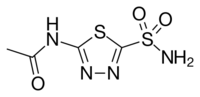
Chemistry:Acetazolamide
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Diamox, Diacarb, others |
| AHFS/Drugs.com | Monograph |
| Pregnancy category |
|
| Routes of administration | By mouth, intravenous |
| Drug class | Carbonic anhydrase inhibitor |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Protein binding | 70–90%[1] |
| Metabolism | None[1] |
| Elimination half-life | 2–4 hours[1] |
| Excretion | Urine (90%)[1] |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| PDB ligand | |
| Chemical and physical data | |
| Formula | C4H6N4O3S2 |
| Molar mass | 222.24 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 258 to 259 °C (496 to 498 °F) |
| |
| |
| (verify) | |
Acetazolamide, sold under the trade name Diamox among others, is a medication used to treat glaucoma, epilepsy, acute mountain sickness, periodic paralysis, idiopathic intracranial hypertension (raised brain pressure of unclear cause), heart failure and to alkalinize urine.[2][3] It may be used long term for the treatment of open angle glaucoma and short term for acute angle closure glaucoma until surgery can be carried out.[4] It is taken by mouth or injection into a vein.[2] Acetazolamide is a first generation carbonic anhydrase inhibitor and it decreases the ocular fluid and osmolality in the eye to decrease intraocular pressure.[5][6]
Common side effects include numbness, ringing in the ears, loss of appetite, vomiting, and sleepiness.[2] It is not recommended in those with significant kidney problems, liver problems, or who are allergic to sulfonamides.[2][4] Acetazolamide is in the diuretic and carbonic anhydrase inhibitor families of medication.[2] It works by decreasing the formation of hydrogen ions and bicarbonate from carbon dioxide and water.[2]
Acetazolamide came into medical use in 1952.[7] It is on the World Health Organization's List of Essential Medicines.[8] Acetazolamide is available as a generic medication.[2]
Medical uses
It is used in the treatment of glaucoma, drug-induced edema, heart failure-induced edema, epilepsy and in reducing intraocular pressure after surgery.[9][10] It has also been used in the treatment of altitude sickness,[11] Ménière's disease, increased intracranial pressure and neuromuscular disorders.[12] Acetazolamide is also used in the critical care setting to stimulate respiratory drive in patients with chronic obstructive pulmonary disease as an off-label indication.[13]
In epilepsy, the main use of acetazolamide is in menstrual-related epilepsy and as an add on to other treatments in refractory epilepsy.[9][14] Though various websites on the internet report that acetazolamide can be used to treat dural ectasia in individuals with Marfan syndrome, the only supporting evidence for this assertion exists from a small study of 14 patients which was not peer-reviewed or submitted for publication.[15][16] Several published cases of intracranial hypotension related to Marfan syndrome would warrant caution in using acetazolamide in these patients unless there is a clear indication, as it could lower intracranial pressure further.[17] A 2012 review and meta-analysis found that there was "limited supporting evidence" but that acetazolamide "may be considered" for the treatment of central (as opposed to obstructive) sleep apnea.[18]
It has also been used to prevent methotrexate-induced kidney damage by alkalinizing the urine, hence speeding up methotrexate excretion by increasing its solubility in urine.[12][19] There is some evidence to support its use to prevent hemiplegic migraine.[20]
Open-angle glaucoma
Acetazolamide is used in the treatment of open-angle glaucoma. The carbonic anhydrase inhibitor is able to decrease ocular fluid and osmolality of the fluid in the humor of the eye and decrease intraocular pressure in the eye. The medication comes in the form of an oral tablet used for this indication.
