Medicine:Anemia
Anemia (also spelt anaemia in British English) is a blood disorder in which the blood has a reduced ability to carry oxygen. This can be due to a lower than normal number of red blood cells, a reduction in the amount of hemoglobin available for oxygen transport, or abnormalities in hemoglobin that impair its function.[1][2] The name is derived from grc ἀν- (an-) 'not', and αἷμα (haima) 'blood'.[3]
When anemia comes on slowly, the symptoms are often vague, such as tiredness, weakness, shortness of breath, headaches, and a reduced ability to exercise.[4] When anemia is acute, symptoms may include confusion, feeling like one is going to pass out, loss of consciousness, and increased thirst.[4] Anemia must be significant before a person becomes noticeably pale.[4] Additional symptoms may occur depending on the underlying cause.[4] Anemia can be temporary or long-term and can range from mild to severe.[5]
Anemia can be caused by blood loss, decreased red blood cell production, and increased red blood cell breakdown.[4] Causes of blood loss include menstruation, bleeding due to inflammation of the stomach or intestines, bleeding from surgery, serious injury, or blood donation.[4] Causes of decreased production include iron deficiency, folate deficiency, vitamin B12 deficiency, thalassemia and a number of bone marrow tumors.[4] Causes of increased breakdown include genetic disorders such as sickle cell anemia, infections such as malaria, and certain autoimmune diseases like autoimmune hemolytic anemia.[4]
Anemia can also be classified based on the size of the red blood cells and amount of hemoglobin in each cell.[4] If the cells are small, it is called microcytic anemia; if they are large, it is called macrocytic anemia; and if they are normal sized, it is called normocytic anemia.[4] The diagnosis of anemia in men is based on a hemoglobin of less than 130 g/L; in non-pregnant women, it is less than 120 g/L, while in pregnant women it is less than 105–110.[6][7] Further testing is then required to determine the cause.[4][8]
Treatment depends on the specific cause. Certain groups of individuals, such as pregnant women, can benefit from the use of iron pills for prevention.[4][9] Dietary supplementation, without determining the specific cause, is not recommended.[4] The use of blood transfusions is typically based on a person's signs and symptoms.[4] In those without symptoms, they are not recommended unless hemoglobin levels are less than 60 to 80 g/L (6 to 8 g/dL).[4][10] These recommendations may also apply to some people with acute bleeding.[4] Erythropoiesis-stimulating agents are only recommended in those with severe anemia.[10]
Anemia is the most common blood disorder, affecting about a fifth to a third of the global population.[4][11][12] Iron-deficiency anemia is the most common cause of anemia worldwide, and affects nearly one billion people.[13] In 2013, anemia due to iron deficiency resulted in about 183,000 deaths – down from 213,000 deaths in 1990.[14] This condition is most prevalent in children[15][16] with also an above average prevalence in elderly[4] and women of reproductive age (especially during pregnancy).[13] Women aged 15 to 49 years experienced an increase in the global prevalence from 27.6% to 30.7% between 2012 to 2023 with either no improvement or an increase in prevalence in nearly all regions.[17] Anemia is one of the six WHO global nutrition targets for 2025 and for diet-related global targets endorsed by World Health Assembly in 2012 and 2013. Efforts to reach global targets contribute to reaching Sustainable Development Goals (SDGs),[18] with anemia as one of the targets in SDG 2 for achieving zero world hunger.[19]
Signs and symptoms
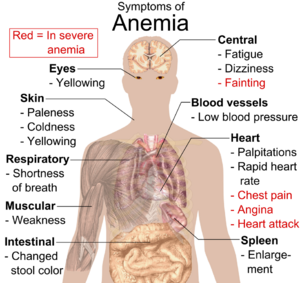
Symptoms of anemia can come on quickly or slowly.[21] If the anemia develops slowly (chronic), the body may adapt and compensate for this change up to a point. In this case, no symptoms may appear until the anemia becomes more severe.[20][22] General symptoms of mild anemia can include feeling tired, weak, dizziness, headaches, shortness of breath, and pale or yellowish skin.[22][23]
Acute anemia, often caused by blood loss (hemorrhagic shock) has more severe symptoms, including rapid heartbeat, low blood pressure,and confusion.[24]
The body may compensate for the lack of oxygen-carrying capability of the blood by increasing cardiac output. Symptoms related to this may include palpitations, angina (if pre-existing heart disease is present), difficulty walking, and symptoms of heart failure.[25] In severe anemia, there may be signs of a hyperdynamic circulation: tachycardia (a fast heart rate), bounding pulse, flow murmurs, and cardiac ventricular hypertrophy (enlargement).[24]
Chronic anemia in infants may result in poor growth and impaired neurological development.[26]
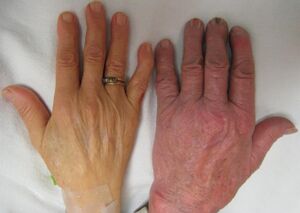
Pallor resulting from severe anemia may be visible in the hand palms and fingernails beds, although it may be difficult to detect in dark toned skin. Other locations to detect pallor are the inner lining of the lower eyelid and the tongue.[27][28][29]
Other symptoms associated with anemia depend on the underlying cause of the disorder; for example -
- Chronic iron-deficiency anemia may be associated with symptoms that can include spoon-shaped nails, sore or abnormally smooth tongue, hair loss, or pica (the desire to eat things which are not food, such as ice or earth).[30]
- Anemia caused by vitamin B12 deficiency may be associated with psychological problems such as anxiety and confusion, memory loss, and depression.[31]
Causes
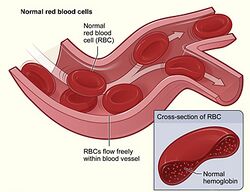
In humans, mature red blood cells (RBCs) are flexible biconcave disks, lacking cell nucleus and organelles. The process by which new RBCs are produced is termed erythropoiesis; committed stem cells in the red bone marrow of large bones take 7 days to mature into red blood cells. Between 2 and 3 million new RBCs are produced per second in human adults.[33] The functional lifetime of a RBC is about 100–120 days, during which time the cells are continually moving within the blood circulation.[34] The aging RBC undergoes changes in its plasma membrane, making it susceptible to recognition by macrophages and subsequent breakdown in the spleen, thus removing old and defective cells and continually purging the blood.[35] This process is termed eryptosis; much of the resulting breakdown products are recirculated in the body.[36] RBC breakdown by eryptosis normally occurs at the same rate as production by erythropoiesis, thus maintaining a balanced RBC population in the circulation.[37]
The causes of anemia may be classified as impaired red blood cell (RBC) production, increased RBC destruction (hemolytic anemia), blood loss, and fluid overload (hypervolemia).[38] Globally, the most common underlying cause of anemia is dietary iron deficiency, followed by the inherited conditions thalassaemia and sickle cell trait, and infectious disease (principally malaria).[28]
Impaired production
- Disturbance of proliferation and differentiation of stem cells
- Pure red cell aplasia[39]
- Aplastic anemia[39] affects all kinds of blood cells. Fanconi anemia is a hereditary disorder or defect featuring aplastic anemia and various other abnormalities, including malformation of the extremities.[40]
- Anemia of kidney failure[39] due to insufficient production of the hormone erythropoietin
- Anemia of endocrine disease[41]
- Disturbance of proliferation and maturation of erythroblasts
- Pernicious anemia[39] is a form of megaloblastic anemia due to vitamin B12 deficiency dependent on impaired absorption of vitamin B12. Lack of dietary B12 causes non-pernicious megaloblastic anemia.
- Iron-deficiency anemia, resulting in deficient heme synthesis[39]. In anemia among older patients, diet alone is rarely the issue; iron loss from the gastrointestinal tract, impaired absorption, chronic inflammation and kidney disease often coexist.[42] Excessive cow milk consumption is a common cause of iron deficiemcy anemia in young children.[43]
- Thalassemias, causing deficient globin synthesis[39]
- Other mechanisms of impaired RBC production
- Myelodysplastic syndrome[39]
- anemia of chronic inflammation[39]
- Leukoerythroblastic anemia is caused by space-occupying lesions in the bone marrow that prevent normal production of blood cells.[44]
- General Global contributors
- In many regions, nutritional deficiencies are major drivers of reduced RBC production. Poor intake of iron, folate, and vitamin B12 can significantly impair hemoglobin synthesis and erythropoiesis. This is especially common in low-income populations, areas with limited food diversity, and communities experiencing famine.[45]
- Pregnancy greatly increases iron requirements, and inadequate dietary intake during pregnancy is one of the leading causes of anemia among reproductive-age women worldwide.[45]
- Chronic infections common in developing countries, such as malaria and hookworm disease, impair erythropoiesis either through inflammatory suppression or recurrent blood loss leading to iron depletion.[45]
- Socioeconomic factors such as poverty, limited access to nutrient-rich foods, and high rates of parasitic exposure increase the risk of iron-deficiency anemia in women and children.[45]
- Anemia of chronic disease
- Chronic inflammatory conditions can inhibit iron mobilization and impair the bone marrow's ability to produce RBC count. This mechanism is a major cause of anemia in developed countries and frequently coexists with other types of anemia.[45]
Chronic inflammation can disrupt iron handling limiting its availability for red blood cell formation. During inflammatory states, the liver produces high levels of hepcidin, a hormone that blocks iron release from intestinal cells and macrophages. This leads to high ferritin levels and low transferrin saturation, a pattern known as "functional iron deficiency." This mechanism is commonly seen in older hospitalized patients with long-standing illnesses such as infections, heart failure or autoimmune conditions.[42]
Intestinal inflammation
Certain gastrointestinal disorders can cause anemia. The mechanisms involved are multifactorial and not limited to malabsorption but mainly related to chronic intestinal inflammation, which causes dysregulation of hepcidin that leads to decreased access of iron to the circulation.[46][47][48] Chronic intestinal inflammation increases hepcidin activity, which restricts iron release from storage sites. This mechanism limits iron availability even when total body iron stores are adequate, contributing to anemia common in inflammatory bowel diseases and chronic infections.[45]
- Helicobacter pylori infection.[49]
- Gluten-related disorders: untreated celiac disease[48][49] and non-celiac gluten sensitivity.[50] Anemia can be the only manifestation of celiac disease, in absence of gastrointestinal or any other symptoms.[51]
- Inflammatory bowel disease.[52][53]
Increased destruction
Anemias of increased red blood cell destruction are generally classified as hemolytic anemias. These types generally feature jaundice, and elevated levels of lactate dehydrogenase.[54][55]
- Intrinsic (intracorpuscular) abnormalities[39] cause premature destruction. All of these, except paroxysmal nocturnal hemoglobinuria, are hereditary genetic disorders.[56]
- Hereditary elliptocytosis[39] is another defect in membrane skeleton proteins.
