Astronomy:Cone beam computed tomography
| Cone beam computed tomography | |
|---|---|
| Medical diagnostics | |
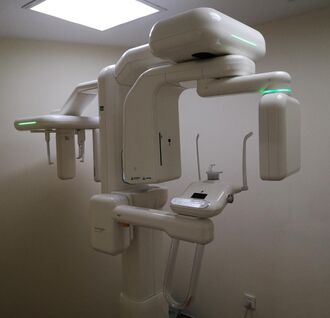 Cone Beam CT scanner | |
| MeSH | D054894 |
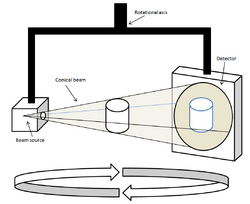
Cone beam computed tomography (or CBCT, also referred to as C-arm CT, cone beam volume CT, flat panel CT or Digital Volume Tomography (DVT)) is a medical imaging technique consisting of X-ray computed tomography where the X-rays are divergent, forming a cone.[1]
CBCT has become increasingly important in treatment planning and diagnosis in implant dentistry, ENT, orthopedics, and interventional radiology (IR), among other things. Because of increased access to the technology, CBCT scanners are now widely used in dentistry, such as in the fields of oral surgery, endodontics and orthodontics. Integrated CBCT is also an important tool for patient positioning and verification in image-guided radiation therapy (IGRT).
During dental and orthodontic imaging, the CBCT scanner rotates around the patient's head, acquiring up to 600 distinct images. For interventional radiology, the patient is positioned offset to the table so that the region of interest is centered in the field of view for the cone beam. A single 200 degree rotation over the region of interest acquires a volumetric data set. The scanning software collects the data and reconstructs it, producing what is termed a digital volume composed of three-dimensional voxels of anatomical data that can then be manipulated and visualized with specialized software.[2][3] CBCT shares many similarities with traditional (fan beam) CT however there are important differences, particularly for reconstruction. CBCT has been described as the gold standard for imaging the oral and maxillofacial area.
History
Oral and Maxillofacial Radiology
In the late 1990s, Dr Yoshinori Arai in Japan and Dr Piero Mozzo in Italy independently developed Cone Beam Computed Technology for oral and maxillofacial radiology.[4] The first commercial system (the NewTom 9000) was introduced in the European market in 1996 and into the US market in 2001, by Italian company Quantitative Radiology (also known as QR, based in Verona).[2][5]
-
Axial image obtained from the first Cone-Beam 3D Scan performed on July 1, 1994[6]
-
Axial image obtained from the first Cone-Beam 3D Scan performed on July 1, 1994
-
Axial image obtained from the first Cone-Beam 3D Scan performed on July 1, 1994
-
Original notes about the first Cone-Beam 3D Scan performed on July 1, 1994
Radiotherapy
Cone beam CT using kilovoltage X-rays (as used for diagnostic, rather than therapeutic purposes) attached to a linear accelerator treatment machine was first developed in the late 1990s and early 2000s.[7] Such systems have since become common on latest generation linacs.[8] In the late 2010s CBCT also started to become available on-board particle therapy delivery systems.[9]
Interventional radiology
While CBCT with X-ray image intensifiers was experimented with in the late 1990s, it was not until the adoption of flat-panel X-ray detectors, with improved contrast and spatial resolution, that CBCT became practical for clinical use in interventional radiology procedures.[10][11] Many fixed, and even mobile, C-arm fluoroscopy systems are now capable of CBCT acquisitions, in addition to traditional planar fluoroscopy.[12][13] CBCT provides image guidance during interventional radiology procedures for conditions such as knee osteoarthritis, benign prostatic hyperplasia, and hepatocellular carcinoma.[14][15][16][17]
Applications
Endodontics
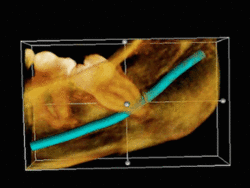
The most significant advantage of the CBCT in Endodontics is that it can show critical root canal anatomical features that conventional intraoral or panoramic images cannot.[18]
According to the American Association of Endodontics, there are numerous specific situations in which 3D images produced by CBCT enhance diagnosis and influence treatment, and its use cannot be disputed over conventional intraoral radiology based on ALARA principles.[19]
Implantology
A dental cone beam scan offers useful information when it comes to the assessment and planning of surgical implants. The American Academy of Oral and Maxillofacial Radiology (AAOMR) suggests cone-beam CT as the preferred method for presurgical assessment of dental implant sites.[20]
Orthodontics
As a 3D rendition, CBCT offers an undistorted view of the dentition that can be used to accurately visualize both erupted and non-erupted teeth, tooth root orientation and anomalous structures, that conventional 2D radiography cannot.[21]
