Medicine:Foodborne illness: Difference between revisions
Importwiki (talk | contribs) (import) |
No edit summary |
||
| Line 2: | Line 2: | ||
{{Use mdy dates|date=February 2015}} | {{Use mdy dates|date=February 2015}} | ||
{{Food safety}} | {{Food safety}} | ||
'''Foodborne illness''' (also known as '''foodborne disease''' and '''food poisoning''')<ref> | '''Foodborne illness''' (also known as '''foodborne disease''' and '''food poisoning''')<ref> | ||
{{DorlandsDict|nine/000952820|food poisoning}} | {{DorlandsDict|nine/000952820|food poisoning}} | ||
Latest revision as of 17:19, 29 July 2024
| Food safety |
|---|
 |
| Terms |
| Critical factors |
| Bacterial pathogens |
| Viral pathogens |
| Parasitic pathogens |
Foodborne illness (also known as foodborne disease and food poisoning)[1] is any illness resulting from the contamination of food by pathogenic bacteria, viruses, or parasites,[2] as well as prions (the agents of mad cow disease), and toxins such as aflatoxins in peanuts, poisonous mushrooms, and various species of beans that have not been boiled for at least 10 minutes.
Symptoms vary depending on the cause. They often include vomiting, fever, and aches, and may include diarrhea. Bouts of vomiting can be repeated with an extended delay in between. This is because even if infected food was eliminated from the stomach in the first bout, microbes, like bacteria (if applicable), can pass through the stomach into the intestine and begin to multiply. Some types of microbes stay in the intestine.
For contaminants requiring an incubation period, symptoms may not manifest for hours to days, depending on the cause and on the quantity of consumption. Longer incubation periods tend to cause those affected to not associate the symptoms with the item consumed, so they may misattribute the symptoms to gastroenteritis, for example.
Causes
Foodborne illness usually arises from improper handling, preparation, or food storage. Good hygiene practices before, during, and after food preparation can reduce the chances of contracting an illness. There is a consensus in the public health community that regular hand-washing is one of the most effective defenses against the spread of foodborne illness. The action of monitoring food to ensure that it will not cause foodborne illness is known as food safety. Foodborne disease can also be caused by a large variety of toxins that affect the environment.[3]
Furthermore, foodborne illness can be caused by a number of chemicals, such as pesticides, medicines, and natural toxic substances such as vomitoxin, poisonous mushrooms or reef fish.[4]
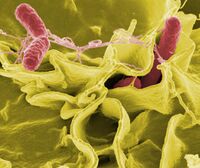
Bacteria
Bacteria are a common cause of foodborne illness. In 2000, the United Kingdom reported the individual bacteria involved as the following: Campylobacter jejuni 77.3%, Salmonella 20.9%, Escherichia coli O157:H7 1.4%, and all others less than 0.56%.[5]
In the past, bacterial infections were thought to be more prevalent because few places had the capability to test for norovirus and no active surveillance was being done for this particular agent. Toxins from bacterial infections are delayed because the bacteria need time to multiply. As a result, symptoms associated with intoxication are usually not seen until 12–72 hours or more after eating contaminated food. However, in some cases, such as Staphylococcal food poisoning, the onset of illness can be as soon as 30 minutes after ingesting contaminated food.[6]
A 2022 study concluded that washing uncooked chicken could increase the risk of pathogen transfer, and that specific washing conditions can decrease the risk of transfer.[7][8]
Most common bacterial foodborne pathogens are:
- Campylobacter jejuni which can lead to secondary Guillain–Barré syndrome and periodontitis[9]
- Clostridium perfringens, the "cafeteria germ"[10][11]
- Salmonella spp. – its S. typhimurium infection is caused by consumption of eggs or poultry that are not adequately cooked or by other interactive human-animal pathogens[12][13][14]
- Medicine:Escherichia coli O157:H7 enterohemorrhagic (EHEC) which can cause hemolytic-uremic syndrome
Other common bacterial foodborne pathogens are:[15]
- Bacillus cereus
- Escherichia coli, other virulence properties, such as enteroinvasive (EIEC), enteropathogenic (EPEC), enterotoxigenic (ETEC), enteroaggregative (EAEC or EAgEC)
- Listeria monocytogenes
- Shigella spp.
- Staphylococcus aureus
- Streptococcus
- Vibrio cholerae, including O1 and non-O1
- Vibrio parahaemolyticus
- Vibrio vulnificus
- Yersinia enterocolitica and Yersinia pseudotuberculosis
- Brucella spp.
- Corynebacterium ulcerans
- Coxiella burnetii or Q fever
- Plesiomonas shigelloides
Enterotoxins
In addition to disease caused by direct bacterial infection, some foodborne illnesses are caused by enterotoxins (exotoxins targeting the intestines). Enterotoxins can produce illness even when the microbes that produced them have been killed. Symptom onset varies with the toxin but may be rapid in onset, as in the case of enterotoxins of Staphylococcus aureus in which symptoms appear in one to six hours.[16] This causes intense vomiting including or not including diarrhea (resulting in staphylococcal enteritis), and staphylococcal enterotoxins (most commonly staphylococcal enterotoxin A but also including staphylococcal enterotoxin B) are the most commonly reported enterotoxins although cases of poisoning are likely underestimated.[17] It occurs mainly in cooked and processed foods due to competition with other biota in raw foods, and humans are the main cause of contamination as a substantial percentage of humans are persistent carriers of S. aureus.[17] The CDC has estimated about 240,000 cases per year in the United States.[18]
The rare but potentially deadly disease botulism occurs when the anaerobic bacterium Clostridium botulinum grows in improperly canned low-acid foods and produces botulin, a powerful paralytic toxin.[citation needed]
Emerging foodborne pathogens
- Aeromonas hydrophila, Aeromonas caviae, Aeromonas sobria
Scandinavian outbreaks of Yersinia enterocolitica have recently increased to an annual basis, connected to the non-canonical contamination of pre-washed salad.[19]
Preventing bacterial food poisoning

Goverments have the primary mandate of ensuring safe food for all, however all actors in the food chain are responsible to ensure only safe food reaches the consumer, thus preventing foodborne illnesses. This is achieved through the implementation of strict hygiene rules and a public veterinary and phytosanitary service that monitors animal products throughout the food chain, from farming to delivery in shops and restaurants. This regulation includes:
- traceability: the origin of the ingredients (farm of origin, identification of the crop or animal) and where and when it has been processed must be known in the final product; in this way, the origin of the disease can be traced and resolved (and possibly penalized), and the final products can be removed from sale if a problem is detected;
- enforcement of hygiene procedures such as HACCP and the "cold chain";
- power of control and of law enforcement of veterinarians.
