Biology:Collagen
Collagen (/ˈkɒlədʒən/) is the main structural protein in the extracellular matrix of the connective tissues of many animals. It is the most abundant protein in mammals,[1] making up 25% to 35% of protein content. Amino acids are bound together to form a triple helix of elongated fibril[2] known as a collagen helix. It is mostly found in cartilage, bones, tendons, ligaments, and skin. Vitamin C is vital for collagen synthesis.
Depending on the degree of mineralization, collagen tissues may be rigid (bone) or compliant (tendon) or have a gradient from rigid to compliant (cartilage). Collagen is also abundant in corneas, blood vessels, the gut, intervertebral discs, and dentin.[3] In muscle tissue, it serves as a major component of the endomysium. Collagen constitutes 1% to 2% of muscle tissue and 6% by weight of skeletal muscle.[4] The fibroblast is the most common cell creating collagen in animals. Gelatin, which is used in food and industry, is collagen that was irreversibly hydrolyzed using heat, basic solutions, or weak acids.[5]
Etymology
The word collagen comes from Greek κόλλα, kólla 'glue' and the suffix -γέν, -gen 'producing'.[6][7]
Types
As of 2011, 28 types of human collagen have been identified, described, and classified according to their structure.[8] This diversity shows collagen's diverse functionality.[9] All of the types contain at least one triple helix.[8] Over 90% of the collagen in humans is Type I and Type III collagen.[10]
- Fibrillar (type I, II, III, V, XI)
- Non-fibrillar
- FACIT (fibril-associated collagens with interrupted triple helices) (types IX, XII, XIV, XVI, XIX, XXI)
- Short-chain (types VIII, X)
- Basement membrane (type IV)
- Multiplexin (multiple triple helix domains with interruptions) (types XV, XVIII)
- MACIT (membrane-associated collagens with interrupted triple helices) (types XIII, XVII)
- Microfibril-forming (type VI)
- Anchoring fibrils (type VII)
The five most common types are:[11]
- Type I: skin, tendon, vasculature, organs, bone (main component of the organic part of bone)
- Type II: cartilage (main collagenous component of cartilage)
- Type III: reticulate (main component of reticular fibers), commonly found alongside type I
- Type IV: forms basal lamina, the epithelium-secreted layer of the basement membrane
- Type V: cell surfaces, hair, and placenta
In humans
Cardiac
Bone grafts
As the skeleton forms the structure of the body, it is vital that it maintains its strength and its structure, even after breaks and injuries. Collagen is used in bone grafting because its triple-helix structure makes it a very strong molecule. It is ideal for use in bones, as it does not compromise the structural integrity of the skeleton. The triple helical structure prevents collagen from being broken down by enzymes, it enables adhesiveness of cells, and it is important for the proper assembly of the extracellular matrix.[12]
Tissue regeneration
Collagen scaffolds are used in tissue regeneration, whether in sponges,[13] thin sheets,[14] gels,[15] or fibers.[16] Collagen has favorable properties for tissue regeneration, such as pore structure, permeability, hydrophilicity, and stability in vivo. Collagen scaffolds also support deposition of cells, such as osteoblasts and fibroblasts, and once inserted, facilitate growth to proceed normally.[17]
Reconstructive surgery
Collagens are widely used in the construction of artificial skin substitutes used for managing severe burns and wounds.[18][19] These collagens may be derived from cow, horse, pig, or even human sources; and are sometimes used in combination with silicones, glycosaminoglycans, fibroblasts, growth factors, and other substances.[20]
Wound healing
Collagen is one of the body's key natural resources and a component of skin tissue that can benefit all stages of wound healing.[21] When collagen is made available to the wound bed, closure can occur. This avoids wound deterioration and procedures such as amputation.
Collagen is used as a natural wound dressing because it has properties that artificial wound dressings do not have. It resists bacteria, which is vitally important in wound dressing. As a burn dressing, collagen helps it heal fast by helping granulation tissue to grow over the burn.[18]
Throughout the four phases of wound healing, collagen performs the following functions:
- Guiding: collagen fibers guide fibroblasts because they migrate along a connective tissue matrix.
- Chemotaxis: collagen fibers have a large surface area which attracts fibrogenic cells which help healing.
- Nucleation: in the presence of certain neutral salt molecules, collagen can act as a nucleating agent causing formation of fibrillar structures.
- Hemostasis: Blood platelets interact with the collagen to make a hemostatic plug.
Use in basic research
Collagen is used in laboratory studies for cell culture, studying cell behavior and cellular interactions with the extracellular environment.[22] Collagen is also widely used as a bioink for 3D bioprinting and biofabrication of 3D tissue models.
Biology
The collagen protein is composed of a triple helix, which generally consists of two identical chains (α1) and an additional chain that differs slightly in its chemical composition (α2).[23] The amino acid composition of collagen is atypical for proteins, particularly with respect to its high hydroxyproline content. The most common motifs in collagen's amino acid sequence are glycine-proline-X and glycine-X-hydroxyproline, where X is any amino acid other than glycine, proline or hydroxyproline.
The table below lists average amino acid composition for fish and mammal skin.[24]
| Amino acid | Abundance in mammal skin (residues/1000) |
Abundance in fish skin (residues/1000) |
|---|---|---|
| Glycine | 329 | 339 |
| Proline | 126 | 108 |
| Alanine | 109 | 114 |
| Hydroxyproline | 95 | 67 |
| Glutamic acid | 74 | 76 |
| Arginine | 49 | 52 |
| Aspartic acid | 47 | 47 |
| Serine | 36 | 46 |
| Lysine | 29 | 26 |
| Leucine | 24 | 23 |
| Valine | 22 | 21 |
| Threonine | 19 | 26 |
| Phenylalanine | 13 | 14 |
| Isoleucine | 11 | 11 |
| Hydroxylysine | 6 | 8 |
| Methionine | 6 | 13 |
| Histidine | 5 | 7 |
| Tyrosine | 3 | 3 |
| Cysteine | 1 | 1 |
| Tryptophan | 0 | 0 |
Synthesis
First, a three-dimensional stranded structure is assembled, mostly composed of the amino acids glycine and proline. This is the collagen precursor procollagen. Then, procollagen is modified by the addition of hydroxyl groups to the amino acids proline and lysine. This step is important for later glycosylation and the formation of collagen's triple helix structure. Because the hydroxylase enzymes performing these reactions require vitamin C as a cofactor, a long-term deficiency in this vitamin results in impaired collagen synthesis and scurvy.[25] These hydroxylation reactions are catalyzed by the enzymes prolyl 4-hydroxylase[26] and lysyl hydroxylase. The reaction consumes one ascorbate molecule per hydroxylation.[27] Collagen synthesis occurs inside and outside cells.
