokine-induced intercellular adhesion molecule-1 and vascular cell adhesion molecule-1 in mesenchymal stem cells are critical for immunosuppression". Journal of Immunology 184 (5): 2321–2328. March 2010. doi:10.4049/jimmunol.0902023. PMID 20130212.
- ↑ "Mesenchymal-stem-cell-induced immunoregulation involves FAS-ligand-/FAS-mediated T cell apoptosis". Cell Stem Cell 10 (5): 544–555. May 2012. doi:10.1016/j.stem.2012.03.007. PMID 22542159.
- ↑ "Mesenchymal Stromal Cell Secretion of Programmed Death-1 Ligands Regulates T Cell Mediated Immunosuppression". Stem Cells 35 (3): 766–776. March 2017. doi:10.1002/stem.2509. PMID 27671847.
- ↑ "Mesenchymal stem cell-educated macrophages: a novel type of alternatively activated macrophages". Experimental Hematology 37 (12): 1445–53. December 2009. doi:10.1016/j.exphem.2009.09.004. PMID 19772890.
- ↑ "Bone marrow stromal cells inhibit mast cell function via a COX2-dependent mechanism". Clinical and Experimental Allergy 41 (4): 526–34. April 2011. doi:10.1111/j.1365-2222.2010.03685.x. PMID 21255158.
- ↑ "Prostaglandin E2 activates EP2 receptors to inhibit human lung mast cell degranulation". British Journal of Pharmacology 147 (7): 707–13. April 2006. doi:10.1038/sj.bjp.0706664. PMID 16432506.
- ↑ "Mesenchymal stem cell-natural killer cell interactions: evidence that activated NK cells are capable of killing MSCs, whereas MSCs can inhibit IL-2-induced NK-cell proliferation". Blood 107 (4): 1484–90. February 2006. doi:10.1182/blood-2005-07-2775. PMID 16239427.
- ↑ "Human mesenchymal stem cells inhibit neutrophil apoptosis: a model for neutrophil preservation in the bone marrow niche". Stem Cells 26 (1): 151–62. January 2008. doi:10.1634/stemcells.2007-0416. PMID 17932421.
- ↑ "Human mesenchymal stem cells inhibit differentiation and function of monocyte-derived dendritic cells". Blood 105 (10): 4120–6. May 2005. doi:10.1182/blood-2004-02-0586. PMID 15692068.
- ↑ "Immunobiology of mesenchymal stem cells". Cell Death and Differentiation 21 (2): 216–25. February 2014. doi:10.1038/cdd.2013.158. PMID 24185619.
- ↑ Stecher, Carmen; Bischl, Romana; Schmid-Böse, Anna; Ferstl, Stefanie; Potzmann, Elisabeth; Frank, Magdalena; Braun, Nina; Farlik, Matthias et al. (2025-07-01). "Heterogeneity of IL-15-expressing mesenchymal stromal cells controls natural killer cell development and immune cell homeostasis" (in en). Nature Communications 16 (1): 5949. doi:10.1038/s41467-025-61231-0. ISSN 2041-1723. PMID 40595636. Bibcode: 2025NatCo..16.5949S.
- ↑ "Mesenchymal stem cell-mediated immunosuppression occurs via concerted action of chemokines and nitric oxide". Cell Stem Cell 2 (2): 141–50. February 2008. doi:10.1016/j.stem.2007.11.014. PMID 18371435.
- ↑ "Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli". Blood 99 (10): 3838–43. May 2002. doi:10.1182/blood.v99.10.3838. PMID 11986244.
- ↑ 42.0 42.1 "Bone marrow mesenchymal progenitor cells inhibit lymphocyte proliferation by activation of the programmed death 1 pathway". European Journal of Immunology 35 (5): 1482–90. May 2005. doi:10.1002/eji.200425405. PMID 15827960.
- ↑ "Bone marrow mesenchymal stem cells induce division arrest anergy of activated T cells". Blood 105 (7): 2821–7. April 2005. doi:10.1182/blood-2004-09-3696. PMID 15591115.
- ↑ "Human mesenchymal stem cells modulate allogeneic immune cell responses". Blood 105 (4): 1815–22. February 2005. doi:10.1182/blood-2004-04-1559. PMID 15494428.
- ↑ "Human mesenchymal stem cells modulate B-cell functions". Blood 107 (1): 367–72. January 2006. doi:10.1182/blood-2005-07-2657. PMID 16141348.
- ↑ "Antibacterial effect of human mesenchymal stem cells is mediated in part from secretion of the antimicrobial peptide LL-37". Stem Cells 28 (12): 2229–38. December 2010. doi:10.1002/stem.544. PMID 20945332.
- ↑ "Antibacterial effect of mesenchymal stem cells against Escherichia coli is mediated by secretion of beta- defensin- 2 via toll- like receptor 4 signalling". Cellular Microbiology 18 (3): 424–36. March 2016. doi:10.1111/cmi.12522. PMID 26350435.
- ↑ "Mesenchymal stem cells enhance survival and bacterial clearance in murine Escherichia coli pneumonia". Thorax 67 (6): 533–9. June 2012. doi:10.1136/thoraxjnl-2011-201176. PMID 22250097.