Processing example using x-ray data from a tooth model:
-
single sampled (noisy) image
-
several samples overlay
-
joined images to panoramic
-
algorithmic reconstruction
-
in-vivo image
Orthopedics
The CBCT scanner offers undistorted views of the extremities. One advantage of orthopedic CBCT is the ability to take weight bearing images of the lower extremities. In the realm of the foot and ankle particularly, weight bearing CBCT is gaining momentum due to its ability to combine 3 dimensional and weight bearing information which are of the utmost importance in diagnosis and surgical planning.[22] The preferred term used for CBCT in the lower limb is thus WBCT for Weight Bearing CT following the first scientific publications on the subject.[23][24][25][26]
Image-guided radiation therapy
Image-guided radiation therapy is a form of external beam radiotherapy where the patient is positioned with the organs to be treated accurately matched in position to the treatment field, to reduce the dose to nearby organs which are not being treated. Many organs inside the body move by millimeters relative to the external skin surfaces, and a CBCT scanner mounted on the head of the radiotherapy unit is used immediately before treatment (and sometimes again during treatment) to ensure the patient's organs are in exactly the right position to match the treatment field, and to adjust the position of the treatment table if necessary.
The images may also be used to check for other requirements of some types of treatment, such as full or empty bladder, empty rectum, etc.[8][27] The same cone beam beam source and detector can alternatively be used to take simple X-ray positioning images if the organ shows particularly well on X-ray or if Fiducial markers have been inserted into the organ.[28]
Interventional radiology
The CBCT scanner is mounted on a C-arm fluoroscopy unit in the interventional radiology (IR) suite, which offers real time imaging with a stationary patient. This eliminates the time needed to transfer a patient from the angiography suite to a conventional computed tomography scanner and facilitates a broad spectrum of applications of CBCT during IR procedures. The clinical applications of CBCT in IR include treatment planning, device or implant positioning and assessment, intra-procedural localization, and assessment of procedure endpoints. CBCT is useful as a primary and supplemental form of imaging. It is an excellent adjunct to DSA and fluoroscopy for soft tissue and vascular visibility during complex procedures. The use of CBCT before fluoroscopy potentially reduces patient radiation exposure.[3]
Clinical applications
- Chemoembolization for Hepatocellular Carcinoma: CBCT with contrast confirms that the proper artery is selected to deliver the therapy. The contrast enhances the parenchyma supplied by the selected artery and therefore reveals if the vasculature also supplies the tumor. Post-treatment non-contrast CBCT confirms lipiodol staining of the tumor, which improves operator confidence of complete tumor coverage or further treatment.[29]
- Prostatic artery embolization for benign prostatic hyperplasia: CBCT provides the soft tissue detail needed to visualize prostatic enhancement, identify duplicated prostatic arteries, and avoid nontarget embolization. CBCT is superior to DSA for this therapy since the enhancement patterns on DSA can be difficult to discern due to the overlapping pelvic structures and variable arterial anatomy.[30]
- Abscess drainage: CBCT confirms needle tip location after placement under ultrasound and confirms drain placement by revealing contrast injection into the desired location.
- Adrenal Vein sampling for an adenoma: contrast-enhanced CBCT shows perfusion of the adrenal gland to confirm catheter placement for obtaining a satisfactory sample.[31]
- Stent placement: CBCT improves the visualization of intracranial and extracranial stents compared to conventional DSA and digital radiography by providing a better depiction of the relationship of the stents to nearby structures (i.e. vascular walls and aneurysm lumen).[32]
- Lung nodule percutaneous transthoracic needle biopsy: CBCT guides needle placement and demonstrated a diagnostic accuracy, sensitivity, and specificity of 98.2%, 96.8%, and 100%, respectively. Diagnostic accuracy was unaffected by technically challenging conditions.[33]
- Vascular Anomalies: After correction of arteriovenous malformations with coiling, CBCT sensitively detects small infarcts in tissue that has been "sacrificed" during the procedure to prevent further shunting. The infarcted tissue appears as a small area of contrast retention.
