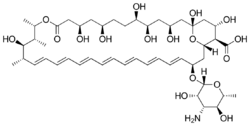
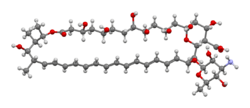
Chemistry:Amphotericin B
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Fungizone, Mysteclin-F, AmBisome and other |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682643 |
| License data | |
| Pregnancy category |
|
| Routes of administration | Intravenous infusion |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | 100% (IV) |
| Metabolism | kidney |
| Elimination half-life |
|
| Excretion |
|
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| NIAID ChemDB | |
| Chemical and physical data | |
| Formula | C47H73NO17 |
| Molar mass | 924.091 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 170 °C (338 °F) |
| |
| |
| (verify) | |
Amphotericin B is an antifungal medication used for serious fungal infections and leishmaniasis.[3] The fungal infections it is used to treat include mucormycosis, aspergillosis, blastomycosis, candidiasis, coccidioidomycosis, and cryptococcosis.[4] For certain infections it is given with flucytosine.[5] It is typically given intravenously.[4]
Common side effects include a reaction with fever, chills, and headaches soon after the medication is given, as well as kidney problems.[4] Allergic symptoms including anaphylaxis may occur.[4] Other serious side effects include low blood potassium and myocarditis (inflammation of the heart).[3] It appears to be relatively safe in pregnancy.[4] There is a lipid formulation that has a lower risk of side effects.[4] It is in the polyene class of medications and works in part by interfering with the cell membrane of the fungus.[3][4]
Amphotericin B was isolated from Streptomyces nodosus in 1955 at the Squibb Institute for Medical Research from cultures isolated from the streptomycete obtained from the river bed of Orinoco in that region of Venezuela[6] and came into medical use in 1958.[7][8] It is on the World Health Organization's List of Essential Medicines.[9] It is available as a generic medication.[4][10]
Medical uses
Antifungal
One of the main uses of amphotericin B is treating a wide range of systemic fungal infections. Due to its extensive side effects, it is often reserved for severe infections in critically ill or immunocompromised patients. It is considered first line therapy for invasive mucormycosis infections, cryptococcal meningitis, and certain aspergillus and candidal infections.[11][12] It has been a highly effective drug for over fifty years in large part because it has a low incidence of drug resistance in the pathogens it treats. This is because amphotericin B resistance requires sacrifices on the part of the pathogen that make it susceptible to the host environment, and too weak to cause infection.[13]
Antiprotozoal
Amphotericin B is used for life-threatening protozoan infections such as visceral leishmaniasis[14] and primary amoebic meningoencephalitis.[15]
Spectrum of susceptibility
The following table shows the amphotericin B susceptibility for several medically important fungi.
| Species | MIC[clarification needed] breakpoint (mg/L) |
|---|---|
| Aspergillus fumigatus | 1[16] |
| Aspergillus terreus | Resistant[16][17] |
| Candida albicans | 1[16] |
| Candida glabrata | 1[16] |
| Candida krusei | 1[16] |
| Candida lusitaniae | Intrinsically resistant[17] |
| Cryptococcus neoformans | 2[18] |
| Fusarium oxysporum | 2[18] |
Available formulations
Intravenous
Amphotericin B alone is insoluble in normal saline at a pH of 7. Therefore, several formulations have been devised to improve its intravenous bioavailability.[19] Lipid-based formulations of amphotericin B are no more effective than conventional formulations, although some evidence suggests lipid-based formulations may be better tolerated and have fewer adverse effects.[20]
Deoxycholate
The original formulation uses sodium deoxycholate to improve solubility.[17] Amphotericin B deoxycholate (ABD) is administered intravenously.[21] As the original formulation of amphotericin, it is often referred to as "conventional" amphotericin.[22]
Liposomal
To improve the tolerability of amphotericin and reduce toxicity, researchers developed several lipid formulations.[17] Liposomal formulations have been found to have less renal toxicity than deoxycholate,[23][24] and fewer infusion-related reactions.[17] They are more expensive than amphotericin B deoxycholate.[25]
AmBisome (liposomal amphotericin B; LAMB) is a liposomal formulation of amphotericin B for injection and consists of a mixture of phosphatidylcholine, cholesterol and distearoyl phosphatidylglycerol that in aqueous media spontaneously arrange into unilamellar vesicles that contain amphotericin B.[17][26] It was developed by NeXstar Pharmaceuticals (acquired by Gilead Sciences in 1999). It was approved by the United States Food and Drug Administration (FDA) in 1997.[27] It is marketed by Gilead in Europe and licensed to Astellas Pharma (formerly Fujisawa Pharmaceuticals) for marketing in the US, and Sumitomo Pharmaceuticals in Japan.[28]
