Medicine:Schizophrenia
Schizophrenia is a mental disorder[1][2] characterized variously by hallucinations (typically, hearing voices), delusions, disorganized thinking or behavior,[3] and flat or inappropriate affect.[2] Symptoms develop gradually and typically begin during young adulthood and rarely resolve.[4][3][5] There is no objective diagnostic test; diagnosis is based on observed behavior, a psychiatric history that includes the person's reported experiences, and reports of others familiar with the person.[3] For a formal diagnosis, the described symptoms need to have been present for at least six months (according to the DSM-5) or one month (according to the ICD-11).[3][6] Many people with schizophrenia have other mental disorders, especially mood, anxiety, and substance use disorders, as well as obsessive–compulsive disorder (OCD).[3]
About 0.3% to 0.7% of people are diagnosed with schizophrenia during their lifetime.[7] In 2017, there were an estimated 1.1 million new cases and in 2022 a total of 24 million cases globally.[8][9] Males are more often affected and on average have an earlier onset than females.[8] The causes of schizophrenia may include genetic and environmental factors.[2] Genetic factors include a variety of common and rare genetic variants.[10] Possible environmental factors include being raised in a city, childhood adversity, cannabis use during adolescence, infections, the age of a person's mother or father, and poor nutrition during pregnancy.[2][11]
About half of those diagnosed with schizophrenia will experience a marked improvement over the long term with no further relapses, and a small proportion of these will recover completely.[3][12] The other half will have a lifelong impairment.[13] In severe cases, people may be admitted to hospitals.[12] Social problems such as long-term unemployment, poverty, homelessness, exploitation, and victimization are commonly correlated with schizophrenia.[14][15] Compared to the general population, people with schizophrenia have a higher suicide rate (about 5% overall) and more physical health problems,[16][17] leading to an average decrease in life expectancy by 20[18] to 28 years.[19] In 2015, an estimated 17,000 deaths were linked to schizophrenia.[20]
The mainstay of treatment is antipsychotic medication, including olanzapine and risperidone, along with counseling, job training, and social rehabilitation.[2] Up to a third of people do not respond to initial antipsychotics, in which case clozapine is offered.[21] A network meta-analysis of 15 antipsychotic drugs found that all were more effective than placebo for schizophrenia, with clozapine showing the highest efficacy; side effect profiles differ substantially across drugs.[22] In situations where doctors judge that there is a risk of harm to self or others, they may impose short involuntary hospitalization.[23] Long-term hospitalization is used on a small number of people with severe schizophrenia.[24] In some countries where supportive services are limited or unavailable, long-term hospital stays are more common.[25]
Signs and symptoms
Schizophrenia is a mental disorder characterized by significant alterations in perception, thoughts, mood, and behavior.[26] Symptoms are described in terms of positive, negative, and cognitive symptoms.[4][27] The positive symptoms of schizophrenia are the same for any psychosis and are sometimes referred to as psychotic symptoms. These may be present in any of the different psychoses and are often transient, making early diagnosis of schizophrenia problematic. Psychosis noted for the first time in a person who is later diagnosed with schizophrenia is referred to as a first-episode psychosis (FEP).[28][29]
Positive symptoms
Positive symptoms are those symptoms that are not normally experienced, but are present in people during a psychotic episode in schizophrenia, including delusions, hallucinations, and disorganized thoughts, speech and behavior or inappropriate affect, typically regarded as manifestations of psychosis.[28] Hallucinations occur at some point in the lifetimes of 80% of those with schizophrenia[30] and most commonly involve the sense of hearing (most often hearing voices), but can sometimes involve any of the other senses such as taste, sight, smell, and touch.[31] The frequency of hallucinations involving multiple senses is double the rate of those involving only one sense.[30] They are also typically related to the content of the delusional theme.[32] Delusions are bizarre or persecutory in nature. Distortions of self-experience such as feeling that others can hear one's thoughts (thought broadcasting delusion) or that thoughts are being inserted into one's mind, sometimes termed passivity phenomena, are also common.[33][4] The type and content of auditory and visual hallucinations appears to be influenced, at least in part, by cultural and religious factors. Patients in the United Kingdom and United States are more likely to report hearing criticisms and commands; patients in Africa, Asia, and the Middle East report more religious messaging in their hallucinations. This is true even among transplants to these countries, suggesting these differences are cultural, and not genetic.[citation needed] Positive symptoms generally respond well to medication[2] and become reduced over the course of the illness, perhaps linked to the age-related decline in dopamine activity.[3]
Negative symptoms
Negative symptoms are deficits of normal emotional responses, or of other thought processes. The five recognized domains of negative symptoms are: blunted affect – showing flat expressions (monotone) or little emotion; alogia – a poverty of speech; anhedonia – an inability to feel pleasure; asociality – the lack of desire to form relationships, and avolition – a lack of motivation and apathy.[34][35] Avolition and anhedonia are seen as motivational deficits resulting from impaired reward processing.[36][37] Reward is the main driver of motivation and this is mostly mediated by dopamine.[37] It has been suggested that negative symptoms are multidimensional and they have been categorised into two subdomains of apathy or lack of motivation, and diminished expression.[34][38] Apathy includes avolition, anhedonia, and social withdrawal; diminished expression includes blunt affect and alogia.[39] Sometimes diminished expression is treated as both verbal and non-verbal.[40]
Apathy accounts for around 50% of the most often found negative symptoms and affects functional outcome and subsequent quality of life. Apathy is related to disrupted cognitive processing affecting memory and planning, including goal-directed behaviour.[41] The two subdomains have suggested a need for separate treatment approaches.[42] A lack of distress is another noted negative symptom.[43] A distinction is often made between those negative symptoms that are inherent to schizophrenia, termed primary; and those that result from positive symptoms, from the side effects of antipsychotics, substance use disorder, and social deprivation, termed secondary negative symptoms.[44] Negative symptoms are less responsive to medication and the most difficult to treat.[42] However, if properly assessed, secondary negative symptoms are amenable to treatment.[38] There is some evidence that the negative symptoms of schizophrenia are amenable to psychostimulant medication, although such drugs have varying degrees of risk for causing positive psychotic symptoms.[45]
Scales for specifically assessing the presence of negative symptoms, and for measuring their severity, and their changes have been introduced since the earlier scales such as the PANNS that deals with all types of symptoms.[42] These scales are the Clinical Assessment Interview for Negative Symptoms (CAINS), and the Brief Negative Symptom Scale (BNSS) also known as second-generation scales.[42][43][46] In 2020, ten years after its introduction, a cross-cultural study of the use of BNSS found valid and reliable psychometric evidence for its five-domain structure cross-culturally. The BNSS can assess both the presence and severity of negative symptoms of the five recognized domains and an additional item of reduced normal distress. It has been used to measure changes in negative symptoms in trials of psychosocial and pharmacological interventions.[43]
Cognitive symptoms

An estimated 70% of those with schizophrenia have cognitive deficits, and these are most pronounced in early-onset and late-onset illness.[47][48] These are often evident long before the onset of illness in the prodromal stage, and may be present in childhood or early adolescence.[49][50] They are core features but not considered core symptoms, as are positive and negative symptoms.[51][52] However, their presence and degree of dysfunction are taken as better indicators of functionality than the presentation of core symptoms.[49] Cognitive deficits become worse at first episode psychosis but then return to baseline, and remain fairly stable over the course of the illness.[53][54]
Cognitive deficits may be of neurocognition (nonsocial) or of social cognition.[47] Neurocognition is the ability to receive and remember information, and includes verbal fluency, memory, reasoning, problem solving, speed of processing, and auditory and visual perception.[54] Verbal memory and attention are seen to be the most affected.[55][56] Verbal memory impairment is associated with a decreased level of semantic processing (relating meaning to words).[57] Another memory impairment is that of episodic memory.[58] An impairment in visual perception that is consistently found in schizophrenia is that of visual backward masking.[54] Visual processing impairments include an inability to perceive complex visual illusions.[59] Social cognition is concerned with the mental operations needed to interpret, and understand the self and others in the social world.[54][47] This is also an associated impairment, and facial emotion perception is often found to be difficult.[60][61] Cognitive impairments do not usually respond to antipsychotics, and there are a number of interventions that are used to try to improve them; cognitive remediation therapy is of particular help.[52]
Neurological soft signs of clumsiness and loss of fine motor movement are often found in schizophrenia, which may resolve with effective treatment of FEP.[6][62]
Onset
Onset typically occurs between the late teens and early 30s, with the peak incidence occurring in males in the early to mid-twenties, and in females in the late twenties.[4][3][6] Onset before the age of 17 is known as early-onset,[63] and before the age of 13, as can sometimes occur, is known as childhood schizophrenia or very early-onset.[3][64] Onset can occur between the ages of 40 and 60, known as late-onset schizophrenia.[47] Onset over the age of 60, which may be difficult to differentiate as schizophrenia, is known as very-late-onset schizophrenia-like psychosis.[47] Late onset has shown that a higher rate of females are affected; they have less severe symptoms and need lower doses of antipsychotics.[47] The tendency for earlier onset in males is later seen to be balanced by a post-menopausal increase in the development in females. Estrogen produced pre-menopause has a dampening effect on dopamine receptors but its protection can be overridden by a genetic overload.[65] There has been a dramatic increase in the numbers of older adults with schizophrenia.[66]
Onset may happen suddenly or may occur after the slow and gradual development of a number of signs and symptoms, a period known as the prodromal stage.[3] Up to 75% of those with schizophrenia go through a prodromal stage.[67] The negative and cognitive symptoms in the prodrome stage can precede FEP (first episode psychosis) by many months and up to five years.[53][68] The period from FEP and treatment is known as the duration of untreated psychosis (DUP) which is seen to be a factor in functional outcome. The prodromal stage is the high-risk stage for the development of psychosis.[54] Since the progression to first episode psychosis is not inevitable, an alternative term is often preferred of at risk mental state.[54] Cognitive dysfunction at an early age impacts a young person's usual cognitive development.[69] Recognition and early intervention at the prodromal stage would minimize the associated disruption to educational and social development and has been the focus of many studies.[53][68]
Risk factors
Schizophrenia is described as a neurodevelopmental disorder with no precise boundary, or single cause, and is thought to develop from gene–environment interactions with involved vulnerability factors.[2][70][71] The interactions of these risk factors are complex, as numerous and diverse insults from conception to adulthood can be involved.[71] A genetic predisposition on its own, without interacting environmental factors, will not give rise to the development of schizophrenia.[71][72] The genetic component means that prenatal brain development is disturbed, and environmental influence affects the postnatal development of the brain.[73] Evidence suggests that genetically susceptible children are more likely to be vulnerable to the effects of environmental risk factors.[73]
Genetic
Estimates of the heritability of schizophrenia are between 70% and 80%, which implies that 70% to 80% of the individual differences in risk of schizophrenia are associated with genetics.[10][74] These estimates vary because of the difficulty in separating genetic and environmental influences, and their accuracy has been queried.[75][76] The greatest risk factor for developing schizophrenia is having a first-degree relative with the disease (risk is 6.5%); more than 40% of identical twins of those with schizophrenia are also affected.[77] If one parent is affected the risk is about 13% and if both are affected the risk is nearly 50%.[74] However, the DSM-5 indicates that most people with schizophrenia have no family history of psychosis.[3] Results of candidate gene studies of schizophrenia have generally failed to find consistent associations,[78] and the genetic loci identified by genome-wide association studies explain only a small fraction of the variation in the disease.[79]
Many genes are known to be involved in schizophrenia, each with small effects and unknown transmission and expression.[10][80][81] The summation of these effect sizes into a polygenic risk score can explain at least 7% of the variability in liability for schizophrenia.[82] Around 5% of cases of schizophrenia are understood to be at least partially attributable to rare copy number variations (CNVs); these structural variations are associated with known genomic disorders involving deletions at 22q11.2 (DiGeorge syndrome) and 17q12 (17q12 microdeletion syndrome), duplications at 16p11.2 (most frequently found) and deletions at 15q11.2 (Burnside–Butler syndrome).[83] Some of these CNVs increase the risk of developing schizophrenia by as much as 20-fold, and are frequently comorbid with autism and intellectual disabilities.[83]
The genes CRHR1 and CRHBP are associated with the severity of suicidal behavior. These genes code for stress response proteins needed in the control of the HPA axis, and their interaction can affect this axis. Response to stress can cause lasting changes in the function of the HPA axis possibly disrupting the negative feedback mechanism, homeostasis, and the regulation of emotion leading to altered behaviors.[72]
The question of how schizophrenia could be primarily genetically influenced, given that people with schizophrenia have lower fertility rates, is a paradox. It is expected that genetic variants that increase the risk of schizophrenia would be selected against, due to their negative effects on reproductive fitness. A number of potential explanations have been proposed, including that alleles associated with schizophrenia risk confers a fitness advantage in unaffected individuals.[84][85] While some evidence has not supported this idea,[76] others propose that a large number of alleles each contributing a small amount can persist.[86]
A meta-analysis found that oxidative DNA damage was significantly increased in schizophrenia.[87]
Environmental
Environmental factors, each associated with a slight risk of developing schizophrenia in later life include oxygen deprivation, infection, prenatal maternal stress, and malnutrition in the mother during prenatal development.[88] A risk is associated with maternal obesity, in increasing oxidative stress, and dysregulating the dopamine and serotonin pathways.[89] Both maternal stress and infection have been demonstrated to alter fetal neurodevelopment through an increase of pro-inflammatory cytokines.[90] There is a slighter risk associated with being born in the winter or spring possibly due to vitamin D deficiency[91] or a prenatal viral infection.[77] Other infections during pregnancy or around the time of birth that have been linked to an increased risk include infections by Toxoplasma gondii and Chlamydia.[92] The increased risk is about five to eight percent.[93] Viral infections of the brain during childhood are also linked to a risk of schizophrenia during adulthood.[94] Cat exposure is also associated with an increased risk of broadly defined schizophrenia-related disorders, with an odds ratio of 2.4.[95] Exposure to specific medications such as tramadol and desmopressin has been found be associated with an increased risk of incident schizophrenia, while other medications including anti-protozoans were associated with a decrease in schizophrenia risk.[96]
Adverse childhood experiences (ACEs), severe forms of which are classed as childhood trauma, range from being bullied or abused, to the death of a parent.[97] Many adverse childhood experiences can cause toxic stress and increase the risk of psychosis.[97][98][99] Chronic trauma, including ACEs, can promote lasting inflammatory dysregulation throughout the nervous system.[100] It is suggested that early stress may contribute to the development of schizophrenia through these alterations in the immune system.[100] Schizophrenia was the last diagnosis to benefit from the link made between ACEs and adult mental health outcomes.[101]
Living in an urban environment during childhood or as an adult has consistently been found to increase the risk of schizophrenia by a factor of two,[16][102] even after taking into account drug use, ethnic group, and size of social group.[103] A possible link between the urban environment and pollution has been suggested to be the cause of the elevated risk of schizophrenia.[104] Other risk factors include social isolation, immigration related to social adversity and racial discrimination, family dysfunction, unemployment, and poor housing conditions.[77][105][106] Having a father older than 40 years, or parents younger than 20 years are also associated with schizophrenia.[2][107]
Substance use
About half of those with schizophrenia use recreational drugs including alcohol, tobacco, and cannabis excessively.[108][109] Use of stimulants such as amphetamine and cocaine can lead to a temporary stimulant psychosis, which presents very similarly to schizophrenia.[110] Rarely, alcohol use can also result in a similar alcohol-related psychosis.[77][111] Drugs may also be used as coping mechanisms by people who have schizophrenia, to deal with depression, anxiety, boredom, and loneliness.[108][112] The use of cannabis and tobacco are not associated with the development of cognitive deficits, and sometimes a reverse relationship is found where their use improves these symptoms.[52] However, substance use disorders are associated with an increased risk of suicide, and a poor response to treatment.[113][114]
Cannabis use may be a contributory factor in the development of schizophrenia, potentially increasing the risk of the disease in those who are already at risk.[115][116][117] The increased risk may require the presence of certain genes within an individual.[11] Its use is associated with doubling the rate.[118]
Causes