In August 2006, the United States Food and Drug Administration approved phage therapy which involves spraying meat with viruses that infect bacteria, and thus preventing infection. This has raised concerns because without mandatory labeling, consumers would not know that meat and poultry products have been treated with the spray.[20]
At home, prevention mainly consists of good food safety practices. Many forms of bacterial poisoning can be prevented by cooking food sufficiently, and either eating it quickly or refrigerating it effectively.[2] Many toxins, however, are not destroyed by heat treatment.
Techniques that help prevent food borne illness in the kitchen are hand washing, rinsing produce,[21] preventing cross-contamination, proper storage, and maintaining cooking temperatures. In general, freezing or refrigerating prevents virtually all bacteria from growing, and heating food sufficiently kills parasites, viruses, and most bacteria. Bacteria grow most rapidly at the range of temperatures between 40 and 140 °F (4 and 60 °C), called the "danger zone". Storing food below or above the "danger zone" can effectively limit the production of toxins. For storing leftovers, the food must be put in shallow containers for quick cooling and must be refrigerated within two hours. When food is reheated, it must reach an internal temperature of 165 °F (74 °C) or until hot or steaming to kill bacteria.[22]
Mycotoxins and alimentary mycotoxicoses
The term alimentary mycotoxicosis refers to the effect of poisoning by mycotoxins through food consumption. The term mycotoxin is usually reserved for the toxic chemical compounds naturally produced by fungi that readily colonize crops under given temperature and moisture conditions. Mycotoxins can have important effects on human and animal health. For example, an outbreak which occurred in the UK during 1960 caused the death of 100,000 turkeys which had consumed aflatoxin-contaminated peanut meal. In the USSR in World War II, 5,000 people died due to alimentary toxic aleukia (ALA).[23]. In Kenya, mycotoxins led to the death of 125 people in 2004, after consumption of contaminated grains.[24] In animals, mycotoxicosis targets organ systems such as liver and digestive system. Other effects can include reduced productivity and suppression of the immune system, thus pre-disposing the animals to other secondary infections.[25] The common foodborne Mycotoxins include:
- Aflatoxins – originating from Aspergillus parasiticus and Aspergillus flavus. They are frequently found in tree nuts, peanuts, maize, sorghum and other oilseeds, including corn and cottonseeds. The pronounced forms of aflatoxins are those of B1, B2, G1, and G2, amongst which Aflatoxin B1 predominantly targets the liver, which will result in necrosis, cirrhosis, and carcinoma. Other forms of aflatoxins exist as metabolites such as Aflatoxin M1.[26][27] In the US, the acceptable level of total aflatoxins in foods is less than 20 μg/kg, except for Aflatoxin M1 in milk, which should be less than 0.5 μg/kg The official document can be found at FDA's website.[28][29] The European union has more stringent standards, set at 10 μg/kg in cereals and cereal products. These references are also adopted in other countries.[30][31]
- Altertoxins – are those of alternariol (AOH), alternariol methyl ether (AME), altenuene (ALT), altertoxin-1 (ATX-1), tenuazonic acid (TeA), and radicinin (RAD), originating from Alternaria spp. Some of the toxins can be present in sorghum, ragi, wheat and tomatoes.[32][33][34] Some research has shown that the toxins can be easily cross-contaminated between grain commodities, suggesting that manufacturing and storage of grain commodities is a critical practice.[35]
- Citrinin
- Citreoviridin
- Cyclopiazonic acid
- Cytochalasins
- Ergot alkaloids / ergopeptine alkaloids – ergotamine
- Fumonisins – Crop corn can be easily contaminated by the fungi Fusarium moniliforme, and its fumonisin B1 will cause leukoencephalomalacia (LEM) in horses, pulmonary edema syndrome (PES) in pigs, liver cancer in rats and esophageal cancer in humans.[36][37] For human and animal health, both the FDA and the EC have regulated the content levels of toxins in food and animal feed.[38][39]
- Fusaric acid
- Fusarochromanone
- Kojic acid
- Lolitrem alkaloids
- Moniliformin
- 3-Nitropropionic acid
- Nivalenol
- Ochratoxins – In Australia, The Limit of Reporting (LOR) level for ochratoxin A (OTA) analyses in 20th Australian Total Diet Survey was 1 μg/kg,[40] whereas the EC restricts the content of OTA to 5 μg/kg in cereal commodities, 3 μg/kg in processed products and 10 μg/kg in dried vine fruits.[41]
- Oosporeine
- Patulin – Currently, this toxin has been advisably regulated on fruit products. The EC and the FDA have limited it to under 50 μg/kg for fruit juice and fruit nectar, while limits of 25 μg/kg for solid-contained fruit products and 10 μg/kg for baby foods were specified by the EC.[41][42]
- Phomopsins
- Sporidesmin A
- Sterigmatocystin
- Tremorgenic mycotoxins – Five of them have been reported to be associated with molds found in fermented meats. These are fumitremorgen B, paxilline, penitrem A, verrucosidin, and verruculogen.[43]
- Trichothecenes – sourced from Cephalosporium, Fusarium, Myrothecium, Stachybotrys, and Trichoderma. The toxins are usually found in molded maize, wheat, corn, peanuts and rice, or animal feed of hay and straw.[44][45] Four trichothecenes, T-2 toxin, HT-2 toxin, diacetoxyscirpenol (DAS), and deoxynivalenol (DON) have been most commonly encountered by humans and animals. The consequences of oral intake of, or dermal exposure to, the toxins will result in alimentary toxic aleukia, neutropenia, aplastic anemia, thrombocytopenia and/or skin irritation.[46][47][48] In 1993, the FDA issued a document for the content limits of DON in food and animal feed at an advisory level.[49] In 2003, US published a patent that is very promising for farmers to produce a trichothecene-resistant crop.[50]
- Zearalenone
- Zearalenols
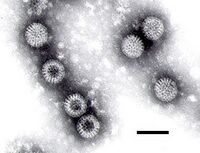
Viruses
- Enterovirus
- Hepatitis A is distinguished from other viral causes by its prolonged (2–6 week) incubation period and its ability to spread beyond the stomach and intestines into the liver. It often results in jaundice, or yellowing of the skin, but rarely leads to chronic liver dysfunction. The virus has been found to cause infection due to the consumption of fresh-cut produce which has fecal contamination.[51][52]
- Hepatitis E
- Norovirus
- Rotavirus
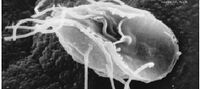
Parasites
Most foodborne parasites are zoonoses.[53]
- Diphyllobothrium sp.