Lipid complex formulations
Several lipid complex preparations are also available. Abelcet was approved by the FDA in 1995.[29] It consists of amphotericin B and two lipids in a 1:1 ratio that form large ribbon-like structures.[17] Amphotec is a complex of amphotericin and sodium cholesteryl sulfate in a 1:1 ratio. Two molecules of each form a tetramer that aggregates into spiral arms on a disk-like complex.[26] It was approved by the FDA in 1996.[29]
By mouth
An oral preparation exists but is not widely available.[30] The amphipathic nature of amphotericin along with its low solubility and permeability has posed major hurdles for oral administration given its low bioavailability. In the past it had been used for fungal infections of the surface of the GI tract such as thrush, but has been replaced by other antifungals such as nystatin and fluconazole.[31]
However, recently novel nanoparticulate drug delivery systems such as AmbiOnp,[32] nanosuspensions, lipid-based drug delivery systems including cochleates, self-emulsifying drug delivery systems,[33] solid lipid nanoparticles[32] and polymeric nanoparticles[34]—such as amphotericin B in pegylated polylactide coglycolide copolymer nanoparticles[35]—have demonstrated potential for oral formulation of amphotericin B.[36] The oral lipid nanocrystal amphotericin by Matinas Biopharma is furthest along, having completed a successful phase 2 clinical trial in cryptococcal meningitis.[37]
Side effects
Amphotericin B is well known for its severe and potentially lethal side effects, earning it the nickname "amphoterrible".[38][39] Very often, it causes a serious reaction soon after infusion (within 1 to 3 hours), consisting of high fever, shaking chills, hypotension, anorexia, nausea, vomiting, headache, dyspnea and tachypnea, drowsiness, and generalized weakness. The violent chills and fevers have caused the drug to be nicknamed "shake and bake".[40][41] The precise etiology of the reaction is unclear, although it may involve increased prostaglandin synthesis and the release of cytokines from macrophages.[42][43] Deoxycholate formulations (ABD) may also stimulate the release of histamine from mast cells and basophils.[44] Reactions sometimes subside with later applications of the drug. This nearly universal febrile response necessitates a critical (and diagnostically difficult) professional determination as to whether the onset of high fever is a novel symptom of a fast-progressing disease or merely the effect of the drug. To decrease the likelihood and severity of the symptoms, initial doses should be low and increased slowly. Paracetamol, pethidine, diphenhydramine, and hydrocortisone have all been used to treat or prevent the syndrome, but the prophylactic use of these drugs is often limited by the patient's condition.[45]
Intravenously administered amphotericin B in therapeutic doses has also been associated with multiple organ damage. Kidney damage, including Type I (distal) renal tubular acidosis, is a frequently reported side effect, and can be severe and/or irreversible.[46] Less kidney toxicity has been reported with liposomal formulations (such as AmBisome) and it has become preferred in patients with preexisting renal injury.[47][48] The integrity of the liposome is disrupted when it binds to the fungal cell wall, but is not affected by the mammalian cell membrane,[49] so the association with liposomes decreases the exposure of the kidneys to amphotericin B, which explains its less nephrotoxic effects.[50]
In addition, electrolyte imbalances such as hypokalemia and hypomagnesemia are also common.[51] In the liver, increased liver enzymes and hepatotoxicity (up to and including fulminant liver failure) are common. In the circulatory system, several forms of anemia and other blood dyscrasias (leukopenia, thrombopenia), serious cardiac arrhythmias (including ventricular fibrillation), and even frank cardiac failure have been reported. Skin reactions are also possible, with rash & itching occurring in about 17% of patients, in rare cases it can cause a serious skin reaction known as Drug rash with eosinophilia and systemic symptoms (DRESS).[52][53]
In very rare instances, amphotericin B has also been shown to cause reversible ototoxicity causing tinnitus, vertigo, and temporary hearing loss. While there have been only a few reported cases, the hearing loss was temporary in all of them, with hearing showing improvement two weeks after discontinuing the drug.[54][55]
The analogue AM-2-19 has been engineered to be less toxic to the kidneys.[56]
Interactions
Drug-drug interactions may occur when amphotericin B is coadministered with the following agents:[57]
- Flucytosine: The toxicity of flucytosine is increased and allows for a lower dose of amphotericin B. Amphotericin B may also facilitate entry of flucytosine into the fungal cell by interfering with the permeability of the fungal cell membrane.