- Enzyme deficiencies
- Hemoglobinopathies
- Paroxysmal nocturnal hemoglobinuria[39]
- Extrinsic (extracorpuscular) abnormalities
- Antibody-mediated
- Warm autoimmune hemolytic anemia is caused by an autoimmune attack against red blood cells, primarily by IgG. It is the most common of the autoimmune hemolytic diseases.[57] It can be idiopathic, that is, without any known cause, drug-associated or secondary to another disease such as systemic lupus erythematosus, or a malignancy, such as chronic lymphocytic leukemia.[58]
- Cold agglutinin hemolytic anemia is primarily mediated by IgM. It can be idiopathic[59] or result from an underlying condition. *** Rh disease,[39] one of the causes of hemolytic disease of the newborn
- Transfusion reaction to blood transfusions[39]
- Mechanical trauma to red blood cells
- Microangiopathic hemolytic anemias, including thrombotic thrombocytopenic purpura and disseminated intravascular coagulation[39]
- Infections, including malaria[39]
- Heart surgery
- Haemodialysis
- Parasitic
- Trypanosoma congolense alters the surfaces of RBCs of its host and this may explain T. c. induced anemia[60]
- Antibody-mediated
Blood loss
- Gastrointestinal tract lesions,[39] causing either acute bleeds (e.g. variceal lesions, peptic ulcers, hemorrhoids[61]) or chronic blood loss (e.g. angiodysplasia)
- Infection by intestinal nematodes feeding on blood, such as hookworms[62] and the whipworm Trichuris trichiura [63]
- Iatrogenic anemia, blood loss from repeated blood draws and medical procedures.[64][65]
- Chronic gastrointestinal blood loss due to hookworm infection is common among children in impoverished regions.[45]
- Repeated pregnancies, short birth intervals, and menstruation contribute to iron loss in women, especially in communities with limited dietary iron intake.[45]
- Persistent low-grade blood loss from parasitic infections, gynecologic conditions, and undiagnosed GI lesions cumulatively results in iron deficiency that may remain unrecognized until anemia becomes severe.[45]
The roots of the words anemia and ischemia both refer to the basic idea of "lack of blood", but anemia and ischemia are not the same thing in modern medical terminology. The word anemia used alone implies widespread effects from blood that either is too scarce (e.g., blood loss) or is dysfunctional in its oxygen-supplying ability (due to whatever type of hemoglobin or erythrocyte problem). In contrast, the word ischemia refers solely to the lack of blood (poor perfusion). Thus, ischemia in a body part can cause localized anemic effects within those tissues.[66]
Fluid overload
Fluid overload (hypervolemia) causes decreased hemoglobin concentration and apparent anemia:[67]
- General causes of hypervolemia include excessive sodium or fluid intake, sodium or water retention, and fluid shifts into the intravascular space.[68]
- From the sixth week of pregnancy, hormonal changes cause an increase in the mother's blood volume due to an increase in plasma.[69]
- During early pregnancy, plasma volume expands while red cell mass increases slowly. This physiological change results in a dilutional decrease in hemoglobin concentration and may mimic or worsen underlying nutritional anemia.[45]
Diagnosis
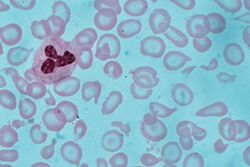
Definitions
There are several definitions of anemia.[70] A strict but broad definition is an absolute decrease in red blood cell mass,[71] however, a broader definition is a lowered ability of the blood to carry oxygen.[72] An operational definition is a decrease in whole-blood hemoglobin concentration of more than 2 standard deviations below the mean of an age- and sex-matched reference range.[73]
| Age or gender group | Hb threshold (g/L) |
|---|---|
| Children (0.5–2 yrs) | 105 |
| Children (2–5 yrs) | 110 |
| Children (5–12 yrs) | 115 |
| Teens (12–15 yrs) | 120 |
| Non-pregnant women (>15yrs) | 120 |
| Pregnant girls and women | 105–110 |
| Men (>15yrs) | 130 |
Testing
Anemia is typically diagnosed on a complete blood count from a blood sample. An automated hematology analyzer measures the hemoglobin level, hematocrit (% volume of RBCs in the blood), the size of the RBCs,[75] and counts of white blood cells and platelets.
Further tests will be needed to determine the underlying cause; these may include (not a complete list):[76][77]
- A count of reticulocytes (immature RBCs), which measures the capacity of the bone marrow to produce new RBCs.[78]
- Iron profile, to establish if there is underlying iron deficiency (the most common cause of anemia).[79]
- Family history and genetic testing, to establish if there is an inherited disorder (the second most common cause).[79]
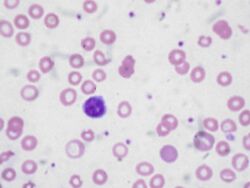
- Peripheral blood smear - a small blood sample is examined under a microscope to check the size and shape of RBCs. Among other things, this should detect malaria parasites, which are globally the third most common cause.[80][81]
- Serum creatinine, to check if poor kidney function underlies the anemia.[82]
Red blood cell size
In the morphological approach, anemia is classified by the size of red blood cells; this is either done automatically or on microscopic examination of a peripheral blood smear. The size is reflected in the mean corpuscular volume (MCV). If the cells are smaller than normal (under 80 fl), the anemia is said to be microcytic; if they are normal size (80–100 fl), normocytic; and if they are larger than normal (over 100 fl), the anemia is classified as macrocytic. This scheme quickly exposes some of the most common causes of anemia; for instance, a microcytic anemia is often the result of iron deficiency.[83]
In clinical workup, the MCV will be one of the first pieces of information available, so even among clinicians who consider the "kinetic" approach more useful philosophically, morphology will remain an important element of classification and diagnosis. Limitations of MCV include cases where the underlying cause is due to a combination of factors, such as iron deficiency (a cause of microcytosis) and vitamin B12 deficiency (a cause of macrocytosis), where the net result can be normocytic cells.
Production vs. destruction or loss
The "kinetic" approach to anemia yields arguably the most clinically relevant classification of anemia. This classification depends on the evaluation of several hematological parameters, particularly the blood reticulocyte (precursor of mature RBCs) count. This then yields the classification of defects by decreased RBC production versus increased RBC destruction or loss. Clinical signs of loss or destruction include abnormal peripheral blood smear with signs of hemolysis; elevated LDH suggesting cell destruction; or clinical signs of bleeding, such as guaiac-positive stool, radiographic findings, or frank bleeding. The following is a simplified schematic of this approach:
| Anemia | |||||||||||||||||||||||||||||||||
| Reticulocyte production index shows inadequate production response to anemia. | Reticulocyte production index shows appropriate response to anemia = ongoing hemolysis or blood loss without RBC production problem. | ||||||||||||||||||||||||||||||||
| No clinical findings consistent with hemolysis or blood loss: pure disorder of production. | Clinical findings and abnormal MCV: hemolysis or loss and chronic disorder of production*. | Clinical findings and normal MCV= acute hemolysis or loss without adequate time for bone marrow production to compensate**. | |||||||||||||||||||||||||||||||
| Macrocytic anemia (MCV>100) | Normocytic anemia (80<MCV<100) | Microcytic anemia (MCV<80) | |||||||||||||||||||||||||||||||
* For instance, sickle cell anemia with superimposed iron deficiency; chronic gastric bleeding with B12 and folate deficiency; and other instances of anemia with more than one cause.
** Confirm by repeating reticulocyte count: ongoing combination of low reticulocyte production index, normal MCV, and hemolysis or loss may be seen in bone marrow failure or anemia of chronic disease, with superimposed or related hemolysis or blood loss.
Here is a schematic representation of how to consider anemia with MCV as the starting point:
| Anemia | |||||||||||||||||||||||||||||||||||||||||||
| Macrocytic anemia (MCV>100) | Normocytic anemia (MCV 80–100) | Microcytic anemia (MCV<80) | |||||||||||||||||||||||||||||||||||||||||
| High reticulocyte count | Low reticulocyte count | ||||||||||||||||||||||||||||||||||||||||||
Microcytic
Microcytic anemia is primarily a result of hemoglobin synthesis failure/insufficiency, which could be caused by several etiologies:
- Heme synthesis defect
- Iron-deficiency anemia (microcytosis is not always present)
- Anemia of chronic disease (more commonly presenting as normocytic anemia)
- Globin synthesis defect
- Alpha-, and beta-thalassemia
- HbE syndrome
- HbC syndrome
- Various other unstable hemoglobin diseases
- Sideroblastic defect
- Hereditary sideroblastic anemia
- Acquired sideroblastic anemia, including lead toxicity[84]
- Reversible sideroblastic anemia
Iron-deficiency anemia is the most common type of anemia overall, and it has many causes. RBCs often appear hypochromic (paler than usual) and microcytic (smaller than usual) when viewed with a microscope.