Industrial applications
Cone beam CT is used for material analysis, metrology, and nondestructive testing in the manufacturing sector. Cone beam CT is also inspect and detect defects of tiny sizes, such as internal pitting corrosion or cracks of an object in quality control.[34]
Reconstruction
Cone beam reconstruction algorithms are similar to typical tomographic reconstruction algorithms, and methods such as filtered backprojection or iterative reconstruction may be used. However, since the reconstruction is three-dimensional, modifications such as the FDK algorithm[35] may be needed.
Risks
Oral and maxillofacial radiology
Total radiation doses from 3D dental CBCT exams are 96% lower than conventional CT exams, but deliver 5-16x more radiation than standard dental 2D x-ray (OPG). The time of exposure in CBCT is also comparatively less when compared to conventional CT. [36][37][38][39][40]
CBCT use is only lightly regulated in the US. The recommended standard of care is to use the smallest possible field of view (FOV), the smallest voxel size, the lowest mA setting and the shortest exposure time in conjunction with a pulsed exposure mode of acquisition.[41] International organisations such as the World Health Organization and ICRP, as well as many local bodies and legislation, encourage the idea of justification for all medical exposures, where risks and benefits must be weighed up before a procedure goes ahead.[42]
Disadvantages
Oral and maxillofacial radiology
There are a number of drawbacks of CBCT technology over that of CT scans, such as increased susceptibility to movement artifacts (in first generation machines) and to the lack of appropriate bone density determination.[43]
Bone density and the Hounsfield scale
The Hounsfield scale is used to measure radiodensity and, in reference to CT scans, can provide an accurate absolute density for the type of tissue depicted. The radiodensity, measured in Hounsfield Units (HU, also known as CT number) is inaccurate in CBCT scans because different areas in the scan appear with different greyscale values depending on their relative positions in the organ being scanned, despite possessing identical densities, because the image value of a voxel of an organ depends on the position[clarification needed] in the image volume.[44] HU measured from the same anatomical area with both CBCT and medical-grade CT scanners are not identical[45] and are thus unreliable for determination of site-specific, radiographically-identified bone density for purposes such as the placement of dental implants, as there is "no good data to relate the CBCT HU values to bone quality."[46]
Although some authors have supported the use of CBCT technology to evaluate bone density by measuring HU,[47][48] such support is provided erroneously because scanned regions of the same density in the skull can have a different grayscale value in the reconstructed CBCT dataset.[49]
X-ray attenuation of CBCT acquisition systems currently produces different HU values for similar bony and soft tissue structures in different areas of the scanned volume (e.g. dense bone has a specific image value at the level of the menton, but the same bone has a significantly different image value at the level of the cranial base).[43]
Dental CBCT systems do not employ a standardized system for scaling the grey levels that represent the reconstructed density values and, as such, they are arbitrary and do not allow for assessment of bone quality.[50] In the absence of such a standardization, it is difficult to interpret the grey levels or impossible to compare the values resulting from different machines. While there is a general acknowledgment that this deficiency exists with CBCT systems (in that they do not correctly display HU), there has been little research conducted to attempt to correct this deficiency.[51]
With time, further advancements in CBCT reconstruction algorithms will allow for improved area detectors,[52] and this, together with enhanced postprocessing, will likely solve or reduce this problem.[44] A method for establishing attenuation coefficients with which actual HU values can be derived from CBCT "HU" values was published in 2010 and further research is currently underway to perfect this method in vivo.[51]
Interventional radiology
While the practicality of CBCT fosters its increasing application in IR, technical limitations hinder its integration into the field. The two most significant factors that affect successful integration are image quality and time (for set up, image acquisition, and image reconstruction). Compared to multidetector computed tomography (MDCT), the wider collimation in CBCT leads to increased scatter radiation and degradation of image quality as demonstrated by artifacts and decreased contrast-to-noise ratio. The temporal resolution of cesium iodide detectors in CBCT slows data acquisition time to approximately 5 to 20 seconds, which increases motion artifacts. The time required for image reconstruction takes longer for CBCT (1 minute) compared to MDCT (real time) due to the computationally demanding cone beam reconstruction algorithms.[3][29]
See also
- Computed tomography
- Cone beam reconstruction
References
- ↑ Technical Description of CBCT from University of Manchester. Citing: "Clinical applications of cone-beam computed tomography in dental practice". Journal of the Canadian Dental Association 72 (1): 75–80. February 2006. PMID 16480609. http://www.cda-adc.ca/jcda/vol-72/issue-1/75.html.