The causes of schizophrenia are still unknown. Several models have been put forward to explain the link between altered brain function and schizophrenia.[16] The prevailing model of schizophrenia is that of a neurodevelopmental disorder, and the underlying changes that occur before symptoms become evident are seen as arising from the interaction between genes and the environment.[119] Extensive studies support this model.[67] Maternal infections, malnutrition and complications during pregnancy and childbirth are known risk factors for the development of schizophrenia, which usually emerges between the ages of 18 and 25, a period that overlaps with certain stages of neurodevelopment.[120] Gene-environment interactions lead to deficits in the neural circuitry that affect sensory and cognitive functions.[67]
The common dopamine and glutamate models proposed are not mutually exclusive; each is seen to have a role in the neurobiology of schizophrenia.[121] The most common model put forward was the dopamine hypothesis of schizophrenia, which attributes psychosis to the mind's faulty interpretation of the misfiring of dopaminergic neurons.[122] This has been directly related to the symptoms of delusions and hallucinations.[123][124][125] Abnormal dopamine signaling has been implicated in schizophrenia based on the usefulness of medications that affect the dopamine receptor and the observation that dopamine levels are increased during acute psychosis.[126][127] A decrease in D1 receptors in the dorsolateral prefrontal cortex may also be responsible for deficits in working memory.[128][129]
The glutamate hypothesis of schizophrenia links alterations between glutamatergic neurotransmission and the neural oscillations that affect connections between the thalamus and the cortex.[130] Studies have shown that a reduced expression of a glutamate receptor – NMDA receptor, and glutamate blocking drugs such as phencyclidine and ketamine can mimic the symptoms and cognitive problems associated with schizophrenia.[130][131][132] Post-mortem studies consistently find that a subset of these neurons fail to express GAD67 (GAD1),[133] in addition to abnormalities in brain morphometry. The subsets of interneurons that are abnormal in schizophrenia are responsible for the synchronizing of neural ensembles needed during working memory tasks. These give the neural oscillations produced as gamma waves that have a frequency of between 30 and 80 hertz. Both working memory tasks and gamma waves are impaired in schizophrenia, which may reflect abnormal interneuron functionality.[133][134][135][136] An important process that may be disrupted in neurodevelopment is astrogenesis – the formation of astrocytes. Astrocytes are crucial in contributing to the formation and maintenance of neural circuits and it is believed that disruption in this role can result in a number of neurodevelopmental disorders including schizophrenia.[137] Evidence suggests that reduced numbers of astrocytes in deeper cortical layers are assocociated with a diminished expression of EAAT2, a glutamate transporter in astrocytes; supporting the glutamate hypothesis.[137]
Deficits in executive functions, such as planning, inhibition, and working memory, are pervasive in schizophrenia. Although these functions are separable, their dysfunction in schizophrenia may reflect an underlying deficit in the ability to represent goal related information in working memory, and to use this to direct cognition and behavior.[138][139] These impairments have been linked to a number of neuroimaging and neuropathological abnormalities. For example, functional neuroimaging studies report evidence of reduced neural processing efficiency, whereby the dorsolateral prefrontal cortex is activated to a greater degree to achieve a certain level of performance relative to controls on working memory tasks. These abnormalities may be linked to the consistent post-mortem finding of reduced neuropil, evidenced by increased pyramidal cell density and reduced dendritic spine density. These cellular and functional abnormalities may also be reflected in structural neuroimaging studies that find reduced grey matter volume in association with deficits in working memory tasks.[140]
Positive symptoms have been linked to cortical thinning in the superior temporal gyrus.[141] The severity of negative symptoms has been linked to reduced thickness in the left medial orbitofrontal cortex.[142] Anhedonia, traditionally defined as a reduced capacity to experience pleasure, is frequently reported in schizophrenia. However, a large body of evidence suggests that hedonic responses are intact in schizophrenia,[143] and that what is reported to be anhedonia is a reflection of dysfunction in other processes related to reward.[144] Overall, a failure of reward prediction is thought to lead to impairment in the generation of cognition and behavior required to obtain rewards, despite normal hedonic responses.[145]
Another theory links abnormal brain lateralization to the development of being left-handed which is significantly more common in those with schizophrenia.[146] This abnormal development of hemispheric asymmetry is noted in schizophrenia.[147] Studies have concluded that the link is a true and verifiable effect that may reflect a genetic link between lateralization and schizophrenia.[146][148]
Bayesian models of brain functioning have been used to link abnormalities in cellular functioning to symptoms.[149][150] Both hallucinations and delusions have been suggested to reflect improper encoding of prior expectations, thereby causing expectation to excessively influence sensory perception and the formation of beliefs. In approved models of circuits that mediate predictive coding, reduced NMDA receptor activation, could in theory result in the positive symptoms of delusions and hallucinations.[151][152][153]
From an evolutionary perspective, schizophrenia is regarded as an "evolutionary puzzle" because it shows high heritability (~60-80 %) and significant impairment in reproduction, yet persists at ~1 % prevalence. One hypothesis suggests that mild schizotypal traits may have historically conferred advantages (such as enhanced creativity or verbal ability,) while more severe forms represent the breakdown of these systems. Experimental models also propose that selection for language and social-cognitive complexity may have increased vulnerability to psychosis when environmental or developmental stressors intervene.[154][155]
Diagnosis
Criteria
Schizophrenia is diagnosed based on criteria in either the Diagnostic and Statistical Manual of Mental Disorders (DSM) published by the American Psychiatric Association or the International Statistical Classification of Diseases and Related Health Problems (ICD) published by the World Health Organization (WHO). These criteria use the self-reported experiences of the person and reported abnormalities in behavior, followed by a psychiatric assessment. The mental status examination is an important part of the assessment.[156] An established tool for assessing the severity of positive and negative symptoms is the Positive and Negative Syndrome Scale (PANSS).[157] This has been seen to have shortcomings relating to negative symptoms, and other scales – the Clinical Assessment Interview for Negative Symptoms (CAINS), and the Brief Negative Symptoms Scale (BNSS) have been introduced.[42] The DSM-5, published in 2013, gives a Scale to Assess the Severity of Symptom Dimensions outlining eight dimensions of symptoms.[51]
DSM-5 states that to be diagnosed with schizophrenia, two diagnostic criteria have to be met over the period of one month, with a significant impact on social or occupational functioning for at least six months. One of the symptoms needs to be either delusions, hallucinations, or disorganized speech. A second symptom could be one of the negative symptoms, or severely disorganized or catatonic behaviour.[3] A different diagnosis of schizophreniform disorder can be made before the six months needed for the diagnosis of schizophrenia.[3]
In Australia, the guideline for diagnosis is for six months or more with symptoms severe enough to affect ordinary functioning.[158] In the UK diagnosis is based on having the symptoms for most of the time for one month, with symptoms that significantly affect the ability to work, study, or carry on ordinary daily living, and with other similar conditions ruled out.[159]
The ICD criteria are typically used in European countries; the DSM criteria are used predominantly in the United States and Canada, and are prevailing in research studies. In practice, agreement between the two systems is high.[160] The current proposal for the ICD-11 criteria for schizophrenia recommends adding self-disorder as a symptom.[33]
A major unresolved difference between the two diagnostic systems is that of the requirement in DSM of an impaired functional outcome. WHO for ICD argues that not all people with schizophrenia have functional deficits and so these are not specific for the diagnosis.[51]
Neuroimaging techniques
Functional magnetic resonance imaging (fMRI) has become a tool in understanding brain activity and connectivity differences in individuals with schizophrenia. Through resting-state fMRI, researchers have observed altered connectivity patterns within several key brain networks, such as the default mode network (DMN),[161] salience network (SN),[162] and central executive network (CEN).[163] Alterations may underlie cognitive and emotional symptoms in schizophrenia, such as disorganized thinking, impaired attention, and emotional dysregulation.
Comorbidities
Many people with schizophrenia may have one or more other mental disorders, such as anxiety disorders, obsessive–compulsive disorder, or substance use disorder. These are separate disorders that require treatment.[3] When comorbid with schizophrenia, substance use disorder and antisocial personality disorder both increase the risk for violence.[164] Comorbid substance use disorder also increases the risk of suicide.[113]
Sleep disorders often co-occur with schizophrenia, and may be an early sign of relapse.[165] Sleep disorders are linked with positive symptoms such as disorganized thinking and can adversely affect cortical plasticity and cognition.[165] The consolidation of memories is disrupted in sleep disorders.[166] They are associated with severity of illness, a poor prognosis, and poor quality of life.[167][168] Sleep onset and maintenance insomnia is a common symptom, regardless of whether treatment has been received or not.[167] Genetic variations have been found associated with these conditions involving the circadian rhythm, dopamine and histamine metabolism, and signal transduction.[169]
Schizophrenia is also associated with a number of somatic comorbidities including diabetes mellitus type 2, autoimmune diseases, and cardiovascular diseases. The association of these with schizophrenia may be partially due to medications (e.g. dyslipidemia from antipsychotics), environmental factors (e.g. complications from an increased rate of cigarette smoking), or associated with the disorder itself (e.g. diabetes mellitus type 2 and some cardiovascular diseases are thought to be genetically linked). These somatic comorbidities contribute to reduced life expectancy among persons with the disorder.[170]
Differential diagnosis
To make a diagnosis of schizophrenia other possible causes of psychosis need to be excluded.[171]: 858 Psychotic symptoms lasting less than a month may be diagnosed as brief psychotic disorder, or as schizophreniform disorder. Psychosis is noted in Other specified schizophrenia spectrum and other psychotic disorders as a DSM-5 category. Schizoaffective disorder is diagnosed if symptoms of mood disorder are substantially present alongside psychotic symptoms. Psychosis that results from a general medical condition or substance is termed secondary psychosis.[3]
Psychotic symptoms may be present in several other conditions, including bipolar disorder,[172] borderline personality disorder,[173] substance intoxication, substance-induced psychosis, and a number of drug withdrawal syndromes. Non-bizarre delusions are also present in delusional disorder, and social withdrawal in social anxiety disorder, avoidant personality disorder and schizotypal personality disorder. Schizotypal personality disorder has symptoms that are similar but less severe than those of schizophrenia.[3] Schizophrenia occurs along with obsessive–compulsive disorder (OCD) considerably more often than could be explained by chance, although it can be difficult to distinguish obsessions that occur in OCD from the delusions of schizophrenia.[174] There can be considerable overlap with the symptoms of post-traumatic stress disorder.[175]
A more general medical and neurological examination may be needed to rule out medical illnesses which may rarely produce psychotic schizophrenia-like symptoms, such as metabolic disturbance, systemic infection, syphilis, HIV-associated neurocognitive disorder, epilepsy, limbic encephalitis, and brain lesions. Stroke, multiple sclerosis, hyperthyroidism, hypothyroidism, and dementias such as Alzheimer's disease, Huntington's disease, frontotemporal dementia, and the Lewy body dementias may also be associated with schizophrenia-like psychotic symptoms.[176] It may be necessary to rule out a delirium, which can be distinguished by visual hallucinations, acute onset and fluctuating level of consciousness, and indicates an underlying medical illness. Investigations are not generally repeated for relapse unless there is a specific medical indication or possible adverse effects from antipsychotic medication.[177] In children hallucinations must be separated from typical childhood fantasies.[3] It is difficult to distinguish childhood schizophrenia from autism.[64]
Prevention
Prevention of schizophrenia is difficult as there are no reliable markers for the later development of the disorder.[178]
Early intervention programs diagnose and treat patients in the prodromal phase of the illness. There is some evidence that these programs reduce symptoms. Patients tend to prefer early treatment programs to ordinary treatment and are less likely to disengage from them. As of 2020, it is unclear whether the benefits of early treatment persist once the treatment is terminated.[179]
Cognitive behavioral therapy may reduce the risk of psychosis in those at high risk after a year[180] and is recommended in this group, by the National Institute for Health and Care Excellence (NICE).[26] Another preventive measure is to avoid drugs that have been associated with development of the disorder, including cannabis, cocaine, and amphetamines.[77]
Antipsychotics are prescribed following a first-episode psychosis, and following remission, a preventive maintenance use is continued to avoid relapse. However, it is recognized that some people do recover following a single episode and that long-term use of antipsychotics will not be needed but there is no way of identifying this group.[181]
Management
The primary treatment of schizophrenia is the use of antipsychotic medications, often in combination with psychosocial interventions and social supports.[16][182] Community support services including drop-in centers, visits by members of a community mental health team, supported employment,[183] and support groups are common. The time between the onset of psychotic symptoms to being given treatment – the duration of untreated psychosis (DUP) – is associated with a poorer outcome in both the short term and the long term.[184]
Voluntary or involuntary admission to hospital may be imposed by doctors and courts who deem a person to be having a severe episode. In the UK, large mental hospitals termed asylums began to be closed down in the 1950s with the advent of antipsychotics, and with an awareness of the negative impact of long-term hospital stays on recovery.[14] This process was known as deinstitutionalization, and community and supportive services were developed to support this change. Many other countries followed suit with the US starting in the 60s.[185] There still remain a smaller group of people who do not improve enough to be discharged.[14][24] In some countries that lack the necessary supportive and social services, long-term hospital stays are more usual.[25]
Medication
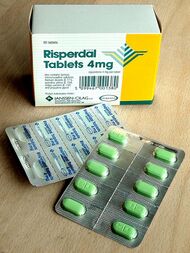
A Bayesian network meta-analysis of 212 randomized controlled trials including 43,049 participants found that all 15 antipsychotic drugs reviewed were more effective than placebo in the acute treatment of schizophrenia, with clozapine showing the greatest efficacy and amisulpride the lowest all-cause discontinuation.[22] While differences in efficacy were modest, side-effect profiles varied widely, indicating that antipsychotic selection should be guided by individual patient needs rather than the traditional classification into first- and second-generation drugs.[22]
The first-line treatment for schizophrenia is an antipsychotic. The first-generation antipsychotics, now called typical antipsychotics, like haloperidol, are dopamine antagonists that block D2 receptors, and affect the neurotransmission of dopamine. Those brought out later, the second-generation antipsychotics known as atypical antipsychotics, including olanzapine and risperidone, can also have an effect on another neurotransmitter, serotonin. Antipsychotics can reduce the symptoms of anxiety within hours of their use, but, for other symptoms, they may take several days or weeks to reach their full effect.[28][186] They have little effect on negative and cognitive symptoms, which may be helped by additional psychotherapies and medications.[187] There is no single antipsychotic suitable for first-line treatment for everyone, as responses and tolerances vary between people.[188] Stopping medication may be considered after a single psychotic episode where there has been a full recovery with no symptoms for twelve months. Repeated relapses worsen the long-term outlook and the risk of relapse following a second episode is high, and long-term treatment is usually recommended.[189][190]
About half of those with schizophrenia will respond favourably to antipsychotics, and have a good return of functioning.[191] However, positive symptoms persist in up to a third of people. Following two trials of different antipsychotics over six weeks, that also prove ineffective, they will be classed as having treatment-resistant schizophrenia (TRS), and clozapine will be offered.[192][21] Clozapine is of benefit to around half of this group although it has the potentially serious side effect of agranulocytosis (lowered white blood cell count) in less than 4% of people.[16][77][193]
About 30 to 50 percent of people with schizophrenia do not accept that they have an illness or comply with their recommended treatment.[194] For those who are unwilling or unable to take medication regularly, long-acting injections of antipsychotics may be used,[195] which reduce the risk of relapse to a greater degree than oral medications.[196] When used in combination with psychosocial interventions, they may improve long-term adherence to treatment.[197]
A 2025 meta-analysis showed xanomeline and trospium's effect in the improvement of symptoms of schizophrenia.[198] The fixed-dose combination medication xanomeline/trospium chloride (Cobenfy) was approved for medical use in the United States in September 2024.[199][200] It is the first cholinergic agonist approved by the US Food and Drug Administration (FDA) to treat schizophrenia.[199]
Negative and cognitive symptoms are an unmet clinical need in antipsychotic-based treatment approaches. Psychostimulant drugs have been found effective in the treatment of negative symptoms, but are rarely prescribed due to concerns about the excacerbation of positive symptoms.[45] It is possible that low-dose psychedelic therapies could be of benefit in schizophrenia through their prosocial and procognitive effects, although there is a serious risk that high dose psychedelic therapies could lead to worsening of positive symptoms.[201]
Adverse effects
Extrapyramidal symptoms, including akathisia, are associated with all commercially available antipsychotic to varying degrees.[202]: 566 There is little evidence that second generation antipsychotics have reduced levels of extrapyramidical symptoms compared to typical antipsychotics.[202]: 566 Tardive dyskinesia can occur due to long-term use of antipsychotics, developing after months or years of use.[203] The antipsychotic clozapine is also associated with thromboembolism (including pulmonary embolism), myocarditis, and cardiomyopathy.
