Biology:Gut flora
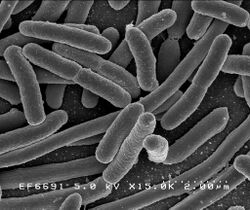
Gut flora, or gut microbiota, or gastrointestinal microbiota, is the complex community of microorganisms that live in the digestive tracts of humans and other animals, including insects. The gut metagenome is the aggregate of all the genomes of gut microbiota.[1] The gut is one niche that human microbiota inhabit.[2]
In humans, the gut microbiota has the largest numbers of bacteria and the greatest number of species compared to other areas of the body.[3] In humans, the gut flora is established at one to two years after birth, and by that time the intestinal epithelium and the intestinal mucosal barrier that it secretes have co-developed in a way that is tolerant to, and even supportive of, the gut flora and that also provides a barrier to pathogenic organisms.[4][5]
The relationship between some gut flora and humans is not merely commensal (a non-harmful coexistence), but rather a mutualistic relationship.[2]:700 Some human gut microorganisms benefit the host by fermenting dietary fiber into short-chain fatty acids (SCFAs), such as acetic acid and butyric acid, which are then absorbed by the host.[3][6] Intestinal bacteria also play a role in synthesizing vitamin B and vitamin K as well as metabolizing bile acids, sterols, and xenobiotics.[2][6] The systemic importance of the SCFAs and other compounds they produce are like hormones and the gut flora itself appears to function like an endocrine organ,[6] and dysregulation of the gut flora has been correlated with a host of inflammatory and autoimmune conditions.[3][7]
The composition of human gut microbiota changes over time, when the diet changes, and as overall health changes.[3][7] A systematic review from 2016 examined the preclinical and small human trials that have been conducted with certain commercially available strains of probiotic bacteria and identified those that had the most potential to be useful for certain central nervous system disorders.[8]
Classifications
The microbial composition of the gut microbiota varies across the digestive tract. In the stomach and small intestine, relatively few species of bacteria are generally present.[9][10] The colon, in contrast, contains a densely-populated microbial ecosystem with up to 1012 cells per gram of intestinal content.[9] These bacteria represent between 300 and 1000 different species.[9][10] However, 99% of the bacteria come from about 30 or 40 species.[11] As a consequence of their abundance in the intestine, bacteria also make up to 60% of the dry mass of feces.[12] Fungi, protists, archaea, and viruses are also present in the gut flora, but less is known about their activities.[13]
Over 99% of the bacteria in the gut are anaerobes, but in the cecum, aerobic bacteria reach high densities.[2] It is estimated that these gut flora have around a hundred times as many genes in total as there are in the human genome.[14]
Many species in the gut have not been studied outside of their hosts because most cannot be cultured.[10][11][15] While there are a small number of core species of microbes shared by most individuals, populations of microbes can vary widely among different individuals.[16] Within an individual, microbe populations stay fairly constant over time, even though some alterations may occur with changes in lifestyle, diet and age.[9][17] The Human Microbiome Project has set out to better describe the microflora of the human gut and other body locations.
The four dominant bacterial phyla in the human gut are Firmicutes, Bacteroidetes, Actinobacteria, and Proteobacteria.[18] Most bacteria belong to the genera Bacteroides, Clostridium, Faecalibacterium,[9][11] Eubacterium, Ruminococcus, Peptococcus, Peptostreptococcus, and Bifidobacterium.[9][11] Other genera, such as Escherichia and Lactobacillus, are present to a lesser extent.[9] Species from the genus Bacteroides alone constitute about 30% of all bacteria in the gut, suggesting that this genus is especially important in the functioning of the host.[10]
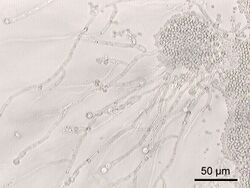
Fungal genera that have been detected in the gut include Candida, Saccharomyces, Aspergillus, Penicillium, Rhodotorula, Trametes, Pleospora, Sclerotinia, Bullera, and Galactomyces, among others.[19][20] Rhodotorula is most frequently found in individuals with inflammatory bowel disease while Candida is most frequently found in individuals with hepatitis B cirrhosis and chronic hepatitis B.[19]
Archaea constitute another large class of gut flora which are important in the metabolism of the bacterial products of fermentation.
Enterotype
An enterotype is a classification of living organisms based on its bacteriological ecosystem in the human gut microbiome not dictated by age, gender, body weight, or national divisions.[21] There are indications that long-term diet influences enterotype.[22] Three human enterotypes have been proposed,[21][23] but their value has been questioned.[24]
Composition
Anatomy
Stomach
Due to the high acidity of the stomach, most microorganisms cannot survive there. The main bacterial inhabitants of the stomach include: Streptococcus, Staphylococcus, Lactobacillus, Peptostreptococcus, and types of yeast.[2]:720 Helicobacter pylori is a Gram-negative spiral organism that establishes on gastric mucosa causing chronic gastritis and peptic ulcer disease and is a carcinogen for gastric cancer.[2]:904
Intestines
| Bacteria commonly found in the human colon[25] | |
| Bacterium | Incidence (%) |
|---|---|
| Bacteroides fragilis | 100 |
| Bacteroides melaninogenicus | 100 |
| Bacteroides oralis | 100 |
| Enterococcus faecalis | 100 |
| Escherichia coli | 100 |
| Enterobacter sp. | 40–80 |
| Klebsiella sp. | 40–80 |
| Bifidobacterium bifidum | 30–70 |
| Staphylococcus aureus | 30–50 |
| Lactobacillus | 20–60 |
| Clostridium perfringens | 25–35 |
| Proteus mirabilis | 5–55 |
| Clostridium tetani | 1–35 |
| Clostridium septicum | 5–25 |
| Pseudomonas aeruginosa | 3–11 |
| Salmonella enterica | 3–7 |
| Faecalibacterium prausnitzii | ?common |
| Peptostreptococcus sp. | ?common |
| Peptococcus sp. | ?common |
The small intestine contains a trace amount of microorganisms due to the proximity and influence of the stomach. Gram-positive cocci and rod-shaped bacteria are the predominant microorganisms found in the small intestine.[2] However, in the distal portion of the small intestine alkaline conditions support gram-negative bacteria of the Enterobacteriaceae.[2] The bacterial flora of the small intestine aid in a wide range of intestinal functions. The bacterial flora provide regulatory signals that enable the development and utility of the gut. Overgrowth of bacteria in the small intestine can lead to intestinal failure.[26] In addition the large intestine contains the largest bacterial ecosystem in the human body.[2] About 99% of the large intestine and feces flora are made up of obligate anaerobes such as Bacteroides and Bifidobacterium.[27] Factors that disrupt the microorganism population of the large intestine include antibiotics, stress, and parasites.[2]
Bacteria make up most of the flora in the colon[28] and 60% of the dry mass of feces.[9] This fact makes feces an ideal source to test for gut flora for any tests and experiments by extracting the nucleic acid from fecal specimens, and bacterial 16S rRNA gene sequences are generated with bacterial primers. This form of testing is also often preferable to more invasive techniques, such as biopsies. Somewhere between 300[9] and 1000 different species live in the gut,[10] with most estimates at about 500.[29][30] However, it is probable that 99% of the bacteria come from about 30 or 40 species, with Faecalibacterium prausnitzii being the most common species in healthy adults.[11][31] Fungi and protists also make up a part of the gut flora, but less is known about their activities.[32] The virome is mostly bacteriophages.[33]
Research suggests that the relationship between gut flora and humans is not merely commensal (a non-harmful coexistence), but rather is a mutualistic, symbiotic relationship.[10] Though people can survive with no gut flora,[29] the microorganisms perform a host of useful functions, such as fermenting unused energy substrates, training the immune system via end products of metabolism like propionate and acetate, preventing growth of harmful species, regulating the development of the gut, producing vitamins for the host (such as biotin and vitamin K), and producing hormones to direct the host to store fats.[2] Extensive modification and imbalances of the gut microbiota and its microbiome or gene collection are associated with obesity.[34] However, in certain conditions, some species are thought to be capable of causing disease by causing infection or increasing cancer risk for the host.[9][28]
Age
It has been demonstrated that there are common patterns of microbiome composition evolution during life.[35] In general, the diversity of microbiota composition of fecal samples is significantly higher in adults than in children, although interpersonal differences are higher in children than in adults.[36] Much of the maturation of microbiota into an adult-like configuration happens during the three first years of life.[36]
As the microbiome composition changes, so does the composition of bacterial proteins produced in the gut. In adult microbiomes, a high prevalence of enzymes involved in fermentation, methanogenesis and the metabolism of arginine, glutamate, aspartate and lysine have been found. In contrast, in infant microbiomes the dominant enzymes are involved in cysteine metabolism and fermentation pathways.[36]
Diet
Studies and statistical analyses have identified the different bacterial genera in gut microbiota and their associations with nutrient intake. Gut microflora is mainly composed of three enterotypes: Prevotella, Bacteroides, and Ruminococcus. There is an association between the concentration of each microbial community and diet. For example, Prevotella is related to carbohydrates and simple sugars, while Bacteroides is associated with proteins, amino acids, and saturated fats. Specialist microbes that break down mucin, survive on their host's carbohydrate excretions.[37] One enterotype will dominate depending on the diet. Altering the diet will result in a corresponding change in the numbers of species.[22]
