| Risk factor |
Notes |
References
|
| Previous episodes of thrombosis
|
also a risk factor for embolism formation[17]
|
[18][19]
|
| Family History of Deep Vein Thrombosis
|
|
[20][14]
|
| Gender, and race
|
not firmly established
increased prevalence in women during childbearing years
|
[14]
|
| Smoking
|
modifiable, difficult
|
[19][21]
|
| Diabetes
|
|
[18]
|
| Arteriosclerosis
|
|
[18]
|
| Renal disease
|
"hypercoagulable state"[18]
|
[18]
|
| Vasoconstriction
|
|
[22]
|
| Myocardial infarction and other types of heart disease
|
Heart attack, Unstable angina Dysrhythmias Heart failure
|
[20][22][18]
|
| Slow or turbulent blood flow
|
modifiable with exercise
|
[22][24]
|
| Stroke
|
heparins contraindicated[24]
|
[18][24]
|
| Sedentary life style
|
modifiable with exercise
|
[22][19][14]
|
| Plaster cast
|
transient
|
[18]
|
| Dehydration
|
modifiable
also related to athletic activities and sports
|
[22][20]
|
| Acute respiratory failure
|
|
[18]
|
| Dysrhythmias
|
|
[22]
|
| Shock |
|
[22]
|
| Obesity |
modifiable |
[15][25][1][22][18][19]
|
| Pregnancy and the post-partum period
|
"hypercoagulable state"[18]
|
[15][1][22][20][14]
|
| Varicose veins
|
|
[18]
|
| Surgery
|
length of the surgical procedure
type of operation
hip or knee surgery[14]
related to subsequent state of hypercoagulability [13]
|
[15][1][25][19][20][21]
|
| Lung disease
|
|
[20]
|
| Trauma
|
related to immobility
|
[15][1][18][14]
|
| Estrogen-based oral contraceptive
|
discontinuation reduces risk
related to progestogen and ethinylestradiol[26]
|
[15][1][22][20][26][14][21]
|
| Hormone replacement therapy
|
discontinuation reduces risk
|
[15]
|
| Ovarian hyper-stimulation therapy to treat infertility
|
|
[15]
|
| Compression of a vein or artery by abnormality, tumor, hematoma
|
|
[15]
|
| Pacing wires
|
|
[1]
|
| Local vein damage, incompetent valves
|
|
[1][22]
|
| Central venous catheters
|
|
[1]
|
| Dialysis catheters
|
|
[1]
|
| Repetitive motion injury
|
|
[1]
|
| Immobility
|
associated with air travel, long travel times and
post-surgical – modifiable risk
|
[1][18][19][14][21][13]
|
| Spinal cord injury
|
|
[1]
|
| Age
|
|
[1][15][22][18]
|
| Cancers
|
|
[1][20][14]
|
| Sepsis
|
|
[1]
|
| Polycythemia
|
heparins contraindicated[24]
|
[1]
|
| Genetic deficiencies or autoimmune disorders, Protein C and/or S deficiency
|
congenital; associated with warfarin necrosis, heparins contraindicated[24]
|
[1][27][21]
|
| Antiphospholipid antibody syndrome
|
altered coagulation; heparins contraindicated[24]
|
[1]
|
| Factor V Leiden defect
|
altered coagulation
|
[1]
|
| Prothrombin G20210A defect
|
altered coagulation; heparins contraindicated[24]
|
[1]
|
| Hyperhomocysteinimia
|
altered coagulation; heparins contraindicated[24]
|
[1]
|
| Elevated factors II, VIII, IX, XI
|
altered coagulation; heparins contraindicated[24]
|
[1][14]
|
| Antithrobin III deficiency
|
altered coagulation; heparins contraindicated[24]
|
[1][14]
|
| Falls and hip fracture
|
related to immobility
|
[1][19]
|
| Selective estrogen-receptor modulators
|
|
[15]
|
| Erythropoiesis-stimulating agents
|
|
[15]
|
| Acute medical illness
|
|
[15][14]
|
| Inflammatory bowel disease
|
|
[15]
|
| Nephrotic syndrome
|
|
[15]
|
| Myeloproliferative disorders
|
|
[15]
|
| Paroxysmal nocturnal hemoglobinnuria
|
|
[15]
|
| Thrombophilias
|
heparins contraindicated[24]
|
