Chemistry:Lurasidone
Lurasidone, sold under the brand name Latuda among others, is an atypical antipsychotic medication used to treat schizophrenia and bipolar depression.[1] It is taken by mouth.
Common side effects include sedation, indigestion, nausea, and insomnia. At higher dosages, there is an increased risk for restlessness and movement problems.[1] Serious side effects are valid for all atypical antipsychotics and may include the potentially permanent movement disorder tardive dyskinesia, as well as neuroleptic malignant syndrome, an increased risk of suicide, angioedema, and high blood sugar levels.[2] Although lurasidone is less likely to cause high blood sugar levels in most patients, hyperosmolar hyperglycemic syndrome may occur.[1][3][4] In older people with psychosis as a result of dementia, it may increase the risk of dying.[1] Use during pregnancy is of unclear safety.[5][6]
Lurasidone was first approved for medical use in the United States in 2010, for treating schizophrenia.[1] In 2013, it was approved in Canada and by the U.S. Food and Drug Administration (FDA) to treat bipolar depression, either as monotherapy or adjunctively with lithium or valproate.[7][8] It is not FDA approved for treating manic symptoms associated with bipolar disorder despite its FDA approval for treating bipolar depression. Generic versions were approved in the United States in 2019, and became available in 2023.[9][10] In 2021, it was the 193rd most commonly prescribed medication in the United States, with more than 2 million prescriptions.[11][12]
Medical uses
Lurasidone is used to treat schizophrenia and bipolar disorder.[1][13] In bipolar disorder, it has been studied both as a monotherapy and adjunctive treatment to lithium or valproate.[14]
The European Medicines Agency approved lurasidone for the treatment of schizophrenia for people aged 13 years and older.[15][16] Its use in Europe for bipolar disorder is considered off-label.[17] In the United States, it is used to treat schizophrenia for people aged 13 years and older. In July 2013, lurasidone received approval for bipolar I depression.[18][19][20][21] This includes depressive episodes of bipolar disorder age 10 and over as a monotherapy, and in conjunction with lithium or valproate in adults.[22]
In June 2020, lurasidone was approved in Japan, eight years after its first approval in the United States.[23] In Japan it is approved for bipolar depression and schizophrenia.[24][25][26] Lurasidone is not approved by the Food and Drug Administration (FDA) for the treatment of behavior disorders in older adults with dementia.[27]
Few available atypical antipsychotics are known to possess antidepressant efficacy in bipolar disorder (with the notable exceptions being cariprazine,[28] quetiapine,[29][30][31][32] olanzapine[33][34][35] and possibly asenapine[36]) as a monotherapy. The majority of atypical antipsychotics are known to possess significant antimanic activity,[37] however lurasidone is unusual as it was never studied for acute mania.[38]
In the early post approval period lurasidone-treated patients with bipolar disorder were retrospectively found to have more complex clinical profiles, comorbidities, and prior treatment history compared to patients initiated with other atypical antipsychotics. The study authors suggest this may be due to "the overall clinical profile of lurasidone, the role perceived for lurasidone in the therapeutic armamentarium by practitioners, and the recent introduction of lurasidone into clinical practice during the study period".[39]
Contraindications
Lurasidone is contraindicated in individuals who are taking strong inhibitors of the liver enzyme CYP3A4 (ketoconazole, clarithromycin, ritonavir, levodropropizine, etc.) or inducers (carbamazepine, St. John's wort, phenytoin, rifampicin etc.).[40] The use of lurasidone in pregnant women has not been studied and is not recommended; in animal studies, no risks have been found.[41] Excretion in breast milk is also unknown; lurasidone is not recommended for breastfeeding women.[42] The enzyme CYP3A4 is involved in the digestion of drugs. Inhibitors such as grapefruit juice block its function, resulting in too much drug in the body.[43]
Side effects
Side effects are generally similar to other antipsychotics. The drug has a relatively well tolerated side effect profile, with low propensity for QTc interval changes,[44][45] weight gain and lipid-related adverse effects.[46] In a 2013 meta-analysis of the efficacy and tolerability of 15 antipsychotic drugs, it was found to produce the second least (after haloperidol) weight gain, the least QT interval prolongation, the fourth most extrapyramidal side effects (after haloperidol, zotepine and chlorpromazine), and the sixth least sedation (after paliperidone, sertindole, amisulpride, iloperidone and aripiprazole).[47]