The most common form of collagen is fibrillary collagen. Another common form is meshwork collagen, which is often involved in the formation of filtration systems. All types of collagen are triple helices, but differ in the make-up of their alpha peptides created in step 2. Below we discuss the formation of fibrillary collagen.
- Transcription of mRNA: Synthesis begins with turning on genes associated with the formation of a particular alpha peptide (typically alpha 1, 2 or 3). About 44 genes are associated with collagen formation, each coding for a specific mRNA sequence, and are typically named with the "COL" prefix.
- Pre-pro-peptide formation: The created mRNA exits the cell nucleus into the cytoplasm. There, it links with the ribosomal subunits and is translated into a peptide. The peptide goes into the endoplasmic reticulum for post-translational processing. It is directed there by a signal recognition particle on the endoplasmic reticulum, which recognizes the peptide's N-terminal signal sequence (the early part of the sequence). The processed product is a pre-pro-peptide called preprocollagen.
- Pro-collagen formation: Three modifications of the pre-pro-peptide form the alpha peptide:
- The signal peptide on the N-terminal is removed. This molecule is called 'propeptide.'
- Lysines and prolines are hydroxylated by the enzymes 'prolyl hydroxylase' and 'lysyl hydroxylase', producing hydroxyproline and hydroxylysine. This helps in cross-linking the alpha peptides. This enzymatic step requires vitamin C as a cofactor. In scurvy, the lack of hydroxylation of prolines and lysines causes a looser triple helix (which is formed by three alpha peptides).
- Glycosylation occurs by adding either glucose or galactose monomers onto the hydroxyl groups that were placed onto lysines, but not on prolines.
- Three of the hydroxylated and glycosylated propeptides twist into a triple helix (except for its ends), forming procollagen. It is packaged into a transfer vesicle destined for the Golgi apparatus.
- Modification and secretion: In the Golgi apparatus, the procollagen goes through one last post-translational modification, adding oligosaccharides (not monosaccharides as in step 3). Then it is packaged into a secretory vesicle to be secreted from the cell.
- Tropocollagen formation: Outside the cell, membrane-bound enzymes called collagen peptidases remove the unwound ends of the molecule, producing tropocollagen. Defects in this step produce various collagenopathies called Ehlers–Danlos syndrome. This step is absent when synthesizing type III, a type of fibrillar collagen.
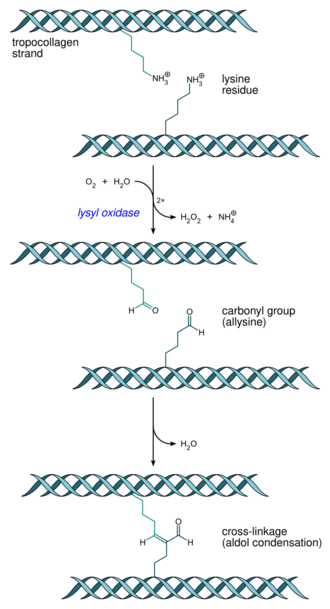
- Collagen fibril formation: Lysyl oxidase, a copper-dependent enzyme, acts on lysines and hydroxylysines, producing aldehyde groups, which eventually form covalent bonds between tropocollagen molecules. This polymer of tropocollagen is called a collagen fibril.
Amino acids
Collagen has an unusual amino acid composition and sequence:
- Glycine is found at almost every third residue.
- Proline makes up about 17% of collagen.
- Collagen contains two unusual derivative amino acids not directly inserted during translation. These amino acids are found at specific locations relative to glycine and are modified post-translationally by different enzymes, both of which require vitamin C as a cofactor.
- Hydroxyproline derived from proline
- Hydroxylysine derived from lysine – depending on the type of collagen, varying numbers of hydroxylysines are glycosylated (mostly having disaccharides attached).
Cortisol stimulates degradation of (skin) collagen into amino acids.[28]
Collagen I formation
Most collagen forms in a similar manner, but the following process is typical for type I:
- Inside the cell
- Two types of alpha chains – alpha-1 and alpha 2, are formed during translation on ribosomes along the rough endoplasmic reticulum (RER). These peptide chains, known as preprocollagen, have registration peptides on each end and a signal peptide.[29]
- Polypeptide chains are released into the lumen of the RER.
- Signal peptides are cleaved inside the RER; these are known as pro-alpha chains.
- Hydroxylation of lysine and proline amino acids occurs inside the lumen. This process is dependent on and consumes ascorbic acid (vitamin C) as a cofactor.
- Glycosylation of specific hydroxylysine residues occurs.
- Triple alpha helical structure is formed inside the endoplasmic reticulum from two alpha-1 chains and one alpha-2 chain.
- Procollagen is shipped to the Golgi apparatus, where it is packaged and secreted into the extracellular space by exocytosis.
- Outside the cell
- Registration peptides are cleaved, and tropocollagen is formed by procollagen peptidase.
- Multiple tropocollagen molecules form collagen fibrils, via covalent cross-linking (aldol reaction) by lysyl oxidase which links hydroxylysine and lysine residues. Multiple collagen fibrils form into collagen fibers.
- Collagen may be attached to cell membranes via several types of protein, including fibronectin, laminin, fibulin, and integrin.
Molecular structure
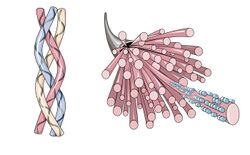
A single collagen molecule, tropocollagen, is used to make up larger collagen aggregates, such as fibrils. It is approximately 300 nm long and 1.5 nm in diameter, and it is made up of three polypeptide strands (called alpha peptides, see step 2), each of which has the conformation of a left-handed helix – this should not be confused with the right-handed alpha helix. These three left-handed helices are twisted together into a right-handed triple helix or "super helix", a cooperative quaternary structure stabilized by many hydrogen bonds. With type I collagen and possibly all fibrillar collagens, if not all collagens, each triple-helix associates into a right-handed super-super-coil referred to as the collagen microfibril. Each microfibril is interdigitated with its neighboring microfibrils to a degree that might suggest they are individually unstable, although within collagen fibrils, they are so well ordered as to be crystalline.