[15][14]
|
| Post-menopausal hormone replacement therapy
|
discontinuation reduces risk
|
[15]
|
| Right heart failure
|
|
[22]
|
| Venous inflammation/phlebitis
|
when a thrombus forms, it is thrombophlebitis
|
[22]
|
| Sickle cell disease
|
|
|
| Artificial heart valves
|
|
[24]
|
Probability and risk estimation for developing blood clots
| Major risk (=1 point) |
Minor risk (=2 points)
|
| Cancer |
Family history of
deep vein thrombosis
|
| Immobility |
Hospitalization within
the past 6 months
|
| Calf swelling |
superficial vein dilation
|
| Recent major surgery |
redness of area
|
| Edema or swelling of only leg |
Recent trauma
to leg
|
Tenderness in
the calf and/or thigh |
|
Scoring of the risks associated with formation of blood clots
| Probability determination and scoring
|
| High probability scoring (12–7 points
|
3 major points OR
2 major points AND >2 minor points
|
| Low probability scoring (3–5 points)
|
0 major points AND > 2 minor points
1 major point AND >2 minor points
0 major points and >3 minor point
1 major point and more than one minor point
|
| Moderate probability scoring (varies)
|
| all other risk combinations
|
Risk for subsequent blood clots
Developing blood clots is more probable after the first episode. Risk assessment and intervention for those with one or more episodes of deep vein thrombosis or blood clots in the veins utilizes the Well's test. It has been inconsistently modified by a number of publishers with the results listed below:[28]
Well's and modified Well's risk scoring
Well's and modified Well's scoring
| Finding |
points |
references
|
| D-dimer abonormal one month after stopping anticoagulants
|
2
|
[28]
|
| Age > or = to 50
|
1
|
[28]
|
| male
|
1
|
[28]
|
| use of hormone at DVT onset
|
1
|
[28]
|
Adapted for the emergency department
modified Well's scoring
| Finding |
points |
references
|
| Malignancy
|
1
|
[29]
|
| Age > or = to 50
|
1
|
[29]
|
| cast on lower leg/Paralysis/paresis/
|
1
|
[29]
|
| Recent surgery or immobility
|
1
|
[29]
|
| tenderness over deep vein
|
1
|
[29]
|
| entire leg swollen
|
1
|
[29]
|
| difference of 3 cm between legs
|
1
|
[29]
|
| pitting edema of affected leg
|
1
|
[29]
|
| Collateral superficial veins
|
1
|
[29]
|
| another diagnosis more probable than DVT
|
−2
|
[29]
|
Scoring:
- less than 2 points – low risk (3%)
- 2–6 points moderate risk (17%)
- > 6 points high risk (75%)[29]
General interventions
The Centers for Disease Control and Prevention have issued general guidelines describing the interventions that can be taken to reduce the risk of the formation of blood clots:
The Centers for Disease Control and Prevention recommend the following:
- Move around as soon as possible after having been confined to bed, such as after surgery, illness, or injury.
- If you're at risk for DVT, talk to your doctor about:
- Graduated compression stockings (sometimes called "medical compression stockings")
- Medication (anticoagulants) to prevent DVT.
- When sitting for long periods of time, such as when traveling for more than four hours:
- Get up and walk around every 2 to 3 hours.
- Exercise your legs while you're sitting by:
- Raising and lowering your heels while keeping your toes on the floor
- Raising and lowering your toes while keeping your heels on the floor
- Tightening and releasing your leg muscles
- Wear loose-fitting clothes.