As with other atypical neuroleptics, lurasidone should be used with caution in the elderly because it puts them at an increased risk for a stroke or transient ischemic attack;[48][49] however, these risks are not likely to be greater than those associated with antipsychotics of other classes.[50] Similarly, lurasidone should not be used to treat dementia-related psychosis, as evidence has shown increased mortality with antipsychotic use.[51]
Weight gain is reported in up to 15 and 16 percent of users.[52][53] Other possible side effects include vomiting, akathisia, dystonia, parkinsonism, somnolence, dizziness, sedation and nausea.[54][55]
Discontinuation
The British National Formulary recommends a gradual withdrawal when discontinuing antipsychotics to avoid acute withdrawal syndrome or rapid relapse.[56] Symptoms of withdrawal commonly include nausea, vomiting, and loss of appetite.[57] Other symptoms may include restlessness, increased sweating, and trouble sleeping.[57] Less commonly there may be a feeling of the world spinning, numbness, or muscle pains.[57] Symptoms generally resolve after a short period of time.[57]
There is tentative evidence that discontinuation of antipsychotics can result in psychosis.[58] It may also result in reoccurrence of the condition that is being treated.[59] Rarely tardive dyskinesia can occur when the medication is stopped.[57]
Interactions
Blood plasma concentrations may be increased when combined with CYP3A4 inhibitors (e.g. ketoconazole, clarithromycin, ritonavir, and voriconazole) possibly leading to more side effects. This has been clinically verified for ketoconazole, which increases lurasidone exposure by a factor of 9, and is also expected for other 3A4 inhibitors such as grapefruit juice. Co-administration of CYP3A4 inducers like rifampicin, carbamazepine or St. John's wort can reduce plasma levels of lurasidone and its active metabolite, and consequently decrease the effects of the drug. For rifampicin, the reduction was sixfold in a study.[60]
Pharmacology
Pharmacodynamics
| Site | Ki (nM) | Action | Species | Ref |
|---|---|---|---|---|
| NET | ND | ND | ND | ND |
| DAT | >1,000 | ND | ND | [61] |
| 5-HT1A | 6.7 | Partial agonist | Human | [62] |
| 5-HT2A | 0.5-2 | antagonist | Rat | [61] |
| 5-HT2B | 24 | ND | Human | [63] |
| 5-HT2C | 415 | ND | Pig | [61] |
| 5-HT3 | >1,000 | ND | ND | [61] |
| 5-HT4 | >1,000 | ND | ND | [61] |
| 5-HT7 | 0.5 | Inverse agonist | Human | [64][61] |
| α1 | 47.9 | ND | Rat | [61] |
| α2A | 41 | Antagonist | Human | [61] |
| α2B | ND | ND | ND | ND |
| α2C | 10.8 | Antagonist | Human | [61] |
| β1 | >1,000 | ND | ND | [61] |
| β2 | >1,000 | ND | ND | [61] |
| D1 | 262 | ND | ND | [61] |
| D2s | 1.2-1.7 | Antagonist | Human | [62] |
| D3S | 15.7 | Antagonist | ND | ND |
| D4.4L | 30 | Positive allosteric modulator | ND | ND |
| D5 | ND | ND | ND | ND |
| H1 | >1,000 | ND | Guinea pig | [61] |
| M1 | >1,000 | ND | Human | [61] |
| Values are Ki (nM). The smaller the value, the more strongly the drug binds to the site. | ||||
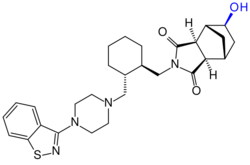
Lurasidone [(3aR,4S,7R,7aS)-2-{(1R,2R)-2-[4-(1,2-benzisothiazol-3-yl) piperazin-1-ylmethyl]-cyclohexylmethyl}-hexahydro-4,7-methano-2Hisoindole-1,3-dione hydrochloride] ][65] is an azapirone derivative[66] and acts as an antagonist of the dopamine D2 and D3 receptors,[67] and the serotonin 5-HT2A and 5-HT7 receptors, and the α2C-adrenergic receptor, and as a partial agonist of the serotonin 5-HT1A receptor. It has moderate-affinity antagonism at α2C-adrenergic receptors; low to very low-affinity antagonism at α1A-adrenergic α2A-adrenergic receptors.[68]
It has only low and likely clinically unimportant affinity for the serotonin 5-HT2C receptor, which may underlie its low propensity for appetite stimulation and weight gain.[61][69][70] The drug also has negligible affinity for the histamine H1 receptor and the muscarinic acetylcholine receptors, and hence has no antihistamine or anticholinergic effects.[71][72] Drowsiness (somnolence) side effect is not explained by its antagonist activity to histamine.[73][74]
The relationship between dose and D2 receptor occupancy levels were 41–43% for 10 mg, 51–55% for 20 mg, 63–67% for 40 mg, 77–84% for 60 mg, and 73–79% for 80 mg.[75]
Pharmacokinetics

Lurasidone is taken by mouth and should be taken with a meal of at least 350 calories to ensure maximum absorption.[79] It has an estimated absorption rate of 9 to 19%.[80] Studies have shown that when lurasidone is taken with food, absorption increases about twofold.[60]
Peak blood plasma concentrations are reached after one to three hours. About 99% of the circulating substance are bound to plasma proteins.[60] Efficacy data for lurasidone have been evaluated for doses of 20 mg to 120 mg daily.