Malnourished human children have less mature and less diverse gut microbiota than healthy children, and changes in the microbiome associated with nutrient scarcity can in turn be a pathophysiological cause of malnutrition.[38][39] Malnourished children also typically have more potentially pathogenic gut flora, and more yeast in their mouths and throats.[40] Altering diet may lead to changes in gut microbiota composition and diversity.[37]
Geography
Gut microbiome composition depends on the geographic origin of populations. Variations in a trade-off of Prevotella, the representation of the urease gene, and the representation of genes encoding glutamate synthase/degradation or other enzymes involved in amino acids degradation or vitamin biosynthesis show significant differences between populations from the US, Malawi or Amerindian origin.[36]
The US population has a high representation of enzymes encoding the degradation of glutamine and enzymes involved in vitamin and lipoic acid biosynthesis; whereas Malawi and Amerindian populations have a high representation of enzymes encoding glutamate synthase and they also have an overrepresentation of α-amylase in their microbiomes. As the US population has a diet richer in fats than Amerindian or Malawian populations which have a corn-rich diet, the diet is probably the main determinant of the gut bacterial composition.[36]
Further studies have indicated a large difference in the composition of microbiota between European and rural African children. The fecal bacteria of children from Florence were compared to that of children from the small rural village of Boulpon in Burkina Faso. The diet of a typical child living in this village is largely lacking in fats and animal proteins and rich in polysaccharides and plant proteins. The fecal bacteria of European children were dominated by Firmicutes and showed a marked reduction in biodiversity, while the fecal bacteria of the Boulpon children was dominated by Bacteroidetes. The increased biodiversity and different composition of gut flora in African populations may aid in the digestion of normally indigestible plant polysaccharides and also may result in a reduced incidence of non-infectious colonic diseases.[41]
On a smaller scale, it has been shown that sharing numerous common environmental exposures in a family is a strong determinant of individual microbiome composition. This effect has no genetic influence and it is consistently observed in culturally different populations.[36]
Acquisition in human infants
The establishment of a gut flora is crucial to the health of an adult, as well the functioning of the gastrointestinal tract.[42] In humans, a gut flora similar to an adult's is formed within one to two years of birth.[4]
The traditional view of the gastrointestinal tract of a normal fetus is that it is sterile, although this view has been challenged in the past few years.[43] Multiple lines of evidence have begun to emerge that suggest there may be bacteria in the intrauterine environment. In humans, research has shown that microbial colonization may occur in the fetus[44] with one study showing Lactobacillus and Bifidobacterium species were present in placental biopsies.[45] Several rodent studies have demonstrated the presence of bacteria in the amniotic fluid and placenta, as well as in the meconium of babies born by sterile cesarean section.[46][47] In another study, researchers administered a culture of bacteria orally to a pregnant dam, and detected the bacteria in the offspring, likely resulting from transmission between the digestive tract and amniotic fluid via the blood stream.[48] However, researchers caution that the source of these intrauterine bacteria, whether they are alive, and their role, is not yet understood.[45] [49]
During birth and rapidly thereafter, bacteria from the mother and the surrounding environment colonize the infant's gut.[4] The exact sources of bacteria is not fully understood, but may include the birth canal, other people (parents, siblings, hospital workers), breastmilk, food, and the general environment with which the infant interacts.[50] However, as of 2013, it remains unclear whether most colonizing arises from the mother or not.[4] Infants born by caesarean section may also be exposed to their mothers' microflora, but the initial exposure is most likely to be from the surrounding environment such as the air, other infants, and the nursing staff, which serve as vectors for transfer.[44] During the first year of life, the composition of the gut flora is generally simple and changes a great deal with time and is not the same across individuals.[4] The initial bacterial population are generally facultative anaerobic organisms; investigators believe that these initial colonizers decrease the oxygen concentration in the gut, which in turn allows obligately anaerobic bacteria like Bacteroides, Actinobacteria, and Firmicutes to become established and thrive.[4] Breast-fed babies become dominated by bifidobacteria, possibly due to the contents of bifidobacterial growth factors in breast milk, and by the fact that breast milk carries prebiotic components, allowing for healthy bacterial growth.[45][51] In contrast, the microbiota of formula-fed infants is more diverse, with high numbers of Enterobacteriaceae, enterococci, bifidobacteria, Bacteroides, and clostridia.[52]
Caesarean section, antibiotics, and formula feeding may alter the gut microbiome composition.[45] Children treated with antibiotics have less stable, and less diverse floral communities.[53] Caesarean sections have been shown to be disruptive to mother-offspring transmission of bacteria, which impacts the overall health of the offspring by raising risks of disease such as celiacs, asthma, and type 1 diabetes.[45] This further evidences the importance of a healthy gut microbiome. Various methods of microbiome restoration are being explored, typically involving exposing the infant to maternal vaginal contents, and oral probiotics.[45]
Functions
When the gut flora first started to be studied, it was thought to have three key roles: directly defending against pathogens, fortifying host defense by its role in developing and maintaining the intestinal epithelium and inducing antibody production there, and metabolizing otherwise indigestible compounds in food; subsequent work discovered its role in training the developing immune system, and yet further work focused on its role in the gut-brain axis.[54]
Direct inhibition of pathogens
The gut flora community plays a direct role in defending against pathogens by fully colonizing the space, making use of all available nutrients, and by secreting compounds that kill or inhibit unwelcome organisms that would compete for nutrients with it.[55] Disruption of the gut flora allows competing organisms like Clostridium difficile to become established that otherwise are kept in abeyance.[55]
Development of enteric protection and immune system
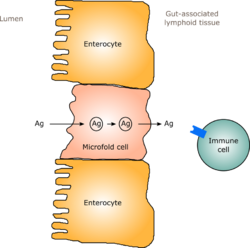
In humans, a gut flora similar to an adult's is formed within one to two years of birth.[4] As the gut flora gets established, the lining of the intestines – the intestinal epithelium and the intestinal mucosal barrier that it secretes – develop as well, in a way that is tolerant to, and even supportive of, commensurate microorganisms to a certain extent and also provides a barrier to pathogenic ones.[4] Specifically, goblet cells that produce the mucosa proliferate, and the mucosa layer thickens, providing an outside mucosal layer in which "friendly" microorganisms can anchor and feed, and an inner layer that even these organisms cannot penetrate.[4][5] Additionally, the development of gut-associated lymphoid tissue (GALT), which forms part of the intestinal epithelium and which detects and reacts to pathogens, appears and develops during the time that the gut flora develops and established.[4] The GALT that develops is tolerant to gut flora species, but not to other microorganisms.[4] GALT also normally becomes tolerant to food to which the infant is exposed, as well as digestive products of food, and gut flora's metabolites (molecules formed from metabolism) produced from food.[4]
The human immune system creates cytokines that can drive the immune system to produce inflammation in order to protect itself, and that can tamp down the immune response to maintain homeostasis and allow healing after insult or injury.[4] Different bacterial species that appear in gut flora have been shown to be able to drive the immune system to create cytokines selectively; for example Bacteroides fragilis and some Clostridia species appear to drive an anti-inflammatory response, while some segmented filamentous bacteria drive the production of inflammatory cytokines.[4][56] Gut flora can also regulate the production of antibodies by the immune system.[4][57] One function of this regulation is to cause B cells to class switch to IgA. In most cases B cells need activation from T helper cells to induce class switching; however, in another pathway, gut flora cause NF-kB signaling by intestinal epithelial cells which results in further signaling molecules being secreted.[58] These signaling molecules interact with B cells to induce class switching to IgA.[58] IgA is an important type of antibody that is used in mucosal environments like the gut. It has been shown that IgA can help diversify the gut community and helps in getting rid of bacteria that cause inflammatory responses.[59] Ultimately, IgA maintains a healthy environment between the host and gut bacteria.[59] These cytokines and antibodies can have effects outside the gut, in the lungs and other tissues.[4]
The immune system can also be altered due to the gut bacteria's ability to produce metabolites that can effect cells in the immune system. For example short-chain fatty acids (SCFA) can be produced by some gut bacteria through fermentation.[60] SCFAs stimulate a rapid increase in the production of innate immune cells like neutrophils, basophils and eosinophils.[60] These cells are part of the innate immune system that try to limit the spread of infection.