- Nanophyetus sp.
- Taenia saginata
- Taenia solium
- Fasciola hepatica
- See also: Tapeworm and Flatworm
- Nematode:[54]
- Anisakis sp.
- Ascaris lumbricoides
- Eustrongylides sp.
- Toxocara
- Trichinella spiralis
- Trichuris trichiura
- Acanthamoeba and other free-living amoebae
- Cryptosporidiosis
- Cyclospora cayetanensis
- Entamoeba histolytica
- Giardia lamblia
- Sarcocystis hominis
- Sarcocystis suihominis
- Toxoplasma
Natural toxins
- Alkaloids
- Ciguatera poisoning
- Grayanotoxin (honey intoxication)
- Hormones from the thyroid glands of slaughtered animals (especially triiodothyronine in cases of hamburger thyrotoxicosis or alimentary thyrotoxicosis)[55][56][57][58][59][60]
- Mushroom toxins
- Phytohaemagglutinin (red kidney bean poisoning; destroyed by boiling)
- Pyrrolizidine alkaloids
- Shellfish toxin, including paralytic shellfish poisoning, diarrhetic shellfish poisoning, neurotoxic shellfish poisoning, amnesic shellfish poisoning and ciguatera fish poisoning
- Scombrotoxin
- Solanine (green potato poisoning)
- Tetrodotoxin (fugu fish poisoning)
Some plants contain substances which are toxic in large doses, but have therapeutic properties in appropriate dosages.
- Foxglove contains cardiac glycosides.
Other pathogenic agents
- Prions, resulting in Creutzfeldt–Jakob disease (CJD) and its variant (vCJD)
"Ptomaine poisoning" misconception
Ptomaine poisoning was a myth that persisted in the public consciousness, in newspaper headlines, and legal cases as an official diagnosis, decades after it had been scientifically disproven in the 1910s.[61]
In the 19th century, the Italian chemist Francesco Selmi, of Bologna, introduced the generic name ptomaine (from Greek ptōma, "fall, fallen body, corpse") for alkaloids found in decaying animal and vegetable matter, especially (as reflected in their names) putrescine and cadaverine.[62] The 1892 Merck's Bulletin stated, "We name such products of bacterial origin ptomaines; and the special alkaloid produced by the comma bacillus is variously named Cadaverine, Putrescine, etc."[63] While The Lancet stated, "The chemical ferments produced in the system, the... ptomaines which may exercise so disastrous an influence."[64] It is now known that the "disastrous... influence" is due to the direct action of bacteria and only slightly due to the alkaloids. Thus, the use of the phrase "ptomaine poisoning" is now largely obsolete.[citation needed]
At a Communist political convention in Massillon, Ohio,[65] and aboard a cruise ship in Washington, D.C., tainted potato salad sickened hundreds in separate incidents during a single week in 1932, drawing national attention to the dangers of so-called "ptomaine poisoning" in the pages of the American news weekly, Time.[66] In 1944, another newspaper article reported that over 150 people in Chicago were hospitalized with ptomaine poisoning, apparently from rice pudding served by a restaurant chain.[67]
Mechanism
Incubation period
The delay between the consumption of contaminated food and the appearance of the first symptoms of illness is called the incubation period. This ranges from hours to days (and rarely months or even years, such as in the case of listeriosis or bovine spongiform encephalopathy), depending on the agent, and on how much was consumed. If symptoms occur within one to six hours after eating the food, it suggests that it is caused by a bacterial toxin or a chemical rather than live bacteria.[citation needed]
The long incubation period of many foodborne illnesses tends to cause those affected to attribute their symptoms to gastroenteritis.[68]
During the incubation period, microbes pass through the stomach into the intestine, attach to the cells lining the intestinal walls, and begin to multiply there. Some types of microbes stay in the intestine, some produce a toxin that is absorbed into the bloodstream, and some can directly invade the deeper body tissues. The symptoms produced depend on the type of microbe.[69]
Infectious dose
The infectious dose is the amount of agent that must be consumed to give rise to symptoms of foodborne illness, and varies according to the agent and the consumer's age and overall health. Pathogens vary in minimum infectious dose; for example, Shigella sonnei has a low estimated minimum dose of < 500 colony-forming units (CFU) while Staphylococcus aureus has a relatively high estimate.[70]
In the case of Salmonella a relatively large inoculum of 1 million to 1 billion organisms is necessary to produce symptoms in healthy human volunteers,[71] as Salmonellae are very sensitive to acid. An unusually high stomach pH level (low acidity) greatly reduces the number of bacteria required to cause symptoms by a factor of between 10 and 100.[citation needed]
Gut microbiota unaccustomed to endemic organisms
Foodborne illness often occurs as travelers' diarrhea in persons whose gut microbiota is unaccustomed to organisms endemic to the visited region. This effect of microbiologic naïveté is compounded by any food safety lapses in the food's preparation.[citation needed]
Epidemiology
Asymptomatic subclinical infection may help spread these diseases, particularly Staphylococcus aureus, Campylobacter, Salmonella, Shigella, Enterobacter, Vibrio cholerae, and Yersinia.[70] For example, as of 1984 it was estimated that in the United States, 200,000 people were asymptomatic carriers of Salmonella.[70]
Infants
Globally, infants are a group that is especially vulnerable to foodborne disease. The World Health Organization has issued recommendations for the preparation, use and storage of prepared formulas. Breastfeeding remains the best preventive measure for protection from foodborne infections in infants.[72]
United States
A CDC report[73] for the period 2017–2019 found that 41% of outbreaks at restaurants were caused by a sick employee. Contributory factors identified included lack of written policy compliance with FDA recommendations for identifying red-flag symptoms, glove use, and hand washing; lack of paid sick leave at the majority of establishments; and social pressure to come to work even while sick.[74] The remaining outbreaks had a variety of causes, including inadequate cooking, improper temperature, and cross-contamination[citation needed].