- Diuretics or cisplatin: Increased renal toxicity and increased risk of hypokalemia
- Corticosteroids: Increased risk of hypokalemia
- Imidazole antifungals: Amphotericin B may antagonize the activity of ketoconazole and miconazole. The clinical significance of this interaction is unknown.
- Neuromuscular-blocking agents: Amphotericin B–induced hypokalemia may potentiate the effects of certain paralytic agents.
- Foscarnet, ganciclovir, tenofovir, adefovir: The risk of hematological and kidney side effects of amphotericin B is increased
- Zidovudine: Increased the risk of kidney and hematological toxicity.
- Other nephrotoxic drugs (such as aminoglycosides): Increased risk of serious renal damage
- Cytostatic drugs: Increased risk of kidney damage, low blood pressure, and airway spasms
- Transfusion of leukocytes: There is a risk that pulmonary (lung) damage may occur. Space the intervals between the application of amphotericin B and the transfusion, and monitor pulmonary function
Mechanism of action
Amphotericin B binds with ergosterol, a component of fungal cell membranes, forming pores that cause rapid leakage of monovalent ions (K+, Na+, H+ and Cl−) and subsequent fungal cell death. This is amphotericin B's primary effect as an antifungal agent.[58][59] It has been found that the amphotericin B/ergosterol bimolecular complex that maintains these pores is stabilized by Van der Waals interactions.[60] Researchers have found evidence that amphotericin B also causes oxidative stress within the fungal cell,[50] but it remains unclear to what extent this oxidative damage contributes to the drug's effectiveness.[58] The addition of free radical scavengers or antioxidants can lead to amphotericin resistance in some species, such as Scedosporium prolificans,[61] without affecting the cell wall.[62][63]
Two amphotericins, amphotericin A and amphotericin B, are known, but only B is used clinically, because it is significantly more active in vivo. Amphotericin A is almost identical to amphotericin B (having a C=C double bond between the 27th and 28th carbons), but has little antifungal activity.[19]
Mechanism of toxicity
Mammalian and fungal membranes contain sterols, a primary membrane target for amphotericin B. Because mammalian and fungal membranes are similar in structure and composition, this is one mechanism by which amphotericin B causes cellular toxicity. Amphotericin B molecules can form pores in the host membrane as well as the fungal membrane. This impairment in membrane barrier function can have lethal effects.[50][64][65] Ergosterol, the fungal sterol, is more sensitive to amphotericin B than cholesterol, the common mammalian sterol. Reactivity with the membrane is also sterol concentration dependent.[66] Bacteria are not affected as their cell membranes do not usually contain sterols.[67][68]
Amphotericin B administration is limited by infusion-related toxicity. This is thought to result from innate immune production of proinflammatory cytokines.[64][68]
Biosynthesis
The natural route to synthesis includes polyketide synthase (PKS) components.[69] The carbon chains of amphotericin B are assembled from sixteen 'C2' acetate and three 'C3' propionate units by polyketide syntheses.[70] Polyketide biosynthesis begins with the decarboxylative condensation of a dicarboxylic acid extender unit with a starter acyl unit to form a β-ketoacyl intermediate. A series of Claisen reactions constructs the growing chain. The extender units are loaded onto the current ACP domain by acetyl transferase (AT) within each module. The ACP-bound elongation group reacts in a Claisen condensation with the KS-bound polyketide chain. Ketoreductase (KR), dehydratase (DH), and enoyl reductase (ER) enzymes may also be present to form alcohol, double bonds, or single bonds.[71] After cyclisation, the macrolactone core undergoes further modification by hydroxylation, methylation and glycosylation. The order of these three post-cyclization processes is unknown.[71]