Metabolism
{{Annotated image 4 | image = Microbiota-derived 3-Indolepropionic acid-notext.svg | link = Commons:File:Microbiota-derived 3-Indolepropionic acid.svg | header = Tryptophan metabolism by human gastrointestinal microbiota ( ) | header_align = center | header_background = #F0F8FF | align = right | image-width = 600 | image-left = 0 | image-top = 10 | width = 580 | height = 470 | alt = Tryptophan metabolism diagram | caption = {{{caption|This diagram shows the biosynthesis of bioactive compounds (indole and certain other derivatives) from by bacteria in the gut.[61] Indole is produced from tryptophan by bacteria that express tryptophanase.[61] Clostridium sporogenes metabolizes tryptophan into indole and subsequently 3-indolepropionic acid (IPA),[62] a highly potent neuroprotective antioxidant that scavenges hydroxyl radicals.[61][63][64] IPA binds to the pregnane X receptor (PXR) in intestinal cells, thereby facilitating mucosal homeostasis and barrier function.[61] Following absorption from the intestine and distribution to the brain, IPA confers a neuroprotective effect against cerebral ischemia and Alzheimer's disease.[61] Lactobacillus species metabolize tryptophan into {{when pagename is|Indole-3-carboxaldehyde=indole-3-carboxaldehyde|other=indole-3-aldehyde}} (I3A) which acts on the aryl hydrocarbon receptor (AhR) in intestinal immune cells, in turn increasing interleukin-22 (IL-22) production.[61] Indole itself triggers the secretion of glucagon-like peptide-1 (GLP-1) in intestinal L cells and acts as a ligand for AhR.[61] Indole can also be metabolized by the liver into ]], a compound that is toxic in high concentrations and associated with vascular disease and renal dysfunction.[61] AST-120 (activated charcoal), an intestinal sorbent that is [[Oral administrat[[Physics:taken by mouth,Chemistry:Adsorption|adsorbs i]]ndole, in turn decreasing the concentration of indoxyl sulfate in blood plasma.[61] }}} | annot-font-size = 14 | annot-text-align = left | annotations =
expressing
bacteria
immune
cells
↓Activation of glial cells and astrocytes
↓4-Hydroxy-2-nonenal levels
↓DNA damage
–Antioxidant
–Inhibits β-amyloid fibril formation
↑IL-22 production
↑Oxidative stress
↑Smooth muscle cell proliferation
↑Aortic wall thickness and calcification
↑Renal dysfunction
–Uremic toxin
}} Without gut flora, the human body would be unable to utilize some of the undigested carbohydrates it consumes, because some types of gut flora have enzymes that human cells lack for breaking down certain polysaccharides.[6] Rodents raised in a sterile environment and lacking in gut flora need to eat 30% more calories just to remain the same weight as their normal counterparts.[6] Carbohydrates that humans cannot digest without bacterial help include certain starches, fiber, oligosaccharides, and sugars that the body failed to digest and absorb like lactose in the case of lactose intolerance and sugar alcohols, mucus produced by the gut, and proteins.[3][6]
Bacteria turn carbohydrates they ferment into short-chain fatty acids by a form of fermentation called saccharolytic fermentation.[30] Products include acetic acid, propionic acid and butyric acid.[11][30] These materials can be used by host cells, providing a major source of energy and nutrients.[30] Gases and organic acids, such as lactic acid, are also produced by fermentation.[11] Acetic acid is used by muscle, propionic acid facilitates liver production of ATP, and butyric acid provides energy to gut cells.[30]
Gut flora also synthesize vitamins like biotin and folate, and facilitate absorption of dietary minerals, including magnesium, calcium, and iron.[9][17] Methanobrevibacter smithii is unique because it is not a species of bacteria, but rather a member of domain Archeae, and is the most abundant methane-producing archaeal species in the human gastrointestinal microbiota.[65]
Host-gut microbiota-xenobiotic interaction
Apart from carbohydrates, gut microbiota can also metabolize other xenobiotics such as drugs, phytochemicals, and food toxicants. More than 30 drugs have been shown to be metabolized by gut microbiota.[66] The microbial metabolism of drugs can sometimes inactivate the drug.[67]
Gut-brain axis
The gut-brain axis is the biochemical signaling that takes place between the gastrointestinal tract and the central nervous system.[54] That term has been expanded to include the role of the gut flora in the interplay; the term "microbiome-gut-brain axis" is sometimes used to describe paradigms explicitly including the gut flora.[54][68][69] Broadly defined, the gut-brain axis includes the central nervous system, neuroendocrine and neuroimmune systems including the hypothalamic–pituitary–adrenal axis (HPA axis), sympathetic and parasympathetic arms of the autonomic nervous system including the enteric nervous system, the vagus nerve, and the gut microbiota.[54][69]
A systematic review from 2016 examined the preclinical and small human trials that have been conducted with certain commercially available strains of probiotic bacteria and found that among those tested, Bifidobacterium and Lactobacillus genera (B. longum, B. breve, B. infantis, L. helveticus, L. rhamnosus, L. plantarum, and L. casei), had the most potential to be useful for certain central nervous system disorders.[8]
Alterations in flora balance
Effects of antibiotic use
Altering the numbers of gut bacteria, for example by taking broad-spectrum antibiotics, may affect the host's health and ability to digest food.[70] Antibiotics can cause antibiotic-associated diarrhea (AAD) by irritating the bowel directly, changing the levels of gut flora, or allowing pathogenic bacteria to grow.[11] Another harmful effect of antibiotics is the increase in numbers of antibiotic-resistant bacteria found after their use, which, when they invade the host, cause illnesses that are difficult to treat with antibiotics.[70]
Changing the numbers and species of gut flora can reduce the body's ability to ferment carbohydrates and metabolize bile acids and may cause diarrhea. Carbohydrates that are not broken down may absorb too much water and cause runny stools, or lack of SCFAs produced by gut flora could cause diarrhea.[11]
A reduction in levels of native bacterial species also disrupts their ability to inhibit the growth of harmful species such as C. difficile and Salmonella kedougou, and these species can get out of hand, though their overgrowth may be incidental and not be the true cause of diarrhea.[9][11][70] Emerging treatment protocols for C. difficile infections involve fecal microbiota transplantation of donor feces. (see Fecal transplant). Initial reports of treatment describe success rates of 90%, with few side effects. Efficacy is speculated to result from restoring bacterial balances of bacteroides and firmicutes classes of bacteria.[71]
Gut flora composition also changes in severe illnesses, due not only to antibiotic use but also to such factors as ischemia of the gut, failure to eat, and immune compromise. Negative effects from this have led to interest in selective digestive tract decontamination (SDD), a treatment to kill only pathogenic bacteria and allow the re-establishment of healthy ones.[72]
Antibiotics alter the population of the gastrointestinal (GI) tract microbiota, may change the intra-community metabolic interactions, modify caloric intake by using carbohydrates, and globally affects host metabolic, hormonal and immune homeostasis.[73]
There is reasonable evidence that taking probiotics containing Lactobacillus species may help prevent antibiotic-associated diarrhea and that taking probiotics with Saccharomyces (e.g., Saccharomyces boulardii) may help to prevent Clostridium difficile infection following systemic antibiotic treatment.[74]
Pregnancy
Women's gut microbiota change as pregnancy advances, with the changes similar to those seen in metabolic syndromes such as diabetes. The change in gut flora causes no ill effects. The newborn's gut biota resemble the mother's first-trimester samples. The diversity of the flora decreases from the first to third trimester, as the numbers of certain species go up.[45][75]
Probiotics, prebiotics, synbiotics, and pharmabiotics
Probiotics are microorganisms that are believed to provide health benefits when consumed.[76][77] With regard to gut flora, prebiotics are typically non-digestible, fiber compounds that pass undigested through the upper part of the gastrointestinal tract and stimulate the growth or activity of advantageous gut flora by acting as substrate for them.[30][78]
Synbiotics refers to food ingredients or dietary supplements combining probiotics and prebiotics in a form of synergism.[79]
The term "pharmabiotics" is used in various ways, to mean: pharmaceutical formulations (standardized manufacturing that can obtain regulatory approval as a drug) of probiotics, prebiotics, or synbiotics;[80] probiotics that have been genetically engineered or otherwise optimized for best performance (shelf life, survival in the digestive tract, etc.);[81] and the natural products of gut flora metabolism (vitamins, etc.).[82]
There is some evidence that treatment with some probiotic strains of bacteria may be effective in irritable bowel syndrome and chronic idiopathic constipation. Those organisms most likely to result in a decrease of symptoms have included:
- Enterococcus faecium
- Lactobacillus plantarum
- Lactobacillus rhamnosus
- Propionibacterium freudenreichii
- Bifidobacterium breve
- Lactobacillus reuteri
- Lactobacillus salivarius
- Bifidobacterium infantis
- Streptococcus thermophilus[83][84][85]
Research
Tests for whether non-antibiotic drugs may impact human gut-associated bacteria were performed by in vitro analysis on more than 1000 marketed drugs against 40 gut bacterial strains, demonstrating that 24% of the drugs inhibited the growth of at least one of the bacterial strains.[86]
Role in disease
Bacteria in the digestive tract can contribute to and be affected by the disease in various ways. The presence or overabundance of some kinds of bacteria may contribute to inflammatory disorders such as inflammatory bowel disease.[9] Additionally, metabolites from certain members of the gut flora may influence host signalling pathways, contributing to disorders such as obesity and colon cancer.[9] Alternatively, in the event of a breakdown of the gut epithelium, the intrusion of gut flora components into other host compartments can lead to sepsis.[9]
Ulcers
Helicobacter pylori can cause stomach ulcers by crossing the epithelial lining of the stomach. Here the body produces an immune response. During this response, parietal cells are stimulated and release extra hydrochloric acid (HCl+) into the stomach. However, the response does not stimulate the mucus-secreting cells that protect and line the epithelium of the stomach. The extra acid sears holes into the epithelial lining of the stomach, resulting in stomach ulcers.[35]
Bowel perforation