- ↑ "Combination therapy of menstrual derived mesenchymal stem cells and antibiotics ameliorates survival in sepsis". Stem Cell Research & Therapy 6. October 2015. doi:10.1186/s13287-015-0192-0. PMID 26474552.
- ↑ "Human but not murine multipotent mesenchymal stromal cells exhibit broad-spectrum antimicrobial effector function mediated by indoleamine 2,3-dioxygenase". Leukemia 25 (4): 648–54. April 2011. doi:10.1038/leu.2010.310. PMID 21242993.
- ↑ "Search of: Mesenchymal stem cells - List Results - ClinicalTrials.gov" (in en). https://clinicaltrials.gov/ct2/results?cond=&term=Mesenchymal+stem+cells&cntry=&state=&city=&dist=.
- ↑ "Mesenchymal stem cell treatment for autoimmune diseases: a critical review". Biological Research 45 (3): 269–77. 2012. doi:10.4067/S0716-97602012000300008. PMID 23283436.
- ↑ "Mesenchymal stem or stromal cells: a review of clinical applications and manufacturing practices". Transfusion 54 (5): 1418–37. May 2014. doi:10.1111/trf.12421. PMID 24898458.
- ↑ "Pulmonary passage is a major obstacle for intravenous stem cell delivery: the pulmonary first-pass effect". Stem Cells and Development 18 (5): 683–92. June 2009. doi:10.1089/scd.2008.0253. PMID 19099374.
- ↑ "Mesenchymal Stem Cells; Defining the Future of Regenerative Medicine". Journal of Genes and Cells 1 (2): 34–39. 2015. doi:10.15562/gnc.15.
- ↑ "Comprehensive Proteomic Analysis of Mesenchymal Stem Cell Exosomes Reveals Modulation of Angiogenesis via Nuclear Factor-KappaB Signaling". Stem Cells 34 (3): 601–13. March 2016. doi:10.1002/stem.2298. PMID 26782178.
- ↑ 57.0 57.1 Pittenger, Mark F.; Mackay, Alastair M.; Beck, Stephen C. et al. (1999-04-02). "Multilineage Potential of Adult Human Mesenchymal Stem Cells". Science 284 (5411): 143–147. doi:10.1126/science.284.5411.143. ISSN 0036-8075. PMID 10102814. Bibcode: 1999Sci...284..143P.
- ↑ Park, Ji Sun; Jeon, Hayoung; Lee, Yeeun et al. (2024-11-19). "Rapid DNA Repair in Mesenchymal Stem Cells and Bone Regeneration by Nanoparticle-Based Codelivery of Nrf2-mRNA and Dexamethasone". ACS Nano 18 (46): 31877–31890. doi:10.1021/acsnano.4c08939. ISSN 1936-0851. PMID 39520360. Bibcode: 2024ACSNa..1831877P.
- ↑ "The STRO-1+ fraction of adult human bone marrow contains the osteogenic precursors". Blood 84 (12): 4164–73. December 1994. doi:10.1182/blood.V84.12.4164.bloodjournal84124164. PMID 7994030. http://www.bloodjournal.org/cgi/pmidlookup?view=long&pmid=7994030.
- ↑ "Isolation and characterization of human clonogenic osteoblast progenitors immunoselected from fetal bone marrow stroma using STRO-1 monoclonal antibody". Journal of Bone and Mineral Research 14 (3): 351–61. March 1999. doi:10.1359/jbmr.1999.14.3.351. PMID 10027900.
- ↑ "Pathogen-free, plasma-poor platelet lysate and expansion of human mesenchymal stem cells". Journal of Translational Medicine 12. January 2014. doi:10.1186/1479-5876-12-28. PMID 24467837.
- ↑ "Effect of low-level laser irradiation on proliferation of human dental mesenchymal stem cells; a systemic review". Journal of Photochemistry and Photobiology B: Biology 162: 577–582. September 2016. doi:10.1016/j.jphotobiol.2016.07.022. PMID 27475781. Bibcode: 2016JPPB..162..577B.
- ↑ Wang, Chengran; Zhao, Xiaoqing; Wang, Keyan et al. (2024). "Prospective Application of Mesenchymal Stem Cell-Derived Exosomes in the Treatment of Disseminated Intravascular Coagulation". International Journal of Nanomedicine 19: 11957–11971. doi:10.2147/ijn.s467158. ISSN 1178-2013. PMID 39569063.
- ↑ "Cytological demonstration of the clonal nature of spleen colonies derived from transplanted mouse marrow cells". Nature 197 (4866): 452–4. February 1963. doi:10.1038/197452a0. PMID 13970094. Bibcode: 1963Natur.197..452B.
- ↑ "The distribution of colony-forming cells among spleen colonies". Journal of Cellular and Comparative Physiology 62 (3): 327–36. December 1963. doi:10.1002/jcp.1030620313. PMID 14086156.