High altitude sickness
Acetazolamide is also used for the treatment of acute mountain sickness. In the prevention or treatment of mountain sickness, acetazolamide inhibits the ability of the kidneys to reabsorb bicarbonate, the conjugate base of carbonic acid. Increasing the amount of bicarbonate excreted in the urine leads to acidification of the blood.[12] Because the body senses CO2 concentration indirectly via blood pH (increase in CO2 causes a decrease in pH), acidifying the blood through decreased renal reabsorption of bicarbonate is sensed as an increase in CO2. This, in turn, causes the body to increase minute ventilation (the amount of air breathed per minute) in order to "breathe off" CO2, which in turn increases the amount of oxygen in the blood.[21][22] Acetazolamide is not an immediate cure for acute mountain sickness; rather, it speeds up (or, when taking before traveling, forces the body to early start) part of the acclimatization process which in turn helps to relieve symptoms.[23] Acetazolamide is still effective if started early in the course of mountain sickness. As prevention, it is started one day before travel to altitude and continued for the first two days at altitude.[24]
Pregnancy and lactation
Acetazolamide is pregnancy category B3 in Australia, which means that studies in rats, mice and rabbits in which acetazolamide was given intravenously or orally caused an increased risk of fetal malformations, including defects of the limbs.[10] Despite this, there is insufficient evidence from studies in humans to either support or discount this evidence.[10]
Limited data are available on the effects of nursing mothers taking acetazolamide. Therapeutic doses create low levels in breast milk and are not expected to cause problems in infants.[25]
Side effects
Common adverse effects of acetazolamide include the following: paraesthesia, fatigue, drowsiness, depression, decreased libido, bitter or metallic taste, nausea, vomiting, abdominal cramps, diarrhea, black stool, polyuria, kidney stones, metabolic acidosis and electrolyte changes (hypokalemia, hyponatremia).[9] Whereas less common adverse effects include Stevens–Johnson syndrome, anaphylaxis and blood dyscrasias.[9]
Contraindications
Contraindications include:[10]
- Hyperchloremic acidosis
- Hypokalemia (low blood potassium)
- Hyponatremia (low blood sodium)
- Adrenal insufficiency
- Impaired kidney function
- Hypersensitivity to acetazolamide or other sulphonamides.
- Marked liver disease or impairment of liver function, including cirrhosis because of the risk of development of hepatic encephalopathy. Acetazolamide decreases ammonia clearance.
Interactions
It is possible that it might interact with:[10]
- Amphetamines, because it increases the pH of the renal tubular urine, hence reducing the clearance of amphetamines.
- Other carbonic anhydrase inhibitors—potential for additive inhibitory effects on carbonic anhydrase and hence potential for toxicity.
- Ciclosporin, may increase plasma levels of ciclosporin.
- Antifolates such as trimethoprim, methotrexate, pemetrexed and raltitrexed.
- Hypoglycemics, acetazolamide can both increase or decrease blood glucose levels.
- Lithium, increases excretion, hence reducing therapeutic effect.
- Methenamine compounds, reduces the urinary excretion of methenamines.
- Phenytoin, reduces phenytoin excretion, hence increasing the potential for toxicity.
- Primidone, reduces plasma levels of primidone. Hence reducing anticonvulsant effect.
- Quinidine, reduces urinary excretion of quinidine, hence increasing the potential for toxicity.
- Salicylates, potential for severe toxicity.
- Sodium bicarbonate, potential for kidney stone formation.
- Anticoagulants, cardiac glycosides, may have their effects potentiated by acetazolamide.
Mechanism of action

Acetazolamide is a carbonic anhydrase inhibitor, hence causing the accumulation of carbonic acid.[12] Carbonic anhydrase is an enzyme found in red blood cells and many other tissues that catalyses the following reaction:[26]
- H2CO3 ⇌ H2O + CO2
hence lowering blood pH, by means of the following reaction that carbonic acid undergoes:[27]
- H2CO3 ⇌ HCO3− + H+
The mechanism of diuresis involves the proximal tubule of the kidney. The enzyme carbonic anhydrase is found here, allowing the reabsorption of bicarbonate, sodium, and chloride. By inhibiting this enzyme, these ions are excreted, along with excess water, lowering blood pressure, intracranial pressure, and intraocular pressure. A general side effect of carbonic anhydrase inhibitors is loss of potassium due to this function. By excreting bicarbonate, the blood becomes acidic, causing compensatory hyperventilation with deep respiration (Kussmaul breathing), increasing levels of oxygen and decreasing levels of carbon dioxide in the blood.[22]
In the eye this results in a reduction in aqueous humour.[10]
Bicarbonate (HCO3−) has a pKa of 10.3 with carbonate (CO32−), far further from physiologic pH (7.35–7.45), and so it is more likely to accept a proton than to donate one, but it is also far less likely for it to do either, thus bicarbonate will be the major species at physiological pH.
Under normal conditions in the proximal convoluted tubule of the kidney, most of the carbonic acid (H2CO3) produced intracellularly by the action of carbonic anhydrase quickly dissociates in the cell to bicarbonate (HCO3−) and an H+ ion (a proton), as previously mentioned. The bicarbonate (HCO3−) exits at the basal portion of the cell via sodium (Na+) symport and chloride (Cl−) antiport and re-enters circulation, where it may accept a proton if blood pH decreases, thus acting as a weak, basic buffer. The remaining H+ left over from the intracellular production of carbonic acid (H2CO3) exits the apical (urinary lumen) portion of the cell by Na+ antiport, acidifying the urine. There, it may join with another bicarbonate (HCO3−) that dissociated from its H+ in the lumen of the urinary space only after exiting the proximal convoluted kidney cells/glomerulus as carbonic acid (H2CO3) because bicarbonate (HCO3−) itself can not diffuse across the cell membrane in its polar state. This will replenish carbonic acid (H2CO3) so that it then may be reabsorbed into the cell as itself or CO2 and H2O (produced via a luminal carbonic anhydrase). As a result of this whole process, there is a greater net balance of H+ in the urinary lumen than bicarbonate (HCO3−), and so this space is more acidic than physiologic pH. Thus, there is an increased likelihood that any bicarbonate (HCO3−) that was left over in the lumen diffuses back into the cell as carbonic acid, CO2, or H2O.