- You can reduce your risk by maintaining a healthy weight, avoiding a sedentary lifestyle, and following your doctor's recommendations based on your individual risk factors.[7]
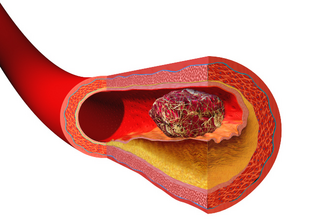
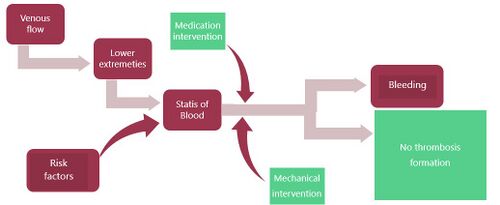
 a lower leg vein with good flow – statis of blood would occur if this vein was compressed and blood flow decreased or was stopped Interventions during travel
Seat-edge pressure from the seat on an airplane on the popliteal area may contribute to vessel wall damage as well as venous stasis. Coagulation activation may result from an interaction between cabin conditions (such as hypobaric hypoxia) and individual risk factors for the formation of blood clots. Studies of the pathophysiologic mechanisms for the increased risk of Venous thrombosis embolism or VTE after long-distance travel have not produced consistent results, but venous stasis appears to play a major role; other factors specific to air travel may increase coagulation activation, particularly in passengers with individual risk factors for VTE.[30]
Interventions for those hospitalized
Compression devices
Mechanical compression devices are used for prevention of thrombosis and are beneficial enough to be used by themselves with patients at low to moderate risk.[4] The use of fitted intermittent pneumatic compression devices before, during and after procedures is used in inpatient settings. It consists of an air pump and inflatable auxiliary compartments that sequentially inflates and deflated to provide an external 'pump' that returns venous blood toward the heart.[31] The use of intermittent pneumatic compression is common.[31][19][5] These devices are also placed on a surgical patient in the operating room (the intra-surgical period) and remain on the person while recovering from the surgery.[32]
The application of antiembolism stockings can be used to prevent thrombosis.[4] The correct use and properly fitted graded compression stockings can reduce the rate of thrombosis by 50%.[15][19]:745–46 Contraindications for the use of antiembolism stockings include the presence of advanced peripheral and obstructive arterial disease, septic phlebitis, heart failure, open wounds, dermatitis and peripheral neuropathy.[33] Differences between the use of thigh-high compression stockings and shorter types to prevent blood clots exist, but remain inconsistent.[4][5]
Assessment
There has been some success in preventing blood clots by an early risk assessment upon admission to the hospital, which is a strategy recognized by the Centers for Disease Control and Prevention. Hospitals that have participated in this effort to reduce the incidence of thrombosis found that rates of DVT decreased in some instances.[34] Some hospitals developed a mandatory assessment quantifying the risk for developing blood clots and a plan of care developed from the results. The person's risk for developing blood clots is entered into their record, 'following' them through their treatment regime. If the hospital stay exceeds three days, the person will be reassessed for risk. Clinicians are then able to apply protocols for prevention based upon best clinical practices.[35][36]
Interventions to treat immobility
 The poplitial vein can be one site of venous stasis in the lower leg. Obstruction of this vein during travel contributes to statis. Immobility is a significant risk factor in the development of thrombosis.[37][38][22][25] Immediate post-surgical interventions, such as out of bed orders (OOB), are typically ordered by the physician to prevent thrombosis. These orders, typically delegated to a nurse, but may include the participation of a physical therapist and others trained to perform the intervention, are to perform range of motion (ROM) activities that include: muscle contractions of the lower legs for those who are very weak, moving the feet, wiggling the toes, bending the knees, raise and lower the legs. In addition, changes in positioning prevents immobility and shifts areas of venous stasis. If the person is too weak to perform these preventative activities, hospital personnel will perform these movements independently. Exercise of the lower extremities is a post-operative method of prophylaxis. Nursing personnel will often perform range of motion exercises and encourage frequent moving of the legs, feet, and ankles. Frequent positioning changes and adequate fluid intake. After a surgical procedure, ambulation as soon as possible is prophylactic in preventing the formation of blood clots.[38][22][25]