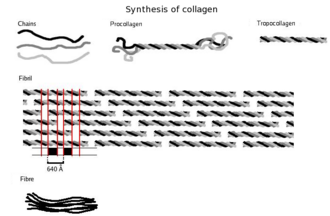
A distinctive feature of collagen is the regular arrangement of amino acids in each of the three chains of these collagen subunits. The sequence often follows the pattern Gly-Pro-X or Gly-X-Hyp, where X may be any of various other amino acid residues.[24] Proline or hydroxyproline constitute about 1/6 of the total sequence. With glycine accounting for the 1/3 of the sequence, this means approximately half of the collagen sequence is not glycine, proline or hydroxyproline, a fact often missed due to the distraction of the unusual GX1X2 character of collagen alpha-peptides. The high glycine content of collagen is important with respect to stabilization of the collagen helix, as this allows the very close association of the collagen fibers within the molecule, facilitating hydrogen bonding and the formation of intermolecular cross-links.[24] This kind of regular repetition and high glycine content is found in only a few other fibrous proteins, such as silk fibroin.
Collagen is not only a structural protein. Due to its key role in the determination of cell phenotype, cell adhesion, tissue regulation, and infrastructure, many sections of its non-proline-rich regions have cell or matrix association/regulation roles. The relatively high content of proline and hydroxyproline rings, with their geometrically constrained carboxyl and (secondary) amino groups, along with the rich abundance of glycine, accounts for the tendency of the individual polypeptide strands to form left-handed helices spontaneously, without any intrachain hydrogen bonding.
Because glycine is the smallest amino acid with no side chain, it plays a unique role in fibrous structural proteins. In collagen, Gly is required at every third position because the assembly of the triple helix puts this residue at the interior (axis) of the helix, where there is no space for a larger side group than glycine's single hydrogen atom. For the same reason, the rings of the Pro and Hyp must point outward. These two amino acids help stabilize the triple helix – Hyp even more so than Pro because of a stereoelectronic effect;[30] a lower concentration of them is required in animals such as fish, whose body temperatures are lower than most warm-blooded animals. Lower proline and hydroxyproline contents are characteristic of cold-water, but not warm-water fish; the latter tend to have similar proline and hydroxyproline contents to mammals.[24] The lower proline and hydroxyproline contents of cold-water fish and other poikilotherm animals lead to their collagen having a lower thermal stability than mammalian collagen.[24] This lower thermal stability means that gelatin derived from fish collagen is not suitable for many food and industrial applications.
The tropocollagen subunits spontaneously self-assemble, with regularly staggered ends, into even larger arrays in the extracellular spaces of tissues.[31][32] Additional assembly of fibrils is guided by fibroblasts, which deposit fully formed fibrils from fibripositors. In the fibrillar collagens, molecules are staggered to adjacent molecules by about 67 nm (a unit that is referred to as 'D' and changes depending upon the hydration state of the aggregate). In each D-period repeat of the microfibril, there is a part containing five molecules in cross-section, called the "overlap", and a part containing only four molecules, called the "gap".[33] These overlap and gap regions are retained as microfibrils assemble into fibrils, and are thus viewable using electron microscopy. The triple helical tropocollagens in the microfibrils are arranged in a quasihexagonal packing pattern.[33][34]

There is some covalent crosslinking within the triple helices and a variable amount of covalent crosslinking between tropocollagen helices forming well-organized aggregates (such as fibrils).[35] Larger fibrillar bundles are formed with the aid of several different classes of proteins (including different collagen types), glycoproteins, and proteoglycans to form the different types of mature tissues from alternate combinations of the same key players.[32] Collagen's insolubility was a barrier to the study of monomeric collagen until it was found that tropocollagen from young animals can be extracted because it is not yet fully crosslinked. However, advances in microscopy techniques (i.e. electron microscopy (EM) and atomic force microscopy (AFM)) and X-ray diffraction have enabled researchers to obtain increasingly detailed images of collagen structure in situ.[36] These later advances are particularly important to better understanding the way in which collagen structure affects cell–cell and cell–matrix communication and how tissues are constructed in growth and repair and changed in development and disease.[37][38] For example, using AFM–based nanoindentation it has been shown that a single collagen fibril is a heterogeneous material along its axial direction with significantly different mechanical properties in its gap and overlap regions, correlating with its different molecular organizations in these two regions.[39]
Collagen fibrils/aggregates are arranged in different combinations and concentrations in various tissues to provide varying tissue properties. In bone, entire collagen triple helices lie in a parallel, staggered array. 40 nm gaps between the ends of the tropocollagen subunits (approximately equal to the gap region) probably serve as nucleation sites for the deposition of long, hard, fine crystals of the mineral component, which is hydroxylapatite (approximately) Ca10(OH)2(PO4)6.[40] Type I collagen gives bone its tensile strength.
Associated disorders
Collagen-related diseases most commonly arise from genetic defects or nutritional deficiencies that affect the biosynthesis, assembly, posttranslational modification, secretion, or other processes involved in normal collagen production.