History
It was originally extracted from Streptomyces nodosus, a filamentous bacterium, in 1955, at the Squibb Institute for Medical Research from cultures of an undescribed streptomycete isolated from the soil collected in the Orinoco River region of Venezuela.[19][72] Two antifungal substances were isolated from the soil culture, amphotericin A and amphotericin B, but B had better antifungal activity. For decades, it remained the only effective therapy for invasive fungal disease until the development of the azole antifungals in the early 1980s.[21]
Its complete stereo structure was determined in 1970 by an X-ray structure of the N-iodoacetyl derivative.[70] The first synthesis of the compound's naturally occurring enantiomeric form was achieved in 1987 by K. C. Nicolaou.[73]
Amphotericin B was used to treat a patient with disseminated coccidioidomycosis who was admitted to the U.S. Public Health Service Hospital, Seattle, Washington, on January 16, 1957. "The course was rapidly downhill with a grim prognosis as manifested by positive blood cultures, rising complement fixation titers, and failure of the skin to react to intradermal coccidioidin. Amphotericin B was started eight weeks following the onset of his illness. Following this, there was a remarkable improvement both objectively and subjectively. A fourteen-month follow-up after drug discontinuation revealed stabilization of all laboratory studies except for a re-elevation of the complement fixation titer from 1 to 16 to 1 to 32. The patient was completely asymptomatic except for the sputum production containing a few spherules. The clinical effect of this drug in this patient has been most encouraging and agrees with results obtained by others. The lasting effect of the drug seems suggested by the patient's complete well-being after fourteen months of cessation of treatment. It is reasonable to assume that this drug will play a major part in the specific treatment of this disease." [74]
Formulations
It is a subgroup of the macrolide antibiotics and exhibits similar structural elements.[75] Currently, the drug is available in many forms. Either "conventionally" complexed with sodium deoxycholate (ABD), as a cholesteryl sulfate complex (ABCD), as a lipid complex (ABLC), and as a liposomal formulation (LAMB). The latter formulations have been developed to improve tolerability and decrease toxicity, but may show considerably different pharmacokinetic characteristics compared to conventional amphotericin B.[17]
Names
Amphotericin's name originates from the chemical's amphoteric properties.[76]
It is commercially known as Fungilin, Fungizone, Abelcet, AmBisome, Fungisome, Amphocil, Amphotec, and Halizon.[77]
References
- ↑ "Updates to the Prescribing Medicines in Pregnancy database". 12 May 2022. https://www.tga.gov.au/resources/resource/guidance/updates-prescribing-medicines-pregnancy-database.
- ↑ "Ambisome- amphotericin b injection, powder, lyophilized, for solution". https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=f7be6506-4d20-401e-a0ff-02ad7c33158a.
- ↑ 3.0 3.1 3.2 Control of the leishmaniasis: report of a meeting of the WHO Expert Committee on the Control of Leishmaniases. Geneva: World Health Organization. March 2010. pp. 55, 88, 186. ISBN 978-92-4-120949-6.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 "Amphotericin B". The American Society of Health-System Pharmacists. https://www.drugs.com/monograph/amphotericin-b.html.
- ↑ WHO Model Formulary 2008. World Health Organization. 2009. p. 145. ISBN 978-92-4-154765-9.
- ↑ (in es) Farmacología y su proyección a la clínica 13a ed.. Oteo.. 1976. p. 966. ISBN 84-85152-05-0.
- ↑ (in en) Trends and Changes in Drug Research and Development. Springer Science & Business Media. 2012. p. 109. ISBN 978-94-009-2659-2. https://books.google.com/books?id=FB_2CAAAQBAJ&pg=PA109.
- ↑ (in en) Analogue-based Drug Discovery. John Wiley & Sons. 2006. p. 477. ISBN 978-3-527-60749-5. https://books.google.com/books?id=FjKfqkaKkAAC&pg=PA477.