- ↑ 2.0 2.1 Hatcher DC (October 2010). "Operational principles for cone-beam computed tomography". Journal of the American Dental Association 141 (Suppl 3): 3S–6S. doi:10.14219/jada.archive.2010.0359. PMID 20884933.
- ↑ 3.0 3.1 3.2 "C-arm cone-beam CT: general principles and technical considerations for use in interventional radiology". Journal of Vascular and Interventional Radiology 19 (6): 814–20. June 2008. doi:10.1016/j.jvir.2008.02.002. PMID 18503894.
- ↑ Venkatesh, Elluru; Elluru, Snehal Venkatesh (2017-12-02). "Cone beam computed tomography: basics and applications in dentistry". Journal of Istanbul University Faculty of Dentistry 51 (3 Suppl 1): S102–S121. doi:10.17096/jiufd.00289. ISSN 2149-2352. PMID 29354314.
- ↑ Molteni, R (2014). "Oral and Maxillofacial Radiology". in Budinger, Thomas; Brahme, Anders (in en). Comprehensive Biomedical Physics. Amsterdam: Elsevier. p. 112. ISBN 978-0-444-53632-7. https://books.google.com/books?id=9RR0AwAAQBAJ&pg=RA1-PA112.
- ↑ "20st Anniversary of the 1st dental CBCT complete scan — NewTom". http://www.newtom.it/it/news-ed-eventi/eventi/2014/20deg-anniversary-of-the-1deg-dental-cbct-complete-scan.
- ↑ Thwaites, David I; Tuohy, John B (2006-07-07). "Back to the future: the history and development of the clinical linear accelerator". Physics in Medicine and Biology 51 (13): R343–R362. doi:10.1088/0031-9155/51/13/R20. PMID 16790912. https://www.sprmn.pt/pdf/pmb6_13_r20_LINACs_(Thwaites&Tuohy).pdf.
- ↑ 8.0 8.1 Shepherd, Justin (2014). "Applications of linac-mounted kilovoltage Cone-beam Computed Tomography in modern radiation therapy: A review". Polish Journal of Radiology 79: 181–193. doi:10.12659/PJR.890745. PMID 25006356.
- ↑ Herrmann, H.; Seppenwoolde, Y.; Georg, D.; Widder, J. (December 2019). "Image guidance: past and future of radiotherapy". Der Radiologe 59 (S1): 21–27. doi:10.1007/s00117-019-0573-y. PMID 31346650.
- ↑ Orth, Robert C.; Wallace, Michael J.; Kuo, Michael D. (June 2008). "C-arm Cone-beam CT: General Principles and Technical Considerations for Use in Interventional Radiology". Journal of Vascular and Interventional Radiology 19 (6): 814–820. doi:10.1016/j.jvir.2008.02.002. PMID 18503894.
- ↑ Wallace, Michael J.; Kuo, Michael D.; Glaiberman, Craig; Binkert, Christoph A.; Orth, Robert C.; Soulez, Gilles (June 2008). "Three-Dimensional C-arm Cone-beam CT: Applications in the Interventional Suite". Journal of Vascular and Interventional Radiology 19 (6): 799–813. doi:10.1016/j.jvir.2008.02.018. PMID 18503893.
- ↑ Siewerdsen, Jeffrey (2019). "Cone-Beam CT Systems". in Samei, Ehsan; Pelc, Norbert (in en). Computed Tomography: Approaches, Applications, and Operations. Cham: Springer Nature Switzerland. p. 20. ISBN 978-3-030-26956-2. https://books.google.com/books?id=saO-DwAAQBAJ&pg=PA20.
- ↑ Floridi, Chiara; Radaelli, Alessandro; Abi-Jaoudeh, Nadine; Grass, Micheal; De Lin, Ming; Chiaradia, Melanie; Geschwind, Jean-Francois; Kobeiter, Hishman et al. (July 2014). "C-arm cone-beam computed tomography in interventional oncology: technical aspects and clinical applications". La Radiologia Medica 119 (7): 521–532. doi:10.1007/s11547-014-0429-5. PMID 25012472.