Early ambulation also prevents venous stasis and physicians order OOB activities on the same day of surgery. This is accomplished in increments. The progression of increasing mobility proceeds by: raising the head of the bed, sitting up in bed, moving to the edge of the bed, dangling the legs off the bed and then ambulating to a close chair.[19][25]
Patient education and compliance reduces the risk of developing blood clots. These exercises and use of equipment and follow up by clinicians reduces the risk of developing blood clots.[25]
Note that if a blood clot has already formed in the deep veins of the leg, bedrest is usually prescribed and the treatment to prevent bloods with physical intervention is contraindicated.[citation needed]
Medication
Anticoagulants and antiplatelets
Thromboprophylaxis, such as anticoagulants or perioperative heparin, is effective for hospitalized patients at risk for VTE.[2][39] Additional risk factors such as obesity, disease, malignancies, long surgeries, and immobility may influence the prescribed dosage. Anticoagulant medications may prevent the formation of blood clots in people who are at high risk for their development.[4] Treating blood clots that have already formed is managed by the use of anti-hemolytic ("clot busters"). Despite its effectiveness, the use of thromboprophylaxis remains under-utilized, though alerts (computer or human) in hospitals are associated with increased prescription and reductions in symptomatic VTE.[39] The list below describes some of the more common medications used to prevent blood clots.[24] Note that generally since blood clotting is inhibited, a side effect typically is increased bleeding, though it can be reversed by administering a medication that stops the bleeding or by discontinuation of the medication itself. Anti-coagulant administration is often given before the start of the operation.[25] Medications that inhibit blood clot formation include:
Medications used to prevent blood clots
|
| Name of medication
|
Therapeutic/pharmologic class
|
Action
|
Route
|
Other uses
|
Notes
|
Side effects
|
References
|
| aspirin
|
|
antiplatelet
|
|
|
|
risks for GI tract bleeding and hemorrhagic stroke[40][41]
|
[32][42][43]
|
| dipyridamole
|
platelet aggregation inhibitor
|
|
oral or intravenous
|
|
|
Abdominal or stomach cramps, diarrhea, dizziness or lightheadedness
|
[44][45][46][41]
|
| clopidogrel
|
antiplatelet
|
|
|
|
|
|
[45][41]
|
| ticlid
|
|
|
|
|
|
|
|
| enoxaparin
|
anticoagulant
|
activation of antiprothrombin, prevents fibrin formation
|
slow IV
|
|
platelet count is monitored
|
|
[45][41]
|
| dalteparin
|
anticoagulant
|
activation of antiprothrombin, prevents fibrin formation
|
IV
|
|
|
|
[41]
|
| fondaparinux
|
anticoagulant
|
inhibits thrombin production
|
injection
|
|
aspirin not recommended with this medication
|
|
[41][24][2]
|
| dabigatran
|
|
inhibits prothrombin
|
|
|
|
|
[41]
|
| bivalirudin
|
|
inhibits prothrombin
|
|
|
often given with aspirin
|
|
[41]
|
| argatroban
|
anticoagulant
|
inhibits prothrombin
|
IV
|
|
alternative to heparin in those developing heparin-induced thrombocytopenia
|
|
[41][24]
|
| desirudin
|
anticoagulant
|
inhibits prothombin
|
injection
|
|
used with hip replacement
|
|
[41][24]
|
| eptifiatide
|
antiplatelet
|
|
|
|
|
|
[41]
|
| tirofiban
|
antiplatelet
|
|
|
|
|
|
[41]
|
| ticlopidine
|
antiplatelet
|
|
|
|
|
|
[41]
|
| pentocifylline
|
antiplatelet
|
|
|
|
|
|
[41]
|
| diyridamole
|