- ↑ World Health Organization model list of essential medicines: 21st list 2019. Geneva: World Health Organization. 2019. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- ↑ "Competitive Generic Therapy Approvals". 29 June 2023. https://www.fda.gov/drugs/generic-drugs/competitive-generic-therapy-approvals.
- ↑ Drugs Active against Fungi, Pneumocystis, and Microsporidia. Elsevier Health Sciences. 28 August 2014. pp. 479–494.e4. ISBN 978-1-4557-4801-3.
- ↑ "Liposomal amphotericin B: a review of its use as empirical therapy in febrile neutropenia and in the treatment of invasive fungal infections". Drugs 69 (3): 361–392. 2012-09-17. doi:10.2165/00003495-200969030-00010. PMID 19275278.
- ↑ "Understanding the evolution of drug resistance points to novel strategy for developing better antimicrobials". 2013-10-29. http://wi.mit.edu/news/archive/2013/understanding-evolution-drug-resistance-points-novel-strategy-developing-better.
- ↑ "Treatment options for visceral leishmaniasis". Expert Review of Anti-Infective Therapy 4 (2): 187–197. April 2006. doi:10.1586/14787210.4.2.187. PMID 16597201.
- ↑ "Naegleria fowleri: pathogenesis, diagnosis, and treatment options". Antimicrobial Agents and Chemotherapy 59 (11): 6677–6681. November 2015. doi:10.1128/AAC.01293-15. PMID 26259797.
- ↑ 16.0 16.1 16.2 16.3 16.4 European Committee on Antimicrobial Susceptibility Testing (2015-11-16). "Antifungal Agents, Breakpoint tables for interpretation of MICs". http://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/AFST/Clinical_breakpoints/Antifungal_breakpoints_v_8.0_November_2015.pdf.
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 17.7 "Amphotericin B formulations: a comparative review of efficacy and toxicity". Drugs 73 (9): 919–934. June 2013. doi:10.1007/s40265-013-0069-4. PMID 23729001.
- ↑ 18.0 18.1 "Index | The Antimicrobial Index Knowledgebase - TOKU-E". http://antibiotics.toku-e.com/.
- ↑ 19.0 19.1 19.2 "The discovery and development of amphotericin B". Diseases of the Chest 54 (Supplement_1): 296–298. October 1968. doi:10.1378/chest.54.Supplement_1.296. PMID 4877964.
- ↑ Steimbach, Laiza M., Fernanda S. Tonin, Suzane Virtuoso, Helena HL Borba, Andréia CC Sanches, Astrid Wiens, Fernando Fernandez-Llimós, and Roberto Pontarolo. "Efficacy and safety of amphotericin B lipid-based formulations—A systematic review and meta-analysis." Mycoses 60, no. 3 (2017): 146-154.
- ↑ 21.0 21.1 "History of the development of azole derivatives". Clinical Microbiology and Infection 10 (Suppl 1): 1–10. March 2004. doi:10.1111/j.1470-9465.2004.00841.x. PMID 14748798.
- ↑ "Comparison of fungizone, Amphotec, AmBisome, and Abelcet for treatment of systemic murine cryptococcosis". Antimicrobial Agents and Chemotherapy 42 (4): 899–902. April 1998. doi:10.1128/AAC.42.4.899. PMID 9559804.
- ↑ "Amphotericin B deoxycholate versus liposomal amphotericin B: effects on kidney function". The Cochrane Database of Systematic Reviews 2015 (11). November 2015. doi:10.1002/14651858.cd010481.pub2. PMID 26595825.
- ↑ "Does lipid emulsion reduce amphotericin B nephrotoxicity? A systematic review and meta-analysis". Clinical Infectious Diseases 54 (12): 1774–1777. June 2012. doi:10.1093/cid/cis290. PMID 22491505.
- ↑ "Editorial response: choosing amphotericin B formulations-between a rock and a hard place". Clinical Infectious Diseases 31 (5): 1164–1165. November 2000. doi:10.1086/317443. PMID 11073746.
- ↑ 26.0 26.1 "Lipid-based amphotericin B for the treatment of fungal infections". Pharmacotherapy 19 (3): 306–323. March 1999. doi:10.1592/phco.19.4.306.30934. PMID 10221369.