Psychosocial interventions
A number of psychosocial interventions that include several types of psychotherapy may be useful in the treatment of schizophrenia such as: family therapy,[204] group therapy, cognitive remediation therapy (CRT),[205] cognitive behavioral therapy (CBT),[206] and metacognitive training.[207][208] Skills training, help with substance use, and weight management – often needed as a side effect of an antipsychotic – are also offered.[209] In the US, interventions for first episode psychosis have been brought together in an overall approach known as coordinated speciality care (CSC) and also includes support for education.[28] In the UK care across all phases is a similar approach that covers many of the treatment guidelines recommended.[26] The aim is to reduce the number of relapses and stays in the hospital.[204]
Other support services for education, employment, and housing are usually offered. For people with severe schizophrenia, who are discharged from a stay in the hospital, these services are often brought together in an integrated approach to offer support in the community away from the hospital setting. In addition to medicine management, housing, and finances, assistance is given for more routine matters such as help with shopping and using public transport. This approach is known as assertive community treatment (ACT) and has been shown to achieve positive results in symptoms, social functioning and quality of life.[210][211] Another more intense approach is known as intensive care management (ICM). ICM is a stage further than ACT and emphasises support of high intensity in smaller caseloads, (less than twenty). This approach is to provide long-term care in the community. Studies show that ICM improves many of the relevant outcomes including social functioning.[212]
Some studies have shown little evidence for the effectiveness of CBT in either reducing symptoms or preventing relapse.[213][214] However, other studies have found that CBT does improve overall psychotic symptoms (when in use with medication) and it has been recommended in Canada, but has been seen to have no effect on social function, relapse, or quality of life.[215] In the UK it is recommended as an add-on therapy in the treatment of schizophrenia.[186][214] Arts therapies are seen to improve negative symptoms in some people, and are recommended by NICE in the UK.[186] This approach is criticised as having not been well-researched,[216][217] and arts therapies are not recommended in Australian guidelines for example.[218] Peer support, in which people with personal experience of schizophrenia, provide help to each other, is of unclear benefit.[219]
Other
Exercise including aerobic exercise has been shown to improve positive and negative symptoms, cognition, working memory, and improve quality of life.[220][221] Exercise has also been shown to increase the volume of the hippocampus in those with schizophrenia. A decrease in hippocampal volume is one of the factors linked to the development of the disease.[220] However, there still remains the problem of increasing motivation for, and maintaining participation in physical activity.[222] Supervised sessions are recommended.[221] In the UK healthy eating advice is offered alongside exercise programs.[223]
An inadequate diet is often found in schizophrenia, and associated vitamin deficiencies including those of folate, and vitamin D are linked to the risk factors for the development of schizophrenia and for early death including heart disease.[224][225] Those with schizophrenia possibly have the worst diet of all the mental disorders. Lower levels of folate and vitamin D have been noted as significantly lower in first episode psychosis.[224] The use of supplemental folate is recommended.[226] A zinc deficiency has also been noted.[227] Vitamin B12 is also often deficient and this is linked to worse symptoms. Supplementation with B vitamins has been shown to significantly improve symptoms, and to put in reverse some of the cognitive deficits.[224] It is also suggested that the noted dysfunction in gut microbiota might benefit from the use of probiotics.[227]
Prognosis

| no data ≤ 185 185–197 197–207 207–218 218–229 229–240 | 240–251 251–262 262–273 273–284 284–295 ≥ 295 |
Schizophrenia has great human and economic costs.[2] It decreases life expectancy by between 10[18] and 28 years.[19] This is primarily because of its association with heart disease,[228] diabetes,[19] obesity, poor diet, a sedentary lifestyle, and smoking, with an increased rate of suicide playing a lesser role.[18][229] Side effects of antipsychotics may also increase the risk.[18]
Almost 40% of those with schizophrenia die from complications of cardiovascular disease which is seen to be increasingly associated.[225] An underlying factor of sudden cardiac death may be Brugada syndrome (BrS) – BrS mutations that overlap with those linked with schizophrenia are the calcium channel mutations.[225] BrS may also be drug-induced from certain antipsychotics and antidepressants.[225] Primary polydipsia, or excessive fluid intake, is relatively common in people with chronic schizophrenia.[230][231] This may lead to hyponatremia which can be life-threatening. Antipsychotics can lead to a dry mouth, but there are several other factors that may contribute to the disorder; it may reduce life expectancy by 13 percent.[231] Barriers to improving the mortality rate in schizophrenia are poverty, overlooking the symptoms of other illnesses, stress, stigma, and medication side effects.[232][233][234]
Schizophrenia is a major cause of disability. In 2016, it was classed as the 12th most disabling condition.[235] Approximately 75% of people with schizophrenia have ongoing disability with relapses.[236] Some people do recover completely and others function well in society.[237] Most people with schizophrenia live independently with community support.[16] About 85% are unemployed.[2] In people with a first episode of psychosis in schizophrenia a good long-term outcome occurs in 31%, an intermediate outcome in 42% and a poor outcome in 31%.[238] Males are affected more often than females, and have a worse outcome.[239] Studies showing that outcomes for schizophrenia appear better in the developing than the developed world[240] have been questioned.[241] Social problems, such as long-term unemployment, poverty, homelessness, exploitation, stigmatization and victimization are common consequences, and lead to social exclusion.[14][15][233][234]
There is a higher than average suicide rate associated with schizophrenia estimated at 5% to 6%, most often occurring in the period following onset or first hospital admission.[6][17] Several times more (20 to 40%) attempt suicide at least once.[3][91] There are a variety of risk factors, including male sex, depression, a high IQ,[242] heavy smoking,[243] and substance use.[113] Repeated relapse is linked to an increased risk of suicidal behavior.[181] The use of clozapine can reduce the risk of suicide, and of aggression.[244]
A strong association between schizophrenia and tobacco smoking has been shown in worldwide studies.[245][246] Smoking is especially high in those diagnosed with schizophrenia, with estimates ranging from 80 to 90% being regular smokers, as compared to 20% of the general population.[246] Those who smoke tend to smoke heavily, and additionally smoke cigarettes with high nicotine content.[32] Some propose that this is in an effort to improve symptoms.[247] Among people with schizophrenia use of cannabis is also common.[113]
Schizophrenia leads to an increased risk of dementia.[248]
Violence
Most people with schizophrenia are not aggressive, and are more likely to be victims of violence rather than perpetrators.[3] People with schizophrenia are commonly exploited and victimized by violent crime as part of a broader dynamic of social exclusion.[14][15] People diagnosed with schizophrenia are also subject to forced drug injections, seclusion, and restraint at high rates.[23][24]
The risk of violence by people with schizophrenia is small. There are minor subgroups where the risk is high.[164] This risk is usually associated with a comorbid disorder such as a substance use disorder – in particular alcohol, or with antisocial personality disorder.[164] Substance use disorder is strongly linked, and other risk factors are linked to deficits in cognition and social cognition including facial perception and insight that are in part included in theory of mind impairments.[249][250] Poor cognitive functioning, decision-making, and facial perception may contribute to making a wrong judgement of a situation that could result in an inappropriate response such as violence.[251] These associated risk factors are also present in antisocial personality disorder which when present as a comorbid disorder greatly increases the risk of violence.[252][253]
Epidemiology

In 2017,[needs update] the Global Burden of Disease Study estimated there were 1.1 million new cases;[9] in 2022 the World Health Organization (WHO) reported a total of 24 million cases globally.[8] Schizophrenia affects around 0.3–0.7% of people at some point in their life.[7][19] In areas of conflict this figure can rise to between 4.0 and 6.5%.[254] It occurs 1.4 times more frequently in males than females and typically appears earlier in men.[77]
Worldwide, schizophrenia is the most common psychotic disorder.[48] The frequency of schizophrenia varies across the world,[3] within countries,[255] and at the local and neighborhood level;[256] this variation in prevalence between studies over time, across geographical locations, and by gender is as high as fivefold.[2]
Schizophrenia causes approximately one percent of worldwide disability adjusted life years[needs update][77] and resulted in 17,000 deaths in 2015.[20]
In 2000,[needs update] WHO found the percentage of people affected and the number of new cases that develop each year is roughly similar around the world, with age-standardized prevalence per 100,000 ranging from 343 in Africa to 544 in Japan and Oceania for men, and from 378 in Africa to 527 in Southeastern Europe for women.[257]
History
Conceptual development

Accounts of a schizophrenia-like syndrome are rare in records before the 19th century; the earliest case reports were in 1797 and 1809.[258] The term dementia praecox ("premature dementia") was used by German psychiatrist Heinrich Schüle in 1886 and then in 1891 by Arnold Pick in a case report of hebephrenia. In 1893 Emil Kraepelin used the term in making a distinction, known as the Kraepelinian dichotomy, between the two psychoses: dementia praecox and manic depression (now called bipolar disorder).[18] When it became evident that the disorder was not a degenerative dementia, it was renamed schizophrenia by Eugen Bleuler in 1908.[259]
The word schizophrenia ("splitting of the mind") is Modern Latin, derived from the Greek schizein (Ancient Greek: σχίζειν, lit. 'to split') and phrēn (Ancient Greek: φρήν, lit. 'mind').[260] Its use was intended to describe the separation of function between personality, thinking, memory, and perception.[259]
In the early 20th century, the psychiatrist Kurt Schneider categorized the psychotic symptoms of schizophrenia into two groups: hallucinations and delusions. The hallucinations were listed as specific to auditory and the delusions included thought disorders. These were seen as important symptoms, termed first-rank. The most common first-rank symptom was found to belong to thought disorders. Cite error: Invalid <ref> tag; refs with no name must have content [261] while they may not be useful in diagnosing schizophrenia, they can assist in differential diagnosis.[262]
Subtypes of schizophrenia—classified as paranoid, disorganized, catatonic, undifferentiated, and residual—were difficult to distinguish and are no longer recognized as separate conditions by DSM-5 (2013) or ICD-11.[263][264][265]
Breadth of diagnosis
Before the 1960s, nonviolent petty criminals and women were sometimes diagnosed with schizophrenia, categorizing the latter as ill for not performing their duties as wives and mothers.[266] In the mid- to late 1960s, black men were categorized as "hostile and aggressive" and diagnosed as schizophrenic at much higher rates, their civil rights and Black Power activism labeled as delusions.[266][267]
In the early 1970s in the United States, the diagnostic model for schizophrenia was broad and clinically based using DSM II. Schizophrenia was diagnosed far more in the United States than in Europe, where the ICD-9 criteria were followed. The US model was criticised for failing to demarcate clearly those people with a mental illness. In 1980 DSM III was published and showed a shift in focus from the clinically based biopsychosocial model to a reason-based medical model.[clarification needed][268] DSM IV brought an increased focus on an evidence-based medical model.[269]
Historical treatment
In the 1930s a number of shock procedures which induced seizures (convulsions) or comas were used to treat schizophrenia.[270] Insulin shock involved injecting large doses of insulin to induce comas, which in turn produced hypoglycemia and convulsions.[270][271] The use of electricity to induce seizures was in use as electroconvulsive therapy (ECT) by 1938.[272]
Carried out from the 1930s until the 1970s in the United States and until the 1980s in France, psychosurgery, including such modalities as the lobotomy, is recognized as a human rights abuse.[273][274] In the mid-1950s, chlorpromazine, the first typical antipsychotic, was introduced,[275] followed in the 1970s by clozapine, the first atypical antipsychotic.[276]
Political abuse
From the 1960s until 1989, psychiatrists in the USSR and Eastern Bloc diagnosed thousands of people with sluggish schizophrenia,[277][278] without signs of psychosis, based on "the assumption that symptoms would later appear".[279] Now discredited, the diagnosis provided a convenient way to confine political dissidents.[280]
Society and culture
In the United States, the annual cost of schizophrenia – including direct costs (outpatient, inpatient, drugs, and long-term care) and non-healthcare costs (law enforcement, reduced workplace productivity, and unemployment) – was estimated at $62.7 billion for the year 2002.[281][lower-alpha 1] In the UK the cost in 2016 was put at £11.8 billion per year with a third of that figure directly attributable to the cost of hospital, social care and treatment.[2]
Stigma

In 2002, the term for schizophrenia in Japan was changed from seishin-bunretsu-byō (精神分裂病; lit. 'mind-split disease') to tōgō-shitchō-shō (統合失調症; lit. 'integration–dysregulation syndrome') to reduce stigma and confusion with "multiple personalities".[284] The new name, also interpreted as "integration disorder", was inspired by the biopsychosocial model.[285] A similar change was made in South Korea in 2012 to attunement disorder.[286]
Stigma may prevent further research and treatment as in history treated some in the past invariably worse to recovery.[233][234]
Cultural depictions
Media coverage, especially movies, reinforce the public perception of an association between schizophrenia and violence.[287][234][233] A majority of movies have historically depicted characters with schizophrenia as criminal, dangerous, violent, unpredictable and homicidal, and depicted delusions and hallucinations as the main symptoms of schizophrenic characters, ignoring other common symptoms,[288] furthering stereotypes of schizophrenia including the idea of a split personality.[289]
The book A Beautiful Mind chronicled the life of John Forbes Nash who had been diagnosed with schizophrenia and won the Nobel Memorial Prize in Economic Sciences. The book was made into a film with the same name; an earlier documentary film was A Brilliant Madness.