| Type | Notes | Gene(s) | Disorders |
| I | This is the most abundant collagen of the human body. It is present in scar tissue, the end product when tissue heals by repair. It is found in tendons, skin, artery walls, cornea, the endomysium surrounding muscle fibers, fibrocartilage, and the organic part of bones and teeth. | COL1A1, COL1A2 | Osteogenesis imperfecta, Ehlers–Danlos syndrome, infantile cortical hyperostosis a.k.a. Caffey's disease |
| II | Hyaline cartilage, makes up 50% of all cartilage protein. Vitreous humour of the eye. | COL2A1 | Collagenopathy, types II and XI |
| III | This is the collagen of granulation tissue and is produced quickly by young fibroblasts before the tougher type I collagen is synthesized. Reticular fiber. Also found in artery walls, skin, intestines and the uterus | COL3A1 | Ehlers–Danlos syndrome, Dupuytren's contracture |
| IV | Basal lamina; eye lens. Also serves as part of the filtration system in capillaries and the glomeruli of nephron in the kidney. | COL4A1, COL4A2, COL4A3, COL4A4, COL4A5, COL4A6 | Alport syndrome, Goodpasture's syndrome |
| V | Most interstitial tissue, assoc. with type I, associated with placenta | COL5A1, COL5A2, COL5A3 | Ehlers–Danlos syndrome (classical) |
| VI | Most interstitial tissue, assoc. with type I | COL6A1, COL6A2, COL6A3, COL6A5 | Ulrich myopathy, Bethlem myopathy, atopic dermatitis[41] |
| VII | Forms anchoring fibrils in dermoepidermal junctions | COL7A1 | Epidermolysis bullosa dystrophica |
| VIII | Some endothelial cells | COL8A1, COL8A2 | Posterior polymorphous corneal dystrophy 2 |
| IX | FACIT collagen, cartilage, assoc. with type II and XI fibrils | COL9A1, COL9A2, COL9A3 | EDM2 and EDM3 |
| X | Hypertrophic and mineralizing cartilage | COL10A1 | Schmid metaphyseal dysplasia |
| XI | Cartilage | COL11A1, COL11A2 | Collagenopathy, types II and XI |
| XII | FACIT collagen, interacts with type I containing fibrils, decorin and glycosaminoglycans | COL12A1 | – |
| XIII | Transmembrane collagen, interacts with integrin a1b1, fibronectin and components of basement membranes like nidogen and perlecan. | COL13A1 | – |
| XIV | FACIT collagen, also known as undulin | COL14A1 | – |
| XV | – | COL15A1 | – |
| XVI | FACIT collagen | COL16A1 | – |
| XVII | Transmembrane collagen, also known as BP180, a 180 kDa protein | COL17A1 | Bullous pemphigoid and certain forms of junctional epidermolysis bullosa |
| XVIII | Source of endostatin | COL18A1 | – |
| XIX | FACIT collagen | COL19A1 | – |
| XX | – | COL20A1 | – |
| XXI | FACIT collagen | COL21A1 | – |
| XXII | FACIT collagen | COL22A1 | – |
| XXIII | MACIT collagen | COL23A1 | – |
| XXIV | – | COL24A1 | – |
| XXV | – | COL25A1 | – |
| XXVI | – | EMID2 | – |
| XXVII | – | COL27A1 | – |
| XXVIII | – | COL28A1 | – |
| XXIX | – | COL29A1 | – |
In addition to the above-mentioned disorders, excessive deposition of collagen occurs in scleroderma.
Diseases
One thousand mutations have been identified in 12 out of more than 20 types of collagen. These mutations can lead to various diseases at the tissue level.[42]
Osteogenesis imperfecta – Caused by a mutation in type 1 collagen, a dominant autosomal disorder, results in weak bones and irregular connective tissue; some cases can be mild while others can be lethal. Mild cases have lowered levels of collagen type 1, while severe cases have structural defects in collagen.[43]
Chondrodysplasias – Skeletal disorder believed to be caused by a mutation in type 2 collagen, further research is being conducted to confirm this.[44]
Ehlers–Danlos syndrome – Thirteen different types of this disorder, which lead to deformities in connective tissue, are known.[45] Some of the rarer types can be lethal, leading to the rupture of arteries. Each syndrome is caused by a different mutation. For example, the vascular type (vEDS) of this disorder is caused by a mutation in collagen type 3.[46]
Alport syndrome – Can be passed on genetically, usually as X-linked dominant, but also as both an autosomal dominant and autosomal recessive disorder. Those with the condition have problems with their kidneys and eyes, and loss of hearing can also develop during childhood or adolescence.[47]
Knobloch syndrome – Caused by a mutation in the COL18A1 gene that codes for the production of collagen XVIII. Patients present with protrusion of the brain tissue and degeneration of the retina; an individual who has family members with the disorder is at an increased risk of developing it themselves since there is a hereditary link.[42]
Animal harvesting
When not synthesized, collagen can be harvested from animal skin. This has led to deforestation, as has occurred in Paraguay, where large collagen producers buy large numbers of cattle hides from regions that have been clear-cut for cattle grazing.[48]
Characteristics
Collagen is one of the long, fibrous structural proteins whose functions are quite different from those of globular proteins, such as enzymes. Tough bundles of collagen called "collagen fibers" are a major component of the extracellular matrix that supports most tissues and gives cells structure from the outside, but collagen is also found inside certain cells. Collagen has great tensile strength and is the main component of fascia, cartilage, ligaments, tendons, bone, and skin.[49][50] Along with elastin and soft keratin, it is responsible for skin strength and elasticity, and its degradation leads to wrinkles that accompany aging.[51] It strengthens blood vessels and plays a role in tissue development. It is present in the cornea and lens of the eye in crystalline form. It may be one of the most abundant proteins in the fossil record, given that it appears to fossilize frequently, even in bones from the Mesozoic and Paleozoic.[52]
Mechanical properties
Collagen is a complex hierarchical material with mechanical properties that vary significantly across different scales.
On the molecular scale, atomistic and coarse-grained modeling simulations, as well as numerous experimental methods, have led to several estimates of the Young's modulus of collagen at the molecular level. Only above a certain strain rate is there a strong relationship between elastic modulus and strain rate, possibly due to the large number of atoms in a collagen molecule.[53] The length of the molecule is also important, where longer molecules have lower tensile strengths than shorter ones due to short molecules having a large proportion of hydrogen bonds being broken and reformed.[54]
On the fibrillar scale, collagen has a lower modulus compared to the molecular scale, and varies depending on geometry, scale of observation, deformation state, and hydration level.[53] By increasing the crosslink density from zero to 3 per molecule, the maximum stress the fibril can support increases from 0.5 GPa to 6 GPa.[55]
Limited tests have been done on the tensile strength of the collagen fiber, but generally it has been shown to have a lower Young's modulus compared to fibrils.[56]
When studying the mechanical properties of collagen, tendon is often chosen as the ideal material because it is close to a pure and aligned collagen structure. However, at the macro, tissue scale, the vast number of structures that collagen fibers and fibrils can be arranged into results in highly variable properties. For example, tendon has primarily parallel fibers, whereas skin consists of a net of wavy fibers, resulting in a much higher strength and lower ductility in tendon compared to skin. The mechanical properties of collagen at multiple hierarchical levels are given.