Normally-commensal bacteria can harm the host if they extrude from the intestinal tract.[4][5] Translocation, which occurs when bacteria leave the gut through its mucosal lining, can occur in a number of different diseases.[5] If the gut is perforated, bacteria invade the interstitium, causing a potentially fatal infection.[2]:715
Inflammatory bowel diseases
The two main types of inflammatory bowel diseases, Crohn's disease and ulcerative colitis, are chronic inflammatory disorders of the gut; the causes of these disease are unknown and issues with the gut flora and its relationship with the host have been implicated in these conditions.[7][87][88][89] Additionally, it appears that interactions of gut flora with the gut-brain axis have a role in IBD, with physiological stress mediated through the hypothalamic–pituitary–adrenal axis driving changes to intestinal epithelium and the gut flora in turn releasing factors and metabolites that trigger signaling in the enteric nervous system and the vagus nerve.[1]
The diversity of gut flora appears to be significantly diminished in people with inflammatory bowel diseases compared to healthy people; additionally, in people with ulcerative colitis, Proteobacteria and Actinobacteria appear to dominate; in people with Crohn's, Enterococcus faecium and several Proteobacteria appear to be over-represented.[1]
There is reasonable evidence that correcting gut flora imbalances by taking probiotics with Lactobacilli and Bifidobacteria can reduce visceral pain and gut inflammation in IBD.[74]
Irritable bowel syndrome
Irritable bowel syndrome is a result of stress and chronic activation of the HPA axis; its symptoms include abdominal pain, changes in bowel movements, and an increase in proinflammatory cytokines. Overall, studies have found that the luminal and mucosal microbiota are changed in irritable bowel syndrome individuals, and these changes can relate to the type of irritation such as diarrhea or constipation. Also, there is a decrease in the diversity of the microbiome with low levels of fecal Lactobacilli and Bifidobacteria, high levels of facultative anaerobic bacteria such as Escherichia coli, and increased ratios of Firmicutes: Bacteroidetes.[69]
Other inflammatory or autoimmune conditions
Allergy, asthma, and diabetes mellitus are autoimmune and inflammatory disorders of unknown cause, but have been linked to imbalances in the gut flora and its relationship with the host.[90] As of 2016 it was not clear if changes to the gut flora cause these auto-immune and inflammatory disorders or are a product of or adaptation to them.[90][91]
Asthma
With asthma, two hypotheses have been posed to explain its rising prevalence in the developed world. The hygiene hypothesis posits that children in the developed world are not exposed to enough microbes and thus may contain lower prevalence of specific bacterial taxa that play protective roles.[92] The second hypothesis focuses on the Western pattern diet, which lacks whole grains and fiber and has an overabundance of simple sugars.[90] Both hypotheses converge on the role of short-chain fatty acids (SCFAs) in immunomodulation. These bacterial fermentation metabolites are involved in immune signalling that prevents the triggering of asthma and lower SCFA levels are associated with the disease.[92][93] Lacking protective genera such as Lachnospira, Veillonella, Rothia and Faecalibacterium has been linked to reduced SCFA levels.[92] Further, SCFAs are the product of bacterial fermentation of fiber, which is low in the Western pattern diet.[90][93] SCFAs offer a link between gut flora and immune disorders, and as of 2016, this was an active area of research.[90] Similar hypotheses have also been posited for the rise of food and other allergies.[94]
Diabetes mellitus type 1
The connection between the gut microbiota and diabetes mellitus type 1 has also been linked to anti-inflammatory SCFAs, such as butyrate, regulating the associated low-grade inflammatory state by controlling gut permeability.[95] Additionally, butyrate has also been shown to decrease insulin resistance, suggesting gut communities low in butyrate-producing microbes may increase chances of acquiring diabetes mellitus type 2.[96]
Obesity and metabolic syndrome
The gut flora has also been implicated in obesity and metabolic syndrome due to the key role it plays in the digestive process; the Western pattern diet appears to drive and maintain changes in the gut flora that in turn change how much energy is derived from food and how that energy is used.[89][97] One aspect of a healthy diet that is often lacking in the Western-pattern diet is fiber and other complex carbohydrates that a healthy gut flora require flourishing; changes to gut flora in response to a Western-pattern diet appear to increase the amount of energy generated by the gut flora which may contribute to obesity and metabolic syndrome.[74] There is also evidence that microbiota influence eating behaviours based on the preferences of the microbiota, which can lead to the host consuming more food eventually resulting in obesity. It has generally been observed that with higher gut microbiome diversity, the microbiota will spend energy and resources on competing with other microbiota and less on manipulating the host. The opposite is seen with lower gut microbiome diversity, and these microbiotas may work together to create host food cravings.[37]
Additionally, the liver plays a dominant role in blood glucose homeostasis by maintaining a balance between the uptake and storage of glucose through the metabolic pathways of glycogenesis and gluconeogenesis. Intestinal lipids regulate glucose homeostasis involving a gut-brain-liver axis. The direct administration of lipids into the upper intestine increases the long chain fatty acyl-coenzyme A (LCFA-CoA) levels in the upper intestines and suppresses glucose production even under subdiaphragmatic vagotomy or gut vagal deafferentation. This interrupts the neural connection between the brain and the gut and blocks the upper intestinal lipids' ability to inhibit glucose production. The gut-brain-liver axis and gut microbiota composition can regulate the glucose homeostasis in the liver and provide potential therapeutic methods to treat obesity and diabetes.[98]
Just as gut flora can function in a feedback loop that can drive the development of obesity, there is evidence that restricting intake of calories (i.e., dieting) can drive changes to the composition of the gut flora.[89]
Liver disease
As the liver is fed directly by the portal vein, whatever crosses the intestinal epithelium and the intestinal mucosal barrier enters the liver, as do cytokines generated there.[99] Dysbiosis in the gut flora has been linked with the development of cirrhosis and non-alcoholic fatty liver disease.[99]
Cancer
Some genera of bacteria, such as Bacteroides and Clostridium, have been associated with an increase in tumor growth rate, while other genera, such as Lactobacillus and Bifidobacteria, are known to prevent tumor formation.[9] As of December 2017 there was preliminary and indirect evidence that gut microbiota might mediate response to PD-1 inhibitors; the mechanism was unknown.[100]
Neuropsychiatric
Interest in the relationship between gut flora and neuropsychiatric issues was sparked by a 2004 study showing that germ-free mice showed an exaggerated HPA axis response to stress compared to non-GF laboratory mice.[54] As of January 2016, most of the work that has been done on the role of gut flora in the gut-brain axis had been conducted in animals, or characterizing the various neuroactive compounds that gut flora can produce, and studies with humans measuring differences between people with various psychiatric and neurological differences, or changes to gut flora in response to stress, or measuring effects of various probiotics (dubbed "psychobiotics in this context), had generally been small and could not be generalized; whether changes to gut flora are a result of disease, a cause of disease, or both in any number of possible feedback loops in the gut-brain axis, remained unclear.[54][74]
A systematic review from 2016 examined the preclinical and small human trials that have been conducted with certain commercially available strains of probiotic bacteria and found that among those tested, Bifidobacterium and Lactobacillus genera (B. longum, B. breve, B. infantis, L. helveticus, L. rhamnosus, L. plantarum, and L. casei), had the most potential to be useful for certain central nervous system disorders.[8]
Other animals
Aside from mammals, some insects also possess complex and diverse gut microbiota that play key nutritional roles.[101] Microbial communities associated termites can constitute a majority of the weight of the individuals and perform important roles in the digestion of lignocellulose and nitrogen fixation.[102] These communities are host-specific, and closely related insect species share comparable similarities in gut microbiota composition.[103][104] In cockroaches, gut microbiota have been shown to assemble in a deterministic fashion, irrespective of the inoculum;[105] the reason for this host-specific assembly remains unclear. Bacterial communities associated with insects like termites and cockroaches are determined by a combination of forces, primarily diet, but there is some indication that host phylogeny may also be playing a role in the selection of lineages.[103][104]
For more than 51 years it has been known that the administration of low doses of antibacterial agents promotes the growth of farm animals to increase weight gain.[73]
In a study performed on mice by Ilseung Cho,[73] the ratio of Firmicutes and Lachnospiraceae was significantly elevated in animals treated with subtherapeutic doses of different antibiotics. By analyzing the caloric content of faeces and the concentration of small chain fatty acids (SCFAs) in the GI tract, they concluded that the changes in the composition of microbiota lead to an increased capacity to extract calories from otherwise indigestible constituents, and to an increased production of SCFAs. These findings provide evidence that antibiotics perturb not only the composition of the GI microbiome but also its metabolic capabilities, specifically with respect to SCFAs.[73]
See also
- Colonisation resistance
- List of human flora
- List of microbiota species of the lower reproductive tract of women
- Skin flora
- Verotoxin-producing Escherichia coli
Sources and notes
- ↑ 1.0 1.1 1.2 Saxena, R.; Sharma, V.K (2016). "A Metagenomic Insight Into the Human Microbiome: Its Implications in Health and Disease". Medical and Health Genomics. Elsevier Science. p. 117. doi:10.1016/B978-0-12-420196-5.00009-5. ISBN 978-0-12-799922-7. https://books.google.com/books?id=3ylOBQAAQBAJ&pg=PA117.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Sherwood, Linda; Willey, Joanne; Woolverton, Christopher (2013). Prescott's Microbiology (9th ed.). New York: McGraw Hill. pp. 713–21. ISBN 9780073402406. OCLC 886600661. https://books.google.com/books?id=sBCSRAAACAAJ.