In the United States, using FoodNet data from 2000 to 2007, the CDC estimated there were 47.8 million foodborne illnesses per year (16,000 cases for 100,000 inhabitants)[75] with 9.4 million of these caused by 31 known identified pathogens.[76]
- 127,839 were hospitalized (43 per 100,000 inhabitants per year).[77][78][79]
- 3,037 people died (1.0 per 100,000 inhabitants per year).[78][79]
|
|
United Kingdom
According to a 2012 report from the Food Standards Agency, there were around a million cases of foodborne illness per year (1,580 cases for 100,000 inhabitants).[80]
- 20,000 were hospitalized (32 per 100,000 inhabitants);[80][81]
- 500 people died (0.80 per 100,000 inhabitants).[80][81]
France
This data pertains to reported medical cases of 23 specific pathogens in the 1990s, as opposed to total population estimates of all foodborne illness for the United States.[82]
In France, for 735,590 to 769,615 cases of infection identified as being with the 23 specific pathogens, 238,836 to 269,085 were estimated to have been contracted from food:
- between 12,995 and 22,030 people were hospitalized (10,188 to 17,771 estimated to have contracted their infections from food);
- between 306 and 797 people died (228 to 691 estimated to have contracted their infections from food).[82]
|
|
Australia
A study by the Australian National University published in 2022 for Food Standards Australia New Zealand estimated there are 4.67 million cases of food poisoning in Australia each year that result in 47,900 hospitalisations, 38 deaths and a cost to the economy of $2.1 billion.[84]
A previous study using different methodology and published in November 2014, found in 2010 that there were an estimated 4.1 million cases of foodborne gastroenteritis acquired in Australia on average each year, along with 5,140 cases of non-gastrointestinal illness.[85]
This study replaces a previous estimate of 5.4 million cases of foodborne illness in Australia every year, causing:[86]
- 18,000 hospitalizations
- 120 deaths (0.5 deaths per 100,000 inhabitants)
- 2.1 million lost days off work
- 1.2 million doctor consultations
- 300,000 prescriptions for antibiotics.
Most foodborne disease outbreaks in Australia have been linked to raw or minimally cooked eggs or poultry.[87] The Australian Food Safety Information Council estimates that one third of cases of food poisoning occur in the home.[88]
Outbreaks
Society and culture
United Kingdom
In postwar Aberdeen (1964) a large-scale (>400 cases) outbreak of typhoid occurred, caused by contaminated corned beef which had been imported from Argentina.Cite error: Closing </ref> missing for <ref> tag and the bovine spongiform encephalopathy (BSE, mad cow disease) outbreak identified in the 1980s. The death of 21 people in the 1996 Wishaw outbreak of E. coli O157[89][90] was a precursor to the establishment of the Food Standards Agency which, according to Tony Blair in the 1998 white paper A Force for Change Cm 3830, "would be powerful, open and dedicated to the interests of consumers".[91]
In May 2015, for the second year running, England's Food Standards Agency devoted its annual Food Safety Week to "The Chicken Challenge". The focus was on the handling of raw chicken in the home and in catering facilities in a drive to reduce the high levels of food poisoning from the campylobacter bacterium. Anne Hardy argues that widespread public education of food hygiene can be useful, particularly through media (TV cookery programmes) and advertisement. She points to the examples set by Scandinavian societies.[92]
United States
In 2001, the Center for Science in the Public Interest petitioned the United States Department of Agriculture to require meat packers to remove spinal cords before processing cattle carcasses for human consumption, a measure designed to lessen the risk of infection by variant Creutzfeldt–Jakob disease. The petition was supported by the American Public Health Association, the Consumer Federation of America, the Government Accountability Project, the National Consumers League, and Safe Tables Our Priority.[93]
None of the US Department of Health and Human Services targets[94] regarding incidence of foodborne infections were reached in 2007.[95]
A report issued in June 2018 by NBC's Minneapolis station using research by both the CDC and the Minnesota Department of Health concluded that foodborne illness is on the rise in the U.S.[96]
India
In India, Entamoeba is the most common cause of food illness, followed by Campylobacter bacteria, Salmonella bacteria, E. coli bacteria, and norovirus.[97] According to statistics, food poisoning was the second most common cause of infectious disease outbreak in India in 2017. The numbers of outbreaks have increased from 50 in 2008 to 242 in 2017. [97]
Organizations
International Food Safety Authorities Network (INFOSAN)
- Promoting the rapid exchange of information during food safety events;
- Sharing information on important food safety issues of global interest;
- Promoting partnership and collaboration between countries; and
- Helping countries strengthen their capacity to manage food safety risks.