| Hierarchical Level | Young's modulus |
|---|---|
| Molecular (via atomistic modeling) | 2.4-7 GPa[57][58] |
| Fibril | 0.2-0.8 GPa[59] |
| Fiber (measured from cross-linked rat tail tendon) | 1.10 GPa[60] |
| Fiber (measured from non-cross-linked rat tail tendon) | 50-250 MPa[60] |
Collagen is known to be a viscoelastic solid. When the collagen fiber is modeled as two Kelvin-Voigt models in series, each consisting of a spring and a dashpot in parallel, the strain in the fiber can be modeled according to the following equation:
where α, β, and γ are defined materials properties, εD is fibrillar strain, and εT is total strain.[61]
Uses

Collagen has a wide variety of applications. In the medical industry, it is used in cosmetic surgery and burn surgery. An example of collagen use for food manufacturing is in casings for sausages.
If collagen is subject to sufficient denaturation, such as by heating, the three tropocollagen strands separate partially or completely into globular domains, containing a different secondary structure to the normal collagen polyproline II (PPII) of random coils. This process describes the formation of gelatin, which is used in many foods, including flavored gelatin desserts. Besides food, gelatin has been used in pharmaceutical, cosmetic, and photography industries. It is also used as a dietary supplement, and has been advertised as a potential remedy against the ageing process.[62][63][64]
From the Greek for glue, kolla, the word collagen means "glue producer" and refers to the early process of boiling the skin and sinews of horses and other animals to obtain glue. Collagen adhesive was used by Egyptians about 4,000 years ago, and Native Americans used it in bows about 1,500 years ago. The oldest glue in the world, carbon-dated as more than 8,000 years old, was found to be collagen – used as a protective lining on rope baskets and embroidered fabrics, to hold utensils together, and in crisscross decorations on human skulls.[65] Collagen normally converts to gelatin, but survived due to dry conditions. Animal glues are thermoplastic, softening again upon reheating, so they are still used in making musical instruments such as fine violins and guitars, which may have to be reopened for repairs – an application incompatible with tough, synthetic plastic adhesives, which are permanent. Animal sinews and skins, including leather, have been used to make useful articles for millennia.
Gelatin-resorcinol-formaldehyde glue (and with formaldehyde replaced by less-toxic pentanedial and ethanedial) has been used to repair experimental incisions in rabbit lungs.[66]
Cosmetics
Collagen is a protein in skin, hair, nails, and other tissues.[67] Collagen cremes are marketed as cosmetics even though collagen cannot penetrate the skin because its fibers are too large.[68] Partially hydrolyzed forms of collagen and low molecular weight collagen peptides, such as glycyl-prolyl-hydroxyproline, are more commonly used in cosmetics products than collagen itself in the unproven belief that topical absorption is improved.[68][69]
History
The molecular and packing structures of collagen eluded scientists over decades of research. The first evidence that it possesses a regular structure at the molecular level was presented in the mid-1930s.[70][71] Research then concentrated on the conformation of the collagen monomer, producing several competing models, although correctly dealing with the conformation of each individual peptide chain. The triple-helical "Madras" model, proposed by G. N. Ramachandran in 1955, provided an accurate model of quaternary structure in collagen.[72][73][74][75][76] This model was supported by further studies of higher resolution in the late 20th century.[77][78][79][80]
The packing structure of collagen has not been defined to the same degree outside of the fibrillar collagen types, although it has been long known to be hexagonal.[34][81][82] As with its monomeric structure, several conflicting models propose either that the packing arrangement of collagen molecules is 'sheet-like', or is microfibrillar.[83][84] The microfibrillar structure of collagen fibrils in tendon, cornea and cartilage was imaged directly by electron microscopy in the late 20th century and early 21st century.[85][86][87] The microfibrillar structure of rat tail tendon was modeled as being closest to the observed structure, although it oversimplified the topological progression of neighboring collagen molecules, and so did not predict the correct conformation of the discontinuous D-periodic pentameric arrangement termed microfibril.[33][88][89]
See also
- Collagen hybridizing peptide, a peptide that can bind to denatured collagen
- Hypermobility spectrum disorder
- Metalloprotease inhibitor
- Osteoid, a collagen-containing component of bone
- Collagen loss
References
- ↑ "Collagen structure and stability". Annual Review of Biochemistry 78: 929–958. 2009. doi:10.1146/annurev.biochem.77.032207.120833. PMID 19344236.
- ↑ "Leather grown using biotechnology is about to hit the catwalk". The Economist. 26 August 2017. https://www.economist.com/news/science-and-technology/21727059-genetic-engineering-used-make-leather-without-animals-leather-grown-using.
- ↑ Britannica Concise Encyclopedia 2007
- ↑ Chemical and Functional Properties of Food Proteins. Boca Raton, Florida: CRC Press. 2001. p. 242. ISBN 978-1-56676-960-0.
- ↑ "Conditions Affecting the Hydrolysis of Collagen to Gelatin". Industrial and Engineering Chemistry 15 (11): 1154–59. 1923. doi:10.1021/ie50167a018.
- ↑ O.E.D. 2nd Edition 2005
- ↑ "The origin of metazoan complexity: porifera as integrated animals". Integrative and Comparative Biology 43 (1): 3–10. February 2003. doi:10.1093/icb/43.1.3. PMID 21680404.
- ↑ 8.0 8.1 "The collagen family". Cold Spring Harbor Perspectives in Biology 3 (1). January 2011. doi:10.1101/cshperspect.a004978. PMID 21421911.
- ↑ "Collagenous transmembrane proteins: recent insights into biology and pathology". Journal of Biological Chemistry 280 (6): 4005–4008. February 2005. doi:10.1074/jbc.R400034200. PMID 15561712.
- ↑ Sabiston textbook of surgery board review, 7th edition. Chapter 5 wound healing, question 14
- ↑ "Materials science perspective of multifunctional materials derived from collagen". International Materials Reviews 66 (3): 160–87. 3 April 2021. doi:10.1080/09506608.2020.1750807. ISSN 0950-6608. Bibcode: 2021IMRv...66..160A. https://www.tandfonline.com/doi/full/10.1080/09506608.2020.1750807.