- ↑ 3.0 3.1 3.2 3.3 3.4 Quigley, E. M (2013). "Gut bacteria in health and disease". Gastroenterology & hepatology 9 (9): 560–9. PMID 24729765.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 Sommer, Felix; Bäckhed, Fredrik (2013). "The gut microbiota — masters of host development and physiology". Nature Reviews Microbiology 11 (4): 227–38. doi:10.1038/nrmicro2974. PMID 23435359.
- ↑ 5.0 5.1 5.2 5.3 Faderl, Martin; Noti, Mario; Corazza, Nadia; Mueller, Christoph (2015). "Keeping bugs in check: The mucus layer as a critical component in maintaining intestinal homeostasis". IUBMB Life 67 (4): 275–85. doi:10.1002/iub.1374. PMID 25914114.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Clarke, Gerard; Stilling, Roman M; Kennedy, Paul J; Stanton, Catherine; Cryan, John F; Dinan, Timothy G (2014). "Minireview: Gut Microbiota: The Neglected Endocrine Organ". Molecular Endocrinology 28 (8): 1221–38. doi:10.1210/me.2014-1108. PMID 24892638.
- ↑ 7.0 7.1 7.2 Shen, Sj; Wong, Connie HY (2016). "Bugging inflammation: Role of the gut microbiota". Clinical & Translational Immunology 5 (4): e72. doi:10.1038/cti.2016.12. PMID 27195115.
- ↑ 8.0 8.1 8.2 Wang, Huiying; Lee, In-Seon; Braun, Christoph; Enck, Paul (2016). "Effect of Probiotics on Central Nervous System Functions in Animals and Humans: A Systematic Review". Journal of Neurogastroenterology and Motility 22 (4): 589–605. doi:10.5056/jnm16018. PMID 27413138.
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 9.12 9.13 9.14 9.15 Guarner, F; Malagelada, J (2003). "Gut flora in health and disease". The Lancet 361 (9356): 512–19. doi:10.1016/S0140-6736(03)12489-0. PMID 12583961.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 Sears, Cynthia L. (2005). "A dynamic partnership: Celebrating our gut flora". Anaerobe 11 (5): 247–51. doi:10.1016/j.anaerobe.2005.05.001. PMID 16701579.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 11.9 Beaugerie, Laurent; Petit, Jean-Claude (2004). "Antibiotic-associated diarrhoea". Best Practice & Research Clinical Gastroenterology 18 (2): 337–52. doi:10.1016/j.bpg.2003.10.002. PMID 15123074.
- ↑ Stephen, A. M.; Cummings, J. H. (1980). "The Microbial Contribution to Human Faecal Mass". Journal of Medical Microbiology 13 (1): 45–56. doi:10.1099/00222615-13-1-45. PMID 7359576.
- ↑ Lozupone, Catherine A.; Stombaugh, Jesse I.; Gordon, Jeffrey I.; Jansson, Janet K.; Knight, Rob (2012). "Diversity, stability and resilience of the human gut microbiota". Nature 489 (7415): 220–30. doi:10.1038/nature11550. PMID 22972295. Bibcode: 2012Natur.489..220L.
- ↑ Qin, Junjie; Li, Ruiqiang; Raes, Jeroen; Arumugam, Manimozhiyan; Burgdorf, Kristoffer Solvsten; Manichanh, Chaysavanh; Nielsen, Trine; Pons, Nicolas et al. (2010). "A human gut microbial gene catalogue established by metagenomic sequencing". Nature 464 (7285): 59–65. doi:10.1038/nature08821. PMID 20203603. Bibcode: 2010Natur.464...59..
- ↑ Shanahan, Fergus (2002). "The host–microbe interface within the gut". Best Practice & Research Clinical Gastroenterology 16 (6): 915–31. doi:10.1053/bega.2002.0342. PMID 12473298.
- ↑ Tap, Julien; Mondot, Stanislas; Levenez, Florence; Pelletier, Eric; Caron, Christophe; Furet, Jean-Pierre; Ugarte, Edgardo; Muñoz-Tamayo, Rafael et al. (2009). "Towards the human intestinal microbiota phylogenetic core". Environmental Microbiology 11 (10): 2574–84. doi:10.1111/j.1462-2920.2009.01982.x. PMID 19601958.
- ↑ 17.0 17.1 O'Hara, Ann M; Shanahan, Fergus (2006). "The gut flora as a forgotten organ". EMBO Reports 7 (7): 688–93. doi:10.1038/sj.embor.7400731. PMID 16819463.
- ↑ Khanna, Sahil; Tosh, Pritish K (2014). "A Clinician's Primer on the Role of the Microbiome in Human Health and Disease". Mayo Clinic Proceedings 89 (1): 107–14. doi:10.1016/j.mayocp.2013.10.011. PMID 24388028.
- ↑ 19.0 19.1 Cui, Lijia; Morris, Alison; Ghedin, Elodie (2013). "The human mycobiome in health and disease". Genome Medicine 5 (7): 63. doi:10.1186/gm467. PMID 23899327.
- ↑ Erdogan, Askin; Rao, Satish S. C (2015). "Small Intestinal Fungal Overgrowth". Current Gastroenterology Reports 17 (4). doi:10.1007/s11894-015-0436-2.
- ↑ 21.0 21.1 Arumugam, Manimozhiyan; Raes, Jeroen; Pelletier, Eric; Le Paslier, Denis; Yamada, Takuji; Mende, Daniel R.; Fernandes, Gabriel R.; Tap, Julien et al. (2011). "Enterotypes of the human gut microbiome". Nature 473 (7346): 174–80. doi:10.1038/nature09944. PMID 21508958. Bibcode: 2011Natur.473..174..
- ↑ 22.0 22.1 Wu, G. D.; Chen, J.; Hoffmann, C.; Bittinger, K.; Chen, Y.-Y.; Keilbaugh, S. A.; Bewtra, M.; Knights, D. et al. (2011). "Linking Long-Term Dietary Patterns with Gut Microbial Enterotypes". Science 334 (6052): 105–08. doi:10.1126/science.1208344. PMID 21885731. Bibcode: 2011Sci...334..105W.
- ↑ Zimmer, Carl (April 20, 2011). "Bacteria Divide People Into 3 Types, Scientists Say". The New York Times. https://www.nytimes.com/2011/04/21/science/21gut.html. Retrieved April 21, 2011. "a group of scientists now report just three distinct ecosystems in the guts of people they have studied."
- ↑ Knights, Dan; Ward, Tonya; McKinlay, Christopher; Miller, Hannah; Gonzalez, Antonio; McDonald, Daniel; Knight, Rob (8 October 2014). "Rethinking "Enterotypes"". Cell Host & Microbe 16 (4): 433–37. doi:10.1016/j.chom.2014.09.013. PMID 25299329.
- ↑ Kenneth Todar (2012). "The Normal Bacterial Flora of Humans". Todar's Online Textbook of Bacteriology. http://www.textbookofbacteriology.net/normalflora_3.html. Retrieved June 25, 2016.
- ↑ Quigley, Eamonn M.M; Quera, Rodrigo (2006). "Small Intestinal Bacterial Overgrowth: Roles of Antibiotics, Prebiotics, and Probiotics". Gastroenterology 130 (2): S78–90. doi:10.1053/j.gastro.2005.11.046. PMID 16473077.
- ↑ Food Microbiology. 2007. doi:10.1039/9781847557940. ISBN 978-0-85404-284-5.
- ↑ 28.0 28.1 University of Glasgow. 2005. The normal gut flora. Available through web archive. Accessed May 22, 2008
- ↑ 29.0 29.1 Steinhoff, U (2005). "Who controls the crowd? New findings and old questions about the intestinal microflora". Immunology Letters 99 (1): 12–16. doi:10.1016/j.imlet.2004.12.013. PMID 15894105.
- ↑ 30.0 30.1 30.2 30.3 30.4 30.5 Gibson, Glenn R (2004). "Fibre and effects on probiotics (the prebiotic concept)". Clinical Nutrition Supplements 1 (2): 25–31. doi:10.1016/j.clnu.2004.09.005.
- ↑ Miquel, S; Martín, R; Rossi, O; Bermúdez-Humarán, LG; Chatel, JM; Sokol, H; Thomas, M; Wells, JM et al. (2013). "Faecalibacterium prausnitzii and human intestinal health". Current Opinion in Microbiology 16 (3): 255–61. doi:10.1016/j.mib.2013.06.003. PMID 23831042.
- ↑ Nash, Andrea K; Auchtung, Thomas A; Wong, Matthew C; Smith, Daniel P; Gesell, Jonathan R; Ross, Matthew C; Stewart, Christopher J; Metcalf, Ginger A et al. (2017). "The gut mycobiome of the Human Microbiome Project healthy cohort". Microbiome 5. doi:10.1186/s40168-017-0373-4.