In schizophrenia, lurasidone has a recommended dose range of 40-160 mg. In bipolar depression, lurasidone has a slightly lower recommended dose range of 20-120 mg.[81]
Lurasidone is extensively metabolised by CYP3A4 leading to contraindication of both strong inhibitors as well as strong inducers of this enzyme,[82] but has negligible affinity to other cytochrome P450 enzymes. It is transported by P-glycoprotein and ABCG2 and also inhibits these carrier proteins in vitro. It also inhibits the solute carrier protein SLC22A1, but no other relevant transporters.[60][48]
Main metabolism pathways are oxidative N-dealkylation between the piperazine and cyclohexane rings, hydroxylation of the norbornane ring, and S-oxidation.[60][78]:59 Other pathways are hydroxylation of the cyclohexane ring and reductive cleavage of the isothiazole ring followed by S-methylation.[77]
The two relevant active metabolites are the norbornane hydroxylation products called ID-14283 and ID-14326, the former reaching pharmacologically relevant blood plasma concentrations. The two major inactive metabolites are the N-dealkylation products (the carboxylic acid ID-20219 and the piperazine ID-11614[77]), and a norbornane hydroxylated derivative of ID-20219 (ID-20220). Of lurasidone and its metabolites circulating in the blood, the native drug makes up 11%, the main active metabolite 4%, and the inactive carboxylic acids 24% and 11%, respectively.[80][60] Several dozen metabolites have been identified altogether.[78]:59–61
Biological half-life is given as 18 hours or 20 to 40 hours in different sources. 80% or 67% of a radiolabelled dose was recovered from the feces, and 9% or 19% from the urine.[80][60]
History
Lurasidone was first synthesised circa 2003.[83] Lurasidone is a structural analogue of ziprasidone.[77] Lurasidone shows a very close pharmacological profile and has been synthesized similarly to ziprasidone.[84] Lurasidone is chemically similar to perospirone (also a chemical analogue of ziprasidone), as well as risperidone, paliperidone and iloperidone.[85]
Lurasidone was developed by Sunovion Pharmaceuticals, a division of Dainippon Sumitomo Pharma Co. of Japan.[86] In 2009, Sunovion decided to develop lurasidone for the treatment of bipolar depression.[87]
Society and culture
Regulatory approval
Lurasidone was approved in the United States for the treatment of schizophrenia in October 2010[88][89] and for the treatment of depressive episodes associated with bipolar I disorder in June 2013.[18][20][21] In 2015, lurasidone was studied for major depressive disorder with mixed features in a randomized trial and had a positive result, however it did not receive an FDA indication for it.[38][90] In 2017, the FDA approved lurasidone for schizophrenia in adolescents age 13-17. In 2018, lurasidone was approved for bipolar depression in children and adolescents age 10-17.[81]
It received regulatory approval in the United Kingdom in September 2014. In October 2014, NHS Scotland advised use of lurasidone for schizophrenic adults who have not seen improvements with previous antipsychotics due to problems that arise from weight gain or changes in metabolic pathways when taking other medications.[91]
The Committee for Medicinal Products for Human Use (CHMP) of the European Medicines Agency (EMA) issued a positive opinion for it in January 2014, and it was approved for medical use by the EMA in March 2014.[16] It was launched in Canada for the treatment of schizophrenia in September 2012, Health Canada giving their Summary Basis of Decision (SBD) as favourable on 15 October 2012.[92] The European Commission has granted a marketing authorization for once-daily oral lurasidone for the treatment of schizophrenia in adults.[93] It is approved for use in the EU.[16]
Generic versions of lurasidone were approved for use in the United States in January 2019 and became available in 2023.[94][9][10]
Brand names
In India, this drug is available under the brand names of Atlura, Lurace, Lurafic, Luramax (Sun Pharma), Lurasid, Lurastar, Latuda, Lurata[95] and additionally as Alsiva, Emsidon, Lurakem, Luratrend, Tablura, and Unisidon.[96]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 "Lurasidone Hydrochloride Monograph for Professionals". American Society of Health-System Pharmacists. https://www.drugs.com/monograph/lurasidone-hydrochloride.html.