anitplatelet
|
|
|
|
|
|
[41]
|
| cilostazol
|
antiplatelet
|
|
|
|
|
|
[41]
|
| rivaroxaban
|
|
inhibits factor Xa
|
|
|
use with antiplatelets cautioned
|
GI bleeding
|
[41]
|
| warfarin
|
anticoagulant
|
Thrombin inhibitor;
|
IV
|
|
|
|
[24]
|
| lipirudin
|
anticoagulant
|
inhits prothrombin
|
IV
|
|
treatment may extend to 10 days
|
|
[24]
|
| dextran
|
|
|
|
|
|
|
[4]
|
Heparins
Adding heparin to the use of compression stockings may prevent thrombosis for those of higher risk.[4][47]
Heparin Prophylaxis
| name |
action |
structure |
references
|
|
|
|
|
Low-molecular weight heparin
(example: Reviparin) |
|
|
[48][49][51][52]
|
The discontinuation of contraceptives also prevents blood clots.[15]
Herbal interactions
The therapeutic effects of warfarin may be decreased by valerian. Anticoagulants can be affected by chamomile. Dong quai, garlic, ginger, Ginkgo biloba, bilberry and feverfew can increase bleeding time. These same herbal supplements taken with warfarin increased prothrombin time.[24]
Dietary interactions
By containing significant content of vitamin K, some foods act as antagonists to antiplatelet and anticoagulant medications; these include green leafy vegetables, like spinach, legumes, and broccoli.[24]
Contraindications
Preventing blood clots with medication is not considered safe in the following circumstances:
Research
An international registry and risk assessment calculator is being used to centralize data on post-surgical venous thrombosis and its prevention.[53] Hospitals are implementing a multi-disciplinary approach to prevent of blood clots. This includes adequate assessment of the risks, follow up on missed doses of medication and instituting a 'patient-centered' approach endorsed by the Joint Commission.[34] Recommendations regarding the prevention of blood clots vary widely between clinicians and treatment facilities. Research continues to clarify these discrepancies.[5] The metabolic state of hypercoagulability (the tendency to form blood clots) tests are being developed. These include the evaluation of the thrombin–antithrombin complexes (TAT), low levels of the anticoagulants ATIII and protein C, but these tests are not yet widely available.[13]
References
 Using Wikipedia for Research Using Wikipedia for Research
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 Brunner, Lillian (2010). Brunner & Suddarth's textbook of medical-surgical nursing. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 876. ISBN 978-0781785907.
- ↑ 2.0 2.1 2.2 2.3 "Anticoagulation for perioperative thromboprophylaxis in people with cancer". The Cochrane Database of Systematic Reviews 2019 (7): CD009447. July 2018. doi:10.1002/14651858.cd009447.pub3. PMID 29993117.
- ↑ 3.0 3.1 Kahale, Lara A.; Matar, Charbel F.; Hakoum, Maram B.; Tsolakian, Ibrahim G.; Yosuico, Victor Ed; Terrenato, Irene; Sperati, Francesca; Barba, Maddalena et al. (2021-12-08). "Anticoagulation for the initial treatment of venous thromboembolism in people with cancer". The Cochrane Database of Systematic Reviews 2021 (12): CD006649. doi:10.1002/14651858.CD006649.pub8. ISSN 1469-493X. PMID 34878173.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 "Towards evidence-based guidelines for the prevention of venous thromboembolism: systematic reviews of mechanical methods, oral anticoagulation, dextran and regional anaesthesia as thromboprophylaxis". Health Technology Assessment 9 (49): iii–iv, ix–x, 1–78. December 2005. doi:10.3310/hta9490. PMID 16336844.
- ↑ 5.0 5.1 5.2 5.3 Grotta, James (2016). Stroke : pathophysiology, diagnosis, and management. Philadelphia: Elsevier. pp. 953–62. ISBN 978-0323295444.
- ↑ "Thrombotic risk factors: basic pathophysiology". Critical Care Medicine 38 (2 Suppl): S3-9. February 2010. doi:10.1097/CCM.0b013e3181c9cbd9. PMID 20083911.
- ↑ 7.0 7.1 "Venous Thromboembolism (Blood Clots) Facts". Division of Blood Disorders National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention. 24 February 2016. https://www.cdc.gov/ncbddd/dvt/facts.html.