- ↑ Scarpellini, Emidio; Ianiro, Gianluca; Attili, Fabia; Bassanelli, Chiara; De Santis, Adriano; Gasbarrini, Antonio (2015). "The human gut microbiota and virome: Potential therapeutic implications". Digestive and Liver Disease 47 (12): 1007–12. doi:10.1016/j.dld.2015.07.008. PMID 26257129.
- ↑ Ley, Ruth E (2010). "Obesity and the human microbiome". Current Opinion in Gastroenterology 26 (1): 5–11. doi:10.1097/MOG.0b013e328333d751. PMID 19901833.
- ↑ 35.0 35.1 Gerritsen, Jacoline; Smidt, Hauke; Rijkers, Ger; de Vos, Willem (27 May 2011). "Intestinal microbiota in human health and disease: the impact of probiotics". Genes & Nutritions 6 (3): 209–40. doi:10.1007/s12263-011-0229-7. PMID 21617937.
- ↑ 36.0 36.1 36.2 36.3 36.4 36.5 Yatsunenko, T.; Rey, F. E.; Manary, M. J.; Trehan, I.; Dominguez-Bello, M. G.; Contreras, M.; Magris, M.; Hidalgo, G. et al. (2012). "Human gut microbiome viewed across age and geography". Nature 486 (7402): 222–27. doi:10.1038/nature11053. PMID 22699611. Bibcode: 2012Natur.486..222Y.
- ↑ 37.0 37.1 37.2 Alcock, Joe; Maley, Carlo C; Aktipis, C. Athena (2014). "Is eating behavior manipulated by the gastrointestinal microbiota? Evolutionary pressures and potential mechanisms". BioEssays 36 (10): 940–9. doi:10.1002/bies.201400071. PMID 25103109.
- ↑ Jonkers, Daisy M.A.E. (2016). "Microbial perturbations and modulation in conditions associated with malnutrition and malabsorption". Best Practice & Research Clinical Gastroenterology 30 (2): 161–72. doi:10.1016/j.bpg.2016.02.006. PMID 27086883.
- ↑ Million, Matthieu; Diallo, Aldiouma; Raoult, Didier (2016). "Gut microbiota and malnutrition". Microbial Pathogenesis 106: 127–138. doi:10.1016/j.micpath.2016.02.003. PMID 26853753. https://www.researchgate.net/profile/Matthieu_Million/publication/293017549_Gut_Microbiota_and_Malnutrition/links/56c748d608ae5488f0d2c94c.pdf.
- ↑ Rytter, Maren Johanne Heilskov; Kolte, Lilian; Briend, André; Friis, Henrik; Christensen, Vibeke Brix (2014). "The Immune System in Children with Malnutrition—A Systematic Review". PLoS ONE 9 (8): e105017. doi:10.1371/journal.pone.0105017. PMID 25153531. Bibcode: 2014PLoSO...9j5017R.
- ↑ De Filippo, C; Cavalieri, D; Di Paola, M; Ramazzotti, M; Poullet, J. B; Massart, S; Collini, S; Pieraccini, G et al. (2010). "Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa". Proceedings of the National Academy of Sciences 107 (33): 14691–6. doi:10.1073/pnas.1005963107. PMID 20679230. Bibcode: 2010PNAS..10714691D.
- ↑ Turroni, Francesca; Peano, Clelia; Pass, Daniel A; Foroni, Elena; Severgnini, Marco; Claesson, Marcus J; Kerr, Colm; Hourihane, Jonathan et al. (2012). "Diversity of Bifidobacteria within the Infant Gut Microbiota". PLoS ONE 7 (5): e36957. doi:10.1371/journal.pone.0036957. PMID 22606315. Bibcode: 2012PLoSO...736957T.
- ↑ Perez-Muñoz, Maria Elisa; Arrieta, Marie-Claire; Ramer-Tait, Amanda E; Walter, Jens (2017). "A critical assessment of the 'sterile womb' and 'in utero colonization' hypotheses: Implications for research on the pioneer infant microbiome". Microbiome 5 (1): 48. doi:10.1186/s40168-017-0268-4. PMID 28454555.
- ↑ 44.0 44.1 Matamoros, Sebastien; Gras-Leguen, Christele; Le Vacon, Françoise; Potel, Gilles; de la Cochetiere, Marie-France (2013). "Development of intestinal microbiota in infants and its impact on health". Trends in Microbiology 21 (4): 167–73. doi:10.1016/j.tim.2012.12.001. PMID 23332725.
- ↑ 45.0 45.1 45.2 45.3 45.4 45.5 45.6 Mueller, Noel T.; Bakacs, Elizabeth; Combellick, Joan; Grigoryan, Zoya; Dominguez-Bello, Maria G. (2015). "The infant microbiome development: mom matters". Trends in Molecular Medicine 21 (2): 109–17. doi:10.1016/j.molmed.2014.12.002. PMID 25578246.
- ↑ Jiménez, Esther; Fernández, Leonides; Marín, María L; Martín, Rocío; Odriozola, Juan M; Nueno-Palop, Carmen; Narbad, Arjan; Olivares, Mónica et al. (2005). "Isolation of Commensal Bacteria from Umbilical Cord Blood of Healthy Neonates Born by Cesarean Section". Current Microbiology 51 (4): 270–4. doi:10.1007/s00284-005-0020-3. PMID 16187156.
- ↑ Collado, Maria Carmen; Rautava, Samuli; Aakko, Juhani; Isolauri, Erika; Salminen, Seppo (2016). "Human gut colonisation may be initiated in utero by distinct microbial communities in the placenta and amniotic fluid". Scientific Reports 6. doi:10.1038/srep23129. Bibcode: 2016NatSR...623129C.
- ↑ Jiménez, Esther; Marín, María L.; Martín, Rocío; Odriozola, Juan M.; Olivares, Mónica; Xaus, Jordi; Fernández, Leonides; Rodríguez, Juan M. (2008). "Is meconium from healthy newborns actually sterile?". Research in Microbiology 159 (3): 187–93. doi:10.1016/j.resmic.2007.12.007. PMID 18281199.
- ↑ Perez-Muñoz, Maria Elisa; Arrieta, Marie-Claire; Ramer-Tait, Amanda E; Walter, Jens (2017). "A critical assessment of the "sterile womb" and "in utero colonization" hypotheses: Implications for research on the pioneer infant microbiome". Microbiome 5. doi:10.1186/s40168-017-0268-4.
- ↑ Adlerberth, I; Wold, AE (2009). "Establishment of the gut microbiota in Western infants". Acta Paediatrica 98 (2): 229–38. doi:10.1111/j.1651-2227.2008.01060.x. PMID 19143664.
- ↑ Coppa, G.V; Zampini, L; Galeazzi, T; Gabrielli, O (2006). "Prebiotics in human milk: A review". Digestive and Liver Disease 38: S291–4. doi:10.1016/S1590-8658(07)60013-9. PMID 17259094.
- ↑ Fanaro, S; Chierici, R; Guerrini, P; Vigi, V (2007). "Intestinal microflora in early infancy: Composition and development". Acta Paediatrica 92 (441): 48–55. doi:10.1111/j.1651-2227.2003.tb00646.x. PMID 14599042.
- ↑ Yassour, Moran; Vatanen, Tommi; Siljander, Heli; Hämäläinen, Anu-Maaria; Härkönen, Taina; Ryhänen, Samppa J; Franzosa, Eric A; Vlamakis, Hera et al. (2016). "Natural history of the infant gut microbiome and impact of antibiotic treatment on bacterial strain diversity and stability". Science Translational Medicine 8 (343): 343ra81. doi:10.1126/scitranslmed.aad0917. PMID 27306663.
- ↑ 54.0 54.1 54.2 54.3 54.4 54.5 Wang, Yan; Kasper, Lloyd H (2014). "The role of microbiome in central nervous system disorders". Brain, Behavior, and Immunity 38: 1–12. doi:10.1016/j.bbi.2013.12.015. PMID 24370461.
- ↑ 55.0 55.1 Yoon, My Young; Lee, Keehoon; Yoon, Sang Sun (2014). "Protective role of gut commensal microbes against intestinal infections". Journal of Microbiology 52 (12): 983–9. doi:10.1007/s12275-014-4655-2. PMID 25467115.
- ↑ Reinoso Webb, Cynthia; Koboziev, Iurii; Furr, Kathryn L; Grisham, Matthew B (2016). "Protective and pro-inflammatory roles of intestinal bacteria". Pathophysiology 23 (2): 67–80. doi:10.1016/j.pathophys.2016.02.002. PMID 26947707.
- ↑ Mantis, N J; Rol, N; Corthésy, B (2011). "Secretory IgA's complex roles in immunity and mucosal homeostasis in the gut". Mucosal Immunology 4 (6): 603–11. doi:10.1038/mi.2011.41. PMID 21975936.
- ↑ 58.0 58.1 Peterson, Lance W; Artis, David (2014). "Intestinal epithelial cells: Regulators of barrier function and immune homeostasis". Nature Reviews Immunology 14 (3): 141–53. doi:10.1038/nri3608. PMID 24566914.
- ↑ 59.0 59.1 Honda, Kenya; Littman, Dan R (2016). "The microbiota in adaptive immune homeostasis and disease". Nature 535 (7610): 75–84. doi:10.1038/nature18848. PMID 27383982. Bibcode: 2016Natur.535...75H.