- ↑ "IMPORTANT SAFETY INFORMATION AND INDICATIONS FOR LATUDA". https://www.latuda.com/sz/important-safety-information.html.
- ↑ "The metabolic side effects of 12 antipsychotic drugs used for the treatment of schizophrenia on glucose: a network meta-analysis". BMC Psychiatry 17 (1). November 2017. doi:10.1186/s12888-017-1539-0. PMID 29162032.
- ↑ "Lurasidone-induced hyperosmolar hyperglycemic syndrome: A case report". Neuropsychopharmacology Reports 42 (3): 377–379. September 2022. doi:10.1002/npr2.12259. PMID 35609885.
- ↑ British national formulary: BNF 76 (76 ed.). Pharmaceutical Press. 2018. pp. 393–394. ISBN 978-0-85711-338-2.
- ↑ "Lurasidone (Latuda) tablets for the treatment of schizophrenia in adults". https://www.sps.nhs.uk/wp-content/uploads/2015/03/final20draft.pdf.
- ↑ "Lurasidone: a new treatment option for bipolar depression-a review". Innovations in Clinical Neuroscience 12 (1–2): 21–23. 2015. PMID 25852975.
- ↑ "Long-term use of lurasidone in patients with bipolar disorder: safety and effectiveness over 2 years of treatment". International Journal of Bipolar Disorders 5 (1). December 2017. doi:10.1186/s40345-017-0075-7. PMID 28168632.
- ↑ 9.0 9.1 "Generic Latuda Availability". https://www.drugs.com/availability/generic-latuda.html.
- ↑ 10.0 10.1 "Generic-Drug Approvals Soar, But Patients Still Go Without". Wall Street Journal. 19 November 2019. https://www.wsj.com/articles/many-generic-drugs-havent-hit-market-hindering-cost-control-efforts-11574198448.
- ↑ "The Top 300 of 2021". https://clincalc.com/DrugStats/Top300Drugs.aspx.
- ↑ "Lurasidone - Drug Usage Statistics". https://clincalc.com/DrugStats/Drugs/Lurasidone.
- ↑ "Lurasidone for major depressive disorder with mixed features and irritability: a post-hoc analysis". CNS Spectrums 22 (2): 228–235. April 2017. doi:10.1017/S1092852917000232. PMID 28300012.
- ↑ "Evaluating lurasidone as a treatment option for bipolar disorder". Expert Opinion on Pharmacotherapy 21 (3): 253–260. February 2020. doi:10.1080/14656566.2019.1695777. PMID 31957501.
- ↑ "Latuda (lurasidone) An overview. European Medicines Agency, 2020". https://www.ema.europa.eu/en/documents/overview/latuda-epar-medicine-overview_en.pdf.
- ↑ 16.0 16.1 16.2 "Latuda EPAR". 17 September 2018. https://www.ema.europa.eu/en/medicines/human/EPAR/latuda.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ "Lurasidone in treatment of manic episode" (in en). European Psychiatry 65 (S1): S400–S400. June 2022. doi:10.1192/j.eurpsy.2022.1013. ISSN 0924-9338. PMC 9565617. https://www.cambridge.org/core/product/identifier/S0924933822010136/type/journal_article.
- ↑ 18.0 18.1 "Lurasidone Approved for Bipolar Depression". Medscape. 2013. http://www.medscape.com/viewarticle/807204.
- ↑ "Lurasidone: a new treatment option for bipolar depression-a review". Innovations in Clinical Neuroscience 12 (1–2): 21–23. 2015. PMID 25852975.
- ↑ 20.0 20.1 "Latuda Supplement Approval Package 1". https://www.accessdata.fda.gov/drugsatfda_docs/nda/2013/200603Orig1s010.pdf.
- ↑ 21.0 21.1 "Latuda Supplement Approval Package 2". https://www.accessdata.fda.gov/drugsatfda_docs/nda/2013/200603Orig1s011.pdf.
- ↑ Canadian Agency for Drugs and Technologies in Health (2014). "Key Limitations". Lurasidone Hydrochloride (Latuda): Management of Manifestations of Schizophrenia. Canadian Agency for Drugs and Technologies in Health. https://www.ncbi.nlm.nih.gov/books/NBK195617/. Retrieved 30 April 2020.
- ↑ "Latuda to Finally Hit Japan Market on June 11" (in en). https://pj.jiho.jp/article/242267.