- ↑ "Drug Approval Package". https://www.accessdata.fda.gov/drugsatfda_docs/nda/97/050740_ambisome_toc.cfm.
- ↑ "Acquisition of an additional indication of AmBisome, a therapeutic agent for systemic fungal infection | Sumitomo Pharma" (in en). https://www.sumitomo-pharma.com/news/20090619.html.
- ↑ 29.0 29.1 "Drugs@FDA: FDA Approved Drug Products". http://www.accessdata.fda.gov/scripts/cder/drugsatfda/index.cfm?fuseaction=Search.DrugDetails.
- ↑ "Highly effective oral amphotericin B formulation against murine visceral leishmaniasis". The Journal of Infectious Diseases 200 (3): 357–360. August 2009. doi:10.1086/600105. PMID 19545212.
- ↑ "Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Diseases Society of America". Clinical Infectious Diseases 48 (5): 503–535. March 2009. doi:10.1086/596757. PMID 19191635.
- ↑ 32.0 32.1 "AmbiOnp: solid lipid nanoparticles of amphotericin B for oral administration". Journal of Biomedical Nanotechnology 7 (5): 632–639. October 2011. doi:10.1166/jbn.2011.1332. PMID 22195480.
- ↑ "Development and characterization of oral lipid-based amphotericin B formulations with enhanced drug solubility, stability and antifungal activity in rats infected with Aspergillus fumigatus or Candida albicans". International Journal of Pharmaceutics 372 (1–2): 76–84. May 2009. doi:10.1016/j.ijpharm.2009.01.003. PMID 19236839.
- ↑ "Biodegradable nanoparticles improve oral bioavailability of amphotericin B and show reduced nephrotoxicity compared to intravenous Fungizone". Pharmaceutical Research 26 (6): 1324–1331. June 2009. doi:10.1007/s11095-009-9841-2. PMID 19214716.
- ↑ "Stealth Amphotericin B nanoparticles for oral drug delivery: In vitro optimization". Saudi Pharmaceutical Journal 23 (3): 290–302. July 2015. doi:10.1016/j.jsps.2014.11.004. PMID 26106277.
- ↑ "Oral amphotericin B: challenges and avenues.". Int. J. Pharm. Biosci. Technol. 1 (1): 1–9. 2013. https://www.researchgate.net/publication/236578662.
- ↑ "Oral Lipid Nanocrystal Amphotericin B for Cryptococcal Meningitis: A Randomized Clinical Trial". Clinical Infectious Diseases 77 (12): 1659–1667. August 2023. doi:10.1093/cid/ciad440. PMID 37606364.
- ↑ "Fluid Stewardship of Maintenance Intravenous Fluids". Journal of Pharmacy Practice 35 (5): 769–782. October 2022. doi:10.1177/08971900211008261. PMID 33827313.
- ↑ "Tolerability profile of the current antifungal armoury". The Journal of Antimicrobial Chemotherapy 73 (suppl_1): i26–i32. January 2018. doi:10.1093/jac/dkx446. PMID 29304209.
- ↑ "Shake and Bake". TheFreeDictionary.com. http://medical-dictionary.thefreedictionary.com/Shake+and+Bake.
- ↑ "Studies on Amphotericin B". Chem 491, Chemistry Department. University of Wisconsin-Eau Claire. http://www.chem.uwec.edu/chem491_w09/ambliposomereview.pdf.
- ↑ "Induction of prostaglandin synthesis as the mechanism responsible for the chills and fever produced by infusing amphotericin B". The Journal of Infectious Diseases 156 (5): 784–789. November 1987. doi:10.1093/infdis/156.5.784. PMID 3309074.
- ↑ "The antifungal drug amphotericin B promotes inflammatory cytokine release by a Toll-like receptor- and CD14-dependent mechanism". The Journal of Biological Chemistry 278 (39): 37561–37568. September 2003. doi:10.1074/jbc.M306137200. PMID 12860979.
- ↑ "Differential effects of amphotericin B and liposomal amphotericin B on inflammatory cells in vitro". Inflammation Research 51 (5): 259–264. May 2002. doi:10.1007/pl00000302. PMID 12056514.