In the UK, guidelines for reporting conditions and award campaigns have shown a reduction in negative reporting since 2013.[290]
In 1964 a case study of three males diagnosed with schizophrenia who each had the delusional belief that they were Jesus Christ was published as The Three Christs of Ypsilanti; a film with the title Three Christs was released in 2020.[291][292]
Research
A 2015 Cochrane review found unclear evidence of benefit from brain stimulation techniques to treat the positive symptoms of schizophrenia, in particular auditory verbal hallucinations (AVHs).[293] Most studies focus on transcranial direct-current stimulation (tDCM), and repetitive transcranial magnetic stimulation (rTMS).[294] Techniques based on focused ultrasound for deep brain stimulation could provide insight for the treatment of AVHs.[294]
The study of potential biomarkers that would help in diagnosis and treatment of schizophrenia is an active area of research as of 2020. Possible biomarkers include markers of inflammation,[90] neuroimaging,[295] brain-derived neurotrophic factor (BDNF),[296] and speech analysis. Some markers such as C-reactive protein are useful in detecting levels of inflammation implicated in some psychiatric disorders but they are not disorder-specific. Other inflammatory cytokines are found to be elevated in first episode psychosis and acute relapse that are normalized after treatment with antipsychotics, and these may be considered as state markers.[297] Deficits in sleep spindles in schizophrenia may serve as a marker of an impaired thalamocortical circuit, and a mechanism for memory impairment.[166] MicroRNAs are highly influential in early neuronal development, and their disruption is implicated in several CNS disorders; circulating microRNAs (cimiRNAs) are found in body fluids such as blood and cerebrospinal fluid, and changes in their levels are seen to relate to changes in microRNA levels in specific regions of brain tissue. These studies suggest that cimiRNAs have the potential to be early and accurate biomarkers in a number of disorders including schizophrenia.[298][299]
Ongoing fMRI research aims to identify biomarkers within these brain networks,[300] potentially aiding in earlier diagnosis and better tracking of treatment responses in schizophrenia.
Explanatory notes
References
- ↑ "ICD-11: 6A20 Schizophrenia". World Health Organization. https://icd.who.int/browse11/l-m/en#/http%3a%2f%2fid.who.int%2ficd%2fentity%2f1683919430.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 "Schizophrenia". The Lancet 388 (10039): 86–97. July 2016. doi:10.1016/S0140-6736(15)01121-6. PMID 26777917. Bibcode: 2016Lanc..388...86O.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 Diagnostic and Statistical Manual of Mental Disorders: DSM-5 (5th ed.). Arlington, VA: American Psychiatric Association. 2013. pp. 99–105. ISBN 978-0-89042-555-8.
- ↑ 4.0 4.1 4.2 4.3 Cite error: Invalid
<ref>tag; no text was provided for refs namedNIH2022 - ↑ Tramazzo, Sara; Lian, Wenxuan; Ajnakina, Olesya; Carlson, Gabrielle; Bromet, Evelyn; Kotov, Roman; Jonas, Katherine (2024-06-01). "Long-Term Course of Remission and Recovery in Psychotic Disorders". American Journal of Psychiatry 181 (6): 532–540. doi:10.1176/appi.ajp.20230189. ISSN 0002-953X. PMID 38745457. https://osf.io/yh74r/. Retrieved 2025-05-23.
- ↑ 6.0 6.1 6.2 6.3 Ferri's clinical advisor 2019: 5 books in 1. Elsevier. 2019. pp. 1225–1226. ISBN 978-0-323-53042-2.
- ↑ 7.0 7.1 "Balancing therapeutic safety and efficacy to improve clinical and economic outcomes in schizophrenia: a clinical overview". The American Journal of Managed Care 20 (8 Suppl): S160-165. June 2014. PMID 25180705.
- ↑ 8.0 8.1 8.2 "Schizophrenia Fact sheet". World Health Organization. 10 January 2022. https://www.who.int/news-room/fact-sheets/detail/schizophrenia.
- ↑ 9.0 9.1 "Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017". The Lancet 392 (10159): 1789–1858. November 2018. doi:10.1016/S0140-6736(18)32279-7. PMID 30496104. Bibcode: 2018Lanc..392.1789J.
- ↑ 10.0 10.1 10.2 Genetics of Schizophrenia: Historical Insights and Prevailing Evidence. Advances in Genetics. 96. 2016. pp. 99–141. doi:10.1016/bs.adgen.2016.08.001. ISBN 978-0-12-809672-7.
- ↑ 11.0 11.1 "Cannabis and psychosis: have we found the missing links?". Asian Journal of Psychiatry 6 (4): 281–287. August 2013. doi:10.1016/j.ajp.2013.03.012. PMID 23810133. "Cannabis acts as a component cause of psychosis, that is, it increases the risk of psychosis in people with certain genetic or environmental vulnerabilities, though by itself, it is neither a sufficient nor a necessary cause of psychosis.".
- ↑ 12.0 12.1 "Recovery from schizophrenia: is it possible?". Current Opinion in Psychiatry 31 (3): 246–255. May 2018. doi:10.1097/YCO.0000000000000407. PMID 29474266.
- ↑ "Chapter 48: Schizophrenia and Other Psychoses". Psychiatry (fourth ed.). John Wiley & Sons, Ltd.. 2015. pp. 798, 816, 819. doi:10.1002/9781118753378.ch48. ISBN 978-1-118-84547-9.
- ↑ 14.0 14.1 14.2 14.3 14.4 "Contemporary mental health rehabilitation". East Asian Archives of Psychiatry 24 (3): 89–94. September 2014. PMID 25316799.
- ↑ 15.0 15.1 15.2 "Global Epidemiology and Burden of Schizophrenia: Findings From the Global Burden of Disease Study 2016". Schizophrenia Bulletin 44 (6): 1195–1203. October 2018. doi:10.1093/schbul/sby058. PMID 29762765.
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 "Schizophrenia". Lancet 374 (9690): 635–645. August 2009. doi:10.1016/S0140-6736(09)60995-8. PMID 19700006. Bibcode: 2009Lanc..374..635V. http://xa.yimg.com/kq/groups/19525360/611943554/name/Schizophrenia+-+The+Lancet.pdf. Retrieved 23 December 2011.
- ↑ 17.0 17.1 "Suicide and schizophrenia: a systematic review of rates and risk factors". Journal of Psychopharmacology 24 (4 Suppl): 81–90. November 2010. doi:10.1177/1359786810385490. PMID 20923923.
- ↑ 18.0 18.1 18.2 18.3 18.4 "Excess early mortality in schizophrenia". Annual Review of Clinical Psychology 10: 425–448. 2014. doi:10.1146/annurev-clinpsy-032813-153657. PMID 24313570.
- ↑ 19.0 19.1 19.2 19.3 "Schizophrenia". Statistics. US National Institute of Mental Health (NIMH). 22 April 2022. https://www.nimh.nih.gov/health/statistics/schizophrenia.
- ↑ 20.0 20.1 "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet 388 (10053): 1459–1544. October 2016. doi:10.1016/S0140-6736(16)31012-1. PMID 27733281.
- ↑ 21.0 21.1 "Clozapine Response Rates among People with Treatment-Resistant Schizophrenia: Data from a Systematic Review and Meta-Analysis". Canadian Journal of Psychiatry 62 (11): 772–777. November 2017. doi:10.1177/0706743717718167. PMID 28655284.
- ↑ 22.0 22.1 22.2 "Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis". Lancet 382 (9896): 951–962. September 2013. doi:10.1016/S0140-6736(13)60733-3. PMID 23810019.
- ↑ 23.0 23.1 "Psychiatric services for people with severe mental illness across western Europe: what can be generalized from current knowledge about differences in provision, costs and outcomes of mental health care?". Acta Psychiatrica Scandinavica. Supplementum 113 (429): 9–16. 2006. doi:10.1111/j.1600-0447.2005.00711.x. PMID 16445476.
- ↑ 24.0 24.1 24.2 "Durées d'hospitalisation des patients souffrant de schizophrénie: implication des systèmes de soin et conséquences médicoéconomiques" (in fr). L'Encéphale 35 (4): 394–399. September 2009. doi:10.1016/j.encep.2008.11.005. PMID 19748377.
- ↑ 25.0 25.1 "Disability in a Group of Long-stay Patients with Schizophrenia: Experience from a Mental Hospital.". Indian Journal of Psychological Medicine 34 (1): 70–75. January 2012. doi:10.4103/0253-7176.96164. PMID 22661812.
- ↑ 26.0 26.1 26.2 "Psychosis and schizophrenia in adults: treatment and management". National Institute for Health and Care Excellence (NICE). March 2014. pp. 4–34. http://www.nice.org.uk/nicemedia/live/14382/66534/66534.pdf.
- ↑ "Current Concepts and Treatments of Schizophrenia". Molecules 23 (8): 2087. 20 August 2018. doi:10.3390/molecules23082087. PMID 30127324.
- ↑ 28.0 28.1 28.2 28.3 "RAISE Questions and Answers". US National Institute of Mental Health. https://www.nimh.nih.gov/health/topics/schizophrenia/raise/raise-questions-and-answers.shtml#4.
- ↑ "Association between duration of untreated psychosis and outcome in cohorts of first-episode patients: a systematic review". Archives of General Psychiatry 62 (9): 975–983. September 2005. doi:10.1001/archpsyc.62.9.975. PMID 16143729.
- ↑ 30.0 30.1 "A Review of Multimodal Hallucinations: Categorization, Assessment, Theoretical Perspectives, and Clinical Recommendations". Schizophr Bull 47 (1): 237–248. January 2021. doi:10.1093/schbul/sbaa101. PMID 32772114.
- ↑ "A possible key role of vision in the development of schizophrenia". Reviews in the Neurosciences 30 (4): 359–379. 27 May 2019. doi:10.1515/revneuro-2018-0022. PMID 30244235.
- ↑ 32.0 32.1 American Psychiatric Association. Task Force on DSM-IV. (2000). Diagnostic and statistical manual of mental disorders: DSM-IV-TR.. American Psychiatric Pub.. pp. 299–304. ISBN 978-0-89042-025-6.
- ↑ 33.0 33.1 "Shall we really say goodbye to first rank symptoms?". European Psychiatry 37: 8–13. September 2016. doi:10.1016/j.eurpsy.2016.04.010. PMID 27429167.
- ↑ 34.0 34.1 "[Negative Symptoms: Clinical and Psychometric Aspects]". L'Encephale 41 (6 Suppl 1): 6S15–17. December 2015. doi:10.1016/S0013-7006(16)30004-5. PMID 26776385.
- ↑ "[Scale for Assessing Negative Symptoms in Schizophrenia: A Systematic Review]". L'Encephale 42 (2): 165–171. April 2016. doi:10.1016/j.encep.2015.12.020. PMID 26923997.
- ↑ "Motivational Deficits in Schizophrenia and the Representation of Expected Value". Behavioral Neuroscience of Motivation. Current Topics in Behavioral Neurosciences. 27. 2016. pp. 375–410. doi:10.1007/7854_2015_385. ISBN 978-3-319-26933-7.
- ↑ 37.0 37.1 "Neuroscience of apathy and anhedonia: a transdiagnostic approach.". Nature Reviews. Neuroscience 19 (8): 470–484. August 2018. doi:10.1038/s41583-018-0029-9. PMID 29946157. https://ora.ox.ac.uk/objects/uuid:3e481f87-0ede-47dd-bdd8-2db78dfd3694.
- ↑ 38.0 38.1 "Negative symptoms of schizophrenia: new developments and unanswered research questions". The Lancet. Psychiatry 5 (8): 664–677. August 2018. doi:10.1016/S2215-0366(18)30050-6. PMID 29602739.
- ↑ "[Negative symptoms in schizophrenia – overview and practical implications]". Revue médicale suisse 14 (619): 1660–1664. 19 September 2018. doi:10.53738/REVMED.2018.14.619.1660. PMID 30230774.
- ↑ "Cognitive Models of Positive and Negative Symptoms of Schizophrenia and Implications for Treatment.". Psychiatria Danubina 31 (Suppl 2): 181–184. June 2019. PMID 31158119.
- ↑ "Apathy in schizophrenia: A review of neuropsychological and neuroanatomical studies.". Neuropsychologia 118 (Pt B): 22–33. September 2018. doi:10.1016/j.neuropsychologia.2017.09.033. PMID 28966139.
- ↑ 42.0 42.1 42.2 42.3 42.4 "Defining and measuring negative symptoms of schizophrenia in clinical trials". European Neuropsychopharmacology 24 (5): 737–743. May 2014. doi:10.1016/j.euroneuro.2013.10.016. PMID 24275698.
- ↑ 43.0 43.1 43.2 "The brief negative symptom scale in translation: A review of psychometric properties and beyond". European Neuropsychopharmacology 33: 36–44. April 2020. doi:10.1016/j.euroneuro.2020.01.018. PMID 32081498.
- ↑ "[Negative Symptoms in Schizophrenia – an Overview].". Therapeutische Umschau 75 (1): 51–56. June 2018. doi:10.1024/0040-5930/a000966. PMID 29909762.
- ↑ 45.0 45.1 Lindenmayer, Jean-Pierre; Nasrallah, Henry; Pucci, Michael; James, Steven; Citrome, Leslie (2013-07-01). "A systematic review of psychostimulant treatment of negative symptoms of schizophrenia: Challenges and therapeutic opportunities". Schizophrenia Research 147 (2): 241–252. doi:10.1016/j.schres.2013.03.019. ISSN 0920-9964. PMID 23619055. https://www.sciencedirect.com/science/article/abs/pii/S0920996413001655.
- ↑ "Clinical picture, pathogenesis and psychometric assessment of negative symptoms of schizophrenia.". Psychiatria Polska 52 (2): 185–197. 30 April 2018. doi:10.12740/PP/70610. PMID 29975360.
- ↑ 47.0 47.1 47.2 47.3 47.4 47.5 "Cognitive Functioning in Older Adults With Schizophrenia". Focus (American Psychiatric Publishing) 15 (1): 26–34. January 2017. doi:10.1176/appi.focus.20160032. PMID 31975837.
- ↑ 48.0 48.1 "Current understandings about cognition and the neurobiological correlates in schizophrenia". Journal of Neurosciences in Rural Practice 7 (3): 412–418. July 2016. doi:10.4103/0976-3147.176185. PMID 27365960.
- ↑ 49.0 49.1 "Longitudinal studies of cognition in first episode psychosis: a systematic review of the literature". The Australian and New Zealand Journal of Psychiatry 45 (2): 93–108. February 2011. doi:10.3109/00048674.2010.541418. PMID 21320033.
- ↑ "Is there evidence for late cognitive decline in chronic schizophrenia?". The Psychiatric Quarterly 83 (2): 127–144. June 2012. doi:10.1007/s11126-011-9189-8. PMID 21863346.
- ↑ 51.0 51.1 51.2 "Psychotic disorders in DSM-5 and ICD-11". CNS Spectrums 21 (4): 349–354. August 2016. doi:10.1017/S1092852916000316. PMID 27418328.
- ↑ 52.0 52.1 52.2 "[First-episode psychosis, cognitive difficulties and remediation]." (in fr). L'Encéphale 39 (Suppl 2): S83-92. September 2013. doi:10.1016/S0013-7006(13)70101-5. PMID 24084427.
- ↑ 53.0 53.1 53.2 "Recent Advances in the Early Intervention in Schizophrenia: Future Direction from Preclinical Findings". Current Psychiatry Reports 21 (8). 5 July 2019. doi:10.1007/s11920-019-1063-7. PMID 31278495.