- ↑ "Sumitomo Dainippon Pharma Announces Approval of Atypical Antipsychotic Agent, LATUDA Tablets in Japan" (in en). IR News | Investor Relations. Sumitomo Pharma. https://www.sumitomo-pharma.com/ir/news/2020/20200325-1.html.
- ↑ "Kusuri-no-Shiori(Drug Information Sheet) Latuda tablets" (in en). https://www.rad-ar.or.jp/siori/english/search/result?n=43474.
- ↑ "Current Limitations and Candidate Potential of 5-HT7 Receptor Antagonism in Psychiatric Pharmacotherapy". Frontiers in Psychiatry 12. 2021. doi:10.3389/fpsyt.2021.623684. PMID 33679481.
- ↑ "Lurasidone". MedlinePlus. U.S. National Library of Medicine. https://medlineplus.gov/druginfo/meds/a611016.html.
- ↑ "Cariprazine for the treatment of bipolar depression: a review". Expert Review of Neurotherapeutics 19 (4): 317–323. April 2019. doi:10.1080/14737175.2019.1580571. PMID 30753085.
- ↑ "A double-blind, placebo-controlled study of quetiapine and lithium monotherapy in adults in the acute phase of bipolar depression (EMBOLDEN I)". The Journal of Clinical Psychiatry 71 (2): 150–162. February 2010. doi:10.4088/JCP.08m04995gre. PMID 20122369.
- ↑ "Effectiveness of the extended release formulation of quetiapine as monotherapy for the treatment of acute bipolar depression". Journal of Affective Disorders 121 (1–2): 106–115. February 2010. doi:10.1016/j.jad.2009.10.007. PMID 19903574.
- ↑ "Corrigendum". Bipolar Disorders 10 (3): 451. 2008. doi:10.1111/j.1399-5618.2008.00585.x.
- ↑ "Quetiapine monotherapy for bipolar depression". Neuropsychiatric Disease and Treatment 4 (1): 11–21. February 2008. doi:10.2147/ndt.s1162. PMID 18728771.
- ↑ "Efficacy of olanzapine and olanzapine-fluoxetine combination in the treatment of bipolar I depression". Archives of General Psychiatry 60 (11): 1079–1088. November 2003. doi:10.1001/archpsyc.60.11.1079. PMID 14609883.
- ↑ "Efficacy of olanzapine monotherapy in acute bipolar depression: a pooled analysis of controlled studies". Journal of Affective Disorders 149 (1–3): 196–201. July 2013. doi:10.1016/j.jad.2013.01.022. PMID 23485111.
- ↑ "A 24-week open-label extension study of olanzapine-fluoxetine combination and olanzapine monotherapy in the treatment of bipolar depression". The Journal of Clinical Psychiatry 67 (5): 798–806. May 2006. doi:10.4088/JCP.v67n0514. PMID 16841630.
- ↑ "Effect of asenapine on manic and depressive symptoms in bipolar I patients with mixed episodes: results from post hoc analyses". Journal of Affective Disorders 145 (1): 62–69. February 2013. doi:10.1016/j.jad.2012.07.013. PMID 22868059.
- ↑ "Comparative efficacy and acceptability of antimanic drugs in acute mania: a multiple-treatments meta-analysis". Lancet 378 (9799): 1306–1315. October 2011. doi:10.1016/S0140-6736(11)60873-8. PMID 21851976.
- ↑ 38.0 38.1 Clinical Psychopharmacology: Principles and Practice (1st ed.). New York, NY: Oxford University Press. 2019. pp. 185-186. ISBN 9780199995486.
- ↑ "Patient Characteristics Associated With Use of Lurasidone Versus Other Atypical Antipsychotics in Patients With Bipolar Disorder: Analysis From a Claims Database in the United States". The Primary Care Companion for CNS Disorders 19 (3). June 2017. doi:10.4088/PCC.16m02066. PMID 28590601.
- ↑ "Lurasidone drug-drug interaction studies: a comprehensive review". Drug Metabolism and Drug Interactions 29 (3): 191–202. 2014. doi:10.1515/dmdi-2014-0005. PMID 24825095.
- ↑ Pregnancy category
- ↑ ACOG Committee on Practice Bulletins--Obstetrics (April 2008). "ACOG Practice Bulletin: Clinical management guidelines for obstetrician-gynecologists number 92, April 2008 (replaces practice bulletin number 87, November 2007). Use of psychiatric medications during pregnancy and lactation". Obstetrics and Gynecology 111 (4): 1001–1020. doi:10.1097/AOG.0b013e31816fd910. PMID 18378767.