- Iron-deficiency anemia is due to insufficient dietary intake or absorption of iron to meet the body's needs. Infants, toddlers, and pregnant women have higher-than-average needs. Increased iron intake is also needed to offset blood losses due to digestive tract issues, frequent blood donations, or heavy menstrual periods.[85] Iron is an essential part of hemoglobin, and low iron levels result in decreased incorporation of hemoglobin into red blood cells. In the United States, 12% of all women of childbearing age have iron deficiency, compared with only 2% of adult men. The incidence is as high as 20% among African American and Mexican American women.[86] In India it is even more than 50%.[87] Studies have linked iron deficiency without anemia to poor school performance and lower IQ in teenage girls, although this may be due to socioeconomic factors.[88][89] Iron deficiency is the most prevalent deficiency state on a worldwide basis. It is sometimes the cause of abnormal fissuring of the angular (corner) sections of the lips (angular stomatitis).
- In the United States, the most common cause of iron deficiency is bleeding or blood loss, usually from the gastrointestinal tract. Fecal occult blood testing, upper endoscopy and lower endoscopy should be performed to identify bleeding lesions. In older men and women, the chances are higher that bleeding from the gastrointestinal tract could be due to colon polyps or colorectal cancer.
- Worldwide, the most common cause of iron-deficiency anemia is parasitic infestation (hookworms, amebiasis, schistosomiasis and whipworms).[90]
The Mentzer index (mean cell volume divided by the RBC count) predicts whether microcytic anemia may be due to iron deficiency or thalassemia, although it requires confirmation.[91]
Macrocytic
- Megaloblastic anemia, the most common cause of macrocytic anemia, is due to a deficiency of either vitamin B12, folic acid, or both.[92] Deficiency in folate or vitamin B12 can be due either to inadequate intake or insufficient absorption. Folate deficiency normally does not produce neurological symptoms, while B12 deficiency does.
- Pernicious anemia is caused by a lack of intrinsic factor, which is required to absorb vitamin B12 from food. A lack of intrinsic factor may arise from an autoimmune condition targeting the parietal cells (atrophic gastritis) that produce intrinsic factor or against intrinsic factor itself. These lead to poor absorption of vitamin B12.
- Macrocytic anemia can also be caused by the removal of the functional portion of the stomach, such as during gastric bypass surgery, leading to reduced vitamin B12/folate absorption. Therefore, one must always be aware of anemia following this procedure.
- Hypothyroidism
- Alcoholism commonly causes a macrocytosis, although not specifically anemia. Other types of liver disease can also cause macrocytosis.
- Drugs such as methotrexate, zidovudine, and other substances may inhibit DNA replication such as heavy metals
Macrocytic anemia can be further divided into "megaloblastic anemia" or "nonmegaloblastic macrocytic anemia". The cause of megaloblastic anemia is primarily a failure of DNA synthesis with preserved RNA synthesis, which results in restricted cell division of the progenitor cells. The megaloblastic anemias often present with neutrophil hypersegmentation (six to 10 lobes). The nonmegaloblastic macrocytic anemias have different etiologies (i.e., unimpaired DNA globin synthesis), which occur, for example, with excessive alcohol use. In addition to the nonspecific symptoms of anemia, specific features of vitamin B12 deficiency include peripheral neuropathy and subacute combined degeneration of the cord with resulting balance difficulties from posterior column spinal cord pathology.[93] Other features may include a smooth, red tongue and glossitis. The treatment for vitamin B12-deficient anemia was first devised by William Murphy, who bled dogs to make them anemic, and then fed them various substances to see what (if anything) would make them healthy again. He discovered that ingesting large amounts of liver seemed to cure the disease. George Minot and George Whipple then set about to isolate the curative substance chemically and ultimately were able to isolate the vitamin B12 from the liver. All three shared the 1934 Nobel Prize in Medicine.[94]
Normocytic
Normocytic anemia occurs when the overall hemoglobin levels are decreased, but the red blood cell size (mean corpuscular volume) remains normal. Causes include:
- Acute blood loss
- Anemia of chronic disease
- Aplastic anemia (bone marrow failure)
- Hemolytic anemia
Dimorphic
A dimorphic appearance on a peripheral blood smear occurs when there are two simultaneous populations of red blood cells, typically of different size and hemoglobin content (this last feature affecting the color of the red blood cell on a stained peripheral blood smear). For example, a person recently transfused for iron deficiency would have small, pale, iron-deficient red blood cells (RBCs) and the donor RBCs of normal size and color. Similarly, a person transfused for severe folate or vitamin B12 deficiency would have two cell populations, but, in this case, the patient's RBCs would be larger and paler than the donor's RBCs.
Heinz body anemia
Heinz bodies form in the cytoplasm of RBCs and appear as small dark dots under the microscope. In animals, Heinz body anemia has many causes. It may be drug-induced, for example, in cats and dogs by acetaminophen (paracetamol),[95] or may be caused by eating various plants or other substances:
- In cats and dogs after eating either raw or cooked plants from the genus Allium, for example, onions or garlic.[96]
- In dogs after ingestion of zinc, for example, after eating U.S. pennies minted after 1982.[95]
- In horses which eat dry or wilted red maple leaves.[97]
Hyperanemia
Hyperanemia is a severe form of anemia, in which the hematocrit is below 10%.[98]
Refractory anemia
Refractory anemia, an anemia which does not respond to treatment,[99] is often seen secondary to myelodysplastic syndromes.[100] Iron-deficiency anemia may also be refractory as a manifestation of gastrointestinal problems which disrupt iron absorption or cause occult bleeding. [101]
Transfusion dependent
Transfusion-dependent anemia is a form of anemia where ongoing blood transfusions are required.[102] Most people with myelodysplastic syndrome develop this state at some point in time.[103] Beta thalassemia may also result in transfusion dependence.[104][105] Concerns from repeated blood transfusions include iron overload.[103] This iron overload may require chelation therapy.[106]
Treatment
In order to treat anemia, the underlying cause and its severity would first need to be identified[5]. Different causes and types of anemia mean there are different treatments. Drugs, for example, are used to treat iron-deficiency anemia, thalassemia, aplastic anemia, hemolytic anemia, sickle cell anemia, and pernicious anemia, with iron-deficiency and sickle cell anemia taking up 60% of market share due to having the highest prevalence as well as highest treatment costs.[107]
More specifically, iron supplements, antibiotics, immunosuppressants, bone marrow stimulants, corticosteroids, gene therapy, and iron chelating agents are forms of anemia treatment drugs, with immunosuppressants and corticosteroids accounting for 58% of the market share.[107] A paradigm shift towards gene therapy and monoclonal antibody therapies is observed.[107] Besides drugs, treatments include replenishing specific deficiencies that may be causing anemia.[5] Vitamin supplements given orally (folic acid or vitamin B12) or intramuscularly (vitamin B12) to replace specific deficiencies.[4] More invasive treatments include blood transfusions, blood or bone marrow transplantation, or even surgery.[2] Otherwise, oxygen may be given, and a dietary change is suggested.[5]
Oral Iron
Iron deficiency results in the decreased production of hemoglobin, the oxygen-carrying protein in red blood cells.[108] In developing nations, an estimated two-thirds of children and women of childbearing age (15-49) are estimated to have iron deficiency without anemia, with one-third of them having an iron deficiency with anemia.[109] Child-bearing women may not have access to certain medications or appropriate nutrition due to socioeconomic factors, which may affect the chances for developing anemia.[110] Iron deficiency due to inadequate dietary iron intake is rare in men and postmenopausal women. In some cases, the diagnosis of iron deficiency mandates a search for potential sources of blood loss, such as gastrointestinal bleeding from ulcers or colon cancer.[109]
Mild to moderate iron-deficiency anemia is treated by oral iron supplementation with ferrous sulfate, ferrous fumarate, or ferrous gluconate.[108] Daily iron supplements are effective in reducing anemia in women of childbearing age.[111] Because these iron supplements are taken orally, gastrointestinal side effects, including stomach upset, vomiting, or darkening of the feces, are commonly experienced.[108] The stomach upset can be alleviated by taking the iron with food; however, this decreases the amount of iron absorbed. Vitamin C aids in the body's ability to absorb iron, so taking oral iron supplements with orange juice is of benefit.[112]
In the anemia of chronic kidney disease, recombinant erythropoietin or epoetin alfa is recommended to stimulate RBC production, and if iron deficiency and inflammation are also present, concurrent parenteral iron is also recommended.[113]
Injectable Iron
In cases where oral iron has either proven ineffective, would be too slow (for example, pre-operatively), or where absorption is impeded (for example, in cases of inflammation), parenteral iron preparations can be used. Parenteral iron can improve iron stores rapidly and is also effective for treating people with postpartum haemorrhage, inflammatory bowel disease, and chronic heart failure.[114] The body can absorb up to 6 mg iron daily from the gastrointestinal tract. In many cases, the patient has a deficit of over 1,000 mg of iron, which would require several months to replace. This can be given concurrently with erythropoietin to ensure sufficient iron for increased rates of erythropoiesis.[115]
Injectable iron (iron supplement) is available both intravenously and intramuscularly, with IV treatment more common than IM as IM may have inconsistent absorption. Possible side effects of IV iron supplementation include infusion reactions and anaphylaxis, depending on the patient's conditions. Possible side effects of IM iron supplementation include site injection pain and stained skin.[108] Before an individual is given any iron supplements, an extensive workup is performed by a primary healthcare provider. Too much iron can be damaging, and intake is monitored.[108]
Blood transfusions