- ↑ 54.0 54.1 54.2 54.3 54.4 54.5 "Nonsocial and social cognition in schizophrenia: current evidence and future directions". World Psychiatry 18 (2): 146–161. June 2019. doi:10.1002/wps.20624. PMID 31059632.
- ↑ "Face perception in schizophrenia: a specific deficit". Cognitive Neuropsychiatry 21 (1): 60–72. 2016. doi:10.1080/13546805.2015.1133407. PMID 26816133.
- ↑ "Cognitive remediation: a new generation of psychosocial interventions for people with schizophrenia". Social Work 57 (3): 235–246. July 2012. doi:10.1093/sw/sws008. PMID 23252315.
- ↑ "Semantic priming in schizophrenia: systematic review and meta-analysis". The British Journal of Psychiatry 192 (2): 92–97. February 2008. doi:10.1192/bjp.bp.106.032102. PMID 18245021.
- ↑ "Circumstances under which practice does not make perfect: a review of the practice effect literature in schizophrenia and its relevance to clinical treatment studies". Neuropsychopharmacology 35 (5): 1053–1062. April 2010. doi:10.1038/npp.2009.211. PMID 20090669.
- ↑ "A review of abnormalities in the perception of visual illusions in schizophrenia.". Psychonomic Bulletin and Review 24 (3): 734–751. June 2017. doi:10.3758/s13423-016-1168-5. PMID 27730532.
- ↑ "Facial emotion perception in schizophrenia: a meta-analytic review". Schizophrenia Bulletin 36 (5): 1009–1019. September 2010. doi:10.1093/schbul/sbn192. PMID 19329561.
- ↑ "[Social cognition in schizophrenia and autism spectrum disorder: Points of convergence and functional differences]". L'Encéphale 44 (6): 523–537. December 2018. doi:10.1016/j.encep.2018.03.004. PMID 30122298.
- ↑ "Neurological soft signs in familial and sporadic schizophrenia". Psychiatry Research 272: 222–229. February 2019. doi:10.1016/j.psychres.2018.12.105. PMID 30590276.
- ↑ "[Neurological soft signs in early onset schizophrenia]". L'Encephale 41 (3): 209–214. June 2015. doi:10.1016/j.encep.2014.01.005. PMID 24854724.
- ↑ 64.0 64.1 "[Very early onset schizophrenia]". L'Encephale 44 (6S): S8–S11. December 2018. doi:10.1016/S0013-7006(19)30071-5. PMID 30935493.
- ↑ "From Onset and Prodromal Stage to a Life-Long Course of Schizophrenia and Its Symptom Dimensions: How Sex, Age, and Other Risk Factors Influence Incidence and Course of Illness". Psychiatry Journal 2019. 2019. doi:10.1155/2019/9804836. PMID 31139639.
- ↑ "Advances in the Conceptualization and Study of Schizophrenia in Later Life". The Psychiatric Clinics of North America 41 (1): 39–53. March 2018. doi:10.1016/j.psc.2017.10.004. PMID 29412847.
- ↑ 67.0 67.1 67.2 "Understanding the schizophrenia prodrome". Indian Journal of Psychiatry 59 (4): 505–509. October 2017. doi:10.4103/psychiatry.IndianJPsychiatry_464_17. PMID 29497198.
- ↑ 68.0 68.1 "Identifying and treating the prodromal phases of bipolar disorder and schizophrenia". Current Treatment Options in Psychiatry 5 (1): 113–128. March 2018. doi:10.1007/s40501-018-0138-0. PMID 30364516.
- ↑ "[Cognitive deficits in first episode psychosis patients and people at risk for psychosis: from diagnosis to treatment]". L'Encephale 39 (Suppl 1): S64-71. May 2013. doi:10.1016/j.encep.2012.10.011. PMID 23528322.
- ↑ "Neurodevelopmental disorders: mechanisms and boundary definitions from genomes, interactomes and proteomes". Translational Psychiatry 3 (12): e329. December 2013. doi:10.1038/tp.2013.108. PMID 24301647.
- ↑ 71.0 71.1 71.2 "A review of vulnerability and risks for schizophrenia: Beyond the two hit hypothesis". Neuroscience and Biobehavioral Reviews 65: 185–194. June 2016. doi:10.1016/j.neubiorev.2016.03.017. PMID 27073049.
- ↑ 72.0 72.1 "Theranostic Biomarkers for Schizophrenia". International Journal of Molecular Sciences 18 (4): 733. March 2017. doi:10.3390/ijms18040733. PMID 28358316.
- ↑ 73.0 73.1 "[Risk factors of schizophrenia]" (in Finnish). Duodecim; Laaketieteellinen Aikakauskirja 126 (8): 869–876. 2010. PMID 20597333.
- ↑ 74.0 74.1 "Chapter 8: Schizophrenia: Etiological considerations". Adult psychopathology and diagnosis (6th ed.). John Wiley & Sons. 2011. ISBN 978-1-118-13884-7. https://books.google.com/books?id=iJtzm1KfU5oC&pg=PT282.
- ↑ "Recent advances in the genetics of schizophrenia". Human Molecular Genetics 12 Spec No 2: R125–133. October 2003. doi:10.1093/hmg/ddg302. PMID 12952866.
- ↑ 76.0 76.1 "Schizophrenia as a pseudogenetic disease: A call for more gene-environmental studies". Psychiatry Research 278: 146–150. August 2019. doi:10.1016/j.psychres.2019.06.006. PMID 31200193.
- ↑ 77.0 77.1 77.2 77.3 77.4 77.5 77.6 77.7 "Schizophrenia". BMJ 335 (7610): 91–95. July 2007. doi:10.1136/bmj.39227.616447.BE. PMID 17626963.
- ↑ "Evaluating historical candidate genes for schizophrenia". Molecular Psychiatry 20 (5): 555–562. May 2015. doi:10.1038/mp.2015.16. PMID 25754081.
- ↑ Schizophrenia and Psychotic Spectrum Disorders. Oxford University Press. 2016. pp. 124–125. ISBN 978-0-19-937806-7. https://books.google.com/books?id=7ukmDAAAQBAJ.
- ↑ "New statistical approaches exploit the polygenic architecture of schizophrenia—implications for the underlying neurobiology". Current Opinion in Neurobiology 36: 89–98. February 2016. doi:10.1016/j.conb.2015.10.008. PMID 26555806.
- ↑ "Mini-review: Update on the genetics of schizophrenia". Annals of Human Genetics 82 (5): 239–243. 2018. doi:10.1111/ahg.12259. ISSN 0003-4800. PMID 29923609. https://discovery.ucl.ac.uk/id/eprint/10064654/.
- ↑ "The Schizophrenia Polygenic Risk Score: To What Does It Predispose in Adolescence?". JAMA Psychiatry 73 (3): 193–194. March 2016. doi:10.1001/jamapsychiatry.2015.2964. PMID 26817666.
- ↑ 83.0 83.1 "Genomic Disorders in Psychiatry—What Does the Clinician Need to Know?". Current Psychiatry Reports 19 (11). September 2017. doi:10.1007/s11920-017-0831-5. PMID 28929285.
- ↑ "A systematic review and meta-analysis of the fertility of patients with schizophrenia and their unaffected relatives: Fertility in schizophrenia". Acta Psychiatrica Scandinavica 123 (2): 98–106. February 2011. doi:10.1111/j.1600-0447.2010.01623.x. PMID 20958271.
- ↑ "The evolutionary paradox and the missing heritability of schizophrenia". American Journal of Medical Genetics Part B: Neuropsychiatric Genetics 162 (2): 122–136. March 2013. doi:10.1002/ajmg.b.32135. PMID 23355297.
- ↑ "Schizophrenia". Lancet 388 (10039): 86–97. 2 July 2016. doi:10.1016/S0140-6736(15)01121-6. PMID 26777917. Bibcode: 2016Lanc..388...86O.
- ↑ "8-Hydroxy-2'-Deoxyguanosine and Reactive Oxygen Species as Biomarkers of Oxidative Stress in Mental Illnesses: A Meta-Analysis". Psychiatry Investig 18 (7): 603–618. July 2021. doi:10.30773/pi.2020.0417. PMID 34340273.
- ↑ "Non-Genetic Factors in Schizophrenia". Current Psychiatry Reports 21 (10). 14 September 2019. doi:10.1007/s11920-019-1091-3. PMID 31522306.
- ↑ "Maternal Obesity as a Risk Factor for Brain Development and Mental Health in the Offspring". Neuroscience 447: 122–135. 5 February 2020. doi:10.1016/j.neuroscience.2020.01.023. PMID 32032668.
- ↑ 90.0 90.1 "Cytokines, Oxidative Stress and Cellular Markers of Inflammation in Schizophrenia". Neuroinflammation and Schizophrenia. Current Topics in Behavioral Neurosciences. 44. 2020. pp. 49–66. doi:10.1007/7854_2018_88. ISBN 978-3-030-39140-9. http://pure-oai.bham.ac.uk/ws/files/74984176/Upthegrove_Khandaker_Cytokines_oxidative_stress_and_cellular_markers_of_inflammation_in_schizophrenia_Current_Topics_in_Behavioral_Neurosciences_2019.pdf.
- ↑ 91.0 91.1 "Vitamin D in schizophrenia: a clinical review". Evidence-Based Mental Health 19 (1): 6–9. February 2016. doi:10.1136/eb-2015-102117. PMID 26767392.
- ↑ "Infectious agents associated with schizophrenia: a meta-analysis". Schizophrenia Research 136 (1–3): 128–136. April 2012. doi:10.1016/j.schres.2011.10.026. PMID 22104141.
- ↑ "Viruses and schizophrenia: a focus on herpes simplex virus". Herpes 11 (Suppl 2): 83A–88A. June 2004. PMID 15319094.
- ↑ "Childhood infection and adult schizophrenia: a meta-analysis of population-based studies.". Schizophr. Res. 139 (1–3): 161–168. August 2012. doi:10.1016/j.schres.2012.05.023. PMID 22704639.
- ↑ "Cat Ownership and Schizophrenia-Related Disorders and Psychotic-Like Experiences: A Systematic Review and Meta-Analysis". Schizophrenia Bulletin 50 (3): 489–495. May 2024. doi:10.1093/schbul/sbad168. PMID 38491934.
- ↑ Israel, Ariel; Weizman, Abraham; Israel, Sarah; Stokar, Joshua; Ashkenazi, Shai; Vinker, Shlomo; Magen, Eli; Merzon, Eugene (2026-01-01). "Systematic screening identifies medication and disease factors associated with schizophrenia risk". Brain, Behavior, and Immunity 131. doi:10.1016/j.bbi.2025.106135. ISSN 0889-1591. PMID 41106616. https://www.sciencedirect.com/science/article/pii/S0889159125003770.
- ↑ 97.0 97.1 "Childhood adversity and trauma:experiences of professionals trained to routinely enquire about childhood adversity". Heliyon 5 (7). July 2019. doi:10.1016/j.heliyon.2019.e01900. PMID 31372522. Bibcode: 2019Heliy...501900P.
- ↑ "Childhood trauma and psychosis". Child and Adolescent Psychiatric Clinics of North America 22 (4): 629–641. October 2013. doi:10.1016/j.chc.2013.04.006. PMID 24012077.
- ↑ "Toward a unified theory of childhood trauma and psychosis: A comprehensive review of epidemiological, clinical, neuropsychological and biological findings". Neuroscience and Biobehavioral Reviews 75: 393–406. April 2017. doi:10.1016/j.neubiorev.2017.02.015. PMID 28216171.
- ↑ 100.0 100.1 "Early-Life Adversity, Systemic Inflammation and Comorbid Physical and Psychiatric Illnesses of Adult Life". Neuroinflammation and Schizophrenia. Current Topics in Behavioral Neurosciences. 44. 2020. pp. 207–225. doi:10.1007/7854_2019_89. ISBN 978-3-030-39140-9. https://kclpure.kcl.ac.uk/portal/en/publications/earlylife-adversity-systemic-inflammation-and-comorbid-physical-and-psychiatric-illnesses-of-adult-life(d2cdfc38-19e7-4918-80f1-5525e6ff45bf).html.
- ↑ "The slow death of the concept of schizophrenia and the painful birth of the psychosis spectrum". Psychological Medicine 48 (2): 229–244. January 2018. doi:10.1017/S0033291717001775. PMID 28689498.
- ↑ "Urban environment and psychiatric disorders: a review of the neuroscience and biology". Metabolism: Clinical and Experimental 100S. November 2019. doi:10.1016/j.metabol.2019.07.004. PMID 31610855.
- ↑ "Does the urban environment cause psychosis?". The British Journal of Psychiatry 184 (4): 287–8. April 2004. doi:10.1192/bjp.184.4.287. PMID 15056569.
- ↑ "Environmental pollution and risk of psychotic disorders: A review of the science to date". Schizophrenia Research 181: 55–59. March 2017. doi:10.1016/j.schres.2016.10.003. PMID 27720315.
- ↑ "Migration and schizophrenia". Current Opinion in Psychiatry 20 (2): 111–115. March 2007. doi:10.1097/YCO.0b013e328017f68e. PMID 17278906.
- ↑ Emamzadeh, Arash. "The Truth About Schizophrenia in Immigrants | Psychology Today" (in en-US). https://www.psychologytoday.com/us/blog/finding-a-new-home/201807/the-truth-about-schizophrenia-in-immigrants.
- ↑ "Effects of increased paternal age on sperm quality, reproductive outcome and associated epigenetic risks to offspring". Reproductive Biology and Endocrinology 13. April 2015. doi:10.1186/s12958-015-0028-x. PMID 25928123.
- ↑ 108.0 108.1 "Reasons for increased substance use in psychosis". Clinical Psychology Review 27 (4): 494–510. May 2007. doi:10.1016/j.cpr.2006.09.004. PMID 17240501.
- ↑ "Smoking and schizophrenia". Psychiatria Danubina 21 (3): 371–375. September 2009. PMID 19794359.
- ↑ Tandon, Rajiv; Shariff, Sonia Motin (September 2019). "Substance-Induced Psychotic Disorders and Schizophrenia: Pathophysiological Insights and Clinical Implications". American Journal of Psychiatry 176 (9): 683–684. doi:10.1176/appi.ajp.2019.19070734. ISSN 0002-953X. PMID 31474121. https://psychiatryonline.org/doi/10.1176/appi.ajp.2019.19070734.
- ↑ "Alcohol-Related Psychosis". EMedicine. 30 March 2006. http://www.emedicine.com/med/topic3113.htm. Retrieved 27 September 2006.
- ↑ "Cannabis and psychiatric disorders: it is not only addiction". Addiction Biology 13 (2): 264–75. June 2008. doi:10.1111/j.1369-1600.2008.00106.x. PMID 18482435.
- ↑ 113.0 113.1 113.2 113.3 "Unique Effects of Clozapine: A Pharmacological Perspective". Apprentices to Genius: A tribute to Solomon H. Snyder. Advances in Pharmacology. 82. 2018. pp. 137–162. doi:10.1016/bs.apha.2017.09.009. ISBN 978-0-12-814087-1.
- ↑ "Psychosocial and psychological interventions for relapse prevention in schizophrenia: a systematic review and network meta-analysis". Lancet Psychiatry 8 (11): 969–980. November 2021. doi:10.1016/S2215-0366(21)00243-1. PMID 34653393. https://boris.unibe.ch/160225/8/Bighelli_LancetPsychiatry_2021.pdf.