- ↑ Office of the Commissioner (14 July 2021). "Grapefruit Juice and Some Drugs Don't Mix" (in en). FDA. https://www.fda.gov/consumers/consumer-updates/grapefruit-juice-and-some-drugs-dont-mix.
- ↑ "Lurasidone is not associated with risk of QTc prolongation". Clinical Research in Practice: The Journal of Team Hippocrates 4 (2). 14 September 2018. doi:10.22237/crp/1536278400. ISSN 2379-4550. https://digitalcommons.wayne.edu/crp/vol4/iss2/8. Retrieved 15 November 2022.
- ↑ "Practical Guidance on the Use of Lurasidone for the Treatment of Adults with Schizophrenia". Neurology and Therapy 8 (2): 215–230. December 2019. doi:10.1007/s40120-019-0138-z. PMID 31098889.
- ↑ "Lurasidone Demonstrated Efficacy in Treating Patients With Schizophrenia in Pivotal Phase 3 Study" (Press release). Dainippon Sumitomo Pharma. 26 August 2009. Archived from the original on 14 May 2015. Retrieved 3 October 2016.
- ↑ "Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis". Lancet 382 (9896): 951–962. September 2013. doi:10.1016/S0140-6736(13)60733-3. PMID 23810019.
- ↑ 48.0 48.1 "Latuda: Prescribing Information". Psychotherapeutic Drugs. http://psychotherapeuticdrugs.com/index.php/new-drug-approvals/latuda-lurasidone-hcl.
- ↑ "Latuda". Drugs.com. https://www.drugs.com/latuda.html.
- ↑ "Atypical antipsychotics and risk of cerebrovascular accidents". The American Journal of Psychiatry 161 (6): 1113–1115. June 2004. doi:10.1176/appi.ajp.161.6.1113. PMID 15169702.
- ↑ "Latuda Prescribing Information". Sunovion Pharmaceuticals. http://www.latuda.com/LatudaPrescribingInformation.pdf.
- ↑ "Weight change during long-term treatment with lurasidone: pooled analysis of studies in patients with schizophrenia". International Clinical Psychopharmacology 30 (6): 342–350. November 2015. doi:10.1097/YIC.0000000000000091. PMID 26196189.
- ↑ "Lurasidone in the Long-Term Treatment of Patients with Bipolar Disorder: A 24-Week Open-Label Extension Study". Depression and Anxiety 33 (5): 424–434. May 2016. doi:10.1002/da.22479. PMID 26918425.
- ↑ "Short-term efficacy and tolerability of lurasidone in the treatment of acute schizophrenia: A meta-analysis of randomized controlled trials". Journal of Psychiatric Research 103: 244–251. August 2018. doi:10.1016/j.jpsychires.2018.06.005. PMID 29906709.
- ↑ "Food Matters: Reduction of Lurasidone-Induced Nausea With Meals". The Primary Care Companion for CNS Disorders 21 (2). March 2019. doi:10.4088/PCC.18l02343. PMID 30869204.
- ↑ BMJ Joint Formulary Committee (March 2009). "4.2.1". British National Formulary (57 ed.). United Kingdom: Royal Pharmaceutical Society of Great Britain. p. 192. ISBN 978-0-85369-845-6. "Withdrawal of antipsychotic drugs after long-term therapy should always be gradual and closely monitored to avoid the risk of acute withdrawal syndromes or rapid relapse."
- ↑ 57.0 57.1 57.2 57.3 57.4 Adverse Syndromes and Psychiatric Drugs: A Clinical Guide. OUP Oxford. 2004. pp. 207–216. ISBN 978-0-19-852748-0. https://books.google.com/books?id=CWR7DwAAQBAJ&pg=PA207. Retrieved 8 May 2020.
- ↑ "Does antipsychotic withdrawal provoke psychosis? Review of the literature on rapid onset psychosis (supersensitivity psychosis) and withdrawal-related relapse". Acta Psychiatrica Scandinavica 114 (1): 3–13. July 2006. doi:10.1111/j.1600-0447.2006.00787.x. PMID 16774655.
- ↑ Adherence to Antipsychotics in Schizophrenia. Springer Science & Business Media. 2013. p. 85. ISBN 978-88-470-2679-7. https://books.google.com/books?id=odE-AgAAQBAJ&pg=PA85. Retrieved 8 May 2020.
- ↑ 60.0 60.1 60.2 60.3 60.4 60.5 60.6 "Latuda: EPAR – Product Information". European Medicines Agency. 14 April 2016. http://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Product_Information/human/002713/WC500164683.pdf.