- ↑ "Precursors for fibroblasts in different populations of hematopoietic cells as detected by the in vitro colony assay method". Experimental Hematology 2 (2): 83–92. 1974. PMID 4455512.
- ↑ "Fibroblast precursors in normal and irradiated mouse hematopoietic organs". Experimental Hematology 4 (5): 267–74. September 1976. PMID 976387.
- ↑ Bell, Julie (September 26, 2002). "New CEO at Osiris toiling as clock ticks". The Baltimore Sun. p. C1. https://www.newspapers.com/article/the-baltimore-sun-new-osiris-ceo-part-1/107612420/.
- ↑ "Ex vivo expansion and subsequent infusion of human bone marrow-derived stromal progenitor cells (mesenchymal progenitor cells): implications for therapeutic use". Bone Marrow Transplantation 16 (4): 557–564. October 1995. PMID 8528172.
- ↑ "Mesenchymal Stromal Cells: Clinical Challenges and Therapeutic Opportunities". Cell Stem Cell 22 (6): 824–833. June 2018. doi:10.1016/j.stem.2018.05.004. PMID 29859173.
- ↑ "FDA Approves First Mesenchymal Stromal Cell Therapy to Treat Steroid-refractory Acute Graft-versus-host Disease" (in en). 2024-12-18. https://www.fda.gov/news-events/press-announcements/fda-approves-first-mesenchymal-stromal-cell-therapy-treat-steroid-refractory-acute-graft-versus-host.
- ↑ "Human bone marrow-derived mesenchymal (stromal) progenitor cells (MPCs) cannot be recovered from peripheral blood progenitor cell collections". Journal of Hematotherapy 6 (5): 447–455. October 1997. doi:10.1089/scd.1.1997.6.447. PMID 9368181.
- ↑ Bianco, Paolo (2014-10-11). "“Mesenchymal” Stem Cells" (in en). Annual Review of Cell and Developmental Biology 30 (1): 677–704. doi:10.1146/annurev-cellbio-100913-013132. ISSN 1081-0706. https://www.annualreviews.org/doi/10.1146/annurev-cellbio-100913-013132.
- ↑ Dominici, Massimo; Paolucci, Paolo; Conte, Pierfranco; Horwitz, Edwin M. (2009-05-15). "Heterogeneity of Multipotent Mesenchymal Stromal Cells: From Stromal Cells to Stem Cells and Vice Versa" (in en). Transplantation 87 (9S): S36–S42. doi:10.1097/TP.0b013e3181a283ee. ISSN 0041-1337. https://journals.lww.com/00007890-200905151-00003.
- ↑ "Medicinal signalling cells: they work, so use them". Nature 566 (7742): 39. February 2019. doi:10.1038/d41586-019-00490-6. PMID 30723355. Bibcode: 2019Natur.566R..39C.
- ↑ Bianco, Paolo (2014-10-06). ""Mesenchymal" Stem Cells" (in en). Annual Review of Cell and Developmental Biology 30: 677–704. doi:10.1146/annurev-cellbio-100913-013132. ISSN 1081-0706. https://www.annualreviews.org/content/journals/10.1146/annurev-cellbio-100913-013132.
- ↑ Bianco, Paolo (July 2013). "Don’t market stem-cell products ahead of proof" (in en). Nature 499 (7458): 255–255. doi:10.1038/499255a. ISSN 1476-4687. https://www.nature.com/articles/499255a.
- ↑ "Lawmaker Promoted Stem Cell Therapy for Covid-19 in Fraud Scheme, U.S. Says" (in en-US). The New York Times. 2021-02-04. ISSN 0362-4331. https://www.nytimes.com/2021/02/03/us/Tricia-Derges-fake-stem-cell-cure-covid.html.
- ↑ Office of the Commissioner (2020-09-09). "FDA Warns About Stem Cell Therapies" (in en). U.S. Food and Drug Administration. https://www.fda.gov/consumers/consumer-updates/fda-warns-about-stem-cell-therapies.
- ↑ "Harms Linked to Unapproved Stem Cell Interventions Highlight Need for Greater FDA Enforcement" (in en). https://pew.org/3fKASu5.
- ↑ Commissioner, Office of the (2024-12-18). "FDA Approves First Mesenchymal Stromal Cell Therapy to Treat Steroid-refractory Acute Graft-versus-host Disease" (in en). https://www.fda.gov/news-events/press-announcements/fda-approves-first-mesenchymal-stromal-cell-therapy-treat-steroid-refractory-acute-graft-versus-host.
Further reading
- "Mesenchymal stem cells: environmentally responsive therapeutics for regenerative medicine". Experimental & Molecular Medicine 45 (11): e54. November 2013. doi:10.1038/emm.2013.94. PMID 24232253.
External links
- "Mesenchymal stem cells fact sheet". Euro Stem Cell. June 2012. http://www.eurostemcell.org/factsheet/mesenchymal-stem-cells-other-bone-marrow-stem-cells. scientist-reviewed and not too technical
- McMacken, Melissa. "Mesenchymal Stem Cell Research". Johns Hopkins University. http://www.hopkinsmedicine.org/stem_cell_research/cell_identity.
 |