Prioritisation of foodborne pathogens
The Food and Agriculture Organization of the United Nations and The World Health Organization have published a global ranking of foodborne parasites using a multicriteria ranking tool concluding that Taenia solium was the most relevant, followed by Echinococcus granulosus, Echinococcus multilocularis, and Toxoplasma gondii.[98] The same method was used regionally to rank the most important foodborne parasites in Europe ranking Echinococcus multilocularis of highest relevance, followed by Toxoplasma gondii and Trichinella spiralis.[99]
Regulatory steps
- European Commission Regulation (EC) No 2073/2005 of November 15, 2005
- European Committee for Standardization (CEN): Standard method for the detection of norovirus and hepatitis A virus in food products (shellfish, fruits and vegetables, surfaces and bottled water)
- CODEX Committee on Food Hygiene (CCFH): Guideline for the application of general principles of food hygiene for the control of viruses in food[100]
See also
- American Public Health Association v. Butz
- Food allergy
- Food microbiology
- Food quality
- Food safety
- Food spoilage
- Food testing strips
- Gastroenteritis
- List of foodborne illness outbreaks by country
- List of food contamination incidents
- Mycotoxicology
- STOP Foodborne Illness
- United States Disease Control and Prevention
- Zoonotic pathogens
References
![]() This article incorporates public domain material from websites or documents of the Centers for Disease Control and Prevention.
This article incorporates public domain material from websites or documents of the Centers for Disease Control and Prevention.
- ↑ "food poisoning" at Dorland's Medical Dictionary
- ↑ 2.0 2.1 "Foodborne Illness - Frequently Asked Questions". US Centers for Disease Control and Prevention. https://www.cdc.gov/ncidod/dbmd/diseaseinfo/foodborneinfections_g.htm.
- ↑ For foodborne illness caused by chemicals, see Food contaminants.
- ↑ "Chemicals, Metals & Pesticides in Food". 2021. https://www.fda.gov/food/chemicals-metals-pesticides-food.
- ↑ "Reducing the risk from E. coli 0157 – controlling cross-contamination". Food Standards Agency, United Kingdom. February 2011. http://food.gov.uk/enforcement/regulation/betregs/ria/ria2011/controllingecoliia2011.
- ↑ "Staphylococcal Food Poisoning". U.S. Centers for Disease Control and Prevention. https://www.cdc.gov/foodsafety/diseases/staphylococcal.html.
- ↑ Chemistry, University of; Prague, Technology. "Chickensplash! Exploring the health concerns of washing raw chicken" (in en). https://phys.org/news/2022-09-chickensplash-exploring-health-raw-chicken.html.
- ↑ "Chickensplash! Exploring the health concerns of washing raw chicken". Physics of Fluids 34 (3): 031910. March 2022. doi:10.1063/5.0083979. PMID 35392485. Bibcode: 2022PhFl...34c1910C.
- ↑ "Campylobacters as zoonotic pathogens: a food production perspective". International Journal of Food Microbiology 117 (3): 237–257. July 2007. doi:10.1016/j.ijfoodmicro.2007.01.006. PMID 17368847.
- ↑ "Foodborne Illness: What Consumers Need to Know". USDA.gov. http://www.fsis.usda.gov/wps/portal/fsis/topics/food-safety-education/get-answers/food-safety-fact-sheets/foodborne-illness-and-disease/foodborne-illness-what-consumers-need-to-know/CT_Index.
- ↑ "Phylogenomic analysis of gastroenteritis-associated Clostridium perfringens in England and Wales over a 7-year period indicates distribution of clonal toxigenic strains in multiple outbreaks and extensive involvement of enterotoxin-encoding (CPE) plasmids". Microbial Genomics 5 (10): e000297. October 2019. doi:10.1099/mgen.0.000297. PMID 31553300.
- ↑ "An outbreak of Salmonella typhimurium phage type 135 infection linked to the consumption of raw shell eggs in an aged care facility". Communicable Diseases Intelligence Quarterly Report 26 (1): 38–39. 2002. PMID 11950200. https://www.health.gov.au/internet/main/publishing.nsf/Content/cda-pubs-cdi-2002-cdi2601-cdi2601h.htm.
- ↑ "Salmonella Infection (salmonellosis) and Animals". Centers for Disease Control and Prevention. https://www.cdc.gov/healthypets/diseases/salmonellosis.htm.
- ↑ "Reducing the carriage of foodborne pathogens in livestock and poultry". Poultry Science 85 (6): 960–973. June 2006. doi:10.1093/ps/85.6.960. PMID 16776463.
- ↑ CDC (March 18, 2020). "Foodborne Germs and Illnesses". https://www.cdc.gov/foodsafety/foodborne-germs.html.
- ↑ Food poisoning: Causes. Mayo Clinic.
- ↑ 17.0 17.1 "Food poisoning and Staphylococcus aureus enterotoxins". Toxins 2 (7): 1751–1773. July 2010. doi:10.3390/toxins2071751. PMID 22069659.
- ↑ Staphylococcus aureus: A Problem When Food Is Left Out Too Long. Ohio State University Extension HYG-5564-11].
- ↑ "Molecular Characterization of Multidrug-Resistant Yersinia enterocolitica From Foodborne Outbreaks in Sweden". Frontiers in Microbiology 12: 664665. 2021-05-13. doi:10.3389/fmicb.2021.664665. PMID 34054769.
- ↑ "FDA Says Viruses Safe for Treating Meat". https://www.forbes.com/business/healthcare/feeds/ap/2006/08/18/ap2959720.html.
- ↑ DeRusha, Jason (2010-11-09). "Good Question: Does Washing Fruit Do Anything?". http://minnesota.cbslocal.com/2010/11/09/good-question-does-washing-fruit-do-anything/.
- ↑ How Temperatures Affect Food. U.D. Department of Agriculture
- ↑ Mount, Michael. "Fungi and Mycotoxins". vetmed.ucdavis.edu. http://www.vetmed.ucdavis.edu/PHR/PHR250/2007/25007Myc.pdf.
- ↑ "Outbreak of Aflatoxin Poisoning --- Eastern and Central Provinces, Kenya, January--July 2004". https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5334a4.htm.
- ↑ Kępińska-Pacelik, Jagoda; Biel, Wioletta (2021). "Mycotoxins—Prevention, Detection, Impact on Animal Health". Processes 9 (11): 2035. doi:10.3390/pr9112035.