- ↑ 61.00 61.01 61.02 61.03 61.04 61.05 61.06 61.07 61.08 61.09 61.10 61.11 61.12 61.13 61.14 Cite error: Invalid
<ref>tag; no text was provided for refs namedpmid20404009 - ↑ 62.0 62.1 "Synthesis and biological evaluation of new multi-target 3-(1H-indol-3-yl)pyrrolidine-2,5-dione derivatives with potential antidepressant effect". European Journal of Medicinal Chemistry 183. December 2019. doi:10.1016/j.ejmech.2019.111736. PMID 31586817.
- ↑ "2B Determined: The Future of the Serotonin Receptor 2B in Drug Discovery". J Med Chem 66 (16): 11027–11039. August 2023. doi:10.1021/acs.jmedchem.3c01178. PMID 37584406.
- ↑ "The preclinical profile of lurasidone: clinical relevance for the treatment of schizophrenia". Expert Opinion on Drug Discovery 8 (10): 1297–1307. October 2013. doi:10.1517/17460441.2013.815163. PMID 23837554.
- ↑ "(3aR,4S,7R,7aS)-2-[[(1R,2R)-2-[[4-(1,2-Benzisothiazol-3-yl)-1-piperazinyl]methyl]cyclohexyl]methyl]hexahydro-4,7-methano-1H-isoindole-1,3(2H)-dione" (in en). PubChem. U.S. National Library of Medicine. https://pubchem.ncbi.nlm.nih.gov/compound/50918847.
- ↑ "Efficacy and Safety of Lurasidone in Children and Adolescents: Recommendations for Clinical Management and Future Research". Current Pharmaceutical Design 27 (39): 4062–4069. 2021. doi:10.2174/1381612827666210804110853. PMID 34348620.
- ↑ "The pharmacodynamic properties of lurasidone and their role in its antidepressant efficacy in bipolar disorder". European Neuropsychopharmacology 25 (3): 335–342. March 2015. doi:10.1016/j.euroneuro.2014.11.010. PMID 25596883.
- ↑ "Lurasidone for the treatment of bipolar depression: an evidence-based review". Neuropsychiatric Disease and Treatment 11: 2143–2152. 19 August 2015. doi:10.2147/NDT.S50961. PMID 26316760.
- ↑ "[Short-term efficacy and safety of lurasidone in the treatment of schizophrenia]" (in fr). L'Encephale 40 (6): 507–517. December 2014. doi:10.1016/j.encep.2014.10.009. PMID 25453735.
- ↑ "Lurasidone for Schizophrenia". Current Psychiatry 10 (1): 67–70. 2011. http://www.mdedge.com/currentpsychiatry/article/64162/schizophrenia-other-psychotic-disorders/lurasidone-schizophrenia. Retrieved 2 October 2016.
- ↑ "Lurasidone (SM-13496), a novel atypical antipsychotic drug, reverses MK-801-induced impairment of learning and memory in the rat passive-avoidance test". European Journal of Pharmacology 572 (2–3): 160–170. October 2007. doi:10.1016/j.ejphar.2007.06.058. PMID 17662268.
- ↑ "Pharmacokinetics and Pharmacodynamics of Lurasidone Hydrochloride, a Second-Generation Antipsychotic: A Systematic Review of the Published Literature". Clinical Pharmacokinetics 56 (5): 493–503. May 2017. doi:10.1007/s40262-016-0465-5. PMID 27722855.
- ↑ "Lurasidone HCl (Latuda), an Oral, Once-Daily Atypical Antipsychotic Agent for the Treatment of Patients with Schizophrenia". P & T 36 (8): 489–492. August 2011. PMID 21935296.
- ↑ "Novel antipsychotics specificity profile: A clinically oriented review of lurasidone, brexpiprazole, cariprazine and lumateperone". European Neuropsychopharmacology 29 (9): 971–985. September 2019. doi:10.1016/j.euroneuro.2019.06.008. PMID 31255396. https://kclpure.kcl.ac.uk/portal/en/publications/bf9947d3-f6a6-486d-9420-771d89443f76.
- ↑ "Determination of dopamine D2 receptor occupancy by lurasidone using positron emission tomography in healthy male subjects". Psychopharmacology 229 (2): 245–252. September 2013. doi:10.1007/s00213-013-3103-z. PMID 23649882.
- ↑ "LC-MS/MS assay for the determination of lurasidone and its active metabolite, ID-14283 in human plasma and its application to a clinical pharmacokinetic study". Biomedical Chromatography 30 (7): 1065–1074. July 2016. doi:10.1002/bmc.3651. PMID 26577488.
- ↑ 77.0 77.1 77.2 77.3 77.4 "Critical appraisal of lurasidone in the management of schizophrenia". Neuropsychiatric Disease and Treatment 8: 155–168. 2012. doi:10.2147/NDT.S18059. PMID 22570547.