- ↑ 60.0 60.1 Levy, M.; Thaiss, C.A.; Elinav, E. (2016). "Metabolites: messengers between the microbiota and the immune system". Genes & Development 30 (14): 1589–97. doi:10.1101/gad.284091.116. PMID 27474437.
- ↑ 61.0 61.1 61.2 61.3 61.4 61.5 61.6 61.7 61.8 "Microbial metabolism of dietary components to bioactive metabolites: opportunities for new therapeutic interventions". Genome Med 8 (1): 46. April 2016. doi:10.1186/s13073-016-0296-x. PMID 27102537. "Lactobacillus spp. convert tryptophan to indole-3-aldehyde (I3A) through unidentified enzymes [125]. Clostridium sporogenes convert tryptophan to IPA [6], likely via a tryptophan deaminase. ... IPA also potently scavenges hydroxyl radicals".
Table 2: Microbial metabolites: their synthesis, mechanisms of action, and effects on health and disease
Figure 1: Molecular mechanisms of action of indole and its metabolites on host physiology and disease - ↑ "Metabolomics analysis reveals large effects of gut microflora on mammalian blood metabolites". Proc. Natl. Acad. Sci. U.S.A. 106 (10): 3698–3703. March 2009. doi:10.1073/pnas.0812874106. PMID 19234110. "Production of IPA was shown to be completely dependent on the presence of gut microflora and could be established by colonization with the bacterium Clostridium sporogenes.".
IPA metabolism diagram - ↑ "3-Indolepropionic acid". University of Alberta. http://www.hmdb.ca/metabolites/HMDB02302. Retrieved 12 June 2018. "Indole-3-propionate (IPA), a deamination product of tryptophan formed by symbiotic bacteria in the gastrointestinal tract of mammals and birds. 3-Indolepropionic acid has been shown to prevent oxidative stress and death of primary neurons and neuroblastoma cells exposed to the amyloid beta-protein in the form of amyloid fibrils, one of the most prominent neuropathologic features of Alzheimer's disease. 3-Indolepropionic acid also shows a strong level of neuroprotection in two other paradigms of oxidative stress. (PMID 10419516) ... More recently it has been found that higher indole-3-propionic acid levels in serum/plasma are associated with reduced likelihood of type 2 diabetes and with higher levels of consumption of fiber-rich foods (PMID 28397877)
Origin: • Endogenous • Microbial" - ↑ "Potent neuroprotective properties against the Alzheimer beta-amyloid by an endogenous melatonin-related indole structure, indole-3-propionic acid". J. Biol. Chem. 274 (31): 21937–21942. July 1999. doi:10.1074/jbc.274.31.21937. PMID 10419516. "[Indole-3-propionic acid (IPA)] has previously been identified in the plasma and cerebrospinal fluid of humans, but its functions are not known. ... In kinetic competition experiments using free radical-trapping agents, the capacity of IPA to scavenge hydroxyl radicals exceeded that of melatonin, an indoleamine considered to be the most potent naturally occurring scavenger of free radicals. In contrast with other antioxidants, IPA was not converted to reactive intermediates with pro-oxidant activity.".
- ↑ Rajilić-Stojanović, Mirjana; De Vos, Willem M (2014). "The first 1000 cultured species of the human gastrointestinal microbiota". FEMS Microbiology Reviews 38 (5): 996–1047. doi:10.1111/1574-6976.12075. PMID 24861948.
- ↑ Sousa, Tiago; Paterson, Ronnie; Moore, Vanessa; Carlsson, Anders; Abrahamsson, Bertil; Basit, Abdul W (2008). "The gastrointestinal microbiota as a site for the biotransformation of drugs". International Journal of Pharmaceutics 363 (1–2): 1–25. doi:10.1016/j.ijpharm.2008.07.009. PMID 18682282.
- ↑ Haiser, H. J; Gootenberg, D. B; Chatman, K; Sirasani, G; Balskus, E. P; Turnbaugh, P. J (2013). "Predicting and Manipulating Cardiac Drug Inactivation by the Human Gut Bacterium Eggerthella lenta". Science 341 (6143): 295–8. doi:10.1126/science.1235872. PMID 23869020. Bibcode: 2013Sci...341..295H.
- ↑ Mayer, E. A; Knight, R; Mazmanian, S. K; Cryan, J. F; Tillisch, K (2014). "Gut Microbes and the Brain: Paradigm Shift in Neuroscience". Journal of Neuroscience 34 (46): 15490–6. doi:10.1523/JNEUROSCI.3299-14.2014. PMID 25392516.
- ↑ 69.0 69.1 69.2 Dinan, Timothy G; Cryan, John F (2015). "The impact of gut microbiota on brain and behaviour". Current Opinion in Clinical Nutrition and Metabolic Care 18 (6): 552–8. doi:10.1097/MCO.0000000000000221. PMID 26372511.
- ↑ 70.0 70.1 70.2 Carman, Robert J.; Simon, Mary Alice; Fernández, Haydée; Miller, Margaret A.; Bartholomew, Mary J. (2004). "Ciprofloxacin at low levels disrupts colonization resistance of human fecal microflora growing in chemostats". Regulatory Toxicology and Pharmacology 40 (3): 319–26. doi:10.1016/j.yrtph.2004.08.005. PMID 15546686.
- ↑ Brandt, Lawrence J.; Borody, Thomas Julius; Campbell, Jordana (2011). "Endoscopic Fecal Microbiota Transplantation". Journal of Clinical Gastroenterology 45 (8): 655–57. doi:10.1097/MCG.0b013e3182257d4f. PMID 21716124.
- ↑ Knight, DJW; Girling, KJ (2003). "Gut flora in health and disease". The Lancet 361 (9371): 512–19. doi:10.1016/S0140-6736(03)13438-1. PMID 12781578.
- ↑ 73.0 73.1 73.2 73.3 Cho, I.; Yamanishi, S.; Cox, L.; Methé, B. A.; Zavadil, J.; Li, K.; Gao, Z.; Mahana, D. et al. (2012). "Antibiotics in early life alter the murine colonic microbiome and adiposity". Nature 488 (7413): 621–26. doi:10.1038/nature11400. PMID 22914093. Bibcode: 2012Natur.488..621C.
- ↑ 74.0 74.1 74.2 74.3 Schneiderhan, J; Master-Hunter, T; Locke, A (2016). "Targeting gut flora to treat and prevent disease". The Journal of family practice 65 (1): 34–8. PMID 26845162.
- ↑ Baker, Monya (2012). "Pregnancy alters resident gut microbes". Nature. doi:10.1038/nature.2012.11118.
- ↑ Hill, Colin; Guarner, Francisco; Reid, Gregor; Gibson, Glenn R; Merenstein, Daniel J; Pot, Bruno; Morelli, Lorenzo; Canani, Roberto Berni et al. (2014). "The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic". Nature Reviews Gastroenterology & Hepatology 11 (8): 506–14. doi:10.1038/nrgastro.2014.66. PMID 24912386.
- ↑ Rijkers, Ger T; De Vos, Willem M; Brummer, Robert-Jan; Morelli, Lorenzo; Corthier, Gerard; Marteau, Philippe (2011). "Health benefits and health claims of probiotics: Bridging science and marketing". British Journal of Nutrition 106 (9): 1291–6. doi:10.1017/S000711451100287X. PMID 21861940.
- ↑ Hutkins, Robert W; Krumbeck, Janina A; Bindels, Laure B; Cani, Patrice D; Fahey, George; Goh, Yong Jun; Hamaker, Bruce; Martens, Eric C et al. (2016). "Prebiotics: Why definitions matter". Current Opinion in Biotechnology 37: 1–7. doi:10.1016/j.copbio.2015.09.001. PMID 26431716.
- ↑ Pandey, Kavita. R; Naik, Suresh. R; Vakil, Babu. V (2015). "Probiotics, prebiotics and synbiotics- a review". Journal of Food Science and Technology 52 (12): 7577–87. doi:10.1007/s13197-015-1921-1. PMID 26604335.
- ↑ Broeckx, Géraldine; Vandenheuvel, Dieter; Claes, Ingmar J.J; Lebeer, Sarah; Kiekens, Filip (2016). "Drying techniques of probiotic bacteria as an important step towards the development of novel pharmabiotics". International Journal of Pharmaceutics 505 (1–2): 303–18. doi:10.1016/j.ijpharm.2016.04.002. PMID 27050865.
- ↑ Sleator, Roy D; Hill, Colin (2009). "Rational Design of Improved Pharmabiotics". Journal of Biomedicine and Biotechnology 2009: 275287. doi:10.1155/2009/275287. PMID 19753318.
- ↑ Patterson, Elaine; Cryan, John F; Fitzgerald, Gerald F; Ross, R. Paul; Dinan, Timothy G; Stanton, Catherine (2014). "Gut microbiota, the pharmabiotics they produce and host health". Proceedings of the Nutrition Society 73 (4): 477–89. doi:10.1017/S0029665114001426. PMID 25196939.