- ↑ "Aflatoxins". Center for Food Safety & Applied Nutrition. https://www.fda.gov/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/ucm071020.htm.
- ↑ "GASGA Technical Leaflet – 3 Mycotoxins in Grain". Food and Agriculture Organization of the United Nations. http://www.fao.org/Wairdocs/X5008E/X5008e01.htm.
- ↑ "Sec. 683.100 Action Levels for Aflatoxins in Animal Feeds (CPG 7126.33)". Food and Drug Administration. https://www.fda.gov/ora/compliance_ref/cpg/cpgvet/cpg683-100.html.
- ↑ Henry, Michael H.. "Mycotoxins in Feeds: CVM's Perspective". FDA.gov. https://www.fda.gov/AnimalVeterinary/Products/AnimalFoodFeeds/Contaminants/ucm050974.htm.
- ↑ "Aflatoxins (Sum of B1, B2, G1, G2) in cereals and cereal-derived food products". EFSA Supporting Publications 10 (3). 2013. doi:10.2903/sp.efsa.2013.EN-406.
- ↑ "Chapter 2 Foodborne Hazards in Basic Food Safety for Health Workers". World Health Organization. https://www.who.int/entity/foodsafety/publications/capacity/en/2.pdf.
- ↑ "Alternaria toxins in weather-damaged wheat and sorghum in the 1995–1996 Australian harvest". Australian Journal of Agricultural Research 48 (8): 1249–56. 1997. doi:10.1071/A97005.
- ↑ "Alternaria mycotoxins in weathered wheat from China". Journal of Agricultural and Food Chemistry 48 (7): 2920–2924. July 2000. doi:10.1021/jf0000171. PMID 10898645.
- ↑ "Survey of Brazilian tomato products for alternariol, alternariol monomethyl ether, tenuazonic acid and cyclopiazonic acid". Food Additives and Contaminants 18 (7): 630–634. July 2001. doi:10.1080/02652030117707. PMID 11469319.
- ↑ "Production of alternaria mycotoxins by Alternaria alternata isolated from weather-damaged wheat". Journal of Food Protection 64 (4): 567–571. April 2001. doi:10.4315/0362-028X-64.4.567. PMID 11307900.
- ↑ "Fumonisins: their implications for human and animal health". Natural Toxins 3 (4): 193–8; discussion 221. 1995. doi:10.1002/nt.2620030405. PMID 7582616.
- ↑ "Occurrence of fumonisins in foods". Food Research International 37 (10): 985–1000. 2004. doi:10.1016/j.foodres.2004.06.009.
- ↑ "CVM and Fumonisins". Food and Drug Administration. https://www.fda.gov/cvm/fumonisin.htm.
- ↑ "More contaminated maize meal products withdrawn from sale". Food Standards Agency. http://www.food.gov.uk/news/newsarchive/2003/sep/moremaize.
- ↑ "20th Australian Total Diet Survey – Part B". Food Standards Australia New Zealand. http://www.foodstandards.gov.au/newsroom/publications/20thaustraliantotaldietsurveyjanuary2003/20thaustraliantotaldietsurveyfullreport/partb20thatds/partbmetals.cfm.
- ↑ 41.0 41.1 "Worldwide regulations for mycotoxins in food and feed in 2003". FAO FOOD AND NUTRITION PAPER 81. http://www.fao.org/docrep/007/y5499e/y5499e0f.htm.
- ↑ "Patulin in Apple Juice, Apple Juice Concentrates and Apple Juice Products". Food and Drug Administration. http://vm.cfsan.fda.gov/~dms/patubckg.html.
- ↑ "Genotoxicity assessment of five tremorgenic mycotoxins (fumitremorgen B, paxilline, penitrem A, verruculogen, and verrucosidin) produced by molds isolated from fermented meats". Journal of Food Protection 66 (11): 2123–2129. November 2003. doi:10.4315/0362-028X-66.11.2123. PMID 14627292.
- ↑ "Occurrence of Fusarium species and trichothecenes in Nigerian maize". International Journal of Food Microbiology 116 (3): 350–357. May 2007. doi:10.1016/j.ijfoodmicro.2007.02.009. PMID 17412440.
- ↑ "Spectrum of noninfectious health effects from molds". Pediatrics 118 (6): e1909–e1926. December 2006. doi:10.1542/peds.2006-2829. PMID 17142508.
- ↑ "Trichothecene toxicity on human megakaryocyte progenitors (CFU-MK)". Human & Experimental Toxicology 20 (2): 84–89. February 2001. doi:10.1191/096032701677428611. PMID 11327514. Bibcode: 2001HETox..20...84F.
- ↑ "Comparative study of the yield of T-2 toxic produced by Fusarium poae, F. sporotrichioides and F. sporotrichioides var. tricinctum strains from different sources". Mycopathologia 60 (2): 93–97. February 1977. doi:10.1007/bf00490378. PMID 846559.
- ↑ "Fusarium infections of the skin". Current Opinion in Infectious Diseases 20 (2): 115–117. April 2007. doi:10.1097/QCO.0b013e328014392d. PMID 17496567.
- ↑ "Guidance for Industry and FDA – Letter to State Agricultural Directors, State Feed Control Officials, and Food, Feed, and Grain Trade Organizations". Food and Drug Administration. http://www.cfsan.fda.gov/~dms/graingui.html.
- ↑ Hohn, Thomas M. "Trichothecene-resistant transgenic plants". U.S. Patent 6,646,184. Priority date March 31, 1999.
- ↑ "Intra-laboratory validation of a concentration method adapted for the enumeration of infectious F-specific RNA coliphage, enterovirus, and hepatitis A virus from inoculated leaves of salad vegetables". International Journal of Food Microbiology 108 (2): 164–171. April 2006. doi:10.1016/j.ijfoodmicro.2005.11.007. PMID 16387377.