- ↑ "Pretreatment regimens for adverse events related to infusion of amphotericin B". Clinical Infectious Diseases 20 (4): 755–761. April 1995. doi:10.1093/clinids/20.4.755. PMID 7795069.
- ↑ "Nephrotoxic effects of amphotericin B, including renal tubular acidosis". The American Journal of Medicine 46 (1): 154–162. January 1969. doi:10.1016/0002-9343(69)90067-9. PMID 4951424.
- ↑ "Liposomal amphotericin B for empirical therapy in patients with persistent fever and neutropenia. National Institute of Allergy and Infectious Diseases Mycoses Study Group". The New England Journal of Medicine 340 (10): 764–771. March 1999. doi:10.1056/NEJM199903113401004. PMID 10072411.
- ↑ "Clinical practice guidelines for the management of cryptococcal disease: 2010 update by the infectious diseases society of america". Clinical Infectious Diseases 50 (3): 291–322. February 2010. doi:10.1086/649858. PMID 20047480.
- ↑ Jill Adler-Moore,* and Richard T. liposomal formulation, structure, mechanism of action and pre-clinical experience. Journal of Antimicrobial Chemotherapy (2002) 49, 21–30
- ↑ 50.0 50.1 50.2 "Amphotericin B and its new derivatives - mode of action". Current Drug Metabolism 10 (5): 459–469. June 2009. doi:10.2174/138920009788898019. PMID 19689243.
- ↑ "Fluid, electrolyte and acid-base disorders associated with antibiotic therapy". Nature Reviews. Nephrology 5 (4): 193–202. April 2009. doi:10.1038/nrneph.2009.17. PMID 19322184.
- ↑ "Acute Infusion-Related Side Effects of Amphotericin B Lipid Complex (ABLC) in Oncohematological Patients: Real-World Data from Brazilian Reference Centers". Infectious Diseases and Therapy (Springer Nature) 14 (1): 133–148. January 2025. doi:10.1007/s40121-024-01086-y. PMID 39615018.
- ↑ "Drug-induced hypersensitivity syndrome by liposomal amphotericin-B: a case report". BMC Research Notes (BioMed Central Ltd.) 8 (1). September 2015. doi:10.1186/s13104-015-1486-0. PMID 26420570.
- ↑ "Liposomal amphotericin B-induced reversible ototoxicity in a patient with disseminated histoplasmosis". Indian Journal of Pharmacology (Wolters Kluwer – Medknow) 53 (2): 157–159. 26 May 2021. doi:10.4103/0253-7613.316948. PMID 34100400.
- ↑ "Reversible ototoxicity: a rare adverse reaction of liposomal amphotericin-B used for the treatment of antimony-resistant visceral leishmaniasis in an elderly male". Clinical Medicine Insights. Case Reports (SAGE Publications Ltd.) 7. 24 July 2014. doi:10.4137/CCRep.S15111. PMID 25093006.
- ↑ "New antifungal kills without toxic side effects". https://www.science.org/content/article/new-antifungal-kills-without-toxic-side-effects.
- ↑ "Abelcet Package Insert". Sigma-Tau Pharmaceuticals. https://leadiant.com/wp-content/uploads/2017/02/Abelcet-PI-PDF.pdf.
- ↑ 58.0 58.1 "It only takes one to do many jobs: Amphotericin B as antifungal and immunomodulatory drug". Frontiers in Microbiology 3: 286. 2012-01-01. doi:10.3389/fmicb.2012.00286. PMID 23024638.
- ↑ "Exposure of the yeast Candida albicans to the anti-neoplastic agent adriamycin increases the tolerance to amphotericin B". The Journal of Pharmacy and Pharmacology 55 (12): 1629–1633. December 2003. doi:10.1211/0022357022359. PMID 14738588.
- ↑ "Molecular modeling of amphotericin B-ergosterol primary complex in water II". Biophysical Chemistry 141 (2–3): 162–168. May 2009. doi:10.1016/j.bpc.2009.01.010. PMID 19233539.