Blood transfusions work to replace blood lost in surgery, injury, or to make up for the blood the body isn't producing. More blood means more hemoglobin and oxygen being carried throughout the body. In this treatment, healthy blood, often voluntarily donated, is provided through an IV line connected to the blood vessels. The healthy blood, before being given, is carefully tested and handled, and further tests are conducted to confirm a match with the patient.[116]
Blood transfusions in those without symptoms is not recommended until the hemoglobin is below 60 to 80 g/L (6 to 8 g/dL).[4] In those with coronary artery disease who are not actively bleeding transfusions are only recommended when the hemoglobin is below 70 to 80g/L (7 to 8 g/dL).[10] Transfusing earlier does not improve survival.[117] Transfusions otherwise should only be undertaken in cases of cardiovascular instability.[118]
A 2012 review concluded that when considering blood transfusions for anaemia in people with advanced cancer who have fatigue and breathlessness (not related to cancer treatment or haemorrhage), consideration should be given to whether there are alternative strategies that can be tried before a blood transfusion.[119]
A blood transfusion is not without risk. During a blood transfusion, the patient is monitored during and after for any side effects. Even if the donor blood is tested, handled, and matched correctly, patients can still experience reactions ranging from mild (fevers) to severe (alloimmunization). Otherwise, there is a chance of getting too much iron from extensive transfusions and a very slim chance of getting an infectious disease (extensive testing is done).[116]
Bone marrow transplant

Bone marrow is the site for new red blood cell production, and if the bone marrow is unable to produce enough red blood cells, a transplant could be recommended. Aplastic anemia, for example, is the result of bone marrow failing to produce red blood cells.[120] In a bone marrow transplant, old defective bone marrow is destroyed using drugs or radiation and replaced with new stem cells. Before the transplant, like a blood transplant, the bone marrow must be carefully tested and must be compatible. Sometimes, the stem cells can come from the patient themselves (autologous), and other times, the cells will come from a donor (allogenic). The patient is monitored before, during, and after the transplant for any complications.[116]
A bone marrow transplant is an intensive therapy and comes with risks and possible complications. The treatment weakens the immune system and leaves the body weak against possible infections and bleeding, especially while the stem cells get settled and grow into bone marrow.[120] In other cases, there's the risk that the donated stem cells attack the body (graft-versus-host disease) or the patient's body rejects the donated stem cells. Additionally, the patient is likely to be put on medication that could have their own side effects, or experience side effects of the radiation and drugs used to destroy the old bone marrow.[116]
Vitamin B12 intramuscular injections
Pernicious anemia results from a lack of vitamin B12 absorbed. Vitamin B12 is supplemented via intramuscular injection in severe cases or cases of malabsorption of dietary-B12. Pernicious anemia caused by loss of intrinsic factor cannot be prevented.[121] If there are other, reversible causes of low vitamin B12 levels, the cause must be treated.[122]
Vitamin B12 deficiency anemia is usually easily treated by providing the necessary level of vitamin B12 supplementation.[123] The injections are quick-acting, and symptoms usually go away within one to two weeks.[123] As the condition improves, doses are reduced to weeks and then can be given monthly. Intramuscular therapy leads to more rapid improvement and should be considered in patients with severe deficiency or severe neurologic symptoms.[123] Treatment should begin rapidly for severe neurological symptoms, as some changes can become permanent.[124] In some individuals lifelong treatment may be needed.[124]
Erythropoiesis-stimulating agents
Erythropoiesis-stimulating agents (ESA) work to increase endogenous erythropoietin (EPO) production, a hormone that increases the production of red blood cells.[125] The objective for the administration of an ESA is to maintain hemoglobin at the lowest level that both minimizes transfusions and meets the person's needs.[126] They should not be used for mild or moderate anemia.[117] They are not recommended in people with chronic kidney disease unless hemoglobin levels are less than 10 g/dL or they have symptoms of anemia. Their use should be along with parenteral iron.[126][127]
The 2020 Cochrane Anaesthesia Review Group review of erythropoietin (EPO) plus iron versus control treatment including placebo or iron for preoperative anaemic adults undergoing non-cardiac surgery demonstrated that patients were much less likely to require red cell transfusion, and in those transfused, the volumes were unchanged (mean difference -0.09, 95% CI -0.23 to 0.05). Pre-operative hemoglobin concentration was increased in those receiving 'high dose' EPO, but not 'low dose'.[128]
The use of ESAs is heavily monitored by healthcare professionals as dosage and type vary among patients. A baseline for hemoglobin is set prior to treatment and continuously monitored throughout treatment. Risks involve reactions to the ESA and possible overdose if not carefully monitored.[125]
Hyperbaric oxygen
Treatment of exceptional blood loss (anemia) is recognized as an indication for hyperbaric oxygen (HBO) by the Undersea and Hyperbaric Medical Society.[129][130] HBO therapy involves being in a higher air pressure chamber filled with pure oxygen. Higher than normal air pressure means heavier breathing, and by supplying the room with pure oxygen, the body takes in more pure oxygen.[131]
The use of HBO is indicated when oxygen delivery to tissue is not sufficient in patients who cannot be given blood transfusions for medical or religious reasons. HBO may be used for medical reasons when the threat of blood product incompatibility or concern for transmissible disease are factors.[129] The beliefs of some religions (ex: Jehovah's Witnesses) may require they use the HBO method.[129] A 2005 review of the use of HBO in severe anemia found that all publications reported positive results.[132]
HBO does not often have lasting side effects. Any complications that arise are often mild and do not last. Ear pain or sinus pressure may arise with the higher air pressure. Serious complications, although very uncommon, can involve seizures from too much oxygen or collapsed lungs from too much pressure. As with many other treatments, the risk of complications increases the longer and the more repeats there are.[131]
Preoperative anemia
An estimated 30% of adults who require non-cardiac surgery have anemia.[133] To determine an appropriate preoperative treatment, it is suggested that the cause of anemia be first determined.[134] There is moderate level medical evidence that supports a combination of iron supplementation and erythropoietin treatment to help reduce the requirement for red blood cell transfusions after surgery in those who have preoperative anemia.[133]
Epidemiology
Anemia affects 24% of the world's population, with iron-deficiency anemia accounting for the majority of cases.[135] Approximately 9.3% of the world population have a moderate degree of anemia, and 0.9% have severe anemia.[136] The proportions of moderate-to-severe anaemia may be higher among hospitalised children in endemic areas.[137][138] Women and girls are more likely to be anemic with a prevalence of 31% compared to 17% for men and boys. The difference is starkest during reproductive years.[135] Women aged 15 to 49 years experienced an increase in the global prevalence from 27.6% to 30.7% between 2012 to 2023 with either no improvement or an increase in prevalence in nearly all regions.[17]
Age-related differences
Anemia is most frequent in older populations, affecting up to ~17% of a cohort of individuals above the age of 65 years old.[139] In neonates (0-6 days old), hemoglobinopathies are the primary contributor to disorders related to anemia, as newborns retain their iron stores they accumulated during pregnancy. As children grow, the causes and patterns of developing anemia shift. Anemia-related disability rate is especially high among children under 5 years old, with boys experiencing slightly higher rates, potentially due to biological differences in iron metabolism.[140]
Population groups at higher risk
Certain populations experience disproportionately higher rates of anemia. For example, African Americans have an elevated risk of developing anemia compared with other racial groups.[141] Severe anaemia is prevalent globally, and especially in sub-Saharan Africa[142] where it is associated with infections including malaria and invasive bacterial infections.[143][144] Children under 5 years old in low-income regions represent a high-risk population, although the age profile might be shifting with declining malaria prevalence in endemic areas[145]. In a survey of 96,804 children across 27 sub-Saharan African countries, nearly 60% were anemic (one of the highest regional burdens worldwide). Socioeconomic and maternal factors accounted for more than two-thirds of this burden, with children from crowded households or communities with inadequate sanitation facing substantially higher risk.[146] Pregnant women also carry an increased risk of developing anemia when infected with malaria.[147] Globally, the prevalence of anaemia in women aged 15 to 49 years increased from 28.5% in 2012 to 29.9% in 2019 and is projected to reach 32.3% by 2030, missing the Sustainable Development Goal target of a 50 percent reduction by 2030.[148]
History
Signs of severe anemia in human bones from 4000 years ago have been uncovered in Thailand.[149]
The first discovery and discussion of blood was in 1674 when Antoni van Leeuwenhoek described red blood cells (RBCs) as "small round globules." RBCs counterpart, hemoglobin, wasn't discovered until much later by FL Hünefeld in 1840. In 1746, Vincenzo Menghini showed that iron was concentrated in the red blood cells using a magnetic knife[150]. Between 1877-1885, many key tools emerged like hemocytometer (RBC count), hemoglobin measurement, and hematocrit measurement that allowed for quantitative diagnosis of blood[151]. By the 1920s it was confirmed by multiple different studies that iron existed in plasma. McCance and Widdowson showed that iron is not excreted from the body in 1938, and it was later confirmed that iron absorption is the main way the body regulates iron levels. Factors that increase absorption are anemia, hypoxia, and iron depletion, while factors that decrease absorption are transfusions and iron overload.