- ↑ Cusumano, Lucas R.; Callese, Tyler E.; Redwood, Karen; Genshaft, Scott; Plotnik, Adam N.; Stewart, Jessica K.; Padia, Siddharth A. (2023-08-11). "Added Value of Cone-Beam CT to Identify Arterial Supply during Genicular Artery Embolization for Knee Osteoarthritis". Journal of Vascular and Interventional Radiology 34 (11): 1861–1867. doi:10.1016/j.jvir.2023.07.033. ISSN 1051-0443. PMID 37573000. https://www.sciencedirect.com/science/article/pii/S1051044323005717.
- ↑ Angle, John F. (September 2013). "Cone-beam CT: vascular applications". Techniques in Vascular and Interventional Radiology 16 (3): 144–149. doi:10.1053/j.tvir.2013.02.009. ISSN 1557-9808. PMID 23993076.
- ↑ Cadour, F.; Tradi, F.; Habert, P.; Scemama, U.; Vidal, V.; Jacquier, A.; Bartoli, J.-M.; Moulin, G. et al. (November 2020). "Prostatic artery embolization using three-dimensional cone-beam computed tomography". Diagnostic and Interventional Imaging 101 (11): 721–725. doi:10.1016/j.diii.2020.05.002. ISSN 2211-5684. PMID 32532575.
- ↑ Pung, Leland; Ahmad, Moiz; Mueller, Kerstin; Rosenberg, Jarrett; Stave, Christopher; Hwang, Gloria L.; Shah, Rajesh; Kothary, Nishita (March 2017). "The Role of Cone-Beam CT in Transcatheter Arterial Chemoembolization for Hepatocellular Carcinoma: A Systematic Review and Meta-analysis". Journal of Vascular and Interventional Radiology 28 (3): 334–341. doi:10.1016/j.jvir.2016.11.037. ISSN 1535-7732. PMID 28109724.
- ↑ Scarfe, William C.; Levin, Martin D.; Gane, David; Farman, Allan G. (2009). "Use of Cone Beam Computed Tomography in Endodontics". International Journal of Dentistry 2009. doi:10.1155/2009/634567. ISSN 1687-8728. PMID 20379362.
- ↑ "Cone Beam-Computed Tomography in Endodontics". Summer 2011. https://www.aae.org/specialty/wp-content/uploads/sites/2/2017/07/ecfe-summer-11-final.pdf.
- ↑ New AAOMR Guidelines on CBCT Use in Implant Planning
- ↑ "Practical applications of cone-beam computed tomography in orthodontics". Journal of the American Dental Association 141 (Suppl 3): 7S–13S. October 2010. doi:10.14219/jada.archive.2010.0361. PMID 20884934. http://jada.ada.org/cgi/pmidlookup?view=long&pmid=20884934.
- ↑ Barg, Alexej; Bailey, Travis; Richter, Martinus; Netto, Cesar; Lintz, François; Burssens, Arne; Phisitkul, Phinit; Hanrahan, Christopher J. et al. (24 November 2017). "Weightbearing Computed Tomography of the Foot and Ankle: Emerging Technology Topical Review". Foot & Ankle International 39 (3): 376–386. doi:10.1177/1071100717740330. PMID 29171283.
- ↑ Tuominen, Esa K. J.; Kankare, Jussi; Koskinen, Seppo K.; Mattila, Kimmo T. (2013-01-01). "Weight-Bearing CT Imaging of the Lower Extremity". American Journal of Roentgenology 200 (1): 146–148. doi:10.2214/AJR.12.8481. ISSN 0361-803X. PMID 23255755.
- ↑ Colin, Fabrice; Horn Lang, Tamara; Zwicky, Lukas; Hintermann, Beat; Knupp, Markus (2014-07-11). "Subtalar Joint Configuration on Weightbearing CT Scan" (in en-US). Foot & Ankle International 35 (10): 1057–1062. doi:10.1177/1071100714540890. ISSN 1071-1007. PMID 25015393.
- ↑ Richter, Martinus; Seidl, Bernd; Zech, Stefan; Hahn, Sarah (September 2014). "PedCAT for 3D-imaging in standing position allows for more accurate bone position (angle) measurement than radiographs or CT". Foot and Ankle Surgery 20 (3): 201–207. doi:10.1016/j.fas.2014.04.004. ISSN 1268-7731. PMID 25103709.