- ↑ "Scedosporium prolificans osteomyelitis in an immunocompetent child treated with voriconazole and caspofungin, as well as locally applied polyhexamethylene biguanide". Journal of Clinical Microbiology (American Society for Microbiology) 41 (8): 3981–3985. August 2003. doi:10.1128/JCM.41.8.3981-3985.2003. PMID 12904435.
- ↑ "The production of reactive oxygen species is a universal action mechanism of Amphotericin B against pathogenic yeasts and contributes to the fungicidal effect of this drug". Antimicrobial Agents and Chemotherapy (American Society for Microbiology) 58 (11): 6627–6638. November 2014. doi:10.1128/AAC.03570-14. PMID 25155595.
- ↑ "Amphotericin B Resistance in Aspergillus terreus Is Overpowered by Coapplication of Pro-oxidants". Antioxidants & Redox Signaling (SAGE Publications Ltd.) 23 (18): 1424–1438. December 2015. doi:10.1089/ars.2014.6220. PMID 26054424.
- ↑ 64.0 64.1 "Amphotericin B: side effects and toxicity". Revista Iberoamericana De Micologia 26 (4): 223–227. December 2009. doi:10.1016/j.riam.2009.06.003. PMID 19836985.
- ↑ "Amphocin, amphotericin B for injection, USP". Pfizer. http://www.pfizer.com/files/products/uspi_amphocin.pdf.
- ↑ "Differences in the interaction of the polyene antibiotic amphotericin B with cholesterol- or ergosterol-containing phospholipid vesicles. A circular dichroism and permeability study". Biochemistry 22 (12): 2939–2944. June 1983. doi:10.1021/bi00281a024. PMID 6871175.
- ↑ "Evaluation of ergosterol content in the air of various environments". Aerobiologia (Springer Nature) 31 (1): 33–44. 6 June 2014. doi:10.1007/s10453-014-9344-4. PMID 25750476.
- ↑ 68.0 68.1 "Pharmacology of amphotericin B". UpToDate (Wolters Kluwer). 18 August 2025. ISSN 0002-7863. https://www.uptodate.com/contents/pharmacology-of-amphotericin-b. Retrieved 20 October 2025.
- ↑ "A labile point in mutant amphotericin polyketide synthases". Biotechnology Letters 33 (6): 1121–1126. June 2011. doi:10.1007/s10529-011-0538-3. PMID 21267757. https://hal.science/hal-00663072.
- ↑ 70.0 70.1 "Biosynthesis of amphotericin B". Journal of the Chemical Society, Perkin Transactions 1 (1): 83–88. January 1998. doi:10.1039/A704545J. https://lra.le.ac.uk/bitstream/2381/33805/1/U087475.pdf. Retrieved 2018-05-16.
- ↑ 71.0 71.1 "Amphotericin biosynthesis in Streptomyces nodosus: deductions from analysis of polyketide synthase and late genes". Chemistry & Biology 8 (7): 713–723. July 2001. doi:10.1016/S1074-5521(01)00046-1. PMID 11451671.
- ↑ "Antibiotics produced by Streptomyces". The Brazilian Journal of Infectious Diseases 16 (5): 466–471. 2012. doi:10.1016/j.bjid.2012.08.014. PMID 22975171.
- ↑ "Total synthesis of amphotericin B". Journal of the American Chemical Society 109 (9): 2821–2822. 1987-04-01. doi:10.1021/ja00243a043. ISSN 0002-7863. Bibcode: 1987JAChS.109.2821N.
- ↑ Salvatore A. La Barbera, M.D. New York State Journal of Medicine, Vol. 59, No. 19, Oct 1, 1959.
- ↑ "Chemistry and biology of the polyene macrolide antibiotics". Bacteriological Reviews 37 (3): 166–196. September 1973. PMID 4202146.
- ↑ Christine D. Waugh, in xPharm: The Comprehensive Pharmacology Reference, 2007.
- ↑ "Halizon". http://edudrugs.com/H/Halizon.html.
External links
- AmBisome Summaries of Product Characteristics (United Kingdom)
- Amphotericin B
- "Amphotericin B Liposomal Injection". https://medlineplus.gov/druginfo/meds/a616018.html.
- "Amphotericin B Lipid Complex Injection". https://medlineplus.gov/druginfo/meds/a601132.html.
 |