In short, under normal conditions, the net effect of carbonic anhydrase in the urinary lumen and cells of the proximal convoluted tubule is to acidify the urine and transport bicarbonate (HCO3−) into the body. Another effect is excretion of Cl− as it is needed to maintain electroneutrality in the lumen, as well as the reabsorption of Na+ into the body.
Thus, by disrupting this process with acetazolamide, urinary Na+ and bicarbonate (HCO3−) are increased, and urinary H+ and Cl− are decreased. Inversely, serum Na+ and bicarbonate (HCO3−) are decreased, and serum H+ and Cl− are increased. H2O generally follows sodium, and so this is how the clinical diuretic effect is achieved, which reduces blood volume and thus preload on the heart to improve contractility and reduce blood pressure, or achieve other desired clinical effects of reduced blood volume such as reducing edema or intracranial pressure.[28]
History
An early description of this compound (as 2-acetylamino-1,3,4-thiadiazole-5-sulfonamide) and its synthesis has been patented.[29]
Research
Smaller clinical trials have also shown promising results in the treatment of normal pressure hydrocephalus (NPH).[30][31][32][33][34]
References
- ↑ 1.0 1.1 1.2 1.3 "Diamox Sequels (acetazolamide) dosing, indications, interactions, adverse effects, and more". Medscape Reference. WebMD. http://reference.medscape.com/drug/diamox-acetazolamide-342809#showall.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 "Acetazolamide". The American Society of Health-System Pharmacists. https://www.drugs.com/monograph/acetazolamide.html.
- ↑ "The Idiopathic Intracranial Hypertension Treatment Trial: A Review of the Outcomes". Headache 57 (8): 1303–1310. September 2017. doi:10.1111/head.13144. PMID 28758206.
- ↑ 4.0 4.1 WHO Model Formulary 2008. World Health Organization. 2009. p. 439. ISBN 9789241547659.
- ↑ "Glaucoma and the Applications of Carbonic Anhydrase Inhibitors". Carbonic Anhydrase: Mechanism, Regulation, Links to Disease, and Industrial Applications. Subcellular Biochemistry. 75. Springer. 2014. pp. 349–359. doi:10.1007/978-94-007-7359-2_17. ISBN 978-94-007-7358-5.
- ↑ "Acetazolamide: mechanism of action" (in en-US). https://www.openanesthesia.org/acetazolamide_mechanism_of_action/.
- ↑ (in en) Drug Discovery: A History. John Wiley & Sons. 2005. p. 390. ISBN 9780471899792. https://books.google.com/books?id=Cb6BOkj9fK4C&pg=PA390.
- ↑ World Health Organization model list of essential medicines: 21st list 2019. Geneva: World Health Organization. 2019. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- ↑ 9.0 9.1 9.2 9.3 Australian Medicines Handbook (2013 ed.). Adelaide: The Australian Medicines Handbook Unit Trust. 2013. ISBN 978-0-9805790-9-3.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 "Product Information Diamox Acetazolamide Tablets" (PDF). TGA eBusiness Services. Aspen Pharma Pty Ltd. 25 February 2005. https://www.ebs.tga.gov.au/ebs/picmi/picmirepository.nsf/pdf?OpenAgent&id=CP-2009-PI-00910-3.
- ↑ "Identifying the lowest effective dose of acetazolamide for the prophylaxis of acute mountain sickness: systematic review and meta-analysis". BMJ 345: e6779. October 2012. doi:10.1136/bmj.e6779. PMID 23081689.
- ↑ 12.0 12.1 12.2 12.3 "Acetazolamide". Martindale: The Complete Drug Reference. Pharmaceutical Press. 7 January 2014. http://www.medicinescomplete.com/mc/martindale/current/ms-2301-x.htm.
- ↑ "Acetazolamide: a second wind for a respiratory stimulant in the intensive care unit?". Critical Care 16 (4): 318. August 2012. doi:10.1186/cc11323. PMID 22866939.