In ancient cultures, like Assyria and Mediterranean societies, used iron for medical treatments, however, this occurred before iron's biological role was understood. In the 1500s, Nicholas Monarde used iron's "healing powers" to treat gout, acne and hair loss[150]. Anemia started out as a clinical entity in 1807. Early diagnosis of anemia in the early 1800s were based solely on physical examinations such as fatigue, paleness, sweating, difficulty breathing, and dizziness. It wasn't until late in the 1800s when new technologies allowed for a more in depth, lab-based diagnosis on anemia. Also in the 17th and 18th century, water borne parasites may have contributed to the spread of iron deficiency anemia.[152] In 1939, anemia was officially defined as "a deficiency of blood not due to hemorrhage[151]." The term Chlorosis or "green disease" was used in the 17th century and referred to a disease that affected mostly adolescent females with the symptoms of paleness, headaches, loss of appetite, indigestion, and exhaustion. In the late 17th century, Thomas Sydenham advocated for the use of iron as treatment for the disease. The disease mysteriously disappeared, and it was determined that it was likely due to the change in American lifestyles in the early 20th century, such as diminished prejudice or eating meat and abandonment of tight lacing/corsets. The term can not be found in any hematology textbooks, but is generally understood that chlorosis was caused by iron deficiency[150].
References
- ↑ "Anemia: Practice Essentials, Pathophysiology, Etiology". 9 November 2021. https://emedicine.medscape.com/article/198475-overview.
- ↑ 2.0 2.1 "Anemia | NHLBI, NIH". https://www.nhlbi.nih.gov/health/anemia.
- ↑ "anaemia". http://dictionary.reference.com/browse/anaemia.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 Cite error: Invalid
<ref>tag; no text was provided for refs namedEBM2013 - ↑ 5.0 5.1 5.2 5.3 "Anemia – Symptoms and causes" (in en). https://www.mayoclinic.org/diseases-conditions/anemia/symptoms-causes/syc-20351360.
- ↑ "Guideline on haemoglobin cutoffs to define anaemia in individuals and populations". 2024. https://iris.who.int/server/api/core/bitstreams/f9f74397-1440-478d-a63c-26f29a01552f/content.
- ↑ National Institute for Care and Health Excellence (NICE) (October 2025). "Anaemia - iron deficiency". https://cks.nice.org.uk/topics/anaemia-iron-deficiency/.
- ↑ Rhodes, Carl E.; Denault, Deanna; Varacallo, Matthew (2024). "Physiology, Oxygen Transport". StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK538336/.
- ↑ "Evidence-based interventions for improvement of maternal and child nutrition: what can be done and at what cost?". Lancet 382 (9890): 452–477. August 2013. doi:10.1016/S0140-6736(13)60996-4. PMID 23746776. Bibcode: 2013Lanc..382..452B.
- ↑ 10.0 10.1 10.2 "Treatment of anemia in patients with heart disease: a clinical practice guideline from the American College of Physicians". Annals of Internal Medicine 159 (11): 770–779. December 2013. doi:10.7326/0003-4819-159-11-201312030-00009. PMID 24297193.
- ↑ Vos, Theo et al. (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMID 27733282.
- ↑ Peyrin-Biroulet, Laurent; Williet, Nicolas; Cacoub, Patrice (1 December 2015). "Guidelines on the diagnosis and treatment of iron deficiency across indications: a systematic review". The American Journal of Clinical Nutrition 102 (6): 1585–1594. doi:10.3945/ajcn.114.103366. PMID 26561626.
- ↑ 13.0 13.1 "Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet 380 (9859): 2163–2196. December 2012. doi:10.1016/S0140-6736(12)61729-2. PMID 23245607.
- ↑ ((GBD 2013 Mortality Causes of Death Collaborators)) (January 2015). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMID 25530442.
- ↑ "WHO Global Anaemia estimates, 2021 Edition". World Health Organization. https://www.who.int/data/gho/data/themes/topics/anaemia_in_women_and_children.
- ↑ Islam, Md Azmir Ibne (6 December 2021). "Modeling the impact of campaign program on the prevalence of anemia in children under five: Anemia model" (in en). Journal of Mathematical Analysis and Modeling 2 (3): 29–40. doi:10.48185/jmam.v2i3.362. ISSN 2709-5924. https://www.sabapub.com/index.php/jmam/article/view/362.
- ↑ 17.0 17.1 FAO; IFAD; UNICEF; WFP; WHO (2025) (in English). The State of Food Security and Nutrition in the World 2025. FAO ; IFAD ; UNICEF ; WFP ; WHO. doi:10.4060/cd6008en. ISBN 978-92-5-139937-8. https://openknowledge.fao.org/handle/20.500.14283/cd6008en.
- ↑ "WHO | Interventions by global target". World Health Organization. https://www.who.int/elena/global-targets/en/.
- ↑ "The case for action on anemia". Devex. 14 June 2016. https://www.devex.com/news/sponsored/the-case-for-action-on-anemia-leave-no-one-behind-88283.
- ↑ 20.0 20.1 "Anemia Types, Treatment, Symptoms, Signs, Causes & Iron Deficiency" (in en). https://www.emedicinehealth.com/anemia/article_em.htm.
- ↑ "What Are Symptoms of Anemia?". 2022-03-24. https://www.nhlbi.nih.gov/health/anemia/symptoms.
- ↑ 22.0 22.1 "Anemia" (in en). https://www.hematology.org:443/education/patients/anemia.
- ↑ "Anemia" (in en). https://www.yalemedicine.org/conditions/anemia.
- ↑ 24.0 24.1 Killeen, Robert B.; Kaur, Anahat; Afzal, Muriam (2026), "Acute Anemia", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 30725917, http://www.ncbi.nlm.nih.gov/books/NBK537232/, retrieved 2026-03-21
- ↑ De Franceschi, Lucia; Iolascon, Achille; Taher, Ali; Cappellini, Maria Domenica (July 2017). "Clinical management of iron deficiency anemia in adults: Systemic review on advances in diagnosis and treatment". European Journal of Internal Medicine 42: 16–23. doi:10.1016/j.ejim.2017.04.018. PMID 28528999.
- ↑ Gallagher, Patrick G. (2022-08-11). "Anemia in the pediatric patient" (in en). Blood 140 (6): 571–593. doi:10.1182/blood.2020006479. ISSN 0006-4971. PMID 35213686. PMC 9373018. https://ashpublications.org/blood/article/140/6/571/484178/Anemia-in-the-pediatric-patient.
- ↑ Ersianti, Yuninda Loviana; Susanah, Susi; Winarno, Gatot Nyarumenteng Adhipurnawan; Susiarno, Hadi; Herman, Herry; Krisnadi, Sofie Rifayani (2026). "Analysis of Pallor Examination for the Identification of Anemia Among Pregnant Women: A Scoping Review" (in English). International Journal of Women's Health 18: 1–12. doi:10.2147/IJWH.S550863. PMID 41835843.
- ↑ 28.0 28.1 "Anaemia" (in en). 10 February 2025. https://www.who.int/news-room/fact-sheets/detail/anaemia.
- ↑ "Identifying AEFI in diverse skin colour" (in en-AU). https://mvec.mcri.edu.au/references/identifying-aefi-in-diverse-skin-colour/.
- ↑ "Iron deficiency anaemia symptoms and treatments" (in en-GB). 21 February 2025. https://www.nhsinform.scot/illnesses-and-conditions/nutritional/iron-deficiency-anaemia/.
- ↑ "Vitamin B12 or folate deficiency anaemia" (in en). 20 February 2023. https://www.nhs.uk/conditions/vitamin-b12-or-folate-deficiency-anaemia/.
- ↑ "Sickle Cell Disease". 22 July 2022. https://www.nhlbi.nih.gov/health/sickle-cell-disease.
- ↑ Dean, Laura (2005), "Blood and the cells it contains" (in en), Blood Groups and Red Cell Antigens [Internet] (National Center for Biotechnology Information (US)), https://www.ncbi.nlm.nih.gov/books/NBK2263/, retrieved 2026-03-16
- ↑ "Red blood cell population dynamics". Clinics in Laboratory Medicine 35 (1): 43–57. March 2015. doi:10.1016/j.cll.2014.10.002. PMID 25676371.
- ↑ Lutz HU, Bogdanova A. Mechanisms tagging senescent red blood cells for clearance in healthy humans. Front Physiol. 2013;4:387
- ↑ "Erythrocyte programmed cell death". IUBMB Life 60 (10): 661–668. October 2008. doi:10.1002/iub.106. PMID 18720418.
- ↑ "Physiology and pathophysiology of eryptosis". Transfusion Medicine and Hemotherapy 39 (5): 308–314. October 2012. doi:10.1159/000342534. PMID 23801921.
- ↑ Amilia, Alifrangis (December 2022). "Anaemia: Symptoms, causes and treatment | Bupa UK" (in en-GB). https://www.bupa.co.uk/health-information/heart-blood-circulation/anaemia.
- ↑ 39.00 39.01 39.02 39.03 39.04 39.05 39.06 39.07 39.08 39.09 39.10 39.11 39.12 39.13 39.14 39.15 39.16 39.17 Table 12-1 in: Mitchell, Richard Sheppard; Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson (2007). Robbins Basic Pathology (8th ed.). Philadelphia: Saunders. ISBN 978-1-4160-2973-1.
- ↑ Bhandari, Jenish; Thada, Pawan K.; Killeen, Robert B.; Puckett, Yana (2024-06-19), "Fanconi Anemia" (in en), StatPearls [Internet] (StatPearls Publishing), PMID 32644559, https://www.ncbi.nlm.nih.gov/sites/books/NBK559133/, retrieved 2026-01-08
- ↑ Gregg, XT; Prchal, JT (2007). "Anemia of Endocrine Disorders". Williams Hermatology. McGraw-Hill.
- ↑ 42.0 42.1 Randi, Maria Luigia; Bertozzi, Irene; Santarossa, Claudia; Cosi, Elisabetta; Lucente, Fabrizio; Bogoni, Giulia; Biagetti, Giacomo; Fabris, Fabrizio (2020-03-30). "Prevalence and Causes of Anemia in Hospitalized Patients: Impact on Diseases Outcome" (in en). Journal of Clinical Medicine 9 (4): 950. doi:10.3390/jcm9040950. ISSN 2077-0383. PMID 32235484.