 This article incorporates text from this source, which is in the public domain. This article incorporates text from this source, which is in the public domain.
- ↑ "ICD-10 Version:2016". International Statistical Classification of Diseases and Related Health Problems 10th Revision. http://apps.who.int/classifications/icd10/browse/2016/en#/I80.
- ↑ Leveno, Kenneth (2013). Williams manual of pregnancy complications. New York: McGraw-Hill Medical. ISBN 978-0071765626.
- ↑ "A systematic review of clinical prediction scores for deep vein thrombosis". Phlebology 32 (8): 516–531. September 2017. doi:10.1177/0268355516678729. PMID 27885107.
- ↑ "Venous Thromboembolism (VTE)". National Center on Birth Defects and Developmental Disabilities. https://www.cdc.gov/ncbddd/aboutus/annualreport2012/documents/ar2012-vte-printversion.pdf.
 This article incorporates text from this source, which is in the public domain. This article incorporates text from this source, which is in the public domain.
- ↑ "Awareness and politics of venous thromboembolism in the United kingdom". Arteriosclerosis, Thrombosis, and Vascular Biology 28 (3): 398–9. March 2008. doi:10.1161/ATVBAHA.108.162586. PMID 18296598.
- ↑ 13.0 13.1 13.2 13.3 Newman, Mark (2008). Perioperative medicine : managing for outcome. Philadelphia: Saunders Elsevier. pp. 29–34. ISBN 978-1437721263. https://archive.org/details/perioperativemed00mdma.
- ↑ 14.00 14.01 14.02 14.03 14.04 14.05 14.06 14.07 14.08 14.09 14.10 14.11 14.12 14.13 Henke, Peter K.; Meissner, Mark H.; Wakefield, Thomas W.. "Chapter 2: Risk Factors for Venous Thrombosis". American Venous Forum. http://www.veinforum.org/uploadDocs/1/Chapter-2---Risk-Factors-for-Venous-Thrombosis.pdf.
- ↑ 15.00 15.01 15.02 15.03 15.04 15.05 15.06 15.07 15.08 15.09 15.10 15.11 15.12 15.13 15.14 15.15 15.16 15.17 15.18 15.19 15.20 Hoffman, Barbara (2012). Williams gynecology. New York: McGraw-Hill Medical. pp. 960–968. ISBN 978-0071716727.
- ↑ "Impact of treatment algorithms on the prescribing of antithrombotic therapy in patients with suspected acute coronary syndrome – a prospective audit". British Journal of Clinical Pharmacology 80 (5): 1176–1184. November 2015. doi:10.1111/bcp.12714. PMID 26147691.
- ↑ "Patients with Venous Thromboembolism ) Registry". RIETE. https://www.riete.org/info/estimate-calculator/index.php.
- ↑ 18.00 18.01 18.02 18.03 18.04 18.05 18.06 18.07 18.08 18.09 18.10 18.11 18.12 18.13 18.14 Moliterno, David (2013). Therapeutic advances in thrombosis. Chichester, West Sussex: Wiley-Blackwell. pp. 306–327. ISBN 978-1405196253.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 19.6 19.7 19.8 19.9 Rosdahl, Caroline (2012). Textbook of basic nursing. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 789. ISBN 978-1605477725. https://archive.org/details/textbookbasicnur00rosd.
- ↑ 20.0 20.1 20.2 20.3 20.4 20.5 20.6 20.7 "DVT: Myths vs. Facts | American Society of Hematology". http://www.hematology.org/Patients/Blood-Disorders/Clots/3816.aspx.
- ↑ 21.0 21.1 21.2 21.3 21.4 Drake, Richard (2012). Gray's basic anatomy, with Student Consult. Philadelphia: Elsevier/Churchill Livingstone. pp. 133–205. ISBN 978-1455710782.
- ↑ 22.00 22.01 22.02 22.03 22.04 22.05 22.06 22.07 22.08 22.09 22.10 22.11 22.12 22.13 22.14 22.15 Copstead, Lee (2013). Pathophysiology. St. Louis, Mo: Elsevier. pp. 320–329. ISBN 978-1455726509.