- ↑ "The Association Between Cannabis Use and Schizophrenia: Causative or Curative? A Systematic Review". Cureus 12 (7). July 2020. doi:10.7759/cureus.9309. PMID 32839678.
- ↑ "Cannabis use and psychosis: a review of reviews". Eur Arch Psychiatry Clin Neurosci 270 (4): 403–412. June 2020. doi:10.1007/s00406-019-01068-z. PMID 31563981.
- ↑ "Causes — Schizophrenia". UK National Health Service. 11 November 2019. https://www.nhs.uk/mental-health/conditions/schizophrenia/causes/.
- ↑ "Cannabis consumption and psychosis or schizophrenia development". The International Journal of Social Psychiatry 64 (7): 690–704. November 2018. doi:10.1177/0020764018801690. PMID 30442059.
- ↑ "Dilemmas in the treatment of early-onset first-episode psychosis". Therapeutic Advances in Psychopharmacology 8 (8): 231–239. August 2018. doi:10.1177/2045125318765725. PMID 30065814.
- ↑ "How Schizophrenia Develops: Cognitive and Brain Mechanisms Underlying Onset of Psychosis". Trends Cogn Sci 19 (12): 744–756. December 2015. doi:10.1016/j.tics.2015.09.009. PMID 26493362.
- ↑ "Negative Symptoms in Schizophrenia: A Review and Clinical Guide for Recognition, Assessment, and Treatment". Neuropsychiatric Disease and Treatment 16: 519–534. 2020. doi:10.2147/NDT.S225643. PMID 32110026.
- ↑ "The Role of Genes, Stress, and Dopamine in the Development of Schizophrenia". Biological Psychiatry 81 (1): 9–20. 1 January 2017. doi:10.1016/j.biopsych.2016.07.014. PMID 27720198.
- ↑ "Dopamine, cognitive biases and assessment of certainty: A neurocognitive model of delusions". Clinical Psychology Review 54: 96–106. June 2017. doi:10.1016/j.cpr.2017.04.006. PMID 28448827. https://kclpure.kcl.ac.uk/portal/en/publications/dopamine-cognitive-biases-and-assessment-of-certainty-a-neurocognitive-model-of-delusions(138513dd-3a44-4deb-bac1-be45767ef51b).html.
- ↑ "Schizophrenia: an integrated sociodevelopmental-cognitive model". Lancet 383 (9929): 1677–1687. May 2014. doi:10.1016/S0140-6736(13)62036-X. PMID 24315522.
- ↑ "Dysregulation of the dopamine system in the pathophysiology of schizophrenia and depression". Nature Reviews. Neuroscience 17 (8): 524–532. August 2016. doi:10.1038/nrn.2016.57. PMID 27256556.
- ↑ "Striatal presynaptic dopamine in schizophrenia, part II: meta-analysis of [(18)F/(11)C-DOPA PET studies"]. Schizophrenia Bulletin 39 (1): 33–42. January 2013. doi:10.1093/schbul/sbr180. PMID 22282454.
- ↑ "The nature of dopamine dysfunction in schizophrenia and what this means for treatment". Archives of General Psychiatry 69 (8): 776–786. August 2012. doi:10.1001/archgenpsychiatry.2012.169. PMID 22474070.
- ↑ "Novel Dopamine Therapeutics for Cognitive Deficits in Schizophrenia". Biological Psychiatry 81 (1): 67–77. January 2017. doi:10.1016/j.biopsych.2015.12.028. PMID 26946382.
- ↑ "An Integrative Perspective on the Role of Dopamine in Schizophrenia". Biological Psychiatry 81 (1): 52–66. January 2017. doi:10.1016/j.biopsych.2016.05.021. PMID 27452791.
- ↑ 130.0 130.1 "Thalamo-cortical communication, glutamatergic neurotransmission and neural oscillations: A unique window into the origins of ScZ?". Schizophrenia Research 180: 4–12. February 2017. doi:10.1016/j.schres.2016.05.013. PMID 27317361. https://eprints.gla.ac.uk/132874/1/132874.pdf.
- ↑ "A quantitative review of the post-mortem evidence for decreased cortical N-methyl-D-aspartate receptor expression levels in schizophrenia: How can we link molecular abnormalities to mismatch negativity deficits?". Biological Psychology 116: 57–67. April 2016. doi:10.1016/j.biopsycho.2015.10.013. PMID 26549579.
- ↑ "The neurobiology of MMN and implications for schizophrenia". Biological Psychology 116: 90–97. April 2016. doi:10.1016/j.biopsycho.2016.01.011. PMID 26826620.
- ↑ 133.0 133.1 "Interneuron dysfunction in psychiatric disorders". Nature Reviews. Neuroscience 13 (2): 107–120. January 2012. doi:10.1038/nrn3155. PMID 22251963.
- ↑ "Cortical inhibitory neurons and schizophrenia". Nature Reviews. Neuroscience 6 (4): 312–324. April 2005. doi:10.1038/nrn1648. PMID 15803162.
- ↑ "Dysfunctional prefrontal gamma-band oscillations reflect working memory and other cognitive deficits in schizophrenia". Biological Psychiatry 77 (12): 1010–1019. June 2015. doi:10.1016/j.biopsych.2015.02.034. PMID 25847179. "Several studies that investigated perceptual processes found impaired GBR in ScZ patients over sensory areas, such as the auditory and visual cortex. Moreover, studies examining steady-state auditory-evoked potentials showed deficits in the gen- eration of oscillations in the gamma band.".
- ↑ "Gamma band oscillations in the early phase of psychosis: A systematic review". Neuroscience and Biobehavioral Reviews 90: 381–399. July 2018. doi:10.1016/j.neubiorev.2018.04.006. PMID 29656029. https://kclpure.kcl.ac.uk/portal/en/publications/e2f500b7-f358-433d-9f9c-7f6b9c52bb2f. "Decreased gamma power in response to a task was a relatively consistent finding, with 5 out of 6 studies reported reduced evoked or induced power.".
- ↑ 137.0 137.1 "Mechanisms of astrocyte development and their contributions to neurodevelopmental disorders". Curr Opin Neurobiol 27: 75–81. August 2014. doi:10.1016/j.conb.2014.03.005. PMID 24694749.
- ↑ "Cognitive control deficits in schizophrenia: mechanisms and meaning". Neuropsychopharmacology 36 (1): 316–338. January 2011. doi:10.1038/npp.2010.156. PMID 20844478.
- ↑ "Cognition in schizophrenia: core psychological and neural mechanisms". Trends in Cognitive Sciences 16 (1): 27–34. January 2012. doi:10.1016/j.tics.2011.11.015. PMID 22169777.
- ↑ "Executive function, neural circuitry, and genetic mechanisms in schizophrenia". Neuropsychopharmacology 35 (1): 258–277. January 2010. doi:10.1038/npp.2009.111. PMID 19693005.
- ↑ "Positive symptoms associate with cortical thinning in the superior temporal gyrus via the ENIGMA Schizophrenia consortium". Acta Psychiatrica Scandinavica 135 (5): 439–447. May 2017. doi:10.1111/acps.12718. PMID 28369804.
- ↑ "Prefrontal cortical thinning links to negative symptoms in schizophrenia via the ENIGMA consortium". Psychological Medicine 48 (1): 82–94. January 2018. doi:10.1017/S0033291717001283. PMID 28545597.
- ↑ "Emotional experience in patients with schizophrenia revisited: meta-analysis of laboratory studies". Schizophrenia Bulletin 36 (1): 143–150. January 2010. doi:10.1093/schbul/sbn061. PMID 18562345.
- ↑ "A new perspective on anhedonia in schizophrenia". The American Journal of Psychiatry 169 (4): 364–373. April 2012. doi:10.1176/appi.ajp.2011.11030447. PMID 22407079.
- ↑ "Cognitive and Motivational Neuroscience of Psychotic Disorders". Charney & Nestler's Neurobiology of Mental Illness (5th ed.). New York: Oxford University Press.. 2018. pp. 215, 217. ISBN 978-0-19-068142-5. "Several recent reviews (e.g., Cohen and Minor, 2010) have found that individuals with schizophrenia show relatively intact self-reported emotional responses to affect-eliciting stimuli as well as other indicators of intact response(215)...Taken together, the literature increasingly suggests that there may be a deficit in putatively DA-mediated reward learning and/ or reward prediction functions in schizophrenia. Such findings suggest that impairment in striatal reward prediction mechanisms may influence "wanting" in schizophrenia in a way that reduces the ability of individuals with schizophrenia to use anticipated rewards to drive motivated behavior.(217)"
- ↑ 146.0 146.1 "Handedness, language areas and neuropsychiatric diseases: insights from brain imaging and genetics". Brain 142 (10): 2938–2947. October 2019. doi:10.1093/brain/awz257. PMID 31504236.
- ↑ "Intra- and Inter-hemispheric Connectivity Supporting Hemispheric Specialization". Micro-, Meso- and Macro-Connectomics of the Brain. Research and Perspectives in Neurosciences. 2016. pp. 129–146. doi:10.1007/978-3-319-27777-6_9. ISBN 978-3-319-27776-9.
- ↑ "Laterality and mental disorders in the postgenomic age—A closer look at schizophrenia and language lateralization". Neuroscience and Biobehavioral Reviews 59: 100–110. December 2015. doi:10.1016/j.neubiorev.2015.08.019. PMID 26598216.
- ↑ "Computational psychiatry: the brain as a phantastic organ". The Lancet. Psychiatry 1 (2): 148–158. July 2014. doi:10.1016/S2215-0366(14)70275-5. PMID 26360579.
- ↑ "Predictive Processing, Source Monitoring, and Psychosis". Annual Review of Clinical Psychology 13: 265–289. May 2017. doi:10.1146/annurev-clinpsy-032816-045145. PMID 28375719.
- ↑ "Perceiving is believing: a Bayesian approach to explaining the positive symptoms of schizophrenia". Nature Reviews. Neuroscience 10 (1): 48–58. January 2009. doi:10.1038/nrn2536. PMID 19050712. https://pure.au.dk/ws/files/48560345/fletcher_frithNRN.pdf.
- ↑ "Toward a neurobiology of delusions". Progress in Neurobiology 92 (3): 345–369. November 2010. doi:10.1016/j.pneurobio.2010.06.007. PMID 20558235.
- ↑ "Canonical microcircuits for predictive coding". Neuron 76 (4): 695–711. November 2012. doi:10.1016/j.neuron.2012.10.038. PMID 23177956.
- ↑ Nettle, Daniel; Clegg, Helen (2006-03-07). "Schizotypy, creativity and mating success in humans" (in en). Proceedings of the Royal Society B: Biological Sciences 273 (1586): 611–615. doi:10.1098/rspb.2005.3349. ISSN 0962-8452. PMID 16537133.
- ↑ Crow, T (March 2000). "Schizophrenia as the price that Homo sapiens pays for language: a resolution of the central paradox in the origin of the species". Brain Research Reviews 31 (2–3): 118–129. doi:10.1016/S0165-0173(99)00029-6. PMID 10719140. https://linkinghub.elsevier.com/retrieve/pii/S0165017399000296.
- ↑ "How to approach the mental state examination". BMJ 357. 8 May 2017. doi:10.1136/sbmj.j1821. PMID 31055448. https://www.bmj.com/content/357/sbmj.j1821. Retrieved 9 January 2020.
- ↑ "Are Shorter Versions of the Positive and Negative Syndrome Scale (PANSS) Doable? A Critical Review.". Innovations in Clinical Neuroscience 14 (11–12): 73–76. 1 December 2017. PMID 29410940.
- ↑ "Diagnosis of schizophrenia". Australian Department of Health. 10 January 2019. https://www.healthdirect.gov.au/diagnosis-of-schizophrenia.
- ↑ "Schizophrenia – Diagnosis". UK National Health Service. 23 October 2017. https://www.nhs.uk/conditions/schizophrenia/diagnosis/.
- ↑ "Reliability of clinical ICD-10 schizophrenia diagnoses". Nordic Journal of Psychiatry 59 (3): 209–212. 2005. doi:10.1080/08039480510027698. PMID 16195122.
- ↑ Whitfield-Gabrieli, Susan; Ford, Judith M. (2012-04-27). "Default Mode Network Activity and Connectivity in Psychopathology" (in en). Annual Review of Clinical Psychology 8 (1): 49–76. doi:10.1146/annurev-clinpsy-032511-143049. ISSN 1548-5943. PMID 22224834. https://www.annualreviews.org/doi/10.1146/annurev-clinpsy-032511-143049.
- ↑ Menon, Vinod (October 2011). "Large-scale brain networks and psychopathology: a unifying triple network model" (in en). Trends in Cognitive Sciences 15 (10): 483–506. doi:10.1016/j.tics.2011.08.003. PMID 21908230. https://linkinghub.elsevier.com/retrieve/pii/S1364661311001719.
- ↑ Baker, Justin T.; Holmes, Avram J.; Masters, Grace A.; Yeo, B. T. Thomas; Krienen, Fenna; Buckner, Randy L.; Öngür, Dost (2014-02-01). "Disruption of Cortical Association Networks in Schizophrenia and Psychotic Bipolar Disorder" (in en). JAMA Psychiatry 71 (2): 109–118. doi:10.1001/jamapsychiatry.2013.3469. ISSN 2168-622X. PMID 24306091.
- ↑ 164.0 164.1 164.2 "[Risk of homicide and major mental disorders: a critical review]". L'Encephale 35 (6): 521–530. December 2009. doi:10.1016/j.encep.2008.10.009. PMID 20004282.
- ↑ 165.0 165.1 "Sleep disorders in schizophrenia". Fortschritte der Neurologie-Psychiatrie 78 (2): 70–80. February 2010. doi:10.1055/s-0028-1109967. PMID 20066610.
- ↑ 166.0 166.1 "Basic Neuroscience Illuminates Causal Relationship Between Sleep and Memory: Translating to Schizophrenia". Schizophrenia Bulletin 44 (1): 7–14. 13 January 2018. doi:10.1093/schbul/sbx151. PMID 29136236.
- ↑ 167.0 167.1 "Sleep and circadian rhythm dysregulation in schizophrenia". Progress in Neuro-Psychopharmacology & Biological Psychiatry 43: 209–216. June 2013. doi:10.1016/j.pnpbp.2012.12.021. PMID 23318689.
- ↑ "Light therapies to improve sleep in intrinsic circadian rhythm sleep disorders and neuro-psychiatric illness: A systematic review and meta-analysis". Sleep Medicine Reviews 46: 108–123. August 2019. doi:10.1016/j.smrv.2019.04.012. PMID 31108433.
- ↑ "Genetic Variations Associated with Sleep Disorders in Patients with Schizophrenia: A Systematic Review". Medicines 5 (2): 27. March 2018. doi:10.3390/medicines5020027. PMID 29587340.
- ↑ "Somatic Comorbidity in Schizophrenia: Some Possible Biological Mechanisms Across the Life Span". Schizophrenia Bulletin 42 (6): 1316–1319. 2016. doi:10.1093/schbul/sbw028. PMID 27033328.
- ↑ "Psychosis". Continuum (Minneap Minn) 24 (3): 845–860. June 2018. doi:10.1212/CON.0000000000000602. PMID 29851881.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedFerri2010 - ↑ "Differential Diagnosis of Borderline Personality Disorder". The Psychiatric Clinics of North America 41 (4): 575–582. December 2018. doi:10.1016/j.psc.2018.07.001. PMID 30447725.