- ↑ Warner, Matthew J.; Kamran, Muhammad T. (2023-08-07), "Iron Deficiency Anemia" (in en), StatPearls [Internet] (StatPearls Publishing), PMID 28846348, https://www.ncbi.nlm.nih.gov/books/NBK448065/, retrieved 2026-01-08
- ↑ "the definition of leukoerythroblastosis" (in en). https://www.dictionary.com/browse/leukoerythroblastosis.
- ↑ 45.00 45.01 45.02 45.03 45.04 45.05 45.06 45.07 45.08 45.09 Dugdale, Marion (2001-06-01). "ANEMIA". Obstetrics and Gynecology Clinics of North America 28 (2): 363–382. doi:10.1016/S0889-8545(05)70206-0. ISSN 0889-8545. PMID 11430182. https://www.sciencedirect.com/science/article/pii/S0889854505702060.
- ↑ "Iron and inflammation – the gut reaction". Metallomics 9 (2): 101–111. February 2017. doi:10.1039/c6mt00282j. PMID 28067386.
- ↑ "Anemia in inflammatory bowel disease: a neglected issue with relevant effects". World Journal of Gastroenterology 20 (13): 3542–3551. April 2014. doi:10.3748/wjg.v20.i13.3542. PMID 24707137.
- ↑ 48.0 48.1 Leffler, Daniel A.; Green, Peter H. R.; Fasano, Alessio (October 2015). "Extraintestinal manifestations of coeliac disease". Nature Reviews Gastroenterology & Hepatology 12 (10): 561–571. doi:10.1038/nrgastro.2015.131. PMID 26260366.
- ↑ 49.0 49.1 "Anemia and iron deficiency in gastrointestinal and liver conditions". World Journal of Gastroenterology 22 (35): 7908–7925. September 2016. doi:10.3748/wjg.v22.i35.7908. PMID 27672287.
- ↑ "Non-Celiac Gluten sensitivity: the new frontier of gluten related disorders". Nutrients 5 (10): 3839–3853. September 2013. doi:10.3390/nu5103839. PMID 24077239.
- ↑ James, Stephen P. (April 2005). "National Institutes of Health Consensus Development Conference statement on Celiac Disease, June 28–30, 2004". Gastroenterology 128 (4): S1–S9. doi:10.1053/j.gastro.2005.02.007. PMID 15825115.
- ↑ "Dietary and nutritional considerations for inflammatory bowel disease". The Proceedings of the Nutrition Society 70 (3): 329–335. August 2011. doi:10.1017/S0029665111000097. PMID 21450124.
- ↑ "The aetiology and impact of malnutrition in paediatric inflammatory bowel disease". Journal of Human Nutrition and Dietetics 24 (4): 313–326. August 2011. doi:10.1111/j.1365-277X.2011.01171.x. PMID 21564345.
- ↑ Despotovic, J; Mahoney, D; Armsby, C (2021). "Overview of hemolytic anemias in children". UpToDate. https://www.lecturio.com/concepts/anemia-overview/.
- ↑ Capriotti, Theresa; Frizzell, Joan Parker (2016). Pathophysiology: introductory concepts and clinical perspectives. Philadelphia: F.A. Davis Company. ISBN 978-0-8036-1571-7. OCLC 900626405.
- ↑ Mitchell, Richard Sheppard; Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson (2007). Robbins Basic Pathology (8th ed.). Philadelphia: Saunders. p. 432. ISBN 978-1-4160-2973-1.
- ↑ Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease. St. Louis, Mo: Elsevier Saunders. p. 637. ISBN 978-0-7216-0187-8.
- ↑ "Autoimmune Hemolytic Anemia (AIHA)" By J.L. Jenkins. The Regional Cancer Center. 2001
- ↑ "Primary chronic cold agglutinin disease: an update on pathogenesis, clinical features and therapy". Hematology 12 (5): 361–370. October 2007. doi:10.1080/10245330701445392. PMID 17891600.
- ↑ Stijlemans, Benoît; Guilliams, Martin; Raes, Geert; Beschin, Alain; Magez, Stefan; De Baetselier, Patrick (August 2007). "African trypanosomosis: From immune escape and immunopathology to immune intervention". Veterinary Parasitology 148 (1): 3–13. doi:10.1016/j.vetpar.2007.05.005. PMID 17560035.
- ↑ "Do Hemorrhoids Cause Iron Deficiency Anemia?". 26 June 2018. https://lacolon.com/article/hemorrhoids-iron-deficiency-can-hemorrhoids-cause-iron-deficiency-anemia.
- ↑ "Hookworm-related anaemia among pregnant women: a systematic review". PLOS Neglected Tropical Diseases 2 (9). September 2008. doi:10.1371/journal.pntd.0000291. PMID 18820740. Bibcode: 2008PNTDi...2..291B.
- ↑ "Trichuris and hookworm infections associated with anaemia during pregnancy". Tropical Medicine & International Health 16 (4): 531–537. April 2011. doi:10.1111/j.1365-3156.2011.02727.x. PMID 21281406.
- ↑ Whitehead, Nedra S.; Williams, Laurina O.; Meleth, Sreelatha; Kennedy, Sara M.; Ubaka-Blackmoore, Nneka; Geaghan, Sharon M.; Nichols, James H.; Carroll, Patrick et al. (December 2019). "Interventions to prevent iatrogenic anemia: a Laboratory Medicine Best Practices systematic review". Critical Care 23 (1): 278. doi:10.1186/s13054-019-2511-9. PMID 31399052.
- ↑ Martin, Niels D.; Scantling, Dane (September 2015). "Hospital-Acquired Anemia: A Contemporary Review of Etiologies and Prevention Strategies". Journal of Infusion Nursing 38 (5): 330–338. doi:10.1097/NAN.0000000000000121. PMID 26339939.
- ↑ Bellotto, Fabio; Cati, Arianna (March 2006). "Anemia ed ischemia miocardica: relazioni ed interferenze" (in it). Recenti Progressi in Medicina 97 (3): 153–164. doi:10.1701/121.1312. PMID 16700423.
- ↑ Hung, Szu-Chun; Kuo, Ko-Lin; Peng, Ching-Hsiu; Wu, Che-Hsiung; Wang, Yi-Chun; Tarng, Der-Cherng (2015). "Association of Fluid Retention With Anemia and Clinical Outcomes Among Patients With Chronic Kidney Disease". Journal of the American Heart Association 4 (1). doi:10.1161/JAHA.114.001480. PMID 25559015.
- ↑ "Fluid imbalances". Portable Fluids and Electrolytes (Portable Series). Hagerstwon, MD: Lippincott Williams & Wilkins. 2007. p. 62. ISBN 978-1-58255-678-9.
- ↑ "ISBT: 8. Obstetric anaemia" (in en). http://www.isbtweb.org/working-parties/clinical-transfusion/8-obstetric-anaemia/.
- ↑ "The definition of anemia: what is the lower limit of normal of the blood hemoglobin concentration?". Blood 107 (5): 1747–1750. March 2006. doi:10.1182/blood-2005-07-3046. PMID 16189263.
- ↑ Anemia at eMedicine
- ↑ Rodak, Bernadette F. (2007). Hematology: Clinical Principles and Applications (3rd ed.). Philadelphia: Saunders. p. 220. ISBN 978-1-4160-3006-5. https://books.google.com/books?id=6sfacydDNsUC&pg=PA220.
- ↑ Pomeranz, Albert J.; Sabnis, Svapna; Busey, Sharon; Kliegman, Robert M. (2016). Pediatric Decision-Making Strategies (2nd ed.). Elsevier. ISBN 978-0-323-29854-4.
- ↑ World Health Organization (2024) (in en). Guideline on haemoglobin cutoffs to define anaemia in individuals and populations. World Health Organization. p. xi. ISBN 978-92-4-008854-2. https://iris.who.int/server/api/core/bitstreams/f9f74397-1440-478d-a63c-26f29a01552f/content. Retrieved 2025-12-23.
- ↑ Chhabra, Gaurav (2017-12-01). "Automated hematology analyzers: Recent trends and applications" (in en). Journal of Laboratory Physicians 10 (1): 15–16. doi:10.4103/JLP.JLP_124_17. ISSN 0974-2727. PMID 29403197.
- ↑ "Anemia" (in en). https://www.radiologyinfo.org/en/info/anemia.
- ↑ Freeman, Andrew M.; Zubair, Muhammad (2026), "Anemia Screening", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 29763080, http://www.ncbi.nlm.nih.gov/books/NBK499905/, retrieved 2026-03-30
- ↑ "Reticulocyte Count: Testing, Purpose & Results" (in en). https://my.clevelandclinic.org/health/diagnostics/22787-reticulocyte-count.
- ↑ 79.0 79.1 Freeman, Andrew M.; Zubair, Muhammad (2026), "Anemia Screening", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 29763080, http://www.ncbi.nlm.nih.gov/books/NBK499905/, retrieved 2026-03-30
- ↑ Al Hadidi, Samer (17 August 2021). "Blood Smear: The Fifth Vital Sign in Hematology - Hematology.org" (in en). https://www.hematology.org/education/trainees/fellows/hematopoiesis/2021/blood-smear.
- ↑ "How should I assess a person with suspected malaria?". January 2024. https://cks.nice.org.uk/topics/malaria/diagnosis/assessment/.
- ↑ "Anaemia" (in en). 2019-03-28. https://www.kidney.org.uk/anaemia.