- ↑ "Acetazolamide in the treatment of seizures". The Annals of Pharmacotherapy 30 (5): 514–519. May 1996. doi:10.1177/106002809603000515. PMID 8740334.
- ↑ "Dural ectasia". SpineUniverse.com. July 2005. http://www.spineuniverse.com/displayarticle.php/article922.html.
- ↑ "Acetazolamide". StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. 2020. https://www.ncbi.nlm.nih.gov/books/NBK532282/.
- ↑ "Intracranial hypotension in a girl with Marfan syndrome: case report and review of the literature". Child's Nervous System 24 (4): 509–513. April 2008. doi:10.1007/s00381-007-0506-3. PMID 17906865.
- ↑ "The treatment of central sleep apnea syndromes in adults: practice parameters with an evidence-based literature review and meta-analyses". Sleep 35 (1): 17–40. January 2012. doi:10.5665/sleep.1580. PMID 22215916.
- ↑ "Acetazolamide for alkalinisation of urine in patients receiving high-dose methotrexate". Cancer Chemotherapy and Pharmacology 28 (2): 150–151. 1991. doi:10.1007/BF00689708. PMID 2060085.
- ↑ "Sporadic and familial hemiplegic migraine: pathophysiological mechanisms, clinical characteristics, diagnosis, and management". The Lancet. Neurology 10 (5): 457–470. May 2011. doi:10.1016/S1474-4422(11)70048-5. PMID 21458376.
- ↑ "Altitude.org". 2004. http://www.altitude.org.
- ↑ 22.0 22.1 "Mechanisms of action of acetazolamide in the prophylaxis and treatment of acute mountain sickness". Journal of Applied Physiology (Bethesda, Md.) 102 (4): 1313–1322. April 2007. doi:10.1152/japplphysiol.01572.2005. PMID 17023566. https://www.life.illinois.edu/ib/426/handouts/Diamox%20mechanism_review_2007.pdf. Retrieved 8 December 2014.
- ↑ "Altitude Acclimatization Guide". US Army Research Inst. Of Environmental Medicine Thermal and Mountain Medicine Division Technical Report (USARIEM–TN–04–05). 2004. http://archive.rubicon-foundation.org/7616. Retrieved 5 March 2009.
- ↑ World Health Organization. "International Travel and Health 2012". http://who.int/ith/ITH_EN_2012_WEB_1.2.pdf.
- ↑ "LactMed: Acetazolamide". National Institutes of Health. http://toxnet.nlm.nih.gov/cgi-bin/sis/search2/r?dbs+lactmed:@term+@DOCNO+489.
- ↑ "January 2004: Carbonic Anhydrase". RCSB PDB Protein Data Bank. January 2004. http://www.rcsb.org/pdb/education_discussion/molecule_of_the_month/download/CarbonicAnhydrase.pdf.
- ↑ 27.0 27.1 "Carbonic Anhydrase 2". UC Davis Chemwiki. University of California. http://chemwiki.ucdavis.edu/@api/deki/pages/2479/pdf?stylesheet=default&deep=false&showtoc=false.
- ↑ "The kidney and acid-base regulation". Advances in Physiology Education 33 (4): 275–281. December 2009. doi:10.1152/advan.00054.2009. PMID 19948674. http://d3qpq7e7yxjovl.cloudfront.net/content/ajpadvan/33/4/275.
- ↑ Clapp Jr JW, Roblin RO, "Heterocyclic sulfonamides and metyhods of preparation thereof", US patent 2554816, published 1951-05-29, assigned to American Cyanamid Company
- ↑ "Low-dose acetazolamide reverses periventricular white matter hyperintensities in iNPH". Neurology 82 (15): 1347–1351. April 2014. doi:10.1212/WNL.0000000000000313. PMID 24634454.
- ↑ "MRI assessment of the effects of acetazolamide and external lumbar drainage in idiopathic normal pressure hydrocephalus". Fluids and Barriers of the CNS 12 (1): 9. April 2015. doi:10.1186/s12987-015-0004-z. PMID 25928394.
- ↑ "Acetazolamide in the treatment of Normal Pressure Hydrocephalus". Neurology. 18 May 2022. https://n.neurology.org/content/acetazolamide-treatment-normal-pressure-hydrocephalus.
- ↑ "[Acetazolamide: an alternative to shunting in normal pressure hydrocephalus? Preliminary results"]. Revue Neurologique 146 (6–7): 437–439. 21 May 1990. PMID 2399408. https://pubmed.ncbi.nlm.nih.gov/2399408/.
- ↑ Clinical trial number NCT03779594 for "Acetazolamide for Treating NPH in Shunt-candidates Patients: an Open Label Feasibility Trial" at ClinicalTrials.gov
 |