- ↑ "Comorbidity: Schizophrenia With Obsessive-Compulsive Disorder". Psychiatric Times 26 (4). 15 April 2009. http://www.psychiatrictimes.com/display/article/10168/1402540.
- ↑ "Distinguishing schizophrenia from posttraumatic stress disorder with psychosis". Curr Opin Psychiatry 28 (3): 249–255. May 2015. doi:10.1097/YCO.0000000000000158. PMID 25785709.
- ↑ "Depression and Psychosis in Neurological Practice". Bradley's neurology in clinical practice. 1 (6th ed.). Philadelphia, PA: Elsevier/Saunders. 2012. pp. 92–111. ISBN 978-1-4377-0434-1.
- ↑ "Examination of Dosing of Antipsychotic Drugs for Relapse Prevention in Patients With Stable Schizophrenia: A Meta-analysis". JAMA Psychiatry 78 (11): 1238–1248. November 2021. doi:10.1001/jamapsychiatry.2021.2130. PMID 34406325.
- ↑ "The empirical status of the ultra high-risk (prodromal) research paradigm". Schizophrenia Bulletin 33 (3): 661–664. May 2007. doi:10.1093/schbul/sbm031. PMID 17470445.
- ↑ "Specialised early intervention teams for recent-onset psychosis". Cochrane Database Syst Rev 11 (11). November 2020. doi:10.1002/14651858.CD013288.pub2. PMID 33135811. "p. 22: There is low-certainty evidence for the use of SEl services in comparison to TAU for a small reduction in psychiatric hospitalisation, and moderate-certainty evidence of a large effect of reduction in disengagement from mental health services. There is moderate-certainty evidence that SEI results in a small reduction of positive (hallucinations, delusions and disordered thinking) and negative symptoms (social withdrawal, flat or blunted affect, and poverty of speech) and low-certainty evidence that it greatly increases satisfaction in care, while there is low-certainty evidence that it improves general functioning and the likelihood of recovery. These effects were only observed during treatment and there was no evidence that outcomes are improved after the treatment has finished, although these were based on only one trial.".
- ↑ "Early interventions to prevent psychosis: systematic review and meta-analysis". BMJ 346: f185. January 2013. doi:10.1136/bmj.f185. PMID 23335473.
- ↑ 181.0 181.1 "Are we getting any better at staying better? The long view on relapse and recovery in first episode nonaffective psychosis and schizophrenia". Therapeutic Advances in Psychopharmacology 9: 204512531987003. September 2019. doi:10.1177/2045125319870033. PMID 31523418.
- ↑ "Beyond Psychopharmacology: Emerging Psychosocial Interventions for Core Symptoms of Schizophrenia.". Focus (American Psychiatric Publishing) 14 (3): 315–327. July 2016. doi:10.1176/appi.focus.20160014. PMID 31975812.
- ↑ "Cognitive training for supported employment: 2–3 year outcomes of a randomized controlled trial". The American Journal of Psychiatry 164 (3): 437–441. March 2007. doi:10.1176/appi.ajp.164.3.437. PMID 17329468.
- ↑ "[Duration of untreated psychosis: A state-of-the-art review and critical analysis]". Encephale 42 (4): 361–366. August 2016. doi:10.1016/j.encep.2015.09.007. PMID 27161262.
- ↑ "Deinstitutionalization and the rise of violence.". CNS Spectrums 20 (3): 207–214. June 2015. doi:10.1017/S1092852914000753. PMID 25683467.
- ↑ 186.0 186.1 186.2 "Schizophrenia – Treatment". UK National Health Service. 23 October 2017. https://www.nhs.uk/conditions/schizophrenia/treatment/.
- ↑ "Modafinil for people with schizophrenia or related disorders". The Cochrane Database of Systematic Reviews 12 (12). December 2019. doi:10.1002/14651858.CD008661.pub2. PMID 31828767.
- ↑ "Antipsychotic medication in schizophrenia: a review". British Medical Bulletin 114 (1): 169–179. June 2015. doi:10.1093/bmb/ldv017. PMID 25957394.
- ↑ "Stopping and switching antipsychotic drugs". Australian Prescriber 42 (5): 152–157. October 2019. doi:10.18773/austprescr.2019.052. PMID 31631928.
- ↑ "Does long-term treatment of schizophrenia with antipsychotic medications facilitate recovery?". Schizophrenia Bulletin 39 (5): 962–5. September 2013. doi:10.1093/schbul/sbt034. PMID 23512950.
- ↑ "Treatment-Resistant Schizophrenia". The Psychiatric Clinics of North America 39 (2): 239–65. June 2016. doi:10.1016/j.psc.2016.01.006. PMID 27216902.
- ↑ "Is treatment-resistant schizophrenia categorically distinct from treatment-responsive schizophrenia? a systematic review". BMC Psychiatry 17 (1). 13 January 2017. doi:10.1186/s12888-016-1177-y. PMID 28086761.
- ↑ "Clozapine versus typical neuroleptic medication for schizophrenia". The Cochrane Database of Systematic Reviews 2009 (1). January 2009. doi:10.1002/14651858.CD000059.pub2. PMID 19160174.
- ↑ "Insight in schizophrenia: a review". Current Psychiatry Reports 12 (4): 356–361. August 2010. doi:10.1007/s11920-010-0125-7. PMID 20526897.
- ↑ "Long-Acting Injections in Schizophrenia: a 3-Year Update on Randomized Controlled Trials Published January 2016 – March 2019". Current Psychiatry Reports 21 (12). November 2019. doi:10.1007/s11920-019-1114-0. PMID 31745659.
- ↑ "Antipsychotic drugs versus placebo for relapse prevention in schizophrenia: a systematic review and meta-analysis". Lancet 379 (9831): 2063–2071. June 2012. doi:10.1016/S0140-6736(12)60239-6. PMID 22560607.
- ↑ "Risks versus benefits of different types of long-acting injectable antipsychotics". The Journal of Clinical Psychiatry 67 (Suppl 5): 15–18. 2006. PMID 16822092.
- ↑ Saint-Georges, Zacharie; MacDonald, Julia; Al-Khalili, Roya; Hamati, Rami; Solmi, Marco; Keshavan, Matcheri S.; Tuominen, Lauri; Guimond, Synthia (20 May 2025). "Cholinergic system in schizophrenia: A systematic review and meta-analysis" (in en). Molecular Psychiatry 30 (7): 3301–3315. doi:10.1038/s41380-025-03023-y. ISSN 1476-5578. PMID 40394282.
- ↑ 199.0 199.1 "FDA Approves Drug with New Mechanism of Action for Treatment of Schizophrenia". U.S. Food and Drug Administration (FDA) (Press release). 26 September 2024. Archived from the original on 27 September 2024. Retrieved 27 September 2024.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ "U.S. Food and Drug Administration Approves Bristol Myers Squibb's Cobenfy (xanomeline and trospium chloride), a First-In-Class Muscarinic Agonist for the Treatment of Schizophrenia in Adults" (Press release). Bristol Myers Squibb. 27 September 2024. Retrieved 27 September 2024 – via Business Wire.
- ↑ Sapienza, Jacopo; Martini, Francesca; Comai, Stefano; Cavallaro, Roberto; Spangaro, Marco; De Gregorio, Danilo; Bosia, Marta (2024-09-18). "Psychedelics and schizophrenia: a double-edged sword" (in en). Molecular Psychiatry 30 (2): 679–692. doi:10.1038/s41380-024-02743-x. ISSN 1476-5578. PMID 39294303. https://www.nature.com/articles/s41380-024-02743-x.
- ↑ 202.0 202.1 "Akathisia and Newer Second-Generation Antipsychotic Drugs: A Review of Current Evidence". Pharmacotherapy 40 (6): 565–574. June 2020. doi:10.1002/phar.2404. PMID 32342999.
- ↑ "Tardive dyskinesia risk with first- and second-generation antipsychotics in comparative randomized controlled trials: a meta-analysis". World Psychiatry 17 (3): 330–340. October 2018. doi:10.1002/wps.20579. PMID 30192088.
- ↑ 204.0 204.1 "Family intervention for schizophrenia". The Cochrane Database of Systematic Reviews 12 (12). December 2010. doi:10.1002/14651858.CD000088.pub2. PMID 21154340.
- ↑ "Cognitive remediation in schizophrenia: the earlier the better?". Epidemiology and Psychiatric Sciences 29. September 2019. doi:10.1017/S2045796019000532. PMID 31556864.
- ↑ Bighelli, Irene; Salanti, Georgia; Huhn, Maximilian; Schneider-Thoma, Johannes; Krause, Marc; Reitmeir, Cornelia; Wallis, Sofia; Schwermann, Felicitas et al. (October 2025). "Psychological Interventions to Reduce Positive Symptoms in Schizophrenia: Systematic Review and Network Meta-Analysis". Focus 23 (4): 475–488. doi:10.1176/appi.focus.25023024. ISSN 1541-4094. https://psychiatryonline.org/doi/abs/10.1176/appi.focus.25023024.
- ↑ "Effectiveness of metacognitive interventions for mental disorders in adults-A systematic review and meta-analysis (METACOG)". Clinical Psychology & Psychotherapy 26 (2): 227–240. March 2019. doi:10.1002/cpp.2345. PMID 30456821.
- ↑ "Systematic review and meta-analysis of metacognitive abilities in individuals with schizophrenia spectrum disorders". Neuroscience and Biobehavioral Reviews 126: 329–337. July 2021. doi:10.1016/j.neubiorev.2021.03.017. PMID 33757817. https://hal.archives-ouvertes.fr/hal-03178486/file/2020.12.03.20243113v1.full.pdf.
- ↑ "The 2009 schizophrenia PORT psychosocial treatment recommendations and summary statements". Schizophrenia Bulletin 36 (1): 48–70. January 2010. doi:10.1093/schbul/sbp115. PMID 19955389.
- ↑ "The critical ingredients of assertive community treatment.". World Psychiatry 14 (2): 240–242. June 2015. doi:10.1002/wps.20234. PMID 26043344.
- ↑ "[Using resource groups in assertive community treatment; literature review and recommendation].". Tijdschrift voor Psychiatrie 59 (8): 466–473. 2017. PMID 28880347.
- ↑ "Intensive case management for severe mental illness". The Cochrane Database of Systematic Reviews 1 (1). 6 January 2017. doi:10.1002/14651858.CD007906.pub3. PMID 28067944.
- ↑ "Cognitive-behavioural therapy for the symptoms of schizophrenia: systematic review and meta-analysis with examination of potential bias". The British Journal of Psychiatry 204 (1): 20–29. January 2014. doi:10.1192/bjp.bp.112.116285. PMID 24385461.
- ↑ 214.0 214.1 "Cognitive behavioural therapy plus standard care versus standard care plus other psychosocial treatments for people with schizophrenia". The Cochrane Database of Systematic Reviews 11 (11). November 2018. doi:10.1002/14651858.CD008712.pub3. PMID 30480760.
- ↑ Health Quality Ontario (2018). "Cognitive Behavioural Therapy for Psychosis: A Health Technology Assessment". Ontario Health Technology Assessment Series 18 (5): 1–141. PMID 30443277.
- ↑ "Art therapy for schizophrenia or schizophrenia-like illnesses". The Cochrane Database of Systematic Reviews 2010 (4). October 2005. doi:10.1002/14651858.CD003728.pub2. PMID 16235338. PMC 12359299. http://www.cochrane.org/reviews/en/ab003728.html.
- ↑ "Drama therapy for schizophrenia or schizophrenia-like illnesses". The Cochrane Database of Systematic Reviews (1). January 2007. doi:10.1002/14651858.CD005378.pub2. PMID 17253555. http://www.cochrane.org/reviews/en/ab005378.html.
- ↑ "Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for the management of schizophrenia and related disorders". Aust N Z J Psychiatry 50 (5): 410–472. May 2016. doi:10.1177/0004867416641195. PMID 27106681.
- ↑ "Peer support for people with schizophrenia or other serious mental illness.". The Cochrane Database of Systematic Reviews 4 (6). 4 April 2019. doi:10.1002/14651858.CD010880.pub2. PMID 30946482.
- ↑ 220.0 220.1 "Exercise as a Treatment for Schizophrenia: A Review.". Psychopharmacology Bulletin 49 (1): 56–69. 15 February 2019. doi:10.64719/pb.4584. PMID 30858639.
- ↑ 221.0 221.1 "Aerobic Exercise Improves Cognitive Functioning in People With Schizophrenia: A Systematic Review and Meta-Analysis". Schizophrenia Bulletin 43 (3): 546–556. 1 May 2017. doi:10.1093/schbul/sbw115. PMID 27521348.
- ↑ "[Physical activity in patients with schizophrenia: From neurobiology to clinical benefits].". L'Encéphale 44 (6): 538–547. December 2018. doi:10.1016/j.encep.2018.05.005. PMID 29983176.
- ↑ "Quality statement 7: Promoting healthy eating, physical activity and smoking cessation | Psychosis and schizophrenia in adults". UK National Institute for Health and Care Excellence. 12 February 2015. https://www.nice.org.uk/guidance/qs80/chapter/Quality-statement-7-Promoting-healthy-eating-physical-activity-and-smoking-cessation.
- ↑ 224.0 224.1 224.2 "Nutritional Deficiencies and Clinical Correlates in First-Episode Psychosis: A Systematic Review and Meta-analysis". Schizophrenia Bulletin 44 (6): 1275–1292. October 2018. doi:10.1093/schbul/sbx162. PMID 29206972.
- ↑ 225.0 225.1 225.2 225.3 "Pathogenesis and management of Brugada syndrome in schizophrenia: A scoping review". General Hospital Psychiatry 67: 83–91. October 2020. doi:10.1016/j.genhosppsych.2020.09.003. PMID 33065406.
- ↑ "Enhancement of recovery from mental illness with l-methylfolate supplementation". Perspectives in Psychiatric Care 54 (2): 331–334. April 2018. doi:10.1111/ppc.12227. PMID 28597528.
- ↑ 227.0 227.1 "The efficacy and safety of nutrient supplements in the treatment of mental disorders: a meta-review of meta-analyses of randomized controlled trials". World Psychiatry 18 (3): 308–324. October 2019. doi:10.1002/wps.20672. PMID 31496103.
- ↑ "Cardiovascular disease in patients with schizophrenia". The Medical Journal of Australia 206 (2): 91–95. 6 February 2017. doi:10.5694/mja16.00650. PMID 28152356.
- ↑ "Schizophrenia—a predictor of suicide during the second half of life?". Schizophrenia Research 134 (2–3): 111–117. February 2012. doi:10.1016/j.schres.2011.09.032. PMID 22018943.
- ↑ Primary Care Medicine: Office Evaluation and Management of The Adult Patient (Sixth ed.). Lippincott Williams & Wilkins. 2011. p. Chapter 101. ISBN 978-1-4511-2159-9. https://books.google.com/books?id=fXpKo1afC2YC&pg=PT1766.
- ↑ 231.0 231.1 "Role of Naltrexone in Improving Compulsive Drinking in Psychogenic Polydipsia.". Cureus 11 (8). 5 August 2019. doi:10.7759/cureus.5320. PMID 31598428.
- ↑ "Schizophrenia Mortality: Barriers to Progress". The Psychiatric Quarterly 90 (3): 553–563. September 2019. doi:10.1007/s11126-019-09645-0. PMID 31147816.