- ↑ Jogu, Prasad; Kamran, Muhammad T. (2026), "Iron-Deficiency Anemia", StatPearls (Treasure Island (FL): StatPearls Publishing), PMID 28846348, http://www.ncbi.nlm.nih.gov/books/NBK448065/, retrieved 2026-03-06
- ↑ "Toxicology of Lead and Its Damage to Mammalian Organs". Lead – Its Effects on Environment and Health. Metal Ions in Life Sciences. 17. 2017. pp. 501–534. doi:10.1515/9783110434330-016. ISBN 978-3-11-043433-0.
- ↑ Recommendations to Prevent and Control Iron Deficiency in the United States MMWR 1998;47 (No. RR-3) p. 5
- ↑ Centers for Disease Control Prevention (CDC) (October 11, 2002). "Iron Deficiency – United States, 1999–2000". MMWR 51 (40): 897–899. PMID 12418542. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5140a1.htm. Retrieved 21 April 2012.
- ↑ "Global Iron-Deficiency Anemia Therapy Market – Industry Trends and Forecast to 2027 –". https://www.databridgemarketresearch.com/reports/global-iron-deficiency-anemia-therapy-market.
- ↑ "Iron deficiency and cognitive achievement among school-aged children and adolescents in the United States". Pediatrics 107 (6): 1381–1386. June 2001. doi:10.1542/peds.107.6.1381. PMID 11389261. Bibcode: 2001Pedia.107.1381H.
- ↑ "A review of studies on the effect of iron deficiency on cognitive development in children". The Journal of Nutrition 131 (2S–2): 649S–666S; discussion 666S–668S. February 2001. doi:10.1093/jn/131.2.649S. PMID 11160596.
- ↑ "Iron Deficiency Anaemia: Assessment, Prevention, and Control: A guide for programme managers". https://www.who.int/nutrition/publications/en/ida_assessment_prevention_control.pdf.
- ↑ "Differentiation of iron deficiency from thalassaemia trait". Lancet 1 (7808): 882. April 1973. doi:10.1016/s0140-6736(73)91446-3. PMID 4123424.
- ↑ Long, Brit; Koyfman, Alex (August 2018). "Emergency Medicine Evaluation and Management of Anemia". Emergency Medicine Clinics of North America 36 (3): 609–630. doi:10.1016/j.emc.2018.04.009. PMID 30037447.
- ↑ eMedicine – "Vitamin B-12 Associated Neurological Diseases": Article by Niranjan N Singh, July 18, 2006. .
- ↑ "Physiology or Medicine 1934 – Presentation Speech". Nobelprize.org. 1934-12-10. http://nobelprize.org/nobel_prizes/medicine/laureates/1934/press.html.
- ↑ 95.0 95.1 Harvey, John W. (2012). Veterinary hematology: a diagnostic guide and color atlas. St. Louis, MO: Elsevier/Saunders. p. 104. ISBN 978-1-4377-0173-9.
- ↑ Hovda, L; Brutlag, A; Poppenga, RH et al., eds (2016). "Chapter 69: Onions and garlic". Blackwell's Five-Minute Veterinary Consult Clinical Companion: Small Animal Toxicology (2nd ed.). John Wiley & Sons. pp. 515–520. ISBN 978-1-119-03652-4.
- ↑ "Hemolytic Disorders". Robinson's Current Therapy in Equine Medicine. 2015. pp. 492–495. doi:10.1016/B978-1-4557-4555-5.00117-5. ISBN 978-1-4557-4555-5.
- ↑ "Laboratory evaluation of anemia". The Western Journal of Medicine 146 (4): 443–451. April 1987. PMID 3577135.
- ↑ "MedTerms Definition: Refractory Anemia". Medterms.com. 2011-04-27. http://www.medterms.com/script/main/art.asp?articlekey=5275.
- ↑ "Good Source for later". Atlasgeneticsoncology.org. http://atlasgeneticsoncology.org/Anomalies/RAID1104.html.
- ↑ "Refractory iron deficiency anemia as the primary clinical manifestation of celiac disease". Journal of Pediatric Hematology/Oncology 25 (2): 169–172. February 2003. doi:10.1097/00043426-200302000-00018. PMID 12571473.
- ↑ "What are RBC-transfusion-dependence and -independence?". Leukemia Research 35 (1): 8–11. January 2011. doi:10.1016/j.leukres.2010.07.015. PMID 20692036.
- ↑ 103.0 103.1 "Management of RBC-transfusion dependence". Hematology. American Society of Hematology. Education Program 2007: 398–404. 2007. doi:10.1182/asheducation-2007.1.398. PMID 18024657.
- ↑ Hillyer, Christopher D.; Silberstein, Leslie E.; Ness, Paul M.; Anderson, Kenneth C.; Roback, John D. (2006). Blood Banking and Transfusion Medicine: Basic Principles and Practice. Elsevier Health Sciences. p. 534. ISBN 978-0-7020-3625-5. https://books.google.com/books?id=8iEPDQAAQBAJ&pg=PT556.
- ↑ Mandel, Jess; Taichman, Darren (2006) (in en). Pulmonary Vascular Disease. Elsevier Health Sciences. p. 170. ISBN 978-1-4160-2246-6. https://books.google.com/books?id=v-pr4P34QjIC&pg=PA170.
- ↑ Ferri, Fred F. (2015) (in en). BOPOD – Ferri's Clinical Advisor 2016. Elsevier Health Sciences. p. 1131.e2. ISBN 978-0-323-37822-2. https://books.google.com/books?id=bbLSCQAAQBAJ&pg=PA1131-IA2.
- ↑ 107.0 107.1 107.2 "Anemia Treatment Drugs: 2019 Global Market Study; Analyzed by Type of Anemia, Type of Drug, and Geography". GlobeNewswire (Press release). 2019-04-26. Retrieved 2023-08-02.
- ↑ 108.0 108.1 108.2 108.3 108.4 Nguyen, Minhthao; Tadi, Prasanna (2025), "Iron Supplementation", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 32491308, retrieved 2025-10-19
- ↑ 109.0 109.1 "Strategies to control nutritional anemia". The American Journal of Clinical Nutrition 64 (5): 789–790. November 1996. doi:10.1093/ajcn/64.5.789. PMID 8901803.
- ↑ Karami, Mohammadmahdi; Chaleshgar, Maryam; Salari, Nader; Akbari, Hakimeh; Mohammadi, Masoud (2022-07-01). "Global Prevalence of Anemia in Pregnant Women: A Comprehensive Systematic Review and Meta-Analysis" (in en). Maternal and Child Health Journal 26 (7): 1473–1487. doi:10.1007/s10995-022-03450-1. ISSN 1573-6628. PMID 35608810.
- ↑ Low, MS; Speedy, J; Styles, CE; De-Regil, LM; Pasricha, SR (18 April 2016). "Daily iron supplementation for improving anaemia, iron status and health in menstruating women.". The Cochrane Database of Systematic Reviews 2016 (4). doi:10.1002/14651858.CD009747.pub2. PMID 27087396.
- ↑ "Intravenous ascorbic acid administration for erythropoietin-hyporesponsive anemia in iron loaded hemodialysis patients". Artificial Organs 26 (4): 366–370. April 2002. doi:10.1046/j.1525-1594.2002.06888.x. PMID 11952508.
- ↑ "Anaemia management in people with chronic kidney disease | Guidance and guidelines | NICE". 9 February 2011. http://guidance.nice.org.uk/CG114/Guidance/pdf/English.
- ↑ Ng, Oliver; Keeler, Barrie D; Mishra, Amitabh; Simpson, J A; Neal, Keith; Al-Hassi, Hafid Omar; Brookes, Matthew J; Acheson, Austin G (7 December 2019). "Iron therapy for preoperative anaemia". Cochrane Database of Systematic Reviews 2019 (12). doi:10.1002/14651858.CD011588.pub3. PMID 31811820.
- ↑ "Clinical use of intravenous iron: administration, efficacy, and safety". Hematology. American Society of Hematology. Education Program 2010: 338–347. 2010. doi:10.1182/asheducation-2010.1.338. PMID 21239816.
- ↑ 116.0 116.1 116.2 116.3 "Anemia - Treatment and Management | NHLBI, NIH". www.nhlbi.nih.gov. 2022-03-24. Retrieved 2025-10-19.
- ↑ 117.0 117.1 "Treatment of anemia in patients with heart disease: a systematic review". Annals of Internal Medicine 159 (11): 746–757. December 2013. doi:10.7326/0003-4819-159-11-201312030-00007. PMID 24297191.
- ↑ . British Society of Gastroenterology"Guidelines for the management of iron deficiency anaemia". Gut 60 (10): 1309–1316. October 2011. doi:10.1136/gut.2010.228874. PMID 21561874.
- ↑ Preston, Nancy J; Hurlow, Adam; Brine, Jennifer; Bennett, Michael I (15 February 2012). "Blood transfusions for anaemia in patients with advanced cancer". Cochrane Database of Systematic Reviews 2012 (2). doi:10.1002/14651858.CD009007.pub2. PMID 22336857.
- ↑ 120.0 120.1 Johns Hopkins Medicine. (n.d.). Aplastic anemia. The Johns Hopkins University & Health System. Retrieved October 19, 2025 https://www.hopkinsmedicine.org/kimmel-cancer-center/cancers-we-treat/blood-bone-marrow-cancers/aplastic-anemia
- ↑ "Pernicious anemia: MedlinePlus Medical Encyclopedia" (in en). https://medlineplus.gov/ency/article/000569.htm.
- ↑ Hankey, Graeme J. (2008). Clinical neurology. Joanna M. Wardlaw. London: Manson. ISBN 978-1-84076-518-2. OCLC 503441695.
- ↑ 123.0 123.1 123.2 Langan, Robert C.; Goodbred, Andrew J. (2017-09-15). "Vitamin B12 Deficiency: Recognition and Management" (in en-US). American Family Physician 96 (6): 384–389. PMID 28925645. https://www.aafp.org/pubs/afp/issues/2017/0915/p384.html.