- ↑ Lintz, François; Welck, Matthew; Bernasconi, Alessio; Thornton, James; Cullen, Nicholas P.; Singh, Dishan; Goldberg, Andy (2017-02-09). "3D Biometrics for Hindfoot Alignment Using Weightbearing CT" (in en-US). Foot & Ankle International 38 (6): 684–689. doi:10.1177/1071100717690806. ISSN 1071-1007. PMID 28183212. https://discovery.ucl.ac.uk/id/eprint/1544650/.
- ↑ Sterzing, Florian; Engenhart-Cabillic, Rita; Flentje, Michael; Debus, Jürgen (22 April 2011). "Image-Guided Radiotherapy". Deutsches Ärzteblatt Online 108 (16): 274–280. doi:10.3238/arztebl.2011.0274. PMID 21603562.
- ↑ O'Neill, Angela G M; Jain, Suneil; Hounsell, Alan R; O'Sullivan, Joe M (December 2016). "Fiducial marker guided prostate radiotherapy: a review". The British Journal of Radiology 89 (1068). doi:10.1259/bjr.20160296. PMID 27585736.
- ↑ 29.0 29.1 "Three-dimensional C-arm cone-beam CT: applications in the interventional suite". Journal of Vascular and Interventional Radiology 19 (6): 799–813. June 2008. doi:10.1016/j.jvir.2008.02.018. PMID 18503893.
- ↑ "Utility of cone-beam CT imaging in prostatic artery embolization". Journal of Vascular and Interventional Radiology 24 (11): 1603–7. November 2013. doi:10.1016/j.jvir.2013.06.024. PMID 23978461.
- ↑ "Adjunctive use of C-arm CT may eliminate technical failure in adrenal vein sampling". Journal of Vascular and Interventional Radiology 18 (9): 1102–5. September 2007. doi:10.1016/j.jvir.2007.06.018. PMID 17804771.
- ↑ "Increased cell opening and prolapse of struts of a neuroform stent in curved vasculature: value of angiographic computed tomography: technical case report". Neurosurgery 58 (4 Suppl 2): ONS–E380; discussion ONS–E380. April 2006. doi:10.1227/01.NEU.0000205287.06739.E1. PMID 16575290.
- ↑ "C-arm cone-beam CT-guided percutaneous transthoracic needle biopsy of small (≤ 20 mm) lung nodules: diagnostic accuracy and complications in 161 patients". American Journal of Roentgenology 199 (3): W322–30. September 2012. doi:10.2214/AJR.11.7576. PMID 22915422.
- ↑ B. N., Ha; T. K., Tuan; T. N., Toan; T. T., Duong; T. M., Anh; B. T., Hung; M. D., Thuy (2021-12-30). "Research and manufacture of cone-beam computed tomography (CBCT) system for industrial use". Nuclear Science and Technology 11 (4): 41–50. doi:10.53747/nst.v11i4.393. ISSN 1810-5408. http://jnst.vn/index.php/nst/article/view/393.
- ↑ Feldkamp, L. A.; Davis, L. C.; Kress, J. W. (1984-06-01). "Practical cone-beam algorithm" (in EN). JOSA A 1 (6): 612–619. doi:10.1364/JOSAA.1.000612. ISSN 1520-8532. Bibcode: 1984JOSAA...1..612F. https://www.osapublishing.org/josaa/abstract.cfm?uri=josaa-1-6-612.
- ↑ Health, Center for Devices and Radiological (28 September 2020). "Medical X-ray Imaging - Dental Cone-beam Computed Tomography". https://www.fda.gov/Radiation-EmittingProducts/RadiationEmittingProductsandProcedures/MedicalImaging/MedicalX-Rays/ucm315011.htm.
- ↑ "Radiation doses and risks of CBCT - SEDENTEXCT". http://www.sedentexct.eu/content/radiation-doses-and-risks-cbct.
- ↑ "Radiation dose of cone-beam computed tomography compared to conventional radiographs in orthodontics". Journal of Orofacial Orthopedics 77 (1): 9–15. January 2016. doi:10.1007/s00056-015-0002-4. PMID 26747662.