- ↑ 24.00 24.01 24.02 24.03 24.04 24.05 24.06 24.07 24.08 24.09 24.10 24.11 24.12 24.13 24.14 24.15 24.16 24.17 24.18 24.19 Kee, Joyce (2012). Pharmacology : a nursing process approach. St. Louis, MO: Elsevier Saunders. p. 670–677. ISBN 978-1437717112. https://archive.org/details/pharmacologynurs7edkeej.
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 25.6 Atlas of gynecologic surgery. Stuttgart: Thieme. 2014. ISBN 978-3136507049; Access provided by the University of Pittsburgh
- ↑ 26.0 26.1 "Combined oral contraceptives: venous thrombosis". The Cochrane Database of Systematic Reviews 2014 (3): CD010813. March 2014. doi:10.1002/14651858.CD010813.pub2. PMID 24590565.
- ↑ "The role of leukocytes in thrombosis". Blood 128 (6): 753–762. August 2016. doi:10.1182/blood-2016-05-718114. PMID 27354721.
- ↑ 28.0 28.1 28.2 28.3 28.4 "Wells criteria for DVT is a reliable clinical tool to assess the risk of deep venous thrombosis in trauma patients". World Journal of Emergency Surgery 11 (1): 24. 2016. doi:10.1186/s13017-016-0078-1. PMID 27279896.
- ↑ 29.00 29.01 29.02 29.03 29.04 29.05 29.06 29.07 29.08 29.09 29.10 Markovchick, Vincent (2016). Emergency medicine secrets. Philadelphia, PA: Elsevier. pp. 190–95. ISBN 978-0323355162.
- ↑ "Deep Vein Thrombosis & Pulmonary Embolism, Chapter 2, Travelers' Health". CDC. https://wwwnc.cdc.gov/travel/yellowbook/2016/the-pre-travel-consultation/deep-vein-thrombosis-pulmonary-embolism.
 This article incorporates text from this source, which is in the public domain. This article incorporates text from this source, which is in the public domain.
- ↑ 31.0 31.1 "Prevention of VTE in nonorthopedic surgical patients: Antithrombotic Therapy and Prevention of Thrombosis 9th ed, American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest 141 (2 Suppl): e227S–e277S. February 2012. doi:10.1378/chest.11-2297. PMID 22315263.
- ↑ 32.0 32.1 "Aspirin for the prophylaxis of venous thromboembolic events in orthopedic surgery patients: a comparison of the AAOS and ACCP guidelines with review of the evidence". The Annals of Pharmacotherapy 47 (1): 63–74. January 2013. doi:10.1345/aph.1R331. PMID 23324504.
- ↑ Stemmer, Robert (February 2013). "Compression Bulletin 24". Sigvaris. p. 2. http://www.sigvariscares.com/ftp/CB/COMPBUL24.pdf.
- ↑ 34.0 34.1 "The Johns Hopkins Venous Thromboembolism Collaborative: Multidisciplinary team approach to achieve perfect prophylaxis". Journal of Hospital Medicine 11 (Suppl 2): S8–S14. December 2016. doi:10.1002/jhm.2657. PMID 27925423.
- ↑ "The 2015 Healthcare-Associated Venous Thromboembolism Prevention Challenge Champions". CDC. 7 December 2016. https://www.cdc.gov/ncbddd/dvt/ha-vte-challenge.html.
 This article incorporates text from this source, which is in the public domain. This article incorporates text from this source, which is in the public domain.
- ↑ "Evaluation of an institutional project to improve venous thromboembolism prevention". Journal of Hospital Medicine 11 (Suppl 2): S29–S37. December 2016. doi:10.1002/jhm.2663. PMID 27925424.
- ↑ "Frequently Asked questions". Thrombosis UK. 2015. http://www.thrombosisuk.org/awareness-questions.php.
- ↑ 38.0 38.1 Potter, Patricia (2013). Fundamentals of nursing. St. Louis, Mo: Mosby Elsevier. p. 1149. ISBN 978-0323079334.