- ↑ 78.0 78.1 78.2 "Lurasidone pharmacology review". Center for Drug Evaluation and Research. 30 December 2009. http://www.accessdata.fda.gov/drugsatfda_docs/nda/2010/200603Orig1s000PharmR.pdf.
- ↑ "Lurasidone". StatPearls. Treasure Island (FL): StatPearls Publishing. 2025. http://www.ncbi.nlm.nih.gov/books/NBK541057/. Retrieved 2026-01-20.
- ↑ 80.0 80.1 80.2 Cite error: Invalid
<ref>tag; no text was provided for refs namedTGA - ↑ 81.0 81.1 "label". December 2019. https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/200603s035lbl.pdf.
- ↑ "European Medicines Agency Assessment report Latuda International non-proprietary name: LURASIDONE Procedure No. EMEA/H/C/002713/0000". https://www.ema.europa.eu/en/documents/assessment-report/latuda-epar-public-assessment-report_en.pdf.
- ↑ "Leading Latuda through the crowd". 1 October 2011. http://www.mmm-online.com/features/leading-latuda-through-the-crowd/article/213096/. "Latuda was developed at an R&D facility established in Fort Lee, NJ, about eight years ago by Sunovion's Japanese parent Dainippon Sumitomo Pharma Co. (DSP)."
- ↑ Synthesis of Best-Seller Drugs. Academic Press. 7 January 2016. ISBN 978-0-12-411524-8. https://books.google.com/books?id=A8oHBgAAQBAJ&pg=PA100. Retrieved 4 September 2017.
- ↑ "EXCLI Journal". 17 November 2016. http://excli.de/vol13/Mauri_13102014_proof.pdf.
- ↑ "FDA approves Sunovion's Latuda to treat some cases of bipolar disorder" (in en-US). 2013-07-03. https://www.boston.com/news/untagged/2013/07/03/fda-approves-sunovions-latuda-to-treat-some-cases-of-bipolar-disorder/.
- ↑ "The development of lurasidone for bipolar depression". Annals of the New York Academy of Sciences 1358 (1): 95–104. November 2015. doi:10.1111/nyas.12965. PMID 26771990.
- ↑ "Drug Approval Package: Latuda (lurasidone hydrochloride) Tablets NDA #200603". 24 December 1999. https://www.accessdata.fda.gov/drugsatfda_docs/nda/2010/200603Orig1s000TOC.cfm.
- ↑ "FDA approves Latuda to treat schizophrenia in adults" (Press release). U.S. Food and Drug Administration (FDA). 28 October 2010. Archived from the original on 30 October 2010. Retrieved 29 October 2010.
- ↑ "Lurasidone for the Treatment of Major Depressive Disorder With Mixed Features: A Randomized, Double-Blind, Placebo-Controlled Study". The American Journal of Psychiatry 173 (4): 400–407. April 2016. doi:10.1176/appi.ajp.2015.15060770. PMID 26552942.
- ↑ "Lurasidone, 18.5mg, 37mg, 74mg film-coated tablets (Latuda) SMC No. (994/14)". scottishmedicines.org.uk. Scottish Medicines Consortium. 2014. http://www.scottishmedicines.org.uk/files/advice/lurasidone__Latuda__FINAL_Sept_2014_amended_15.09.14_for_website.pdf.
- ↑ "Summary Basis of Decision (SBD) for Latuda". hc-sc.gc.ca. Health Canada. 2012. http://www.hc-sc.gc.ca/dhp-mps/prodpharma/sbd-smd/drug-med/sbd_smd_2012_latuda_145406-eng.php#a2.
- ↑ "European Marketing Authorization for Latuda". takeda.com. http://www.tpi.takeda.com/media/news-releases/2014/european-marketing-authorization-for-latuda/.
- ↑ "Lurasidone: FDA-Approved Drugs". https://www.accessdata.fda.gov/scripts/cder/daf/index.cfm?event=overview.process&ApplNo=208049.
- ↑ "'Lurasidone' drug search". CIMS India. http://www.mims.com/india/drug/search?q=Lurasidone.
- ↑ "Generic Drugs (ndrugs.com)". https://www.ndrugs.com/?s=lurasidone#substitutes.
External links
- "FDA Drug Safety Communication: FDA urges caution about withholding opioid addiction medications from patients taking benzodiazepines or CNS depressants: careful medication management can reduce risks". 7 January 2021. https://www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-fda-urges-caution-about-withholding-opioid-addiction-medications.
 |