- ↑ "Collagen scaffolds for orthopedic regenerative medicine". The Journal of the Minerals, Metals & Materials Society 63 (4): 66–73. 2011. doi:10.1007/s11837-011-0061-y. Bibcode: 2011JOM....63d..66C.
- ↑ "Collagen sponges for bone regeneration with rhBMP-2". Advanced Drug Delivery Reviews 55 (12): 1613–1629. November 2003. doi:10.1016/j.addr.2003.08.010. PMID 14623404.
- ↑ "Collagen membranes: a review". Journal of Periodontology 72 (2): 215–229. February 2001. doi:10.1902/jop.2001.72.2.215. PMID 11288796.
- ↑ "Hydrogels for tissue engineering: scaffold design variables and applications". Biomaterials 24 (24): 4337–4351. November 2003. doi:10.1016/S0142-9612(03)00340-5. PMID 12922147.
- ↑ "Collagen multifilament spinning". Materials Science & Engineering. C, Materials for Biological Applications 106. January 2020. doi:10.1016/j.msec.2019.110105. PMID 31753356.
- ↑ "An improved collagen scaffold for skeletal regeneration". Journal of Biomedical Materials Research. Part A 94 (2): 371–379. August 2010. doi:10.1002/jbm.a.32694. PMID 20186736.
- ↑ 18.0 18.1 "Collagen dressing versus conventional dressings in burn and chronic wounds: a retrospective study". Journal of Cutaneous and Aesthetic Surgery 4 (1): 12–16. January 2011. doi:10.4103/0974-2077.79180. PMID 21572675.
- ↑ "Topical Collagen-Based Biomaterials for Chronic Wounds: Rationale and Clinical Application". Advances in Wound Care 5 (1): 19–31. January 2016. doi:10.1089/wound.2014.0595. PMID 26858912.
- ↑ "Collagen and Rosehip Extract Sachet". http://alainapharma.com/Collagen%20+%20Rosehip%20Extract.html.
- ↑ "Type-1 pericytes accumulate after tissue injury and produce collagen in an organ-dependent manner". Stem Cell Research & Therapy 5 (6). November 2014. doi:10.1186/scrt512. PMID 25376879.
- ↑ "Cell culture: building a better matrix". Nature Methods 6 (8): 619–22. 2009. doi:10.1038/nmeth0809-619.
- ↑ "Molecular structure of the collagen triple helix". Advances in Protein Chemistry 70: 301–339. 2005-01-01. doi:10.1016/S0065-3233(05)70009-7. ISBN 978-0-12-034270-9. PMID 15837519.
- ↑ 24.0 24.1 24.2 24.3 24.4 "Fish bone chemistry and ultrastructure: implications for taphonomy and stable isotope analysis". Journal of Archaeological Science 38 (12): 3358–72. 2011. doi:10.1016/j.jas.2011.07.022. Bibcode: 2011JArSc..38.3358S.
- ↑ "Ascorbate requirement for hydroxylation and secretion of procollagen: relationship to inhibition of collagen synthesis in scurvy". The American Journal of Clinical Nutrition 54 (6 Suppl): 1135S–1140S. December 1991. doi:10.1093/ajcn/54.6.1135s. PMID 1720597.
- ↑ "Prolyl 4-hydroxylase". Critical Reviews in Biochemistry and Molecular Biology 45 (2): 106–124. April 2010. doi:10.3109/10409231003627991. PMID 20199358.
- ↑ "Ascorbate is consumed stoichiometrically in the uncoupled reactions catalyzed by prolyl 4-hydroxylase and lysyl hydroxylase". The Journal of Biological Chemistry 259 (9): 5403–5405. May 1984. doi:10.1016/S0021-9258(18)91023-9. PMID 6325436.
- ↑ "Induction of collagenolytic and proteolytic activities by anti-inflammatory drugs in the skin and fibroblast". Biochemical Pharmacology 17 (10): 2081–2090. October 1968. doi:10.1016/0006-2952(68)90182-2. PMID 4301453.
- ↑ "preprocollagen". https://medical-dictionary.thefreedictionary.com/preprocollagen.
- ↑ "Code for collagen stability deciphered". Nature 392 (6677): 666–667. 1998. doi:10.1038/33573. PMID 9565027. Bibcode: 1998Natur.392..666H.
- ↑ "Building collagen molecules, fibrils, and suprafibrillar structures". Journal of Structural Biology 137 (1–2): 2–10. 2002. doi:10.1006/jsbi.2002.4450. PMID 12064927.
- ↑ 32.0 32.1 "The collagen superfamily--diverse structures and assemblies". Essays in Biochemistry 27: 49–67. 1992. PMID 1425603.
- ↑ 33.0 33.1 33.2 "Microfibrillar structure of type I collagen in situ". Proceedings of the National Academy of Sciences of the United States of America 103 (24): 9001–9005. June 2006. doi:10.1073/pnas.0502718103. PMID 16751282. Bibcode: 2006PNAS..103.9001O.
- ↑ 34.0 34.1 "Quasi-hexagonal molecular packing in collagen fibrils". Nature 282 (5741): 878–880. 1979. doi:10.1038/282878a0. PMID 514368. Bibcode: 1979Natur.282..878H.
- ↑ "Collagen fibril architecture, domain organization, and triple-helical conformation govern its proteolysis". Proceedings of the National Academy of Sciences of the United States of America 105 (8): 2824–2829. February 2008. doi:10.1073/pnas.0710588105. PMID 18287018. Bibcode: 2008PNAS..105.2824P.
- ↑ "Role of X-ray Scattering Techniques in Understanding the Collagen Structure of Leather" (in en). ChemistrySelect 4 (48): 14091–102. 2019. doi:10.1002/slct.201902908. ISSN 2365-6549. http://nectar.northampton.ac.uk/15330/1/Role_Xray_Scattering_Leather_Covington_etel_2019.pdf.
- ↑ "Candidate cell and matrix interaction domains on the collagen fibril, the predominant protein of vertebrates". The Journal of Biological Chemistry 283 (30): 21187–21197. July 2008. doi:10.1074/jbc.M709319200. PMID 18487200.