- ↑ Schmidt HM (2004). Improving the microbiological quality and safety of fresh-cut tomatoes by low dose electron beam irradiation (MS thesis). Texas A&M University. hdl:1969.1/2767. Retrieved December 14, 2022.
- ↑ "Zoonotic foodborne parasites and their surveillance". Revue Scientifique et Technique 32 (2): 559–569. August 2013. doi:10.20506/rst.32.2.2239. PMID 24547659.
- ↑ Britannica (2021). "Nematode". https://www.britannica.com/animal/nematode.
- ↑ "An unusual cause of epidemic thyrotoxicosis". Acta Clinica Belgica 72 (6): 451–453. December 2017. doi:10.1080/17843286.2017.1309336. PMID 28361645.
- ↑ "An outbreak of thyrotoxicosis caused by the consumption of bovine thyroid gland in ground beef". The New England Journal of Medicine 316 (16): 993–998. April 1987. doi:10.1056/NEJM198704163161605. PMID 3561455.
- ↑ "Recurrent hamburger thyrotoxicosis". CMAJ 169 (5): 415–417. September 2003. PMID 12952802.
- ↑ "Exogenous thyrotoxicosis in dogs attributable to consumption of all-meat commercial dog food or treats containing excessive thyroid hormone: 14 cases (2008-2013)". Journal of the American Veterinary Medical Association 246 (1): 105–111. January 2015. doi:10.2460/javma.246.1.105. PMID 25517332.
- ↑ "Hyperthyroidism caused by excessive consumption of sausages". The Netherlands Journal of Medicine 68 (3): 135–137. March 2010. PMID 20308711.
- ↑ "Community outbreak of thyrotoxicosis: epidemiology, immunogenetic characteristics, and long-term outcome". The American Journal of Medicine 84 (1): 10–18. January 1988. doi:10.1016/0002-9343(88)90002-2. PMID 3257352.
- ↑ "The Ptomaine-Poisoning Myth". The Spectator. 1934-05-25. http://archive.spectator.co.uk/article/25th-may-1934/9/the-ptomaine-poisoning-myth.
- ↑ Oxford English Dictionary (First ed.). London: Oxford University Press. 1933. p. 1557.
- ↑ Merck's Bulletin, Volume 5, William Henry Porter, 1892.
- ↑ Lancet, 3 Oct 1891, page 752
- ↑ "Report Next Week," Evening Independent (Massillon, OH), July 22, 1932, pg. 6
- ↑ "Medicine: Potato Salad," Time, August 1, 1932.
- ↑ "Poisoning Hits 150 in Chicago". Kenosha Evening News. May 27, 1944. http://ken.stparchive.com/Archive/KEN/KEN05271944p01.php.
- ↑ "Incubation periods of viral gastroenteritis: a systematic review". BMC Infectious Diseases 13: 446. September 2013. doi:10.1186/1471-2334-13-446. PMID 24066865.
- ↑ "Food-Related Diseases". US Centers for Disease Control and Prevention. 2018-03-29. https://www.cdc.gov/ncidod/diseases/food/index.htm.
- ↑ 70.0 70.1 70.2 "Infective Doses and Pathogen Carriage". https://www.researchgate.net/publication/265305465.
- ↑ Owens, Michael D (January 2014) Salmonella Infection in Emergency Medicine. emedicine.com
- ↑ FAO/WHO (2006). "Enterobacter sakazakii and Salmonella in powdered infant formula". in World Health Organization. https://www.who.int/foodsafety/publications/mra10/en/.
- ↑ Foodborne Illness Outbreaks at Retail Food Establishments — National Environmental Assessment Reporting System, 25 State and Local Health Departments, 2017–2019
- ↑ Food poisoning often caused by sick restaurant workers, CDC says
- ↑ "Foodborne illness acquired in the United States--unspecified agents". Emerging Infectious Diseases 17 (1): 16–22. January 2011. doi:10.3201/eid1701.P21101. PMID 21192849.
- ↑ 76.0 76.1 76.2 "Foodborne illness acquired in the United States--major pathogens". Emerging Infectious Diseases 17 (1): 7–15. January 2011. doi:10.3201/eid1701.P11101. PMID 21192848.
- ↑ "Obama Proposes Single Overseer for Food Safety". The New York Times. February 20, 2015. https://www.nytimes.com/2015/02/21/us/obama-proposes-single-overseer-for-food-safety.html. "According to the C.D.C., an estimated 87 million Americans are sickened each year by contaminated food, 371,000 are hospitalized with food-related illness and 5,700 die from food-related disease"
- ↑ 78.0 78.1 Sabrina Tavernise (July 26, 2013). "F.D.A. Says Importers Must Audit Food Safety". The New York Times. https://www.nytimes.com/2013/07/27/health/fda-proposes-rules-to-ensure-safety-of-imported-food.html. "One in every six Americans becomes ill from eating contaminated food each year, Dr. Margaret A. Hamburg, F.D.A. commissioner, estimated. About 130,000 are hospitalized and 3,000 die."
- ↑ 79.0 79.1 Stephanie Strom (January 4, 2013). "F.D.A. Offers Sweeping Rules to Fight Food Contamination". The New York Times. https://www.nytimes.com/2013/01/05/business/fda-offers-rules-to-stop-food-contamination.html. "One in six Americans becomes ill from eating contaminated food each year, the government estimates; of those, roughly 130,000 are hospitalized and 3,000 die."
- ↑ 80.0 80.1 80.2 "Annual Report of the Chief Scientist 2012/13". Food Standards Agency. England. 2013. https://acss.food.gov.uk/sites/default/files/multimedia/pdfs/publication/cstar_2013.pdf.
- ↑ 81.0 81.1 Liebling, Alison; Maruna, Shadd; McAra, Lesley (2017) (in en). The Oxford Handbook of Criminology. Oxford University Press. pp. 290. ISBN 978-0-19-871944-1. https://books.google.com/books?id=iJjJDgAAQBAJ&pg=PA290.
- ↑ 82.0 82.1 82.2 "Report of the French sanitary agencies" (in fr). INVS/Afssa. http://www.invs.sante.fr/publications/2004/inf_origine_alimentaire/inf_origine_alimentaire.pdf.