- ↑ 39.0 39.1 Kahn, Susan R.; Morrison, David R.; Diendéré, Gisèle; Piché, Alexandre; Filion, Kristian B.; Klil-Drori, Adi J.; Douketis, James D.; Emed, Jessica et al. (24 April 2018). "Interventions for implementation of thromboprophylaxis in hospitalized patients at risk for venous thromboembolism". The Cochrane Database of Systematic Reviews 2018 (4): CD008201. doi:10.1002/14651858.CD008201.pub3. ISSN 1469-493X. PMID 29687454.
- ↑ "Evidence Summary: Bleeding Risks With Aspirin Use: Aspirin Use to Prevent Cardiovascular Disease and Colorectal Cancer: Preventive Medication". US Preventive Services Task Force. April 2016. https://www.uspreventiveservicestaskforce.org/Page/Document/evidence-summary-bleeding-risks-with-aspirin-use/aspirin-to-prevent-cardiovascular-disease-and-cancer.
- ↑ 41.00 41.01 41.02 41.03 41.04 41.05 41.06 41.07 41.08 41.09 41.10 41.11 41.12 41.13 41.14 41.15 41.16 Henry, Norma (2016). RN pharmacology for nursing : review module. Overland Park, KS: Assessment Technologies Institute. pp. 191–98. ISBN 978-1565335738.
- ↑ "Final Update Summary: Aspirin Use to Prevent Cardiovascular Disease and Colorectal Cancer: Preventive Medication". US Preventive Services Task Force. April 2016. https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/aspirin-to-prevent-cardiovascular-disease-and-cancer?ds=1&s=Aspirin.
- ↑ "Talk with Your Doctor about Taking Aspirin Every Day". US Preventive Services Task Force. April 2016. https://healthfinder.gov/HealthTopics/Category/health-conditions-and-diseases/heart-health/talk-with-your-doctor-about-taking-aspirin-every-day#the-basics_2.
- ↑ "Dipyridamole" at Dorland's Medical Dictionary
- ↑ 45.0 45.1 45.2 "Recommended Use of Aspirin and Other Antiplatelet Medications Among Adults, National Ambulatory Medical Care Survey and National Hospital Ambulatory Medical Care Survey, United States, 2005–2008". Centers for Disease Control and Prevention. 15 June 2012. https://www.cdc.gov/mmwr/preview/mmwrhtml/su6102a3.htm.
- ↑ "Dipyridamole Monograph for Professionals". https://www.drugs.com/monograph/dipyridamole.html.
- ↑ "Meta-analysis of randomized trials comparing combined compression and anticoagulation with either modality alone for prevention of venous thromboembolism after surgery". The British Journal of Surgery 101 (9): 1053–62. August 2014. doi:10.1002/bjs.9527. PMID 24916118.
- ↑ "Patients at risk of venous thromboembolism—clinical results with reviparin". Thrombosis Research 81 (2 Suppl): S39-45. 1996. doi:10.1016/0049-3848(95)00228-6. PMID 8822126.
- ↑ "Deep-vein thrombosis prophylaxis in orthopedic surgery: hip surgery". Seminars in Thrombosis and Hemostasis 25 (Suppl 3): 79–82. 1999. PMID 10549720.
- ↑ "Parenteral anticoagulants: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest 141 (2 Suppl): e24S–e43S. February 2012. doi:10.1378/chest.11-2291. PMID 22315264.
- ↑ "Enhanced Recovery after Urological Surgery: A Contemporary Systematic Review of Outcomes, Key Elements, and Research Needs". European Urology 70 (1): 176–187. July 2016. doi:10.1016/j.eururo.2016.02.051. PMID 26970912.
- ↑ "Computerized Registry of Patients with Veneous Thromboembolism — RIETE Registry". S & H Medical Science Service. https://www.riete.org/info/estimate-calculator/index.php.
 | Original source: https://en.wikipedia.org/wiki/Thrombosis prevention. Read more |
|
|