- ↑ "Type I collagen and collagen mimetics as angiogenesis promoting superpolymers". Current Pharmaceutical Design 13 (35): 3608–3621. 2007. doi:10.2174/138161207782794176. PMID 18220798.
- ↑ "Nanomechanical heterogeneity in the gap and overlap regions of type I collagen fibrils with implications for bone heterogeneity". Biomacromolecules 10 (9): 2565–2570. September 2009. doi:10.1021/bm900519v. PMID 19694448.
- ↑ Ross, M. H. and Pawlina, W. (2011) Histology, 6th ed., Lippincott Williams & Wilkins, p. 218.
- ↑ "Variants in a novel epidermal collagen gene (COL29A1) are associated with atopic dermatitis". PLOS Biology 5 (9). September 2007. doi:10.1371/journal.pbio.0050242. PMID 17850181.
- ↑ 42.0 42.1 "Collagen XVIII mutation in Knobloch syndrome with acute lymphoblastic leukemia". American Journal of Medical Genetics. Part A 152A (11): 2875–2879. November 2010. doi:10.1002/ajmg.a.33621. PMID 20799329.
- ↑ "Mutations in type I collagen genes resulting in osteogenesis imperfecta in humans". Acta Biochimica Polonica 49 (2): 433–441. 2002. doi:10.18388/abp.2002_3802. PMID 12362985. http://www.actabp.pl/pdf/2_2002/433-441.pdf.
- ↑ "Type II collagen screening in the human chondrodysplasias". American Journal of Medical Genetics 34 (4): 579–583. December 1989. doi:10.1002/ajmg.1320340425. PMID 2624272.
- ↑ "The 2017 international classification of the Ehlers-Danlos syndromes". American Journal of Medical Genetics. Part C, Seminars in Medical Genetics 175 (1): 8–26. March 2017. doi:10.1002/ajmg.c.31552. PMID 28306229.
- ↑ "Ehlers-Danlos syndrome and type III collagen abnormalities: a variable clinical spectrum". Clinical Genetics 53 (6): 440–446. June 1998. doi:10.1111/j.1399-0004.1998.tb02592.x. PMID 9712532.
- ↑ "Alport Syndrome and Thin Basement Membrane Nephropathy". GeneReviews. Collagen IV-Related Nephropathies. Seattle WA: University of Washington, Seattle. 1993. https://www.ncbi.nlm.nih.gov/books/NBK1207/.
- ↑ Alexander, Iñigo (2024-10-09). "Collagen and meat giants fuel deforestation and rights violations in Paraguay: Report" (in en-US). https://news.mongabay.com/2024/10/collagen-and-cattle-fuel-deforestation-and-rights-violations-in-paraguay-says-new-report/.
- ↑ Collagen: Structure and Mechanics. New York: Springer. 2008. ISBN 978-0-387-73905-2.
- ↑ "Nature designs tough collagen: explaining the nanostructure of collagen fibrils". Proceedings of the National Academy of Sciences of the United States of America 103 (33): 12285–12290. August 2006. doi:10.1073/pnas.0603216103. PMID 16895989. Bibcode: 2006PNAS..10312285B.
- ↑ Dermal Fillers | The Ageing Skin . Pharmaxchange.info. Retrieved on 21 April 2013.
- ↑ "Analysis of fossil bone organic matrix by transmission electron microscopy". Comptes Rendus Palevol 11 (5–6): 357–66. 2011. doi:10.1016/j.crpv.2011.04.004.
- ↑ 53.0 53.1 "Hierarchical structure and nanomechanics of collagen microfibrils from the atomistic scale up". Nano Letters 11 (2): 757–766. February 2011. doi:10.1021/nl103943u. PMID 21207932. Bibcode: 2011NanoL..11..757G.
- ↑ "Steered Molecular Dynamics Study of Mechanical Response of Full Length and Short Collagen Molecules" (in en). Journal of Nanomechanics and Micromechanics 1 (3): 104–110. 2011. doi:10.1061/(ASCE)NM.2153-5477.0000035. ISSN 2153-5434.
- ↑ "Nanomechanics of collagen fibrils under varying cross-link densities: atomistic and continuum studies". Journal of the Mechanical Behavior of Biomedical Materials 1 (1): 59–67. January 2008. doi:10.1016/j.jmbbm.2007.04.001. PMID 19627772.
- ↑ "Mechanical characterization of collagen fibers and scaffolds for tissue engineering". Biomaterials 24 (21): 3805–3813. September 2003. doi:10.1016/s0142-9612(03)00206-0. PMID 12818553.
- ↑ "Molecular assessment of the elastic properties of collagen-like homotrimer sequences". Biomechanics and Modeling in Mechanobiology 3 (4): 224–234. June 2005. doi:10.1007/s10237-004-0064-5. PMID 15824897.
- ↑ "Atomistic and continuum modeling of mechanical properties of collagen: Elasticity, fracture, and self-assembly" (in en). Journal of Materials Research 21 (8): 1947–1961. August 2006. doi:10.1557/jmr.2006.0236. ISSN 2044-5326. Bibcode: 2006JMatR..21.1947B.
- ↑ "Micromechanical testing of individual collagen fibrils". Macromolecular Bioscience 6 (9): 697–702. September 2006. doi:10.1002/mabi.200600063. PMID 16967482.
- ↑ 60.0 60.1 "Mechanical characterization of collagen fibers and scaffolds for tissue engineering". Biomaterials 24 (21): 3805–3813. September 2003. doi:10.1016/S0142-9612(03)00206-0. PMID 12818553.
- ↑ "Viscoelastic properties of collagen: synchrotron radiation investigations and structural model". Philosophical Transactions of the Royal Society of London. Series B, Biological Sciences 357 (1418): 191–197. February 2002. doi:10.1098/rstb.2001.1033. PMID 11911776.
- ↑ "Collagen Supplements for Aging and Wrinkles: A Paradigm Shift in the Fields of Dermatology and Cosmetics". Dermatology Practical & Conceptual 12 (1): e2022018. February 2022. doi:10.5826/dpc.1201a18. PMID 35223163.