- ↑ "Summary of Report of the French sanitary agencies" (in fr). INVS/Afssa. http://www.invs.sante.fr/publications/2004/inf_origine_alimentaire/grilleLecture.pdf.
- ↑ "The Annual Cost of Foodborne Illness in Australia Final Report September 2022". Australian National University. https://www.foodstandards.gov.au/publications/Documents/ANU%20Foodborne%20Disease%20Final%20Report.pdf.
- ↑ Kirk, Martyn (2014). "Foodborne Illness, Australia, Circa 2000 and Circa 2010". Emerging Infectious Diseases (Emerging Infectious Diseases v 20:11) 20 (11): 1857–1864. doi:10.3201/eid2011.131315. PMID 25340705.
- ↑ "Foodborne illness in Australia. Annual incidence circa 2000". OzFoodNet. p. 10. Archived from the original on 2014-01-25. https://webarchive.nla.gov.au/awa/20140125145815/http://ozfoodnet.gov.au/internet/ozfoodnet/publishing.nsf/Content/7BDEF9F8EC3835D9CA257165001AB31D/$File/foodborne_report.pdf.
- ↑ "Foodborne disease outbreaks in Australia 2001-2009". Food Australia 63 (12): 44–50. 2011.
- ↑ "Food Hygiene". https://www.bupa.com.au/health-and-wellness/health-information/healthy-living/nutrition/eating/doc/food-hygiene.
- ↑ "BBC News - Health - Sheriff criticises E. coli butcher". http://news.bbc.co.uk/1/hi/health/154107.stm.
- ↑ "Epidemiological investigation of the central Scotland outbreak of Escherichia coli O157 infection, November to December 1996". Epidemiology and Infection 126 (3): 335–341. June 2001. doi:10.1017/S0950268801005520. PMID 11467789.
- ↑ "The Food Standards Agency: A Force for Change". Food Standards Agency, United Kingdom. January 14, 1998. http://www.archive.official-documents.co.uk/document/maffdh/fsa/fsa.htm.
- ↑ Hardy, Anne (13 January 2016). "Food Poisoning: An On-going Saga". http://www.historyandpolicy.org/policy-papers/papers/food-poisoning-an-on-going-saga.
- ↑ "Meat Produced by Advanced Meat/Bone Separation Machinery and Meat Recovery (AMR) Systems". U.S. National Archive and Records Administration. 2004-01-12. https://www.federalregister.gov/articles/2004/01/12/04-626/meat-produced-by-advanced-meatbone-separation-machinery-and-meat-recovery-amr-systems#footnote-10.
- ↑ "Healthy People 2010 Home Page". http://www.healthypeople.gov.
- ↑ Centers for Disease Control Prevention (CDC) (April 2008). "Preliminary FoodNet data on the incidence of infection with pathogens transmitted commonly through food--10 states, 2007". MMWR. Morbidity and Mortality Weekly Report 57 (14): 366–370. PMID 18401330. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5714a2.htm.
- ↑ Severson, Gordon (June 15, 2018). "Why are we seeing so many food recalls?". KARE 11. https://www.kare11.com/article/news/why-are-we-seeing-so-many-food-recalls/89-564858966.
- ↑ 97.0 97.1 "Symptoms of food poisoning". The Times of India. ISSN 0971-8257. https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/how-fast-does-food-poisoning-set-in-what-are-the-symptoms-one-should-know/photostory/79493562.cms?picid=79493721.
- ↑ Multicriteria-based ranking for risk management of foodborne parasites. Microbiological Risk Assessment Series No. 23. FAO/WHO. 2014. ISBN 978-92-5-108199-0. http://www.fao.org/publications/card/en/c/ee07c6ae-b86c-4d5f-915c-94c93ded7d9e/.
- ↑ "Prioritisation of food-borne parasites in Europe, 2016". Euro Surveillance 23 (9). March 2018. doi:10.2807/1560-7917.ES.2018.23.9.17-00161. PMID 29510783.
- ↑ "Codex Committee on Food Hygiene (CCFH)", European Commission, Retrieved April 7, 2015
Further reading
Periodicals
- International Journal of Food Microbiology, ISSN 0168-1605, Elsevier
- Foodborne Pathogens and Disease, ISSN 1535-3141, Mary Ann Liebert, Inc.
- Mycopathologia, ISSN 1573-0832 (electronic), ISSN 0301-486X (paper), Springer
Books
- Hocking, Ailsa D.; Pitt, John I.; Samson, Robert A.; Thrane, Ulf (2005). Advances in Food Mycology. Springer. ISBN 978-0-387-28385-2. https://books.google.com/books?id=9xlIicZfQ5IC. ISBN:978-0-387-28391-3 (electronic).
- Hobbs, Betty C. (1993). Food Poisoning and Food Hygiene. 7. Edward Arnold. 167–70. doi:10.1093/oxfordjournals.bmb.a073825. ISBN 978-0-340-53740-4.
- Riemann, Hans P.; Cliver, Dean O. (2006). FoodBorne Infections and Intoxications. Academic Press. ISBN 978-0-12-588365-8. https://books.google.com/books?id=_OsZ9TcQTSsC&pg=PA485.
- Smith, James L. (2005). Fratamico, Pina M.; Bhunia, Arun K.; Smith, James L.. eds. Foodborne Pathogens: Microbiology And Molecular Biology. Horizon Scientific Press. ISBN 978-1-904455-00-4. https://books.google.com/books?id=-HNavPPs-JoC.
External links
- Foodborne diseases, emerging, WHO, Fact sheet N°124, revised January 2002
- Foodborne illness information pages , NSW Food Authority
- Food safety and foodborne illness, WHO, Fact sheet N°237, revised January 2002
- UK Health protection Agency
- US PulseNet
- Food poisoning from NHS Direct Online
- Food Safety Network hosted at the University of Guelph, Canada.
- Food Standard Agency website
Template:Concepts in infectious disease
 |