- ↑ "Dosimetry of a cone-beam computed tomography machine compared with a digital x-ray machine in orthodontic imaging". American Journal of Orthodontics and Dentofacial Orthopedics 141 (4): 436–43. April 2012. doi:10.1016/j.ajodo.2011.10.024. PMID 22464525.
- ↑ Yeh, Jih-Kuei; Chen, Chia-Hui (2018-08-03). "Estimated radiation risk of cancer from dental cone-beam computed tomography imaging in orthodontics patients". BMC Oral Health 18 (1): 131. doi:10.1186/s12903-018-0592-5. ISSN 1472-6831. PMID 30075771.
- ↑ "Use of Cone-Beam Computed Tomography in Endodontics". 2010. https://www.aaomr.org/assets/Journal_Publications/Position_Papers/aaomr-aae_position_paper_cb.pdf.
- ↑ "Justification of medical exposures". https://www.who.int/ionizing_radiation/medical_radiation_exposure/justification/en/.
- ↑ 43.0 43.1 "Cone-beam computerized tomography (CBCT) imaging of the oral and maxillofacial region: a systematic review of the literature". International Journal of Oral and Maxillofacial Surgery 38 (6): 609–25. June 2009. doi:10.1016/j.ijom.2009.02.028. PMID 19464146.
- ↑ 44.0 44.1 "Three-dimensional cephalometry: spiral multi-slice vs cone-beam computed tomography". American Journal of Orthodontics and Dentofacial Orthopedics 130 (3): 410–6. September 2006. doi:10.1016/j.ajodo.2005.11.035. PMID 16979502.
- ↑ Armstrong RT (2006). "Acceptability of cone beam ct vs. multi-detector CT for 3D Anatomic model construction". Journal of Oral and Maxillofacial Surgery 64 (9): 37. doi:10.1016/j.joms.2006.06.086.
- ↑ "A clinician's guide to understanding cone beam volumetric imaging (CBVI)". INeedCE. 2007. http://www.ineedce.com/courses/1413/PDF/A_Clin_Gde_ConeBeam.pdf.
- ↑ Ganz SD (December 2005). "Conventional CT and cone beam CT for improved dental diagnostics and implant planning". Dental Implantology Update 16 (12): 89–95. PMID 16422471.
- ↑ "Bone density assessments of dental implant sites: 3. Bone quality evaluation during osteotomy and implant placement". The International Journal of Oral & Maxillofacial Implants 22 (2): 208–12. 2007. PMID 17465345.
- ↑ "Image artifact in dental cone-beam CT". Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics 101 (5): 652–7. May 2006. doi:10.1016/j.tripleo.2005.07.027. PMID 16632279.
- ↑ "Bone classification: an objective scale of bone density using the computerized tomography scan". Clinical Oral Implants Research 12 (1): 79–84. February 2001. doi:10.1034/j.1600-0501.2001.012001079.x. PMID 11168274.
- ↑ 51.0 51.1 "Deriving Hounsfield units using grey levels in cone beam computed tomography". Dentomaxillofacial Radiology 39 (6): 323–35. September 2010. doi:10.1259/dmfr/19603304. PMID 20729181. See also this linear method adapted to different machines (in PMID 29076750 & citations); and a comparatively unusual neural network approach (in PMID 34301984 & citations).
- ↑ Vannier MW (2003). "Craniofacial computed tomography scanning: technology, applications and future trends". Orthodontics & Craniofacial Research 6 (Suppl 1): 23–30; discussion 179–82. doi:10.1034/j.1600-0544.2003.232.x. PMID 14606531.
Further reading
- Gupta R, Cheung AC, Bartling SH (2008). "Flat-panel volume CT: fundamental principles, technology, and applications". Radiographics 28: 2009–22. doi:10.1148/rg.287085004. PMID 19001655.
- Gupta R, Grasruck M, Suess C (June 2006). "Ultra-high resolution flat-panel volume CT: fundamental principles, design architecture, and system characterization". Eur Radiol 16: 1191–205. doi:10.1007/s00330-006-0156-y. PMID 16528556.
 |
![Axial image obtained from the first Cone-Beam 3D Scan performed on July 1, 1994[6]](/wiki/images/thumb/6/63/Prima_Immagine_Cone-Beam-1994-07-01_-1.jpg/79px-Prima_Immagine_Cone-Beam-1994-07-01_-1.jpg)