- ↑ 124.0 124.1 "Pernicious Anemia Clinical Presentation: History, Physical Examination". 2017-09-14. http://emedicine.medscape.com/article/204930-clinical#b3.
- ↑ 125.0 125.1 Schoener, Benjamin; Borger, Judith (2025), "Erythropoietin Stimulating Agents", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30725682, retrieved 2025-10-19
- ↑ 126.0 126.1 "September 2007 update on EORTC guidelines and anemia management with erythropoiesis-stimulating agents". The Oncologist 13 Suppl 3 (Supplement 3): 33–36. 2008. doi:10.1634/theoncologist.13-S3-33. PMID 18458123.
- ↑ American Society of Nephrology, "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation (American Society of Nephrology), http://choosingwisely.org/wp-content/uploads/2012/04/5things_12_factsheet_Amer_Soc_Neph.pdf, retrieved August 17, 2012
- ↑ "Erythropoietin plus iron versus control treatment including placebo or iron for preoperative anaemic adults undergoing non-cardiac surgery". Cochrane Database of Systematic Reviews 2020 (8). 2020. doi:10.1002/14651858.CD012451.pub2. PMID 32790892.
- ↑ 129.0 129.1 129.2 "Exceptional Blood Loss – Anemia". http://www.uhms.org/ResourceLibrary/Indications/ExceptionalBloodLossAnemia/tabid/277/Default.aspx.
- ↑ "Hyperbaric oxygen in exceptional acute blood-loss anemia". J. Hyperbaric Med 2 (4): 205–210. 1987. http://archive.rubicon-foundation.org/4352. Retrieved 2008-05-19.
- ↑ 131.0 131.1 "Hyperbaric oxygen therapy - Mayo Clinic". www.mayoclinic.org. Retrieved 2025-10-20.
- ↑ "A systematic review of the application of hyperbaric oxygen in the treatment of severe anemia: an evidence-based approach". Undersea & Hyperbaric Medicine 32 (1): 61–83. 2005. PMID 15796315. http://archive.rubicon-foundation.org/4038.
- ↑ 133.0 133.1 Kaufner, Lutz; von Heymann, Christian; Henkelmann, Anne; Pace, Nathan L; Weibel, Stephanie; Kranke, Peter; Meerpohl, Joerg J; Gill, Ravi (13 August 2020). "Erythropoietin plus iron versus control treatment including placebo or iron for preoperative anaemic adults undergoing non-cardiac surgery". Cochrane Database of Systematic Reviews 2020 (8). doi:10.1002/14651858.CD012451.pub2. PMID 32790892.
- ↑ Kotzé, Alwyn; Harris, Andrea; Baker, Charles; Iqbal, Tariq; Lavies, Nick; Richards, Toby; Ryan, Kate; Taylor, Craig et al. (November 2015). "British Committee for Standards in Haematology Guidelines on the Identification and Management of Pre-Operative Anaemia". British Journal of Haematology 171 (3): 322–331. doi:10.1111/bjh.13623. PMID 26343392.
- ↑ 135.0 135.1 Gardner, William M; Razo, Christian; McHugh, Theresa A; Hagins, Hailey; Vilchis-Tella, Victor M; Hennessy, Conor; Taylor, Heather Jean; Perumal, Nandita et al. (2023). "Prevalence, years lived with disability, and trends in anaemia burden by severity and cause, 1990–2021: findings from the Global Burden of Disease Study 2021" (in English). The Lancet Haematology 10 (9): e713–e734. doi:10.1016/S2352-3026(23)00160-6. ISSN 2352-3026. PMID 37536353.
- ↑ Abuga, Kelvin Mokaya (2026). Severe Anaemia and Bacteraemia in Kenyan Children: Epidemiology and Mechanisms (Thesis). The Open University. doi:10.21954/OU.RO.00108090.
- ↑ Abuga, Kelvin Mokaya; Muriuki, John Muthii; Mutua, Agnes M.; Atkinson, Sarah H.; PDF, See (2025). Severe Anaemia and Invasive Bacterial Infections in Kenyan Children: A 26-Year Hospital Surveillance Observational Study. doi:10.2139/ssrn.5839018. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=5839018. Retrieved 2026-03-07.
- ↑ Abuga, Kelvin Mokaya (2026). Severe Anaemia and Bacteraemia in Kenyan Children: Epidemiology and Mechanisms (Thesis). The Open University. doi:10.21954/OU.RO.00108090.
- ↑ Gaskell, Helen; Derry, Sheena; Andrew Moore, R.; McQuay, Henry J. (2008-01-14). "Prevalence of anaemia in older persons: systematic review" (in en). BMC Geriatrics 8 (1). doi:10.1186/1471-2318-8-1. ISSN 1471-2318. PMID 18194534.
- ↑ Liu, Yujuan; Ren, Weifang; Wang, Shuying; Xiang, Minmin; Zhang, Shunxian; Zhang, Feng (2024-10-15). "Global burden of anemia and cause among children under five years 1990–2019: findings from the global burden of disease study 2019" (in English). Frontiers in Nutrition 11. doi:10.3389/fnut.2024.1474664. ISSN 2296-861X. PMID 39474456.
- ↑ Vanasse, Gary J.; Berliner, Nancy (2010-12-04). "Anemia in Elderly Patients: An Emerging Problem for the 21st Century" (in en). Hematology 2010 (1): 271–275. doi:10.1182/asheducation-2010.1.271. ISSN 1520-4391. PMID 21239805. https://ashpublications.org/hematology/article/2010/1/271/95939/Anemia-in-Elderly-Patients-An-Emerging-Problem-for.
- ↑ van Hensbroek, MB; Jonker, F; Bates, I (September 2011). "Severe acquired anaemia in Africa: new concepts.". British Journal of Haematology 154 (6): 690–5. doi:10.1111/j.1365-2141.2011.08761.x. PMID 21707575.
- ↑ Abuga, KM; Muriuki, JM; Williams, TN; Atkinson, SH (22 September 2020). "How Severe Anaemia Might Influence the Risk of Invasive Bacterial Infections in African Children". International Journal of Molecular Sciences 21 (18): 6976. doi:10.3390/ijms21186976. PMID 32972031.
- ↑ Abuga, Kelvin M.; Nairz, Manfred; MacLennan, Calman A.; Atkinson, Sarah H. (2023-02-02). "Severe anaemia, iron deficiency, and susceptibility to invasive bacterial infections" (in en). Wellcome Open Research 8: 48. doi:10.12688/wellcomeopenres.18829.1. ISSN 2398-502X. PMID 37600584.
- ↑ Abuga, Kelvin Mokaya; Muriuki, John Muthii; Mutua, Agnes M.; Atkinson, Sarah H.; PDF, See (2025). Severe Anaemia and Invasive Bacterial Infections in Kenyan Children: A 26-Year Hospital Surveillance Observational Study. doi:10.2139/ssrn.5839018. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=5839018. Retrieved 2026-03-07.
- ↑ Moschovis, Peter P; Wiens, Matthew O; Arlington, Lauren; Antsygina, Olga; Hayden, Douglas; Dzik, Walter; Kiwanuka, Julius P; Christiani, David C et al. (May 2018). "Individual, maternal and household risk factors for anaemia among young children in sub-Saharan Africa: a cross-sectional study" (in en). BMJ Open 8 (5). doi:10.1136/bmjopen-2017-019654. ISSN 2044-6055. PMID 29764873.
- ↑ Karami, Mohammadmahdi; Chaleshgar, Maryam; Salari, Nader; Akbari, Hakimeh; Mohammadi, Masoud (2022-07-01). "Global Prevalence of Anemia in Pregnant Women: A Comprehensive Systematic Review and Meta-Analysis" (in en). Maternal and Child Health Journal 26 (7): 1473–1487. doi:10.1007/s10995-022-03450-1. ISSN 1573-6628. PMID 35608810.
- ↑ FAO; IFAD; UNICEF; WFP; WHO (2024) (in English). The State of Food Security and Nutrition in the World 2024. FAO; IFAD; UNICEF; WFP; WHO. doi:10.4060/cd1254en. ISBN 978-92-5-138882-2. https://openknowledge.fao.org/handle/20.500.14283/cd1254en.
- ↑ "Anemia, genetic diseases, and malaria in prehistoric mainland Southeast Asia". American Journal of Physical Anthropology 101 (1): 11–27. September 1996. doi:10.1002/(SICI)1096-8644(199609)101:1<11::AID-AJPA2>3.0.CO;2-G. PMID 8876811.
- ↑ 150.0 150.1 150.2 Sheftel, Alex D.; Mason, Anne B.; Ponka, Prem (March 2012). "The long history of iron in the Universe and in health and disease". Biochimica et Biophysica Acta (BBA) - General Subjects 1820 (3): 161–187. doi:10.1016/j.bbagen.2011.08.002. ISSN 0006-3002. PMID 21856378. Bibcode: 2012BBAcG1820..161S.
- ↑ 151.0 151.1 Aird, William (2022-05-12). "Did you know that anemia was first named as a clinical entity in 1807? • The Blood Project". https://www.thebloodproject.com/did-you-know-that-anemia-was-recognized-as-a-clinical-construct-well-before-lab-tests-were-available/.
- ↑ Hens, Samantha M.; Godde, Kanya; Macak, Kristin M. (2019-03-07). "Iron deficiency anemia, population health and frailty in a modern Portuguese skeletal sample" (in en). PLOS ONE 14 (3). doi:10.1371/journal.pone.0213369. ISSN 1932-6203. PMID 30845224. Bibcode: 2019PLoSO..1413369H.
External links
| Classification | |
|---|---|
| External resources |
 |