- ↑ 233.0 233.1 233.2 233.3 Farrell, Michael (2024). Controversies in schizophrenia: issues, causes, and treatment. New York, NY: Routledge, Taylor & Francis Group. ISBN 978-1-003-41355-4.
- ↑ 234.0 234.1 234.2 234.3 Assis, Jorge Cândido de; Villares, Cecília Cruz; Bressan, Rodrigo Affonseca (2023) (in en). Between Reason and Illusion: Demystifying Schizophrenia. Copernicus Books. Cham: Springer Nature Switzerland. doi:10.1007/978-3-031-24556-5. ISBN 978-3-031-24555-8. https://link.springer.com/10.1007/978-3-031-24556-5.
- ↑ "Global Epidemiology and Burden of Schizophrenia: Findings From the Global Burden of Disease Study 2016". Schizophrenia Bulletin 44 (6): 1195–1203. October 2018. doi:10.1093/schbul/sby058. PMID 29762765.
- ↑ "Schizophrenia (maintenance treatment)". American Family Physician 82 (4): 338–339. August 2010. PMID 20704164.
- ↑ "Recovery from schizophrenia and the recovery model". Current Opinion in Psychiatry 22 (4): 374–380. July 2009. doi:10.1097/YCO.0b013e32832c920b. PMID 19417668.
- ↑ "A systematic review of longitudinal outcome studies of first-episode psychosis". Psychological Medicine 36 (10): 1349–62. October 2006. doi:10.1017/S0033291706007951. PMID 16756689. https://pdfs.semanticscholar.org/8539/923c1b4f6bacb128d478b9ec7f6e95559210.pdf.
- ↑ "Schizophrenia: Basic and Clinical". Neurodegenerative Diseases. Advances in Neurobiology. 15. 2017. pp. 255–280. doi:10.1007/978-3-319-57193-5_9. ISBN 978-3-319-57191-1.
- ↑ "Schizophrenia outcome measures in the wider international community". The British Journal of Psychiatry. Supplement 50: s71–77. August 2007. doi:10.1192/bjp.191.50.s71. PMID 18019048.
- ↑ "Questioning an axiom: better prognosis for schizophrenia in the developing world?". Schizophrenia Bulletin 34 (2): 229–244. March 2008. doi:10.1093/schbul/sbm105. PMID 17905787.
- ↑ "Suicide in schizophrenia". Expert Review of Neurotherapeutics 10 (7): 1153–1164. July 2010. doi:10.1586/ern.10.82. PMID 20586695.
- ↑ "Interventions for smoking cessation and reduction in individuals with schizophrenia". The Cochrane Database of Systematic Reviews 2013 (2). 28 February 2013. doi:10.1002/14651858.CD007253.pub3. PMID 23450574.
- ↑ "Pharmacogenetics of clozapine treatment response and side-effects in schizophrenia: an update". Expert Opinion on Drug Metabolism & Toxicology 11 (11): 1709–1731. 2015. doi:10.1517/17425255.2015.1075003. PMID 26364648.
- ↑ "A meta-analysis of worldwide studies demonstrates an association between schizophrenia and tobacco smoking behaviors". Schizophrenia Research 76 (2–3): 135–157. July 2005. doi:10.1016/j.schres.2005.02.010. PMID 15949648.
- ↑ 246.0 246.1 "Smoke, smoke, smoke that cigarette". Perspectives in Psychiatric Care 42 (4): 256–261. November 2006. doi:10.1111/j.1744-6163.2006.00085.x. PMID 17107571.
- ↑ "Nicotine use in schizophrenia: the self medication hypotheses". Neuroscience and Biobehavioral Reviews 29 (6): 1021–1034. January 2005. doi:10.1016/j.neubiorev.2005.02.006. PMID 15964073.
- ↑ "Schizophrenia and risk of dementia: a meta-analysis study". Neuropsychiatr Dis Treat 14: 2047–2055. 2018. doi:10.2147/NDT.S172933. PMID 30147318.
- ↑ "Insight and theory of mind in schizophrenia.". Psychiatry Research 225 (1–2): 169–174. 30 January 2015. doi:10.1016/j.psychres.2014.11.010. PMID 25467703.
- ↑ "Relationship between insight and theory of mind in schizophrenia: A meta-analysis". Schizophrenia Research 190: 11–17. December 2017. doi:10.1016/j.schres.2017.03.029. PMID 28302393.
- ↑ "[Preventing violence in schizophrenia with cognitive remediation]". L'Encephale 44 (2): 158–167. April 2018. doi:10.1016/j.encep.2017.05.001. PMID 28641817.
- ↑ "[Homicide, schizophrenia and substance abuse: a complex interaction]". Revue d'Épidemiologie et de Santé Publique 61 (4): 339–350. August 2013. doi:10.1016/j.respe.2013.01.096. PMID 23816066.
- ↑ "Neuropsychology and emotion processing in violent individuals with antisocial personality disorder or schizophrenia: The same or different? A systematic review and meta-analysis". The Australian and New Zealand Journal of Psychiatry 51 (12): 1178–1197. December 2017. doi:10.1177/0004867417731525. PMID 28992741.
- ↑ "New WHO prevalence estimates of mental disorders in conflict settings: a systematic review and meta-analysis". Lancet 394 (10194): 240–248. July 2019. doi:10.1016/S0140-6736(19)30934-1. PMID 31200992.
- ↑ "Heterogeneity in incidence rates of schizophrenia and other psychotic syndromes: findings from the 3-center AeSOP study". Archives of General Psychiatry 63 (3): 250–258. March 2006. doi:10.1001/archpsyc.63.3.250. PMID 16520429.
- ↑ "Neighbourhood variation in the incidence of psychotic disorders in Southeast London". Social Psychiatry and Psychiatric Epidemiology 42 (6): 438–445. June 2007. doi:10.1007/s00127-007-0193-0. PMID 17473901.
- ↑ [needs update] "Global burden of schizophrenia in the year 2000". World Health Organization. 15 August 2006. https://www.who.int/healthinfo/statistics/bod_schizophrenia.pdf.
- ↑ "Historical origins of schizophrenia: two early madmen and their illness". Journal of the History of the Behavioral Sciences 39 (4): 349–363. 2003. doi:10.1002/jhbs.10152. PMID 14601041.
- ↑ 259.0 259.1 "Eugen Bleuler's concepts of psychopathology". History of Psychiatry 15 (59 Pt 3): 361–366. September 2004. doi:10.1177/0957154X04044603. PMID 15386868.
- ↑ "Schizophrenia | Definition of Schizophrenia by Lexico". Lexico Dictionaries | English. https://www.lexico.com/en/definition/schizophrenia.
- ↑ [page needed]
- ↑ "The Two Faces of First-Rank Symptoms". Psychopathology 52 (4): 221–231. 2019. doi:10.1159/000503152. PMID 31610542.
- ↑ "Innovations and changes in the ICD-11 classification of mental, behavioural and neurodevelopmental disorders". World Psychiatry 18 (1): 3–19. February 2019. doi:10.1002/wps.20611. PMID 30600616.
- ↑ "Updates to DSM-5 Criteria & Text". www.psychiatry.org. https://www.psychiatry.org/psychiatrists/practice/dsm/updates-to-dsm-5/updates-to-dsm-5-criteria-text.
- ↑ "Schizophrenia and Other Psychotic Disorders in Diagnostic and Statistical Manual of Mental Disorders (DSM)-5: Clinical Implications of Revisions from DSM-IV". Indian Journal of Psychological Medicine 36 (3): 223–225. July 2014. doi:10.4103/0253-7176.135365. PMID 25035542.
- ↑ 266.0 266.1 "How Schizophrenia Became a Black Disease: An Interview With Jonathan Metzl". Psychology Today. 5 May 2010. http://www.psychologytoday.com/blog/side-effects/201005/how-schizophrenia-became-black-disease-interview-jonathan-metzl.
- ↑ The Protest Psychosis. Beacon Press. 2010. ISBN 978-0-8070-8592-9.
- ↑ "DSM-III and the transformation of American psychiatry: a history". The American Journal of Psychiatry 150 (3): 399–410. March 1993. doi:10.1176/ajp.150.3.399. PMID 8434655.
- ↑ "A review of American psychiatry through its diagnoses: the history and development of the Diagnostic and Statistical Manual of Mental Disorders.". The Journal of Nervous and Mental Disease 200 (12): 1022–1030. December 2012. doi:10.1097/NMD.0b013e318275cf19. PMID 23197117.
- ↑ 270.0 270.1 "Insulin coma therapy in schizophrenia". Journal of the Royal Society of Medicine 93 (3): 147–149. March 2000. doi:10.1177/014107680009300313. PMID 10741319.
- ↑ "One Size Does Not Fit All: A Comprehensive Clinical Approach to Reducing Suicidal Ideation, Attempts, and Deaths.". International Journal of Environmental Research and Public Health 16 (19): 3606. 26 September 2019. doi:10.3390/ijerph16193606. PMID 31561488.
- ↑ "Electroconvulsive Therapy and Schizophrenia: A Systematic Review". Molecular Neuropsychiatry 5 (2): 75–83. April 2019. doi:10.1159/000497376. PMID 31192220.
- ↑ "Psychosurgery: past, present, and future". Brain Research. Brain Research Reviews 48 (3): 409–419. June 2005. doi:10.1016/j.brainresrev.2004.09.002. PMID 15914249.
- ↑ "Report of the Special Rapporteur on torture and other cruel, inhuman or degrading treatment or punishment". Office of the High Commissioner for Human Rights. 1 February 2013. https://www.ohchr.org/sites/default/files/Documents/HRBodies/HRCouncil/RegularSession/Session22/A.HRC.22.53_English.pdf.
- ↑ "Chlorpromazine: unlocking psychosis". BMJ 334 Suppl 1 (suppl): s7. January 2007. doi:10.1136/bmj.39034.609074.94. PMID 17204765.
- ↑ "Molecular targets of atypical antipsychotics: From mechanism of action to clinical differences.". Pharmacology & Therapeutics 192: 20–41. December 2018. doi:10.1016/j.pharmthera.2018.06.012. PMID 29953902.
- ↑ "Psychiatry in former socialist countries: implications for north korean psychiatry". Psychiatry Investigation 11 (4): 363–370. 2014. doi:10.4306/pi.2014.11.4.363. ISSN 1738-3684. PMID 25395966.
- ↑ Punishing the patient: how psychiatrists misunderstand and mistreat schizophrenia. Melbourne: Scribe Publications. 2001. ISBN 0-908011-52-0. OCLC 47177633.
- ↑ "Can Psychiatry be Misused Again?". Frontiers in Psychiatry 4: 101. September 2013. doi:10.3389/fpsyt.2013.00101. PMID 24058348.
- ↑ "IPPNW: Forum for Soviet anti-American propaganda?". CMAJ: Canadian Medical Association Journal 139 (8): 699–700. 15 October 1988. ISSN 0820-3946.
- ↑ "The economic burden of schizophrenia in the United States in 2002". The Journal of Clinical Psychiatry 66 (9): 1122–1129. September 2005. doi:10.4088/jcp.v66n0906. PMID 16187769.
- ↑ "The costs of schizophrenia". The Journal of Clinical Psychiatry 68 (Suppl 14): 4–7. 2007. PMID 18284271.
- ↑ "A systematic literature review of the clinical and health economic burden of schizophrenia in privately insured patients in the United States". Clinicoecon Outcomes Res 10: 309–320. 2018. doi:10.2147/CEOR.S156308. PMID 29922078.
- ↑ "Associations between renaming schizophrenia and stigma-related outcomes: A systematic review". Psychiatry and Clinical Neurosciences 71 (6): 347–362. June 2017. doi:10.1111/pcn.12510. PMID 28177184.
- ↑ "Renaming schizophrenia: a Japanese perspective". World Psychiatry 5 (1): 53–55. February 2006. PMID 16757998.
- ↑ "Korea in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition". Journal of Korean Medical Science 35 (2). January 2020. doi:10.3346/jkms.2020.35.e6. PMID 31920014.
- ↑ "Schizophrenia and violence: systematic review and meta-analysis". PLOS Medicine 6 (8). August 2009. doi:10.1371/journal.pmed.1000120. PMID 19668362.
- ↑ "Portrayals of schizophrenia by entertainment media: a content analysis of contemporary movies". Psychiatr Serv 63 (7): 655–9. July 2012. doi:10.1176/appi.ps.201100371. PMID 22555313.
- ↑ "Psychiatry's contribution to the public stereotype of schizophrenia: Historical considerations". J Eval Clin Pract 24 (5): 1093–1100. October 2018. doi:10.1111/jep.13011. PMID 30112785.
- ↑ "Newspaper depictions of mental and physical health.". BJPsych Bulletin 41 (6): 308–313. December 2017. doi:10.1192/pb.bp.116.054775. PMID 29234506.
- ↑ "Ways of understanding of religious delusions associated with a change of identity on the example of identification with Jesus Christ.". Psychiatria Polska 52 (1): 69–80. 28 February 2018. doi:10.12740/PP/64378. PMID 29704415.
- ↑ "Religion and psychosis: a common evolutionary trajectory?". Transcultural Psychiatry 48 (3): 318–335. July 2011. doi:10.1177/1363461511402723. PMID 21742955.
- ↑ "Transcranial magnetic stimulation (TMS) for schizophrenia.". The Cochrane Database of Systematic Reviews 2015 (8). 20 August 2015. doi:10.1002/14651858.CD006081.pub2. PMID 26289586.
- ↑ 294.0 294.1 "Auditory verbal hallucinations in schizophrenia: current perspectives in brain stimulation treatments.". Neuropsychiatric Disease and Treatment 15: 2105–2117. 2019. doi:10.2147/NDT.S168801. PMID 31413576.
- ↑ "Neuroimaging Biomarkers in Schizophrenia". Am J Psychiatry 178 (6): 509–521. January 2021. doi:10.1176/appi.ajp.2020.20030340. PMID 33397140.
- ↑ "Epigenomic Dysregulation in Schizophrenia: In Search of Disease Etiology and Biomarkers". Cells 9 (8): 1837. August 2020. doi:10.3390/cells9081837. PMID 32764320.
- ↑ "An Update on Promising Biomarkers in Schizophrenia". Focus (American Psychiatric Publishing) 16 (2): 153–163. April 2018. doi:10.1176/appi.focus.20170046. PMID 31975910.
- ↑ "Are circulating microRNAs peripheral biomarkers for Alzheimer's disease?". Biochim Biophys Acta 1862 (9): 1617–1627. September 2016. doi:10.1016/j.bbadis.2016.06.001. PMID 27264337.
- ↑ "Circulating microRNAs as potential biomarkers for psychiatric and neurodegenerative disorders". Prog Neurobiol 185. February 2020. doi:10.1016/j.pneurobio.2019.101732. PMID 31816349.
- ↑ Palaniyappan, Lena; Liddle, Peter F. (2013-04-24). "Diagnostic Discontinuity in Psychosis: A Combined Study of Cortical Gyrification and Functional Connectivity". Schizophrenia Bulletin 40 (3): 675–684. doi:10.1093/schbul/sbt050. ISSN 1745-1701. PMID 23615812. PMC 3984507. https://academic.oup.com/schizophreniabulletin/article-abstract/40/3/675/1903745?redirectedFrom=fulltext.
External links
- Schizophrenia: Evolution and Synthesis
- The American Psychiatric Association Practice Guideline for the Treatment of Patients With Schizophrenia, Third Edition
| Classification | |
|---|---|
| External resources |
 |