- ↑ Ford, Alexander C; Quigley, Eamonn M M; Lacy, Brian E; Lembo, Anthony J; Saito, Yuri A; Schiller, Lawrence R; Soffer, Edy E; Spiegel, Brennan M R et al. (2014). "Efficacy of Prebiotics, Probiotics and Synbiotics in Irritable Bowel Syndrome and Chronic Idiopathic Constipation: Systematic Review and Meta-analysis". The American Journal of Gastroenterology 109 (10): 1547–61; quiz 1546, 1562. doi:10.1038/ajg.2014.202. PMID 25070051.
- ↑ Dupont, Andrew; Richards; Jelinek, Katherine A; Krill, Joseph; Rahimi, Erik; Ghouri, Yezaz (2014). "Systematic review of randomized controlled trials of probiotics, prebiotics, and synbiotics in inflammatory bowel disease". Clinical and Experimental Gastroenterology 7: 473–87. doi:10.2147/CEG.S27530. PMID 25525379.
- ↑ Yu, Cheng Gong; Huang, Qin (2013). "Recent progress on the role of gut microbiota in the pathogenesis of inflammatory bowel disease". Journal of Digestive Diseases 14 (10): 513–7. doi:10.1111/1751-2980.12087. PMID 23848393.
- ↑ Maier, Lisa; Pruteanu, Mihaela; Kuhn, Michael; Zeller, Georg; Telzerow, Anja; Anderson, Exene Erin; Brochado, Ana Rita; Fernandez, Keith Conrad et al. (2018). "Extensive impact of non-antibiotic drugs on human gut bacteria". Nature 555 (7698): 623–628. doi:10.1038/nature25979. PMID 29555994. Bibcode: 2018Natur.555..623M.
- ↑ Burisch, Johan; Jess, Tine; Martinato, Matteo; Lakatos, Peter L (2013). "The burden of inflammatory bowel disease in Europe". Journal of Crohn's and Colitis 7 (4): 322–37. doi:10.1016/j.crohns.2013.01.010. PMID 23395397.
- ↑ Blandino, G; Inturri, R; Lazzara, F; Di Rosa, M; Malaguarnera, L (2016). "Impact of gut microbiota on diabetes mellitus". Diabetes & Metabolism 42 (5): 303–315. doi:10.1016/j.diabet.2016.04.004. PMID 27179626.
- ↑ 89.0 89.1 89.2 Boulangé, Claire L; Neves, Ana Luisa; Chilloux, Julien; Nicholson, Jeremy K; Dumas, Marc-Emmanuel (2016). "Impact of the gut microbiota on inflammation, obesity, and metabolic disease". Genome Medicine 8. doi:10.1186/s13073-016-0303-2.
- ↑ 90.0 90.1 90.2 90.3 90.4 Shen, Sj; Wong, Connie HY (2016). "Bugging inflammation: Role of the gut microbiota". Clinical & Translational Immunology 5 (4): e72. doi:10.1038/cti.2016.12. PMID 27195115.
- ↑ Spiller, Robin (2016). "Irritable bowel syndrome: New insights into symptom mechanisms and advances in treatment". F1000Research 5: 780. doi:10.12688/f1000research.7992.1. PMID 27158477.
- ↑ 92.0 92.1 92.2 Arrieta, Marie-Claire; Stiemsma, Leah T; Dimitriu, Pedro A; Thorson, Lisa; Russell, Shannon; Yurist-Doutsch, Sophie; Kuzeljevic, Boris; Gold, Matthew J et al. (2015). "Early infancy microbial and metabolic alterations affect risk of childhood asthma". Science Translational Medicine 7 (307): 307ra152. doi:10.1126/scitranslmed.aab2271. PMID 26424567.
- ↑ 93.0 93.1 Stiemsma, Leah T; Turvey, Stuart E (2017). "Asthma and the microbiome: Defining the critical window in early life". Allergy, Asthma & Clinical Immunology 13: 3. doi:10.1186/s13223-016-0173-6. PMID 28077947.
- ↑ Ipci, Kagan; Altıntoprak, Niyazi; Muluk, Nuray Bayar; Senturk, Mehmet; Cingi, Cemal (2016). "The possible mechanisms of the human microbiome in allergic diseases". European Archives of Oto-Rhino-Laryngology 274 (2): 617–626. doi:10.1007/s00405-016-4058-6. PMID 27115907.
- ↑ Knip, Mikael; Siljander, Heli (2016). "The role of the intestinal microbiota in type 1 diabetes mellitus". Nature Reviews Endocrinology 12 (3): 154–67. doi:10.1038/nrendo.2015.218. PMID 26729037.
- ↑ Gao, Z; Yin, J; Zhang, J; Ward, R. E; Martin, R. J; Lefevre, M; Cefalu, W. T; Ye, J (2009). "Butyrate Improves Insulin Sensitivity and Increases Energy Expenditure in Mice". Diabetes 58 (7): 1509–17. doi:10.2337/db08-1637. PMID 19366864.
- ↑ Mazidi, Mohsen; Rezaie, Peyman; Kengne, Andre Pascal; Mobarhan, Majid Ghayour; Ferns, Gordon A (2016). "Gut microbiome and metabolic syndrome". Diabetes & Metabolic Syndrome: Clinical Research & Reviews 10 (2): S150–7. doi:10.1016/j.dsx.2016.01.024. PMID 26916014.
- ↑ Chen, Xiao; d'Souza, Roshan; Hong, Seong-Tshool (2013). "The role of gut microbiota in the gut-brain axis: Current challenges and perspectives". Protein & Cell 4 (6): 403–14. doi:10.1007/s13238-013-3017-x. PMID 23686721.
- ↑ 99.0 99.1 Minemura, Masami (2015). "Gut microbiota and liver diseases". World Journal of Gastroenterology 21 (6): 1691–702. doi:10.3748/wjg.v21.i6.1691. PMID 25684933.
- ↑ Syn, Nicholas L; Teng, Michele W L; Mok, Tony S K; Soo, Ross A (2017). "De-novo and acquired resistance to immune checkpoint targeting" (in en). The Lancet Oncology 18 (12): e731–41. doi:10.1016/s1470-2045(17)30607-1. PMID 29208439.
- ↑ Engel, P.; Moran, N. (2013). "The gut microbiota of insects–diversity in structure and function". FEMS Microbiology Reviews 37 (5): 699–735. doi:10.1111/1574-6976.12025. PMID 23692388.
- ↑ Brune, A. (2014). "Symbiotic digestion of lignocellulose in termite guts". Nature Reviews Microbiology 12 (3): 168–80. doi:10.1038/nrmicro3182. PMID 24487819.
- ↑ 103.0 103.1 Dietrich, C.; Köhler, T.; Brune, A. (2014). "The cockroach origin of the termite gut microbiota: patterns in bacterial community structure reflect major evolutionary events". Applied and Environmental Microbiology 80 (7): 2261–69. doi:10.1128/AEM.04206-13. PMID 24487532.
- ↑ 104.0 104.1 Mikaelyan, A.; Dietrich, C.; Köhler, T.; Poulsen, M.; Sillam-Dussès, D.; Brune, A. (2015). "Diet is the primary determinant of bacterial community structure in the guts of higher termites". Molecular Ecology 24 (20): 5824–95. doi:10.1111/mec.13376. PMID 26348261.
- ↑ Mikaelyan, A.; Thompson, C.; Hofer, M.; Brune, A. (2016). "The deterministic assembly of complex bacterial communities in germ-free cockroach guts". Applied and Environmental Microbiology 82 (4): 1256–63. doi:10.1128/AEM.03700-15. PMID 26655763.
Further reading
- Review articles
- Maranduba, Carlos Magno da Costa; De Castro, Sandra Bertelli Ribeiro; Souza, Gustavo Torres de; Rossato, Cristiano; Da Guia, Francisco Carlos; Valente, Maria Anete Santana; Rettore, João Vitor Paes; Maranduba, Claudinéia Pereira et al. (2015). "Intestinal Microbiota as Modulators of the Immune System and Neuroimmune System: Impact on the Host Health and Homeostasis". Journal of Immunology Research 2015: 931574. doi:10.1155/2015/931574. PMID 25759850.
- De Preter, Vicky; Hamer, Henrike M; Windey, Karen; Verbeke, Kristin (2011). "The impact of pre- and/or probiotics on human colonic metabolism: Does it affect human health?". Molecular Nutrition & Food Research 55 (1): 46–57. doi:10.1002/mnfr.201000451. PMID 21207512.
- Prakash, Satya; Rodes, Laetitia; Coussa-Charley, Michael; Tomaro-Duchesneau, Catherine; Tomaro-Duchesneau, Catherine; Coussa-Charley; Rodes (2011). "Gut microbiota: Next frontier in understanding human health and development of biotherapeutics". Biologics: Targets and Therapy 5: 71–86. doi:10.2147/BTT.S19099. PMID 21847343.
- Wu, G. D.; Chen, J.; Hoffmann, C.; Bittinger, K.; Chen, Y.-Y.; Keilbaugh, S. A.; Bewtra, M.; Knights, D. et al. (2011). "Linking Long-Term Dietary Patterns with Gut Microbial Enterotypes". Science 334 (6052): 105–08. doi:10.1126/science.1208344. PMID 21885731. Bibcode: 2011Sci...334..105W.