- ↑ "The radical new theory that wrinkles actually cause ageing". New Scientist. Apr 1, 2023. https://www.newscientist.com/article/2366093-the-radical-new-theory-that-wrinkles-actually-cause-ageing/.
- ↑ Campos, Luana Dias; Santos Junior, Valfredo de Almeida; Pimentel, Júlia Demuner; Carregã, Gabriel Lusi Fernandes; Cazarin, Cinthia Baú Betim (2023). "Collagen supplementation in skin and orthopedic diseases: A review of the literature". Heliyon 9 (4). doi:10.1016/j.heliyon.2023.e14961. ISSN 2405-8440. PMID 37064452. Bibcode: 2023Heliy...914961C.
- ↑ "Oldest Glue Discovered". Archaeology. 21 May 1998. http://www.archaeology.org/online/news/glue.html.
- ↑ "Formaldehyde-free collagen glue in experimental lung gluing". The Annals of Thoracic Surgery 57 (6): 1622–1627. June 1994. doi:10.1016/0003-4975(94)90136-8. PMID 8010812.
- ↑ "Considering collagen drinks and supplements?". Harvard Health Publishing. 2023-04-12. https://www.health.harvard.edu/blog/considering-collagen-drinks-and-supplements-202304122911.
- ↑ 68.0 68.1 "Collagen" (in en-us). 2021-05-26. https://www.hsph.harvard.edu/nutritionsource/collagen/.
- ↑ "Bioactive Peptide Profiling in Collagen Hydrolysates: Comparative Analysis Using Targeted and Untargeted Liquid Chromatography-Tandem Mass Spectrometry Quantification". Molecules 29 (11). May 2024. doi:10.3390/molecules29112592. PMID 38893467.
- ↑ "X-Ray Reflections of Long Spacing from Tendon". Science 82 (2121): 175–176. August 1935. doi:10.1126/science.82.2121.175. PMID 17810172. Bibcode: 1935Sci....82..175W.
- ↑ "New measurements of previously unknown large interplanar spacings in natural materials". J. Am. Chem. Soc. 57 (8): 1509. 1935. doi:10.1021/ja01311a504. Bibcode: 1935JAChS..57.1509C.
- ↑ "Structure of collagen". Nature 176 (4482): 593–595. September 1955. doi:10.1038/176593a0. PMID 13265783. Bibcode: 1955Natur.176..593R.
- ↑ "Structure of collagen". Nature 174 (4423): 269–270. August 1954. doi:10.1038/174269c0. PMID 13185286. Bibcode: 1954Natur.174..269R.
- ↑ Balasubramanian, D . (October 2001). "GNR – A Tribute". Resonance 6 (10): 2–4. doi:10.1007/BF02836961. http://www.ias.ac.in/resonance/php/toc.php?vol=06&issue=10.
- ↑ "Binding of phosphate and pyrophosphate ions at the active site of human angiogenin as revealed by X-ray crystallography". Protein Science 10 (8): 1669–1676. August 2001. doi:10.1110/ps.13601. PMID 11468363.
- ↑ "G.N. Ramachandran". Nature Structural Biology 8 (6): 489–491. June 2001. doi:10.1038/88544. PMID 11373614.
- ↑ "Chain conformation in the collagen molecule". Journal of Molecular Biology 129 (3): 463–481. April 1979. doi:10.1016/0022-2836(79)90507-2. PMID 458854.
- ↑ "Crystal and molecular structure of a collagen-like polypeptide (Pro-Pro-Gly)10". Journal of Molecular Biology 152 (2): 427–443. October 1981. doi:10.1016/0022-2836(81)90252-7. PMID 7328660.
- ↑ "On the molecular structure of collagen". Nature 221 (5184): 914–917. March 1969. doi:10.1038/221914a0. PMID 5765503. Bibcode: 1969Natur.221..914T.
- ↑ "Crystal and molecular structure of a collagen-like peptide at 1.9 A resolution". Science 266 (5182): 75–81. October 1994. doi:10.1126/science.7695699. PMID 7695699. Bibcode: 1994Sci...266...75B.
- ↑ "Crystalline three-dimensional packing is a general characteristic of type I collagen fibrils". FEBS Letters 113 (2): 238–240. May 1980. doi:10.1016/0014-5793(80)80600-4. PMID 7389896. Bibcode: 1980FEBSL.113..238J.
- ↑ "Unit cell and molecular connectivity in tendon collagen". International Journal of Biological Macromolecules 3 (3): 193–200. 1981. doi:10.1016/0141-8130(81)90063-5.
- ↑ "Molecular packing in type I collagen fibrils". Journal of Molecular Biology 193 (1): 115–125. January 1987. doi:10.1016/0022-2836(87)90631-0. PMID 3586015.
- ↑ "Molecular packing of type I collagen in tendon". Journal of Molecular Biology 275 (2): 255–267. January 1998. doi:10.1006/jmbi.1997.1449. PMID 9466908.
- ↑ "Subfibrillar architecture and functional properties of collagen: a comparative study in rat tendons". Journal of Anatomy 172: 157–164. October 1990. PMID 2272900.
- ↑ "Corneal collagen fibril structure in three dimensions: Structural insights into fibril assembly, mechanical properties, and tissue organization". Proceedings of the National Academy of Sciences of the United States of America 98 (13): 7307–7312. June 2001. doi:10.1073/pnas.111150598. PMID 11390960. Bibcode: 2001PNAS...98.7307H.
- ↑ "The 10+4 microfibril structure of thin cartilage fibrils". Proceedings of the National Academy of Sciences of the United States of America 103 (46): 17249–17254. November 2006. doi:10.1073/pnas.0608417103. PMID 17088555. Bibcode: 2006PNAS..10317249H.
- ↑ "Re: Microfibrillar structure of type I collagen in situ". Acta Crystallographica. Section D, Biological Crystallography 65 (Pt 9): 1009–10. September 2009. doi:10.1107/S0907444909023051. PMID 19690380. Bibcode: 2009AcCrD..65.1007O.
- ↑ Orgel, Joseph (2009). "On the packing structure of collagen: response 0to Okuyama et al.'s comment on Microfibrillar structure of type I collagen in situ". Acta Crystallographica Section D D65 (9): 1009. doi:10.1107/S0907444909028741. Bibcode: 2009AcCrD..65.1009O.
 |
